Pulmonary rehabilitation in Africa: where are we? a multimethod study
Abbi-Monique Mamani Bilungula, Patrick Katoto, Rik Gosselink, Jean-Marie Ntumba Kayembe, Daniel Langer
Corresponding author: Abbi-Monique Mamani Bilungula, Department of Physical Medicine and Rehabilitation, Division of Cardio-Pulmonary Rehabilitation, Faculty of Medicine, University of Kinshasa, Lemba, B-190, Kinshasa, Democratic Republic of the Congo 
Received: 08 Oct 2021 - Accepted: 26 Apr 2022 - Published: 27 May 2022
Domain: Physical medicine and rehabilitation�or Physiatry
Keywords: Exercise, physiotherapy, pulmonary rehabilitation, Africa
©Abbi-Monique Mamani Bilungula et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Abbi-Monique Mamani Bilungula et al. Pulmonary rehabilitation in Africa: where are we? a multimethod study. Pan African Medical Journal. 2022;42:78. [doi: 10.11604/pamj.2022.42.78.31954]
Available online at: https://www.panafrican-med-journal.com//content/article/42/78/full
Pulmonary rehabilitation in Africa: where are we? a multimethod study
![]() Abbi-Monique Mamani Bilungula1,2,&, Patrick Katoto3,4,5,
Abbi-Monique Mamani Bilungula1,2,&, Patrick Katoto3,4,5, ![]() Rik Gosselink2,
Rik Gosselink2, ![]() Jean-Marie Ntumba Kayembe6, Daniel Langer2
Jean-Marie Ntumba Kayembe6, Daniel Langer2
&Corresponding author
Pulmonary rehabilitation (PR) is an integral part of the management of patients with chronic respiratory diseases. However, there is limited information available on the effectiveness and practice of PR in Africa. This study was conducted to examine the prevalence, structure, and organization of PR in Africa, as well as its substance and claimed efficacy. We conducted a multimethod study involving systematic review of PR studies (obtained from PubMed, Google Scholar, and Cochrane databases) and a web-based survey of African healthcare professionals engaged in PR (using a standardized questionnaire). The review included papers on at least one component of PR in Africa and excluded those on PR from other continents or assessing pulmonary disorders in general without PR, cardio-rehabilitation, or physiotherapy practice in general in Africa. The Cochrane risk of bias and the Newcastle Ottawa scale instruments were used to assess the quality of included studies. We narratively synthesised data across the studies to produce a holistic picture. Of the 14 studies included for qualitative synthesis, seven were randomized controlled trials on the effectiveness of PR treatments with a total number of 333 participants. Of the 39 surveys mailed to health professionals working in Africa, only 14 (35.8%) were returned. We found aerobic exercise and breathing exercises were the most used technique and that quality of life, exercise capacity, and lung function improved significantly after PR treatments. There were differences in the duration, frequency, and length of the programs across the continent. Half of the respondents indicated that their institutions had one or more PR programs for inpatient, outpatient, maintenance, and/or home-based programs. Additionally, aerobic activities, upper and lower extremity strength training were the most frequently used exercise modalities in PR programs, followed by breathing exercises. Pulmonary rehabilitation is understudied in Africa, but it has been linked to improved lung function, exercise capacity, and quality of life. There is a need to invest in techniques tailored to the continent to enhance the implementation of pulmonary rehabilitation in Africa.
In developing countries, public health is facing the impact of chronic respiratory diseases (CRDs) which is challenging because of their frequency, severity, projected trends and economic impact [1]. In low and middle income countries, CRDs are significantly involved in morbidity and mortality [2]. Detailed information on CRDs in Africa is limited. However, the scarce data suggests that the burden in this setting may be high: The international BOLD (Burden of Obstructive Lung Disease) study demonstrated a considerably higher prevalence of moderate to severe airway obstruction among adults aged 40 years or older in Cape Town, South Africa (19.1%) compared with that seen in Western Europe and North American settings (5.9-14.3%) [3]. Moreover, a systematic review summarizing data from 13 studies conducted in Africa, showed a median prevalence of chronic obstructive pulmonary diseases (COPD) in persons? 40 years of 13.4% (IQR: 9.4%-22.1%) with no significant differences in gender or the year of the study on the reported prevalence of COPD [4]. When applied to the appropriate age group (40 years or more), which accounted for 196.4 million people in Africa in 2010, the estimated prevalence translates into 26.3 million (18.5-43.4 million) cases of COPD suggesting an increase of 31.5% over a decade that is attributable to ageing of the African population alone (if compared to year 2000) [4].
