A scoping review on research agendas to enhance prevention of epidemics and pandemics in Africa
Jill Ryan, Alison Wiyeh, Humphrey Karamagi, Joseph Okeibunor, Prosper Tumusiime, Charles Shey Wiysonge
Corresponding author: Jill Ryan, Cochrane South Africa, South African Medical Research Council, Cape Town, South Africa 
Received: 12 May 2020 - Accepted: 15 May 2020 - Published: 24 Nov 2020
Domain: Epidemiology,Health system development
Keywords: Research agenda, pandemic, epidemic, prevention, Africa
This article is published as part of the supplement PAMJ Special issue on COVID 19 in Africa (Volume 2), commissioned by The Pan African Medical Journal.
©Jill Ryan et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Jill Ryan et al. A scoping review on research agendas to enhance prevention of epidemics and pandemics in Africa. Pan African Medical Journal. 2020;37(1):40. [doi: 10.11604/pamj.supp.2020.37.1.23458]
Available online at: https://www.panafrican-med-journal.com//content/series/37/1/40/full
Research 
A scoping review on research agendas to enhance prevention of epidemics and pandemics in Africa
A scoping review on research agendas to enhance prevention of epidemics and pandemics in Africa
![]() Jill Ryan1,&, Alison Wiyeh1,2, Humphrey Karamagi3, Joseph Okeibunor3, Prosper Tumusiime3, Charles Shey Wiysonge1,4,5
Jill Ryan1,&, Alison Wiyeh1,2, Humphrey Karamagi3, Joseph Okeibunor3, Prosper Tumusiime3, Charles Shey Wiysonge1,4,5
&Corresponding author
Introduction: research is not only needed to prioritise the best possible response during an epidemic and pandemic, it is also understood to be a core pillar of outbreak response. However, few African countries are equipped to perform the needed surveillance and research activities during an outbreak. Therefore, we mapped out research agendas aimed at increased research preparedness towards epidemics or pandemics in Africa.
Methods: eligible studies were searched for in in PubMed, Scopus, and Google Scholar. Additionally, grey literature was sought in Google, citation searches, as well as targeted sites such as the World Health Organization (WHO), Africa Centres for Disease Control and Prevention, African Union, and the Wellcome Trust. Searches were done in March 2020.
Results: the electronic searches yielded 7344 records, of which 34 articles were included in the study. The studies identified around 18 factors highlighted through various research agendas. Majority of the research agendas spoke to general epidemic preparedness and focused largely on understanding virus transmission such as its characteristics and dynamics, and the infrastructure needed to carry out vital research activities.
Conclusion: the review highlights the research needs in order to carry out vital research work but to also bridge knowledge gaps and harmonize outbreak response from key stakeholders. However, Africa needs to create its own health research agendas and capacitate itself to conduct and lead these studies. African health research decisions must center on Africa, with African researchers taking the lead not only on the science produced but ensuring inclusive and equitable involvement from fellow researchers, and in engaging national health ministries as well as the communities.
Conducting valuable research during pandemics and epidemics is not only needed to prioritize the best possible response but is also acknowledged as a core pillar of outbreak response [1]. During recent public health crises, such as the 2009 H1N1 influenza pandemic, government leaders needed to make decisions at a time where information was limited and highly uncertain [2]. Effective processes were needed between stakeholders to facilitate the utilization of scientific information to assess each scenario, and ultimately identify interventions offering the most beneficial outcomes [2]. However, with emerging and re-emerging infections such as Ebola, Zika, Influenza, and the subsets of coronavirus, there are challenges regarding rapid research output or to rapidly undertake intervention trials to inform practice and patient care [1,3]. These challenges are linked to the unpredictable nature of the virus, as well as its time and location of onset [1,3]. Thus, the need for scientific and research preparedness is unquestionable in its necessity when prioritizing effective outbreak responses [1,2].
