Ocular Mpox in Southern Nigeria during the 2022/2024 outbreak: a report of two cases
Chizaram Anselm Onyeaghala, Nneka Marian Chika-Igwenyi
Corresponding author: Chizaram Anselm Onyeaghala, Department of Internal Medicine, University of Port Harcourt Teaching Hospital, Port Harcourt, Nigeria 
Received: 29 Jun 2025 - Accepted: 28 Sep 2025 - Published: 16 Apr 2026
Domain: Public health emergencies,Infectious disease
Keywords: Mpox, ocular mpox, ophthalmic manifestations, surveillance, Nigeria
Funding: This work received no specific grant from any funding agency in the public, commercial, or non-profit sectors.
©Chizaram Anselm Onyeaghala et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Chizaram Anselm Onyeaghala et al. Ocular Mpox in Southern Nigeria during the 2022/2024 outbreak: a report of two cases. Pan African Medical Journal. 2026;53:162. [doi: 10.11604/pamj.2026.53.162.48485]
Available online at: https://www.panafrican-med-journal.com//content/article/53/162/full
Images in clinical medicine 
Ocular Mpox in Southern Nigeria during the 2022/2024 outbreak: a report of two cases
Ocular Mpox in Southern Nigeria during the 2022/2024 outbreak: a report of two cases
&Corresponding author
There are significant knowledge gaps regarding the burden and clinical progression of ocular manifestations of mpox in Nigeria and worldwide. Here, we report two laboratory-confirmed mpox cases in young male adults with different presentations of ocular mpox at two tertiary hospitals in southern Nigeria during the 2022/2024 global outbreak. The first patient, a 28-year-old man, presented at the Alex Ekwueme Federal University Teaching Hospital in Abakaliki with a vesiculopustular rash on his nasal bridge and right lower eyelid, along with redness, pain, and itching. He later developed corneal ulcers and vision problems during follow-up after discharge. The second case involved a 44-year-old man with advanced, treatment-naive HIV infection. He presented with widespread vesiculo-pustular skin eruptions, including characteristic rashes around the periorbital and orbital areas. His condition rapidly worsened, leading to his death after seven days of hospitalisation. Consistent with guidance from the Nigeria Center for Disease Control and Prevention, lesional skin swabs from both patients were sent to the National Reference Laboratory in Abuja for quantitative polymerase chain reaction (qPCR), which tested positive for the monkeypox virus. Supportive care included antibiotics, fluids, nutritional support, and skin care, as no specific mpox treatments were available at that time. A multidisciplinary team, without an ophthalmologist, managed the care. Ocular mpox has been increasingly reported since the 2022 global outbreak. Continued surveillance and research are vital for monitoring mpox's evolving epidemiology, understanding eye-related diseases and potential complications, and improving prevention and treatment strategies for both systemic and ocular symptoms to prevent severe vision loss and enhance overall patient outcomes.
Mpox (formerly known as monkeypox) is an emerging viral zoonotic disease caused by the monkeypox virus (MPXV). This double-stranded DNA virus belongs to the genus Orthopoxvirus and the family Poxviridae. MPXV has two genetically distinct clades: Clade I and Clade II, with Clade II historically associated with a lower fatality rate than infections of Clade I. Before the 2022 global outbreak, mpox was mainly limited to Central and Western Africa, where it had been overlooked for decades. Clade I was found in Central Africa, while Clade II was common in Western Africa [1]. Mpox typically begins with an initial prodromal phase, characterised by fever, lymphadenopathy, myalgia, fatigue, and headache. This is followed by vesiculopustular skin eruptions that start on the face and spread outward in a centrifugal pattern, typically occurring 2 to 3 days after the initial onset of symptoms [2]. The incubation period of MPXV generally ranges from 5 to 21 days, depending on the infecting Clade of the virus, the host's immune status, and the transmission route [3]. Most patients with mpox recover within 2 to 4 weeks after skin eruptions appear, either spontaneously or with supportive care. However, severe illness with complications such as pneumonia, encephalitis, sepsis, secondary bacterial infections, and death can occur in the elderly, children, pregnant women, and individuals with chickenpox coinfection [4], as well as in those with weakened immune systems [5], if not properly managed.