The management of COPD is multidisciplinary [5] and pulmonary rehabilitation (PR) is an evidence-based treatment for CRDs [6]. PR program includes exercise training, education, psychosocial and behavioural intervention, nutritional education, outcome assessment and promotion of long-term adherence to rehabilitation recommendations [5]. PR should be prescribed for patients with chronic respiratory conditions like dyspnoea or other respiratory symptoms, which reduced tolerance to exercise and decreased daily activities [5]. PR is an integral part of the management of patients suffering from CRDs [7], also other than COPD [6], as well as restrictive lung disease [8]. However, there is not much information on the practice of PR in Africa. Though it is evident that in some African countries, such as South Africa, there are hospitals or healthcare with well-established PR programs [9]. Thus, we aimed to ascertain the nature of current PR practice in Africa to provide an overview of its organization (structure and content) as well as of its effectiveness to inform practice and policy.
We conducted a multimethod study combining a systematic review of the literature and a cross-sectional study among health workers involved in PR practice in Africa.
Systematic review
Search strategy and selection criteria: we searched the following electronic databases: PubMed, Google scholar, Cochrane. In general, databases were searched with a combination of terms (respiratory OR pulmonary) AND (rehabilitation OR exercise OR physiotherapy) AND (Africa OR Afrique) and derived keywords, including variations of the following terms: “chronic obstructive pulmonary disease OR COPD”, “asthma”, “tuberculosis”, “physiotherapy”, “exercise”, “rehabilitation”, “Africa”, “Afrique” or North Africa or “sub-Saharan-Africa”. No language restriction was applied; the timeframe of the search included all records from the electronic database inception December 2018 to September 30, 2020, and an update was realisedend ofJanuary 2021. In addition, grey literature was searched, and individual authors or organization were contacted for data completeness. The PR definition was described as “comprehensive intervention based on thorough patient assessment followed by patient-tailored therapies that include, but are not limited to, exercise training, education, and behaviour change, designed to improve the physical and psychological condition of people with chronic respiratory disease and to promote the long-term adherence to health-enhancing behaviours”[6]. We considered that every paper reporting on a part of PR in Africa was eligible for inclusion in the review. Consequently, studies reporting data on PR from other continents than Africa, on pulmonary diseases in general and not including PR, on other therapy than PR for pulmonary diseases, on cardio-rehabilitation and on physiotherapy practice in general in Africa were excluded. Our study population included children, adults or elderly residing in Africa. We assessed lung function [forced vital capacity (FVC), forced expiratory volume in one second (FEV1), and peak expiratory flow (PEF)] in randomized trials, as well as physical activity [six-minute walking distance (6MWD)] and quality of life (QoL). These findings were analysed to examine the effectiveness of the public relations programs provided in each study. The outcomes of patients with CRDs or a disease that results in a respiratory deficit were sought because this population is the target demographic for a PR program and the treatments employed in each trial. We used Zotero to manage references and eliminate duplications. Two reviewers (AB and PK) evaluated the eligibility of studies. In cases of discrepancy a third reviewer (JK) provided arbitration. All papers were screened on the content (patient population, country, aim of the paper, findings) and summed up in a table to provide an overview of the kind of research on PR in Africa in observational studies. A second table was built to report on the design of the study, population, intervention, outcome, and key findings of effectiveness studies.
Data analysis: we performed a narrative synthesis and produced summary tables of findings of included papers because methodological heterogeneity in exposure and outcome assessment precluded meta-analyses. This systematic review was reported according to the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guideline [10].
Risk of bias: two reviewers (AB and PK) independently assessed the papers' risk of bias and then debated the appropriate interpretation. In case of discrepancies, a third reviewer (JK) was asked to provide the final judgment. The Cochrane risk of bias instrument was used to assess the risk of bias in randomized trials studies, while the Newcastle Ottawa scale was utilized for observational studies.