The World Health Organization (WHO) has indicated its awareness regarding the need for such preparedness, and in a 2018 document on managing epidemics, they mention their global strategy and preparedness plan highlighted as their research and development blueprint [4]. The strategies highlighted in this document will aim to allow rapid activation of research and development activities which will fast-track the availability of effective diagnostic tests and treatment, averting large scale crises [4,5]. However, when epidemics overlap and occur at the same time, the challenge is creating an efficient global response to increase multiple public health emergencies. Such a response requires integration from health, economic and global systems to prepare for said epidemics or outbreaks [6]. This proves difficult when not all countries are equipped to carry out these research activities and required surveillance, as is the case in many low- and middle-income settings in the African continent.
Outbreaks in Africa have shown time and time again, to be a cause of global concern [7]. Out of the 55 African countries, only 15 currently have institutions equipped to perform the functions of an effective National Public Health Institution (NPHI) which includes disease surveillance of diagnostic laboratories, capacity to activate response teams for outbreaks, as well as being operation centres for public health crises [7]. Equipping African NPHIs is vital for health security [7,8]. With Africa´s 1.2 billion population expected to expand to 2.4 billion by 2050, this rapidly expanding population means greater urbanization but also increased informal settlements; where, already half of urban areas do not have access to sanitation, and even less have access to scheduled childhood vaccinations [7]. Furthermore, rapid population increase, and urbanization also means increased risk for outbreaks and limited response to address it. This is due primarily to Africa´s incapacity to swiftly and effectively manage these emergencies [7,8]. The Africa Centres for Disease Control and Prevention (Africa CDC) estimates that Africa requires 2-3.5 billion US dollars per year to be adequately capitated for epidemic preparedness, yet only receives $700 million [7]. In this scoping review, research agendas aimed at increasing research preparedness toward epidemics or pandemics, which may facilitate and streamline effective response for emerging and re-emerging disease outbreak were mapped.
A scoping review maps the existing literature on a given topic and identifies key concepts and gaps in the existing research on that topic. In this scoping review we followed the methods proposed by Levac et al. [9] and enhanced by Peters et al. [10]. We have used the preferred reporting items for systematic reviews and meta-analysis - extension for Scoping reviews (PRISMA-ScR) checklist to shape structure and content [11].
Eligibility criteria: the inclusion criteria are structured according to the components suggested in Peters et al. [10]. Inclusion criteria were broken down into the following elements: participants, concepts, and context.
Participants: African “think tank” organizations: African Union, WHO, United Nations (UN), United Nations Children Fund (UNICEF), and universities, focusing research on Africa.
Concepts
Research agendas: research strategies which facilitate preparedness.
Epidemic: “a disease (infectious and noninfectious) that affects a large number of people, with a recent and substantial increase in the number of cases” [12].
Pandemic: an outbreak with characteristics which include wide geographic expansion, disease movement which can be traced from place to place, has high attack rates and explosiveness (multiple cases within short space of time); minimal population immunity; novelty (new or new variants of pathogen); it is infectious as well as severe [13].
Context: within Africa; no specificity related to cultural factors, racial or sex-based factor, setting such as a health facility or school or discipline.
Search strategy: one author (JR) conducted a search of PubMed, Scopus, and Google Scholar in March 2020. She also searched grey literature such as technical reports, research reports, committee meeting reports, conference proceedings, abstracts, and dissertations on websites identified to relate to research agendas and outbreaks in Africa. Grey literature from relevant organization sites were hand searched and snowballing technique used when going through relevant documents found. Grey literature sites included WHO, Africa CDC, African Union, and the Wellcome Trust. Literature published within a 10-year time span from date of this current review (2010 - 2020) to elicit latest trends addressing recent response outbreak needs. Keywords used for index search were "research", "outbreak preparedness", "research priorities", "epidemic response", "pandemic response", "real-time research", and "Africa". Furthermore, the search term 'Africa' was further expanded to include all African countries through a search strategy filter created by Pienaar and colleagues [14]. The search strategy for PubMed is shown in Table 1. In addition to searching organization websites for relevant documents, not all of the organization documents presented in the website search, and as such documents, for example from WHO, were also searched for through Google.