There are notable gaps in understanding regarding the clinical features, long-term effects, and treatment options for ocular mpox. Most information about its symptoms and signs comes from case reports, and further research is needed. The 2022 global outbreak may suggest changes in the frequency and patterns of ocular mpox, which has increasingly been identified as a complication. However, it remains poorly understood in endemic regions of mpox in Africa. The reported rate of eye-related symptoms ranges from 0.3% to 11% in Clade II mpox infections during the 2022 outbreak, which is significantly lower than the rates of 4.1% to 23.1% observed in Clade I mpox infections before 2022. During the 2017 mpox resurgence in Nigeria, caused by Clade IIb, the most common ocular feature was the characteristic rash in the periorbital and orbital areas. However, Clade I reports often list conjunctivitis as the most frequent eye issue, usually associated with more severe illness [6]. Serious eye complications such as corneal ulcers, perforations, or episcleritis have also been reported, sometimes resulting in substantial vision loss [7]. Given the ongoing increase in mpox cases in Africa, this study aimed to report two cases of laboratory-confirmed mpox with different ocular manifestations that were managed during the 2022/2024 outbreaks in southern Nigeria.
Case 1
Patient information: a 28-year-old male artisan presented to Alex Ekwueme Federal University Teaching Hospital in Abakaliki, Nigeria, with a seven-day history of high-grade fever, a generalised throbbing headache, sore throat, and body pain. Three days later, he developed a solitary vesicular rash on a hypertrophied scar on his left shoulder, which then spread to his scalp, face, trunk, and groin. Initially, the rash was itchy, but later became painful genital ulcers. About two days later, he noticed a similar rash on his lower eyelid, which became very painful, accompanied by redness and a decrease in vision. He was recently released from a correctional facility where he had close contact with inmates with similar lesions.
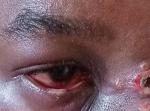
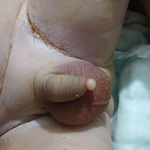
Clinical findings: during the general examination, he was febrile with a temperature of 38.2°C, not pale, anicteric, dehydrated, with right-sided conjunctival injection and enlarged cervical and inguinal lymph nodes. His pulse rate was 92 beats per minute, blood pressure was 110/70 mmHg, respiratory rate was 21 breaths per minute, and oxygen saturation was 98% on room air. Skin examination revealed generalised vesiculo-pustular skin lesions. Gross eye examination showed bilateral red conjunctivae (Figure 1). Other systemic examination was unremarkable.
Diagnostic assessment: a skin swab and crust specimen submitted for quantitative PCR at the National Reference Laboratory of the Nigeria Centre for Disease Control and Prevention tested positive for monkeypox virus. The HIV screening test was negative.
Therapeutic interventions: he was admitted to the isolation ward and received supportive care, including fluid management with normal saline, empirical broad-spectrum antibiotics (IV ceftriaxone and azithromycin), intravenous valacyclovir, and antipyretics.
Follow-up and outcomes of interventions: the patient was discharged after a 10-day hospital stay once the rash resolved. During follow-up, he developed a corneal ulcer with worsening vision, which required a referral to the ophthalmology department for further specialised care. Patient perspective: He was grateful for the care and treatment he received for his illness.
Informed consent: consent was obtained for this publication.
Case 2
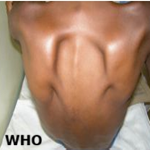
Patient information: a 44-year-old male security officer presented to the University of Port Harcourt Teaching Hospital in Port Harcourt with a 9-day history of fever and widespread skin rashes. The skin lesions were first noted on the genitals and rapidly spread to the limbs, trunk, scalp, and face, including the upper and lower eyelids of both eyes. Over a short period, the lesions became painful and necrotising, and the patient reported decreased vision in both eyes. There was a history of unprotected sexual intercourse with an acquaintance about 10 days before the first lesions appeared.
Clinical findings: during physical examination, he appeared acutely ill, febrile, dehydrated, with enlarged axillary lymph nodes and generalised body swelling. Vital signs indicated an axillary temperature of 38.9°C, a pulse rate of 110 beats per minute, a blood pressure of 90/60 mmHg, a respiratory rate of 36 breaths per minute, and an oxygen saturation of 86% on room air. Skin examination showed widespread necrotising skin lesions involving both eyes. He was conscious but lethargic, with crepitations heard in both lung fields on auscultation and vague abdominal tenderness.
