Prevalence of metronidazole resistance and Helicobacter pylori infection in Moroccan children: a cross-sectional study
Fatima Zahra Kheir, Aicha Baalala, Ghizlane Bounder, Abdelhak Abkari, Dalal Ben Sabbahia, Meriem Atrassi, Halima Rchid, Nourdin Harich, Mariama Lasky, Hasna Boura
Corresponding author: Hasna Boura, Laboratory of Helicobacter pylori and Gastric Pathologies, Institut Pasteur du Maroc, Casablanca 20360, Morocco 
Received: 15 Mar 2024 - Accepted: 07 Jun 2024 - Published: 04 Jul 2024
Domain: Epidemiology,Molecular Biology,Pediatric gastroenterology
Keywords: Helicobacter pylori, prevalence, resistance, metronidazole, children
©Fatima Zahra Kheir et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Fatima Zahra Kheir et al. Prevalence of metronidazole resistance and Helicobacter pylori infection in Moroccan children: a cross-sectional study. Pan African Medical Journal. 2024;48:89. [doi: 10.11604/pamj.2024.48.89.43271]
Available online at: https://www.panafrican-med-journal.com//content/article/48/89/full
Research 
Prevalence of metronidazole resistance and Helicobacter pylori infection in Moroccan children: a cross-sectional study
Prevalence of metronidazole resistance and Helicobacter pylori infection in Moroccan children: a cross-sectional study
![]() Fatima Zahra Kheir1,2, Aicha Baalala1,3, Ghizlane Bounder1, Abdelhak Abkari4,
Fatima Zahra Kheir1,2, Aicha Baalala1,3, Ghizlane Bounder1, Abdelhak Abkari4, ![]() Dalal Ben Sabbahia4, Meriem Atrassi4, Halima Rchid2, Nourdin Harich3, Mariama Lasky2,
Dalal Ben Sabbahia4, Meriem Atrassi4, Halima Rchid2, Nourdin Harich3, Mariama Lasky2, ![]() Hasna Boura1,&
Hasna Boura1,&
&Corresponding author
Introduction: the prevalence of Helicobacter pylori (H. pylori) infection in children is very high in Morocco. Eradication rates of H. pylori infection decrease due to the emergence of resistance to antibiotics. Data on the antimicrobial susceptibility of H. pylori in Moroccan children are not available. This study aims to assess the prevalence of H. pylori infection and the metronidazole resistance rate of H. pylori in Moroccan pediatric patients, and their association with epidemiologic factors.
Methods: a cross-sectional study was conducted on 132 pediatric patients who had an indication for upper gastrointestinal endoscopy and attended pediatric hospital Abderrahim Harouchi of the University Hospital Ibn Rochd, Casablanca, Morocco. Detection of H. pylori infection and the susceptibility to metronidazole was performed by classic PCR. Statistical analysis was performed using R Studio software.
Results: the overall prevalence of H. pylori infection was 80.3%. vomiting was significantly associated with H. pylori infection (p-value=0.01). Regarding the resistance rate of metronidazole, we found that the prevalence of H. pylori resistance to metronidazole was high (70.8%) and it significantly increased, especially in pediatric patients living in urban areas (p-value=0.01).
Conclusion: the prevalence of H. pylori infection and resistance rate of metronidazole were very high in Moroccan children. Therefore, triple therapy with metronidazole must be preceded by a study of the bacterium�s susceptibility to the prescribed antibiotics, in particular to metronidazole.
Helicobacter pylori (H. pylori) is a spiral, gram-negative, curved, microaerophilic bacterium. Infection with H. pylori is widespread throughout the world, usually occurring in childhood and remaining in the infected children for life unless appropriate treatment is applied [1,2]. It is the leading cause of chronic gastritis and peptic ulcer disease in children, and the prevalence of this infection ranges from 1.7% to 97.1% in children in different countries [3,4]. A study conducted in Morocco revealed that the prevalence of H. pylori infection in children was around 53% [5].
In Morocco, the first-line eradication therapy for H. pylori in children according to the European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) and North American Society For Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) includes a proton pump inhibitor (PPI) and amoxicillin in combination with clarithromycin or metronidazole for two weeks [6]. Eradication success rates with this regimen have historically exceeded 90%. However, there has been a recent increase in the failure rate of this therapy due to the increasing resistance of H. pylori to antibiotics worldwide [7,8].