Google was also used to search for additional grey literature, while searching for missing WHO documents. As noted in a paper by Godin et al. [15], Google can be overwhelming owing to the immense information available and inconsistent website organization. For this reason, Godin and colleagues further stated that it is impossible to screen all retrieved results and as such one must rely on the power of the relevancy ranking within the Google search engines, which is to bring out the most relevant results to the top of the list [15]. The relevancy list generated by Google, is presented in a set number of pages to be screened in advance, ensuring consistency and time management and thus narrowing the search results to specific subject area allowing refined and targeted searching [15]. The first 10 pages of hits were screened (100 results), through title screen and the short text beneath the title, similar to the method used in Godin et al. [15]. The review strategy had been shaped using the PRESS (Peer Review of Electronic Search Strategies) 2015 guideline statement, which allowed the discovery of search errors and offers enhancements to the selection of subject headings and text words, resulting in additional studies [16].
Study selection: selection criteria was based on the specifics of the research question and later refined with new familiarity on the subject matter through reading the studies. Clarity in decision-making of selection criteria was clarified using the following steps: i) Initial team meetings were conducted every week to discuss inclusion and exclusion criteria. ii) More than one authors was used to clarify situations of disagreement to determine final inclusion. iii) Meetings between two authors (JR and CSW) were held at the beginning, midpoint and final stages of the abstract review process discussing challenges and uncertainties related to study selection and to go back and refine the search strategy if needed.
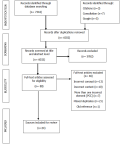
Extraction and charting the results: results were extracted and narratively described contextual or process-oriented information from each document, accompanied by a flow chart to show search decision and final selection (Figure 1). Firstly, the data extraction sheet in tabular form summarized each study according to: 1) author(s), 2) year of publication, 3) country of focus, and 9 key messages that relate to the review question. Furthermore, the extracted data has been translated into a logical and descriptive summary of the results linked to addressing the review question. As such the results have been presented below through a narrative synthesis.
Selection of sources of evidence: we found a collective 7344 publications from the database search, and an additional 15 documents from other means described in Figure 1. After duplicate removal, 6032 records were screened at title and abstract level, resulting in the exclusion of 5952 records. The remaining 80 articles were assessed for eligibility. Of the 80 titles a further exclusion of 46 articles, with reasons, was undertaken, as shown in Figure 1. One of the reasons for exclusion involved missed duplicates, which can occur as false negatives (duplicates which were to be deleted but were not) in reference managers [17]. After these exclusions, 34 articles were included in the review [18-52].
Characteristics of sources of evidence: of the included documents, 22 were journal articles, 7 were research frameworks, 3 were reports, and 2 were commentaries. Majority of the articles assessed the relevance of current epidemic research agendas and its alignment to context and current research needs. Furthermore, the journal article records also aimed in establishing research priorities and in showing the process and tools used to create these priorities. Commentaries focused on having research sites and networks established and strengthened, which would streamline barrier resolutions, case definitions, protocols, and create rapid exchange mechanisms for high quality data and samples to reduce duplication. The frameworks and reports set out establishing research areas for preparedness and in highlighting the need for strengthening infrastructure to carry out the research in a safe and effective manner.