Cross-sectional study
Study design, population, and settings: a cross-sectional study (from December 2018 to February 2020) was conducted using the questionnaire from a Canadian survey of 2005 published by Brooks et al. [11]. We obtained the ethical committee approval from the National Health Ethical Committee of Democratic Republic of Congo (amended as n�258/CNES/BN/PMMF/2021). This questionnaire contains 32-items that we used to assess PR program components, healthcare professionals working on PR, outcome measures and follow-up components in Africa. No personal information was asked. Health professionals (physiotherapists, physicians, and nurses) were identified online (through Google searches by country or by publication in the aforementioned databases) or via national, regional, and international respiratory societies (South African Physiotherapy Society, Algerian Physical Medicine and Rehabilitation Society, Pan African Thoracic Society and, European Respiratory Society). They were then asked if they have a functional unit of PR and if they would volunteer for the study. The survey was distributed through email to individuals who indicated an interest in participating.
Statistical analysis: data were collected via Microsoft Excel spreadsheet. SPSS statistical program was used to perform statistical analysis. Descriptive statistics such as the mean (standard deviation) and median (interquartile ranges) were calculated for data summary. The distribution of PR programs was calculated by expressing the number of facilities (public hospitals and private hospitals) per city and presenting the number of rehabilitation programs available per city. All programs mentioned in the survey (inpatient, outpatient, home-based, maintenance) and online support (other program) were present in different facilities in South Africa.
Ethical approval: we obtained the ethical approval from the National Health Ethical Committee of Democratic Republic of Congo (amendment n�258/CNES/BN/PMMF/2021).
Literature review on pulmonary rehabilitation in Africa
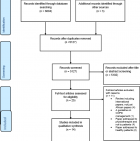
Characteristics of included studies: as shown in the PRISMA flow diagram (Figure 1), the initial searches provided 5127 non-duplicate records, of which 25 full texts were further assessed for eligibility and 14 studies were retained for qualitative synthesis. Eleven full texts were excluded because: Review including international papers, not just African papers (4), a guideline on COPD management (1), paper addressed to physiotherapist and not to patients (4), and paper addressed to healthy patients (2). Five thousand one hundred and two (5102) others do not rich the criteria (papers did not reported on pulmonary rehabilitation but on pulmonary diseases or others treatment and on other kinds of rehabilitation (neurological, orthopaedic). Geographically, included studies provided data from nine countries of which, four were from South Africa [12-15], two from Uganda [16,17], two from Nigeria[18,19] two from Zimbabwe [20,21], and one from Benin [22], one from Malawi [23], one from Egypt [24] and one from Democratic Republic of Congo (DRC) [25]. The study population was made of patients diagnosed for asthma, COPD, tuberculosis (TB) and post-tuberculosis lung disease (p-TBLD). Patients were also recruited from surgery department (who underwent a laparotomy), intensive care units (ICU) and from the human immunodeficiency virus/acquired immunodeficiency syndrome (HIV/AIDS) clinics. Table 1 provides a summary of observational studies assessing PR in Africa.
Risk of bias: Figure 2 and (Annex 1) summarize the authors´ judgment of risk of bias among included individual randomized studies using the Cochrane risk of bias tool and observational studies using the Newcastle Ottawa scale, respectively. The overall methodological quality assessment for interventional studies indicated a low risk of bias for selection and reporting bias while it showed an unclear to high risk of bias for performance, detection, and attrition biases. Further, among observational studies, the quality assessment of all the studies was high risk of bias with a substantial concern for lack of comparative groups.