Diagnostic assessment: skin samples were sent to the National Reference Laboratory of the Nigerian Centre for Disease Control and Prevention and tested positive for both monkeypox virus and varicella-zoster virus. HIV-1 and HIV-2 screening was positive, with a CD4 count of less than 200 cells/mm³.
Therapeutic interventions: he was admitted to the infectious diseases treatment center and began on broad-spectrum intravenous antibiotics (ceftriaxone and metronidazole), received fluid management with normal saline, oxygen therapy, intravenous acyclovir, antiretroviral therapy (tenofovir disoproxil fumarate, lamivudine, and dolutegravir), antipyretics (paracetamol), nutritional support, and skin care.
Follow-up and outcomes of interventions: the patient gradually deteriorated and ultimately died after 7 days in the hospital.
Informed consent: the wife provided consent for this publication.
Ocular mpox has emerged as an increasingly common yet underreported complication of mpox infection. This paper describes two cases of ocular manifestations of mpox in young adult males managed at two tertiary hospitals in southern Nigeria during the 2022/2024 outbreak, emphasising the importance of early ophthalmic intervention in mpox case management to prevent sight-threatening complications of severe mpox.
The spectrum of ocular signs associated with mpox ranges from mild symptoms, including blepharitis, conjunctivitis, focal conjunctival lesions, photophobia, and early-diagnosed keratitis, to more serious complications, such as corneal scarring and vision loss in later stages [7]. This aligns with the diverse eye-related signs observed in our two patients; the first case had conjunctivitis, while the second developed distinctive rashes on the periorbital and orbital regions. In a retrospective study conducted by Ogoina and colleagues from September 2017 to December 2018, 25% of hospitalised patients with mpox in Nigeria presented with rashes near the eyes, indicating that vesiculo-pustular rashes in the periorbital and orbital areas may be the most common presentation of ocular mpox in Nigeria [6]. However, conjunctivitis is the most reported eye problem in studies from regions affected by Clade I mpox, and it has been linked to more severe disease progression.
Although mild and early complications are usually associated with visual and symptom recovery, our first case, who had conjunctivitis, developed a corneal ulcer and impaired vision due to a lack of early ophthalmic review during the hospital stay. This highlights the increasing importance of prompt referral to or invitation of ophthalmologists for patients with ocular mpox to prevent vision loss. The reported prevalence of ophthalmic manifestations during the 2022 multi-country outbreak is lower compared to earlier reports from the endemic DRC, ranging from 0.3% to 11% in Clade II mpox infections, versus 4.1% to 23.1% in Clade I mpox infections [1,7]. This variation may be due to differences in Clade type, underdiagnosis and underreporting by clinicians, host immune responses, and modes of transmission, as the epidemiology and risk factors associated with the clade II outbreak differ from previous outbreaks [8].
The exact cause of ocular symptoms in patients with mpox remains unclear, whether it results from systemic spread of the virus during the early viraemic phase or from self-inoculation into the eyes. Additionally, emerging data suggest that MPXV genomes can persist in both external and internal ocular fluids, though the significance of this finding remains uncertain. While it is proposed that MPXV may enter conjunctival secretions through the plasma compartment, the fact that skin lesions often appear before ocular symptoms indicates that self-inoculation may be the primary cause. Therefore, healthcare professionals should implement preventive measures to protect patients' eyes during acute mpox infection, such as advising patients on proper infection prevention strategies like hand hygiene and avoiding contact with their eyes.
Ocular mpox should be considered in any patient with recent or past skin lesions indicative of mpox or laboratory-confirmed mpox presenting with new eye symptoms. These symptoms are more common in unvaccinated individuals, consistent with our patients who neither received the smallpox vaccine nor the MVA-BN mpox vaccine, which was unavailable in Nigeria during the 2022 global outbreak. This highlights the importance of deploying mpox vaccines in high-risk groups, including those with advanced HIV infection, like our second patient, to prevent illness and death. In addition to diagnosing and treating ocular mpox, patients should also be assessed for secondary bacterial (Staphylococcus aureus, Pseudomonas aeruginosa, syphilis), viral (herpes simplex virus, varicella-zoster virus), or fungal (Aspergillus spp.) co-infections, which may complicate or mimic ocular mpox [9].