Synthesized results: Table 2, Table 3 and Table 4 highlights the key message of each document included in the study. Majority of the studies had focused their research agendas around understanding transmission and infrastructure. Studies which focused on transmission sought to understand the characterization, etiology, or pathogenesis of the disease so as to better identify the pathogen, how it may interplay with other disease (e.g. TB and diabetes or HIV associated TB), as well as to study disease interaction such as vector-virus interaction or if the pandemic goes from region to region, the impact this may have on the pathogen strain [18,30,34,45,48-51]. Infrastructure was seen as vital in many of the documents, which includes creating infrastructure to safely and efficiently carry out real-time research during epidemics, in a way where samples are kept in a safe manner and where cold chain is adequate [26,27,37,40,42-44,47]. Data sharing had been regarded to play an integral role during an epidemic especially to prevent duplication but also to create comparable data sets [21,25,27,36,41,50]. Five sources spoke explicitly on prevention as an important component, but to have contextual consideration when thinking prevention, for example, many forms of cancers which can be prevented, still have high rates in Africa [18,22,33,40,49]. Sensitivity to context had been expressed more in terms of interventions and its implementation, which includes contextualizing well-known or proven interventions which would be closely aligned to population-based information [18,26,46,52]. Treatment had been addressed in diverse ways, either through the inclusion of particular populations (men who have sex with men for appropriate HIV treatment options), to understand co-morbidity (HIV associated TB/TB associated diabetes) for integrated treatment options, to link treatment to understanding transmission, and lastly treatment studies to focus treatment for present-day and not future epidemics, which had been a strong assertion in the Ebola studies as a sentiment from community engagement [22,30,33,39,48].
Surveillance was discussed in four sources, which focused more on biosurveillance of animal or livestock infections or monitoring a disease in the disease hotspot (e.g. meningitis in the African meningitis belt) [26,30,38,48]. Four sources spoke to services, namely in terms of aligning services to relevant populations into studies, integrating services, and optimizing clinical management and public health practice [22,33,49,50]. Three studies stressed the importance in creating standards, either through data collection, protocol eligibility, sharing data, score cards for comparative studies, or robust research [21,32,50]. Vaccine development was mentioned in relation to health policies in that it could help influence which vaccines get prioritised, but also to have pathways to vaccine development streamlined for timeous response. Other vaccine development factors include ethical inclusion of pregnant women into studies and the validation of serological correlates [23,29,30,38]. Furthermore, improved diagnostics and therapeutics are needed for better preparedness especially more rapid, point of care diagnostics are needed [26,51,52]. Two studies addressed transparent reporting in the use of predictive modelling, by improving the models and clearly communicating its finding including uncertainty [21,26]. Streamlined processes had been emphasized by two studies specifically, in order to efficiently begin vaccine development, resolve barriers, create case definitions and guidelines, pre-approved protocols, create mechanisms of exchange for data sharing [23,24].
Two studies mentioned the importance in research looking at the long-term, socio-cultural and health impacts these diseases have on the community or country but also measuring the impact on certain populations (e.g. tobacco research focusing on girls than boys due to increased prevalence) [21,40]. Research participation also received mention but mainly in terms of the ethical inclusion of vulnerable groups such youth participation in HIV research or pregnant women in vaccine research [28,29]. Only one study focused specifically on research priorities reducing maternal mortality [20]. Case management had been touched on by two documents linking to case finding, patient care, and screening [22,49]. Lastly, vector control was mostly discussed in terms of Ebola and Zika, and it being combined with vaccine development for improved response [35,51].
This scoping review identified 34 documents deemed to be eligible for inclusion. Majority of the research agendas were derived from documents dealing with general epidemic or pandemic response [24,32,34,36,37,39,41-44,47,52], followed by research agendas drawing from lessons learned from the Ebola outbreak [25,27,31,35,50] which greatly informed response to the Zika outbreak which followed soon after [21,51]. General epidemic preparedness is needed as emerging and re-emerging diseases are increasing especially in developing countries [53]. This general framework equips health systems to have general preparedness as described by Fatiregun and colleagues [54] whereby epidemic management guides all activities from the national to health facility level, to adequately detect disease outbreaks, effectively respond to it by ensuring staff are well organized to investigate and thus effectively respond to disease outbreak.
Of the included studies, the broad manner in which transmission was addressed throughout the documents, illustrates the various levels at which one should understand the characteristics of the pathogen, and mechanisms of transmission in successful isolation and limiting of the disease spread [4]. Furthermore, understanding transmission falls part of early detection of which a new disease might mean new interventions [4]. This in turn links to infrastructure in building research capacity, which too was largely addressed by most of the documents, which would allow for mobilization and rapid deployment of and testing of candidate products within countries where outbreaks are most likely to occur [55]. An example of this lack of infrastructure goes back to the Ebola outbreaks, which delayed response in the form of vaccine and therapeutics ultimately resulting in a hindered outcome impact [55].