Metronidazole requires an activation step by reduction of the nitro group attached to the imidazole ring to achieve antimicrobial activity [9]. The reduction of this antibiotic is mainly mediated by oxygen-insensitive NADPH nitroreductase (RdxA), NADPH-flavin-oxidoreductase (FrxA), and ferredoxinlike enzymes (FrxB) in H. pylori [9]. The mechanism of resistance of H. pylori to metronidazole are complex and primarily due to the mutational inactivation of the rdxA and FrxA genes which encode the oxygen-insensitive NADPH nitroreductase and NADPH-flavin oxidoreductase respectively [10]. These mutations include frameshifts, deletions, premature truncations, and missense mutations within the two genes [10]. Inactivation of the rdxA by deletion of 200-bp in the rdxA encoding gene is the most common mechanism of metronidazole resistance [10,11].
Metronidazole resistance frequency in children varies depending on the geographic area and ranges from 10% to 91% [12]. In Morocco, a high prevalence of H. pylori resistance to metronidazole has been reported in adults (62.7%) [13]. To our knowledge, the prevalence of H. pylori resistance to metronidazole in Moroccan children has never been investigated by molecular test. Therefore, we conducted this study to assess the prevalence of H. pylori infection and the metronidazole resistance rate of H. pylori in Moroccan pediatric patients by targeting the rdxA gene deletion mutation in H. pylori, and their association with epidemiological factors.
Study design: a cross-sectional study was conducted at Children´s Hospital Abderrahim Harouchi Casablanca, Morocco from September 2022 to October 2023. This study was carried out to evaluate the prevalence of H. pylori infection and the metronidazole resistance rate of H. pylori in Moroccan pediatric patients, and their association with epidemiologic factors.
Study population and data collection: the study involved 132 children (aged between 2 and 17 years old) referred for endoscopy for digestive symptoms such as nausea or vomiting, heartburn, epigastric pain, recurrent abdominal pain, digestive hemorrhage, weight loss, and refractory anemia in pediatric Hospital Abderrahim Harouchi of the University Hospital Ibn Rochd, Casablanca, Morocco. Patients younger than 2 years, use of antibiotics or PPI in the four weeks before endoscopy, and patients not born or living in Morocco were excluded from the present study. Upper endoscopy was conducted by experienced endoscopists and endoscopic findings were recorded during endoscopy. Four gastric biopsies were obtained from each patient, two from the antrum and two from the fundus, for molecular detection and histological examination. One of the four gastric biopsies was fixed in 10% formalin and embedded in paraffin, and histologic sections were then colored with hematoxylin-eosin and modified Giemsa. Histomorphologic evaluation was carried out following the updated Sydney System criteria [14] by the pathologist who determined the presence/absence of H. pylori, and gastric lesions (chronic gastritis, gastric atrophy, intestinal dysplasia, and intestinal metaplasia). Chronic inflammation intensity of inflammation was reported as none, mild, moderate, and severe. A questionnaire was used to collect information such as demographic characteristics of the participants, and history of family infection with H. pylori, and history of previous eradication of H. pylori. Informed consent was acquired from the patient's parents.
Molecular test for H. pylori detection
Deoxyribonucleic acid (DNA) extraction: extraction of total DNA from gastric biopsies was performed using the isolate Genomic DNA Kit (Bioline, Memphis, USA) following the provided instructions, and the isolated DNA was stored at -20°C until use.
H. pylori infection: the detection of H. pylori infection was performed by amplification of the ureC gene (296 bp) using specific primers (Table 1) [15]. Each reaction mixture was prepared in a final volume of 20 μL by adding dNTPs (0.5 mM), primers (0.5 μM of each primer), 300 ng of DNA, MgCl2 (1.5 mM), and 1 U Taq polymerase (My Taq DNA Polymerase, Bioline). The PCR thermal conditions were as follows: 95°C denaturation for 1 min, followed by 35 cycles at 95°C for 15 sec, 55°C for 30 sec, 72°C for 30 sec, and 72°C final elongation cycle for 7 min.
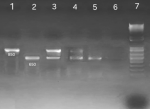
Metronidazole susceptibility detection: resistance to metronidazole was determined by detecting the 200 bp deletion of the rdxA gene, which is one of the most common mechanisms of H. pylori metronidazole resistance [16]. Polymerase chain reaction (PCR) was carried out to amplify the rdxA gene using specific primers (Table 1). For susceptible strains (wild-type gene of H. pylori) PCR amplification of this gene results in the amplification of an 850 bp fragment. Conversely, for resistant strains (mutant gene of H. pylori), PCR results in the amplification of a 650 bp fragment. The presence of two genes type and mutant genes was considered resistance [16,17]. The PCR amplification of the rdxA gene was carried out in a final volume of 20 μL comprising 300 ng of DNA, primers (0.8 μM of each primer), dNTPs (0.5 mM), MgC2 (1.5 mM), and 1U of Taq polymerase (My Taq DNA Polymerase, Bioline). The PCR thermal condition consisted of pre-denaturation at 95°C for 1 min, followed by 35 cycles of 95°C for 15 sec, 58°C for 30 sec, 72°C for 30 sec, and finally an elongation at 72°C for 7 min. After that 5 μL of PCR products were added to 1 μL of loading buffer (10x) and electrophoresed on agarose gel 1.5% (Figure 1).