Managing ocular mpox requires collaboration between infectious disease specialists and ophthalmologists, who will perform a thorough evaluation of the affected ocular structures (e.g., cornea, conjunctiva, intraocular involvement) and ongoing monitoring of the patient's condition and disease extent, especially in cases with vision changes, eye pain, or increasing redness. Although there is no definitive or established treatment for ocular mpox, oral tecovirimat (Tpoxx), a systemic antiviral medication, has been used despite the lack of pharmacokinetic data on its penetration into surface or deeper eye structures. Emerging evidence from the PALM 007 and STOMP trials indicated that Tpoxx did not improve outcomes. Additionally, simple therapies such as regular and enhanced lubrication, trifluridine eye drops, vitamins, other antivirals, and prophylactic topical antibiotics may be considered [10]. Topical or oral antibiotics are often used together, either to treat bacterial superinfection or as prophylaxis. The use of topical corticosteroids to control ocular inflammation could unintentionally worsen disease progression by contributing to virus persistence when the corneal epithelium is compromised [10].
Ocular disease has become an increasingly reported manifestation of mpox in Nigeria since the 2022 global outbreak. Ongoing surveillance and research are vital for tracking the evolving epidemiology of mpox, understanding eye-related complications, and improving prevention and treatment of both systemic and ocular issues to prevent significant vision loss and improve overall patient outcomes. Ophthalmologists should be included in the multidisciplinary team of specialists caring for mpox patients with ocular manifestations.
The authors declare no competing interests.
Chizaram Anselm Onyeaghala conceptualised and wrote the initial draft. Nneka Chika-Igwenyi wrote the report for the first case. All authors read and agreed to the final manuscript.
Figure 1: an ocular Mpox patient showing unilateral conjunctivitis with blepharitis
- Beer EM, Rao VB. A systematic review of the epidemiology of human monkeypox outbreaks and implications for outbreak strategy. PLoS Negl Trop Dis. 2019 Oct;13(10):e000779. PubMed | Google Scholar
- Begley J, Kaftan T, Song H, Fashina T, Hartley CD, Nguyen N et al. Ocular Complications of Mpox: Evolving Understanding and Future Directions. International Ophthalmology Clinics. 2024 Fall;64(4):15. PubMed | Google Scholar
- Miura F, van Ewijk CE, Backer JA, Xiridou M, Franz E, Op de Coul E et al. Estimated incubation period for monkeypox cases confirmed in the Netherlands, May 2022. Euro Surveill. 2022 Jun;27(24):2200448. PubMed | Google Scholar
- Mmerem JI, Umenzekwe CC, Johnson SM, Onukak AE, Chika-Igwenyi NM, Chukwu SK et al. Mpox and Chickenpox Coinfection: Case Series From Southern Nigeria. J Infect Dis. 2024 Mar 26;229(Supplement_2):S260-. PubMed | Google Scholar
- Mitjà O, Alemany A, Marks M, Mora JIL, Rodríguez-Aldama JC, Silva MST et al. Mpox in people with advanced HIV infection: a global case series. The Lancet. 2023 Mar 18;401(10380):939-49. PubMed | Google Scholar
- Ogoina D, Iroezindu M, James HI, Oladokun R, Yinka-Ogunleye A, Wakama P et al. Clinical Course and Outcome of Human Monkeypox in Nigeria. Clin Infect Dis. 2020 Nov 5;71(8):e210-4. PubMed | Google Scholar
- Hughes C, McCollum A, Pukuta E, Karhemere S, Nguete B, Lushima RS et al. Ocular complications associated with acute monkeypox virus infection, DRC. International Journal of Infectious Diseases. 2014 Apr 1;21:276-7. Google Scholar
- Bragazzi NL, Kong JD, Mahroum N, Tsigalou C, Khamisy-Farah R, Converti M, Wu J. Epidemiological trends and clinical features of the ongoing monkeypox epidemic: A preliminary pooled data analysis and literature review. J Med Virol. 2023 Jan;95(1):e27931. PubMed | Google Scholar
- Bhamray-Sanchez D, Subramanian S, Dever LL, Chew D. Ocular MPox: A report of two cases. IDCases. 2023;31:e01706. PubMed | Google Scholar
- Reynolds MG, McCollum AM, Nguete B, Shongo Lushima R, Petersen BW. Improving the Care and Treatment of Monkeypox Patients in Low-Resource Settings: Applying Evidence from Contemporary Biomedical and Smallpox Biodefense Research. Viruses. 2017; 9(12):380. PubMed | Google Scholar