In having research agendas, we allow opportunities to bridge medium- and long-term knowledge gaps [56]. Yet in respect to epidemic research, research agendas create a harmonized response with key stakeholders. Epidemic research agendas allow high-quality research protocols and tools to be shared whilst inviting materials and samples from research partners in an ethical manner [56]. However, Africa needs to create its own health research agendas and capacitate itself to conduct and lead these studies, as the notion of 'safari science' whereby African scientists act as data gatherers for Western research agendas, is not an effective route any longer [57]. African health research decisions must center on Africa, with African researchers taking the lead not only on the science produced but ensuring inclusive and equitable involvement from fellow researchers, and in engaging national health ministries as well as the communities [57]. This engagement with community needs and contextualized interventions had been highlighted in four documents included in this study [18,26,46,52]. These may in turn further build sustainability and local commitment, which must transcend the need of funders or any project [57].
Limitations: this review, though attempting a highly sensitive search to capture as much eligible evidence as possible, may not have located all sources, especially when searching grey literature, in which some documents may be missed.
It is vital for Africa to take the lead on its health decisions as well as lead the science in Africa's epidemic response. However, to do this we must ensure we are capacitated to do so and have the infrastructure for secure and adequate response and mobilization of real-time research and deployment of vaccines or other therapeutic products.
What is known about this topic
- Research agendas are vital for a coordinated epidemic response;
- Low to middle income countries are limited in ability to carry out necessary outbreak surveillance and research activities.
What this study adds
- An overview of available research agendas focusing on African relevant outbreaks and opportunities for research preparedness.
- This study highlights the need for context relevant outbreak research agendas and the need for sufficient infrastructure to address them.
The authors declare no competing interests.
CSW conceived the study following a request from AFRO for a policy brief on the topic and JR wrote the first draft of the proposal and the review. JR, AW, HK, JO, PT, and CSW provided important intellectual input to the study. All the authors have read and agreed to the final manuscript.
The authors acknowledge the support received from the World Health Organization Regional Office for Africa (AFRO) and the South African Medical Research Council (SAMRC) during the conduct and reporting of this study.
Table 1: search strategy for PubMed
Table 2: summary of evidence for included studies addressing general epidemic research agendas
Table 3: summary of evidence for included studies addressing zoonotic epidemic research agendas
Table 4: summary of evidence for included studies addressing other specific epidemic research agendas
Figure 1: preferred reporting item for systematic reviews and meta-analysis flow diagram
- Sigfrid L, Moore C, Salam AP, Maayan N, Hamel C, Garritty C et al. A rapid research needs appraisal methodology to identify evidence gaps to inform clinical research priorities in response to outbreaks-results from the Lassa fever pilot. BMC medicine. 2019;17(1):107. PubMed | Google Scholar
- Lant T, Lurie N. Science preparedness and science response: perspectives on the dynamics of preparedness conference. J Public Health Manag Pract. 2013;19(Suppl 2):S3-5. PubMed | Google Scholar