Effectiveness of pulmonary rehabilitation: Table 2, Table 2 (suite), Table 2 (suite 1) provide an overview of the seven randomized controlled trials studies that reported effectiveness of the intervention, (two from South Africa[12,15], two from Nigeria[18,19], one from Malawi [23], one from Egypt [24] and one from Democratic Republic of the Congo (DRC) [25]). Studies differed regarding the type of intervention used. Differences were observed regarding the duration, frequency, and length of programs. In general, exercise programs lasted 10 to 30 minutes, conducted 2 or 3 times per week for 6 to 8 weeks and sometimes 16 weeks. Exercise capacity was assessed in three studies by the 6-minute walking test (6MWT) [15,24,25], and maximal power developed on cycle ergometer [25]. Significant improvements in exercise capacity were found [15,24,25]. Quality of life was measured in three studies [15,19,24], using the St Georges Respiratory Questionnaire (SGRQ) or COPD Assessment tool. There was no statistically significant difference between the intervention group and the control group in one study (p=0.789) [15], but significant improvements were observed in two others studies[19,24]. Most of studies reported significant improvement in lung function (FEV1, FVC, PEF, MVV, FEF, FEV1/FVC) [12,15,18,19,24,25] ((Table 2, Table 2 (suite), Table 2 (suite 1)).
Pulmonary rehabilitation components: Table 3 shows the components of PR programs. Exercise training (aerobic exercise) was included in five studies (walking, cycling and others aerobic exercises such as rower, step, whole-body exercise, climbing stairs and stretching) [12,15,18,19,25]. The most used component was breathing exercises reported in six studies [12,15,18,23-25]. Other components were education reported in three studies [15,18,19], home-exercises (in two studies) [12,15], resistance/strength training (in one study) [18], inspiratory muscle training (in one study) [12] and self-management (in one study) [12].
Survey
General consideration: E-mail addresses were hard to find and sometimes when they were found, they did not even exist anymore. Some correspondents did not answer directly to our e-mail, and some never responded. Of 39 surveys mailed to health professionals around Africa, only 14 (35,8%) were returned (from South Africa, DRC, Uganda, Nigeria, Angola, Cameroon, Niger, Senegal) from which seven health professionals (physiotherapist, pulmonologist, and physiatrist) reported having at least one or more PR programs in their facilities such as inpatient, outpatient, maintenance and/or home-based programs. One respondent (from South Africa) reported online support via an email/Skype program. The remaining seven respondents from South Africa, Senegal, Niger, Angola, Nigeria, and DRC reported the absence of a program in their facilities. The others 25 health professionals never answer to the mail.
Program characteristic, components, follow-up, and health worker: in- and outpatient programs were the most reported programs with a duration of 60 minutes (for each session) in general for three (outpatient program) or six (inpatient program) days per week with a length of six (inpatient program) or eight (outpatient program) weeks per session (Annex 2). Aerobic exercises, mostly walking (100% of in- and outpatient programs) and strength training of upper and lower extremities (100% of in- and outpatient programs) were the most used exercise modalities in PR programs, followed by breathing exercises (100% of in- and outpatient programs) (Annex 2). Home exercise prescription was provided for outpatient (86%) and for inpatient (80%) programs. There was little use of education (20% of inpatient, 57% of outpatient programs) and psychological support (20% of inpatient and 43% of outpatient programs) reported in PR programs. The distribution of follow-up components is summarized in Annex 2. Follow-up was added as part of the pulmonary rehabilitation program in all facilities that reported having a PR program in this study. Reassessment was the most used follow-up component (80% of inpatient and 100% of outpatient programs) and supervised exercises the least (0% of inpatient and 28% of outpatient programs). Pulmonologist, physiatrist, internist, and physical therapist were the most represented health professionals (100%, 71%, 57% and 43% respectively of outpatient program), while social worker (14% of outpatient program) and psychologist (28% of outpatient) were the least represented (Annex 2). Nurse and spiritual leader were absent in the reported programs. Other healthcare professionals, i.e., resuscitator/anaesthetist, thoracic surgeon, paediatrician was part of the PR program team in the Kinshasa facilities.
Outcome measures: outcome measures are shown in (Annex 3). The 6-minute walking test was the most frequently used measure (100% of in- and outpatient programs) followed by St Georges Respiratory Questionnaire (100% of in- and outpatient programs) and simple spirometry with bronchodilator response (100% of in- and outpatient programs). The Chronic Respiratory Disease Questionnaire, constant work rate test, 12-minute walking test and shuttle walk test were not used.