- Rishu AH, Marinoff N, Julien L, Dumitrascu M, Marten N, Eggertson S et al. Time required to initiate outbreak and pandemic observational research. J Crit Care. 2017;40:7-10. PubMed | Google Scholar
- World Health Organization. Managing epidemics: key facts about major deadly diseases. Geneva; 2018. Google Scholar
- Mehand MS, Al-Shorbaji F, Millett P, Murgue B. The WHO R&D Blueprint: 2018 review of emerging infectious diseases requiring urgent research and development efforts. Antiviral res. 2018 Nov;159:63-67. PubMed | Google Scholar
- Bedford J, Farrar J, Ihekweazu C, Kang G, Koopmans M, Nkengasong J. A new twenty-first century science for effective epidemic response. Nature. 2019 Nov;575(7781):130-136. PubMed | Google Scholar
- Nkengasong JN. How Africa can quell the next disease outbreaks. Nature. 2019;567(7747):147. PubMed | Google Scholar
- Tomori O. Will Africa´s future epidemic ride on forgotten lessons from the ebola epidemic? BMC medicine. 2015 Dec;13(1):116. Google Scholar
- Levac D, Colquhoun H, O'Brien KK. Scoping studies: advancing the methodology. Implement sci. 2010 Dec 1;5(1):69. PubMed | Google Scholar
- Peters MD, Godfrey CM, Khalil H, McInerney P, Parker D, Soares CB. Guidance for conducting systematic scoping reviews. Int J Evid Based Healthc. 2015 Sep 1;13(3):141-6. PubMed | Google Scholar
- Tricco AC, Lillie E, Zarin W, O'Brien KK, Colquhoun H, Levac D et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann intern med. 2018;169(7):467-73. PubMed | Google Scholar
- Martin PM, Martin-Granel E. 2,500-year evolution of the term epidemic. Emerg Infect Dis. 2006;12(6):976-80. PubMed
- Morens DM, Folkers GK, Fauci AS. What is a pandemic? J Infect Dis. 2009;200(7):1018-1021. PubMed
- Pienaar E, Grobler L, Busgeeth K, Eisinga A, Siegfried N. Developing a geographic search filter to identify randomised controlled trials in Africa: finding the optimal balance between sensitivity and precision. Health Info Libr J. 2011;28(3):210-5. PubMed | Google Scholar
- Godin K, Stapleton J, Kirkpatrick SI, Hanning RM, Leatherdale ST. Applying systematic review search methods to the grey literature: a case study examining guidelines for school-based breakfast programs in Canada Syst rev. 2015;4(1):138. PubMed | Google Scholar
- McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C. PRESS peer review of electronic search strategies: 2015 guideline statement. J Clin Epidemiol. 2016;75:40-6. PubMed | Google Scholar
- Kwon Y, Lemieux M, McTavish J, Wathen N. Identifying and removing duplicate records from systematic review searches. J Med Libr Assoc. 2015 Oct;103(4):184-8. PubMed | Google Scholar
- Sylla BS, Wild CP. A million Africans a year dying from cancer by 2030: what can cancer research and control offer to the continent? Int J Cancer. 2012;130(2):245-50. PubMed | Google Scholar
- Gotch F, Gilmour J. Science, medicine and research in the developing world: a perspective. Nat Immunol. 2007;8(12):1273-1276. PubMed | Google Scholar
- Chapman E, Reveiz L, Sangalang S, Manu C, Bonfill X, Munoz S et al. A survey study identified global research priorities for decreasing maternal mortality. J Clin Epidemiol. 2014;67(3):314-24. PubMed | Google Scholar
- Kobres PY, Chretien JP, Johansson MA, Morgan JJ, Whung PY, Mukundan H et al. A systematic review and evaluation of Zika virus forecasting and prediction research during a public health emergency of international concern. PLOS Negl. Trop. Dis. 2019;13(10):e0007451. PubMed | Google Scholar
- Odone A, Matteelli A, Chiesa V, Cella P, Ferrari A, Pezzetti F et al. Assessing the impact of defining a global priority research agenda to address HIV-associated tuberculosis. Trop. Med Int Health. 2016;21(11):1420-7. PubMed | Google Scholar
- Gouglas D, Christodoulou M, Plotkin SA, Hatchett R. CEPI: driving progress towards epidemic preparedness and response. Epidemiol. Rev. 2019 Jan 31;41(1):28-33. PubMed | Google Scholar
- Zumla A, Ippolito G, McCloskey B, Bates M, Ansumana R, Heymann D et al. Enhancing preparedness for tackling new epidemic threats. Lancet Resp Med. 2017;5(8):606-8. PubMed | Google Scholar
- Rojek A, Horby P, Dunning J. Insights from clinical research completed during the west Africa ebola virus disease epidemic. Lancet Infect Dis. 2017 Sep;17(9):e280-e292. PubMed | Google Scholar
- Jacobsen KH, Aguirre AA, Bailey CL, Baranova AV, Crooks AT, Croitoru A et al. Lessons from the ebola outbreak: action items for emerging infectious disease preparedness and response. Ecohealth. 2016;13(1):200-12. PubMed | Google Scholar
- Abramowitz SA, Hipgrave DB, Witchard A, Heymann DL. Lessons from the west africa ebola epidemic: a systematic review of epidemiological and social and behavioral science research priorities. Int J Infect Dis. 2018;218(11):1730-8. PubMed | Google Scholar
- Oliveras C, Cluver L, Bernays S, Armstrong A. Nothing about us without RIGHTS-meaningful engagement of children and youth: from research prioritization to clinical trials, implementation science, and policy. J Acquir Immune Defic Syndr. 2018 Aug 15;78 Suppl 1(1):S27-S31. PubMed | Google Scholar
- Krubiner CB, Faden RR, Karron RA, Little MO, Lyerly AD, Abramson JS et al. Pregnant women & vaccines against emerging epidemic threats: ethics guidance for preparedness, research, and response. Vaccine. 2019 May 3;S0264-410X(19)30045-3. PubMed | Google Scholar
- Papa A, Mirazimi A, Köksal I, Estrada-Pena A, Feldmann H. Recent advances in research on Crimean-Congo hemorrhagic fever. J Med Virol. 2015;64:137-43. PubMed | Google Scholar
- Calnan M, Gadsby EW, Kondé MK, Diallo A, Rossman JS. The response to and impact of the Ebola epidemic: towards an agenda for interdisciplinary research. Int J Workplace Health Manag. 2018 May 1;7(5):402-411. PubMed | Google Scholar
- Sprint-Sari Investigators. Using research to prepare for outbreaks of severe acute respiratory infection. BMJ glob health. 2019 Feb 13;4(1):e001061. PubMed | Google Scholar
- Imrie J, Hoddinott G, Fuller S, Oliver S, Newell ML. Why MSM in rural South African communities should be an HIV prevention research priority. AIDS and Behav. 2013;17(1):70-6. PubMed | Google Scholar
- Moon S, Leigh J, Woskie L, Checchi F, Dzau V, Fallah M et al. Post-Ebola reforms: ample analysis, inadequate action. BMJ. 2017;356:j280. PubMed | Google Scholar
- Wilder-Smith A, Gubler DJ, Weaver SC, Monath TP, Heymann DL, Scott TW. Epidemic arboviral diseases: priorities for research and public health. Lancet Infect Dis. 2017;17(3):e101-6. PubMed | Google Scholar
- Evans NG, Hills K, Levine AC. How should the WHO guide access and benefit sharing during infectious disease outbreaks? AMA J Ethics. 2020;22(1):28-35. PubMed | Google Scholar
- Cardoen S, De Clercq K, Vanholme L, De Winter P, Thiry E, Van Huffei X. Preparedness activities and research needs in addressing emerging infectious animal and zoonotic diseases. Revue Scientifique et Technique. Off Int Epizoot. 2017;36(2):557-68. PubMed | Google Scholar
- Greenwood B. Priorities for research on meningococcal disease and the impact of serogroup A vaccination in the African meningitis belt. Vaccine. 2013;31(11):1453-7. PubMed | Google Scholar
- Folayan MO, Haire B, Allman D, Yakubu A, Afolabi MO. Research priorities during infectious disease emergencies in West Africa. BMC Res. Notes. 2018;11(1):159. PubMed | Google Scholar
- Yach D, Pratt A, Glynn TJ, Reddy KS. Research to stop tobacco deaths. Global Health. 2014;10(1):39. PubMed | Google Scholar
- Nkengasong J, Djoudalbaye B, Maiyegun O. A new public health order for Africa's health security. The Lancet Glob. Health. 2017;5(11):e1064-5. PubMed | Google Scholar
- African Centre for Disease Control. First scientific symposium. 25 March 2017. Accessed 27 April 2020.