The interest of this review and survey was to investigate the current evidence and practice of PR in Africa (North and Sub-Saharan Africa). In the systematic review, 14 studies were included and showed a disparate existence of structured PR in some African facilities indicated for COPD patients, asthma, pulmonary tuberculosis and post-tuberculosis lung disease patients, surgical patients, ICU patients and HIV/AIDS patients. The improvement of quality of life of CRDs patients was also shown.
A web-based survey yielded a very limited response rate despite several reminders and thus reduces the generalizability of our survey´ findings. Additionally, due to the significant level of heterogeneity, we were unable to do meta-analyses. The interpretation of the results must therefore be made with caution.
Nevertheless, from the respondents, we noted that despite the high burden of CRDs in the continent [26], PR as a structured practice is still not well established as a popular treatment for CRDs in Africa. We found that outpatient (100%) PR program was offered by the respondents in the survey study with a median of six patients per program, attending for three days a week, for sixty minutes (one hour) per day over eight weeks. PR program offered to inpatient was shorter than outpatient program (six weeks) but more intense, four to seven days a week for sixty minutes. Although some of these findings might compare well with the international guidelines´ requirements, considering the paucity of data and the scarcity of equipment, we will recommend that throughout the development of new PR in Africa, instead of constructing de novo guidelines- or simple adopting other guidelines, combining local experiences, local evidence to adapt current international guidelines might support faster implementation of PR practice in the African region.
The systematic review found that programs take 10 to 30 minutes, 2 or 3 time per week for 6 to 8 weeks. The British Thoracic Society guideline on PR also recommended PR program 2 to 3 time per week for 6 to 12 weeks and is in line with current literature [27]. Moreover, endurance training was largely used with walking (100% of program in the survey) and in the review (four studies [12,15,18,25], out of seven reported in effectiveness studies) as it is suggested by the American thoracic society/European respiratory society statement (ATS/ERS) statement [6] and other professional societies [28]. Walking is easier to practice and cheap since it does not necessarily require sophisticated equipment (such bicycle ergometer, treadmill). In addition, walking is very important as daily life activity.
Furthermore, breathing exercise was among the most used component for PR practice in Africa and this was also reported in both inpatient and outpatient program in our survey. This type of exercise aims at modifying respiratory muscle recruitment and reduces dyspnoea in COPD patients [29]. However, its effect on dyspnoea, exercise capacity and wellbeing it is unclear despite the fact that some studies have reported positive short-term physiological effects of breathing exercises in COPD patients [29].
Unfortunately, despite its well-known importance as PR component [6] and evidence of effectiveness in COPD self-management skills [30], patient education was only used in 3 studies in this paper [15,18,19].
Frequently measured outcomes included 6MWT (100% for inpatient, 86% for outpatient of the survey and reported on three papers in the review [15,24,25]) which is the most established field walking test and is more used because it is low-cost, necessitates little equipment, it is suitable for evaluation in the community setting, and it is considered to be more reflective of daily living than laboratory-based treadmill or cycle ergometer tests [6]. The 6 MWT provides data on the patient's physical activity level which can be a better indicator of the patient's ability to perform daily activities [31]. Improvement in walking distance was effective and common as reported in several included studies across Africa for COPD [24,25], asthma [25] and post-tuberculosis [15] patients after PR according to ATS/ERS statement [6].
Lung function measurement was mostly evaluated with simple spirometry with bronchodilator response in inpatient (100%) and outpatient (86%) programs in the survey study. Though some studies reported statistically and clinically significant improvements in Forced Vital Capacity (FVC), Forced Expiratory Volume in 1 second (FEV1), FEV1/FVC ratio in patients with asthma, pulmonary tuberculosis and COPD in the review, it is known that a short-term improvement of lung function in COPD patients after a PR program is unexpected [32]. In accordance with the current opinion, reversing the progressive decline in lung function in COPD patients is unlikely [33].
All pulmonary rehabilitation programs have the same essential characteristics, but the resources available, the program setting, structure, staff and duration vary considerably from one health system to another[6]. Currently, clear evidence to assign the right patient, in the most necessary setting, for the necessary rehabilitative treatment, including medical and non-medical therapies tailored to the patient is lacking, there is also no consensus of experts around the world, especially because of all the differences in local situations [34]. It is therefore evident that PR program in Africa have to be adapted to the patients culture, habits and systems to make it more accessible to Africans.
Consequently, further studies on PR are warranted to accelerate the adaptation of guidelines in Africa while considering health system constraints especially during COVID-19 era. PR programs delivery was severely impacted by the coronavirus disease 19 (COVID-19) pandemic what prompted to review the methods of application of exercises [35]. As tele-rehabilitation becomes an interesting tool for PR in developed countries [35], in Africa it becomes crucial to find a program that would keep patients and caregivers safe. An inexpensive program would be ideal for Africans like dance which doesn´t require expensive device. Dance can be practiced with physical distance and even outdoor and could improve physical performance, function, mood and social engagement, and is a core aspect of societies and cultures globally [36]. It would be a good program for futures researches in the area of PR in Africa if combined to adapted patients educations practices.
Despite the relative presence of pulmonary rehabilitation in Africa, its practice is still limited across many countries with high disparities within countries. Considering, the high burden of chronic respiratory diseases in Africa, there is a necessity to conduct robust studies testing local practices (such as traditional dance) to help engineering adapted PR guidelines for easy implementation in poor resource settings where more chronic respiratory diseases are reported.
What is known about this topic
- Pulmonary rehabilitation increases the quality of life of patients with chronic respiratory disease;
- Pulmonary rehabilitation works in occidental settings but given the difference in resources and trained personnel in Africa, it is important to understand the existing evidence for pulmonary rehabilitation in the continent.
What this study adds
- Pulmonary rehabilitation is underutilized in North and Sub-Saharan Africa;
- Pulmonary rehabilitation program varies in African countries but generally respects guideline of occidental societies which do not have same realities with African countries in general.
The authors declare that no competing interests.
Abbi-Monique Mamani Bilungula, Jean-Marie Kayembe Ntumba and Rik Gosselink were responsible for the design; Abbi-Monique Mamani Bilungula and Patrick Katoto acquired the data; Abbi-Monique Mamani Bilungula, Patrick Katoto, Jean-Marie Kayembe Ntumba, Rik Gosselink and Daniel Langer analysed the data; Abbi-Monique Mamani Bilungula wrote the first draft. All the authors read and approved the final manuscript of the manuscript.
Abbi-Monique Bilungula is a fellow of the Alumni of the Katholieke Universiteit of Leuven (KUL).
Table 1: summary of observational studies assessing pulmonary rehabilitation in Africa
Table 2: effectiveness of pulmonary rehabilitation in Africa
Table 2 (suite): effectiveness of pulmonary rehabilitation in Africa
Table 2 (suite1): effectiveness of pulmonary rehabilitation in Africa
Table 3: components of pulmonary rehabilitation program in included effectiveness studies
Figure 1: study flow chart
Figure 2: (A,B) quality of randomized controlled studies using the Cochrane risk of bias tool
Annex 1: quality of observational studies Assessing Pulmonary Rehabilitation in Africa using the Newcastle Ottawa scale
Annex 2: program characteristics, components, follow-up, and category of health care workers involved in pulmonary rehabilitation in Africa
Annex 3: reported outcome measurements at the start and the End of the Program
- Aït-Khaled N, Enarson D, Bousquet J. Chronic respiratory diseases in developing countries: the burden and strategies for prevention and management. Bull World Health Organ 2001;79(10):971-9. PubMed| Google Scholar
- Klionsky DJ, Abdelmohsen K, Abe A, Abedin MJ, Abeliovich H, Acevedo Arozena A et al. Guidelines for the use and interpretation of assays for monitoring autophagy (3rd edition ). Autophagy 2016;12:1-222. PubMed | Google Scholar
- Meghji J, Nadeau G, Davis KJ, Wang D, Nyirenda MJ, Gordon SB et al. Noncommunicable lung disease in sub-Saharan Africa a community-based cross-sectional study of adults in urban Malawi. Am J Respir Crit Care Med. 2016;194(1):67-76. PubMed | Google Scholar