- African Union Commission. Agenda 2063 first ten year implementation plan 2014-2023. Addis Ababa, Ethiopia. 2015.
- African Union. Africa Health Strategy 2016-2030. Addis Ababa; 2016.
- Critchley JA, Restrepo BI, Ronacher K, Kapur A, Bremer AA, Schlesinger LS et al. Defining a research agenda to address the converging epidemics of tuberculosis and diabetes: part 1: epidemiology and clinical management. Chest. 2017;152(1):165-73. PubMed | Google Scholar
- Geng EH, Holmes CB, Moshabela M, Sikazwe I, Petersen ML. Personalized public health: an implementation research agenda for the HIV response and beyond. PLoS Med. 2019 Dec 31;16(12):e1003020. PubMed | Google Scholar
- World Health Organization. An R&D blueprint for action to prevent epidemics. 2016.
- World Health Organization. Limiting the spread of pandemic, zoonotic and seasonal epidemic influenza. Geneva; 2010. Accessed 27 April 2020.
- Farrar J, Focks D, Gubler D, Barrera R, Guzman MG, Simmons C et al. Towards a global dengue research agenda. Trop Med Int Health. 2007;12(6):695-9. PubMed | Google Scholar
- World Health Organization. WHO Ebola research committee. Prioritized research agenda. 19 October 2015. Accessed 27 April 2020.
- World Health Organization. Zika virus research agenda. October 2016. Accessed 27 April 2020.
- Wellcome Trust. Advancing epidemics R&D to keep up with a changing world: progress, challenges, and opportunities. 2019. Accessed 27 April 2020.
- WHO Ebola Response Team. Ebola virus disease in West Africa - The first 9 months of the epidemic and forward projections. N Engl J Med. 2014;371:1481-95. Google Scholar
- Fatiregun AA, Isere EE. Epidemic preparedness and management: a guide on lassa fever outbreak preparedness plan. Niger Med J. 2017;58(1):1-6. PubMed | Google Scholar
- World Bank. International vaccines task force. Money and microbes - strengthening clinical research capacity to prevent epidemics. Washington DC: World Bank, 2018.
- Qin Y, Wang Q, Yang X, Yin W, Zhang M, Xia Y et al. Urgent research agenda for the novel coronavirus epidemic: transmission and non-pharmaceutical mitigation strategies. Chinese Center for Disease Control and Prevention; 2020. Google Scholar
- Mutapi F. Africa should set its own health-research agenda. Nature. 2019;575(7784):567. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
This supplement
- Clinical characteristics, treatment regimen and duration of hospitalization among COVID-19 patients in Ghana: a retrospective cohort study (Accessed 8047 times)
- Comment différencier une pneumonie COVID-19 et un œdème aigu du poumon? À propos d´un cas (Accessed 4252 times)
- A descriptive study of the trends of COVID-19 in Zimbabwe from March-June 2020: policy and strategy implications (Accessed 2975 times)
- Regional vulnerability for COVID-19 in Cameroon (Accessed 2740 times)
- La lutte contre la COVID-19 au Cameroun nécessite un second souffle (Accessed 2648 times)
- Malaria and COVID-19: commonalities, intersections and implications for sustaining malaria control (Accessed 2374 times)
- A descriptive study of the trends of COVID-19 in Zimbabwe from March-June 2020: policy and strategy implications (Downloaded 211 times)
- Clinical characteristics, treatment regimen and duration of hospitalization among COVID-19 patients in Ghana: a retrospective cohort study (Downloaded 163 times)
- Regional vulnerability for COVID-19 in Cameroon (Downloaded 162 times)
- Malaria and COVID-19: commonalities, intersections and implications for sustaining malaria control (Downloaded 141 times)
- Comment différencier une pneumonie COVID-19 et un œdème aigu du poumon? À propos d´un cas (Downloaded 115 times)