- Adeloye D, Basquill C, Papana A, Chan KY, Rudan I, Campbell H. An estimate of the prevalence of COPD in Africa: a systematic analysis. J Chronic Obstr Pulm Dis 2015;12:71-81. PubMed | Google Scholar
- Celli BR, Macnee W, ATS/ERS Task Force. Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS / ERS position paper. Eur Respir J. 2004;23(6):932-46. PubMed | Google Scholar
- Spruit MA, Singh SJ, Garvey C, Richard ZuWallack, Linda Nici, Carolyn Rochester et al. An official American thoracic society/European respiratory society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med. 2013;188(8):13-64. PubMed | Google Scholar
- Rochester CL, Vogiatzis I, Holland AE, Suzanne Lareau, Darcy Marciniuk, Milo Puhan et al. An official American Thoracic Society/European Respiratory Society policy statement: enhancing implementation, use, and delivery of pulmonary rehabilitation. Am J Respir Crit Care Med. 2015;192:1373-86. PubMed | Google Scholar
- Varadi RG, Goldstein RS. Pulmonary rehabilitation for restrictive lung diseases. Chest. 2010;137(2):247-8. PubMed | Google Scholar
- Abdool-Gaffar MS, Ambaram A, Ainslie GM, Bolliger CT, Feldman C, Geffen I et al. Guideline for the management of chronic obstructive pulmonary disease 2011 update. South African Med J. 2011;101(1 Pt 2):63-73. PubMed | Google Scholar
- Liberati A, Altman DG, Tetzlaff J, Cynthia Mulrow, Peter C G�tzsche, John P A Ioannidis et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. PubMed | Google Scholar
- Brooks D, Sottana R, Bell B, Hanna M, Laframboise L, Selvanayagarajah S et al. Characterization of pulmonary rehabilitation programs in Canada in 2005. Can Respir J. 2007;14:87-92. PubMed | Google Scholar
- Shaw BS, Shaw I. Pulmonary function and abdominal and thoracic kinematic changes following aerobic and inspiratory resistive diaphragmatic breathing training in asthmatics. Lung. 2011;189(2):131-9. PubMed | Google Scholar
- Morrow B, Brink J, Grace S, Lisa Pritchard, Alison Lupton-Smith et al. The effect of positioning and diaphragmatic breathing exercises on respiratory muscle activity in people with chronic obstructive pulmonary disease. South African J Physiother. 2016;72(5):1-6. PubMed | Google Scholar
- Clarke H, Voss M. The role of a multidisciplinary student team in the community management of chronic obstructive pulmonary disease. Prim Heal Care Res Dev. 2016;17(4):415-20. PubMed | Google Scholar
- de Grass D, Manie S, Amosun SL. Effectiveness of a home-based pulmonary rehabilitation programme in pulmonary function and health related quality of life for patients with pulmonary tuberculosis: a pilot study. Afr Health Sci. 2014;14(4):866-72. PubMed | Google Scholar
- Jones R, Kirenga BJ, Katagira W, Singh SJ, Pooler J, Okwera A et al. A pre-post intervention study of pulmonary rehabilitation for adults with post-tuberculosis lung disease in Uganda. Int J COPD. 2017;12:3533-9. PubMed | Google Scholar
- Jones R, Kirenga BJ, Katagira W, Singh SJ, Pooler J, Okwera A. Does pulmonary rehabilitation alter patients´ experiences of living with chronic respiratory disease: a qualitative study. Int J COPD. 2018;13:2375-85. PubMed | Google Scholar
- Aweto HA, Akodu A, Adedara A, HA Aweto, OA Olawale. A comparative study of the effects of aerobic and resisted exercises on selected cardiopulmonary parameters in patients with asthma. African J Physiother Rehabil Sci. 2015;7:1-2. PubMed | Google Scholar
- Aweto HA, Aiyegbusi AI, Ugonabo AJ, Adeyemo TA. Effects of aerobic exercise on the pulmonary functions, respiratory symptoms and psychological status of people living with HIV. J Res Health Sci. 2016;16(1):17-21. PubMed | Google Scholar
- Tadyanemhandu C, Manie S. Profile of patients and physiotherapy patterns in intensive care units in public hospitals in Zimbabwe: a descriptive cross-sectional study. BMC Anesthesiol. 2015;15:136. PubMed | Google Scholar
- Tadyanemhandu C, Mupanda C, Dambi J, Chiwaridzo M, Chikwasha V, Chengetanai S. Human immunodeficiency virus associated pulmonary conditions leading to hospital admission and the pulmonary rehabilitation services received by patients at two central hospitals in Harare. BMC Res Notes.11(1):407. PubMed | Google Scholar
- Kpadonou TG, Mehinto D, Alagnide E et al. Rééducation des patients ayant subi une laparotomie en milieu hospitalier universitaire à Cotonou. Rev Pneumol Trop. 2011;16:9-14.
- Tyson AF, Kendig CE, Mabedi C, Bruce A Cairns, Anthony Charles. The effect of incentive spirometry on postoperative pulmonary function following laparotomy a randomized clinical trial. JAMA Surg. 2015;150(3):229-36. PubMed | Google Scholar
- Shamakh M, Badr N, El-Batanouny M, Mohamed Shamakh, Nagwa Badr, Mohamed El-Batanouny, Mohamed Shendy.Acapella versus hand-held positive expiratory pressure on Pulmonary functions in management of chronic obstructive Pulmonary diseases. J Adv Pharm Educ Res. 2020;10(2):27-34. Google Scholar
- Muzembo JN, Nkakudulu HB, Frans A. La réadaptation respiratoire de patients atteints d´asthme bronchique et de broncho-pneumopathies obstructives chroniques (BPCO) à Kinshasa. Rev Pneumol Clin. 2001;57(3):209-18. PubMed | Google Scholar
- Ahmed R, Robinson R, Mortimer K. The epidemiology of noncommunicable respiratory disease in sub-Saharan Africa, the Middle East, and North Africa. Malawi Med J. 2017;29:203-11. PubMed | Google Scholar
- Bolton CE, Bevan-Smith EF, Blakey JD, Crowe P, Elkin SL, Garrod R et al. British thoracic Society guideline on pulmonary rehabilitation in adults. Thorax. 2013;68(Suppl 2):ii1-30. PubMed | Google Scholar
- Morgan MDL, Calverley PMA, Clark CJ, Davidson AC, Garrod R, Goldman JM et al. British thoracic society standards of care subcommittee on pulmonary rehabilitation. Thorax. 2001;56(11):827-34. PubMed | Google Scholar
- Holland AE, Hill CJ, Jones AY, McDonald CF. Breathing exercises for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2012;10:CD008250. PubMed | Google Scholar
- Ibrahim RA, Abd El-Maksoud MM. Effect of educational programs on knowledge and self-management of patients with chronic obstructive pulmonary disease. Egypsian Nurs J. 2018;15:246-57. Google Scholar
- Crapo RO, Casaburi R, Coates AL. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002 Jul 1;166(1):111-7. PubMed | Google Scholar
- Topalovic M, Helsen T, Troosters T, Janssens W. Unexpected improvements of lung function in chronic obstructive pulmonary disease. Respir Med Case Reports. 2016;18:81-4. PubMed | Google Scholar
- Incorvaia C, Riario-sforza G, Ridolo E. About the effect of pulmonary rehabilitation on lung function in patients with chronic obstructive pulmonary disease. Respir Med Case Report.s 2016;19:53. PubMed | Google Scholar
- Spruit MA, Wouters EFM. Organizational aspects of pulmonary rehabilitation in chronic respiratory diseases. Off J Asian Pacific Soc Respirol. 2019;24(9):838-43. PubMed | Google Scholar
- Tsutsui M, Gerayeli F, Sin DD. Pulmonary rehabilitation in a post-COVID-19 world: telerehabilitation as a new standard in patients with copd. Int J COPD. 2021;16:379-91. PubMed | Google Scholar
- Philip KEJ, Lewis A, Williams S, Buttery SC, Polkey MI, Man W et al. Dance for people with chronic respiratory disease?: a qualitative study. BMJ Open Respir Res. 2020;10(10):e038719. PubMed | Google Scholar