Statistical analysis: Rstudio for Windows version 4.3.1 was used for statistical analyses. Missing data of specific variables were excluded from the analysis, resulting in adjustments to the sample size for those variables. Descriptive data are expressed as frequencies and means ± standard deviations (SD). For continuous variables, differences between groups were assessed using the t-test or Kruskal test, and for categorical variables using the Chi-square or Fisher´s exact test. The differences were considered significant at p < 0.05.
Ethical considerations: the study was conducted according to the ethical standards of Helsinki and approved by the Ethics Committee of the Mohamed VI University of Health Sciences of Casablanca of Morocco (CE/UM6SS/18/24). Informed consent was obtained from the patient's parents.
Patient characteristics: this study included 132 biopsies obtained from children with a histopathological diagnosis of chronic gastritis, 65 were males (49.2%), and 67 were females (50.8%), with an overall mean age was 9.27 ± 3.4 years, ranging from 2 to 17 years. Children were stratified into two age groups: 66 children among the group of [2-9 years], and 66 among the group of [10-17 years]. Most of our patients lived in urban rather than rural areas (85.6% vs 14.4%, respectively). Nodular gastritis was the most frequent endoscopic finding (41.7%) in our study. Out of 132 patients included in this study, histologic examination results were available for 114 participants and revealed a predominance of chronic gastritis in 80.3%, while atrophic and follicular gastritis was found in 2.3% and 3.8% of patients respectively. The intensity of chronic inflammation showed that moderate gastritis was the predominant finding in 62.3% of patients, while mild gastritis and severe gastritis were found in 36.8% and 0.9% of patients respectively (Table 2).
Prevalence of H. pylori infection and risk factors: of the 132 patients included in this study, 106 (80.3%) were positive and 26 (19.7%) were negative for H. pylori infection based on PCR results for detection of the UreC gene. For the histological results among the 114 patients, 101 were positive for H. pylori infection (88.6%) and 13 (11.4%) were negative and it was not performed in 18 patients. Demographic data, history of previous eradication of H. pylori, family history of H. pylori infection, endoscopy findings, symptoms, and histological findings in H. pylori infected patients, compared to those who were uninfected, are presented in Table 2. The prevalence of H. pylori infection was higher in children aged between 2 and 9 years (83.3% VS 77.3%), but the difference was not statistically significant (p-value=0.47). Regarding the living area, H. pylori infection was higher in patients living in urban and rural areas (80.5%, and 78,9%, respectively) statistically, the difference was not significant. The distribution of H. pylori infection was roughly similar between females and males (79.1% vs 81.5% respectively). Vomiting as a presenting symptom was more common among infected children and the difference was statistically significant (p-value=0.01). There were no statistically significant differences between positive and negative children in terms of gender, and history of previous eradication of H. pylori, family history of H. pylori infection, endoscopy findings, and histological findings.
Prevalence of metronidazole resistance: several mechanisms were reported to contribute to H. pylori resistance to metronidazole in this study we investigate the frequency of rdxA gene deletion mutation in H. pylori. Our study revealed a high resistance rate to metronidazole of 70.8% (75/106) in infected patients, whereas only 29.2% (31/106) were susceptible to metronidazole.
Resistance to metronidazole and risk factors: the results of the study of risk factors contributing to metronidazole resistance are summarized in Table 3. The metronidazole resistance rate was higher in children older than 9 years (80.4% vs 61.8%) but this difference was not statistically significant (p-value=0.35). According to gender, the resistance rate in females was slightly higher (75.5 vs 66%). However, no significant difference was found between resistance to metronidazole and genders (p-value=0.28). In this study, we have also assessed the correlation between living areas and metronidazole resistance. Our data showed that children living in urban areas have the highest rate of metronidazole resistance (75.8%) compared to those from rural areas (40%) and the difference was statistically significant (p-value=0.01). The relationship between resistance and gastric lesions showed that chronic gastritis was higher in children infected with resistance strains (71.3%). However, the correlation between the severity of histological gastritis and metronidazole resistance did not reveal a statistically significant difference (p-value=0.35) (Table 3).
H. pylori infection represents a serious public health problem in Morocco, several studies reported prevalence is very high in children and adults [5,18,19]. Hence, it is very essential to know the incidences of its resistance to different antibiotics used for the treatment of this bacterium. In the present study, a high incidence of H. pylori infection (80.3%) was observed in the patients enrolled. Its rate was higher compared to our neighboring countries such as Tunisia [20], Egypt [21], and Nigeria [22], but lower than that reported in Vietnam [23]. There was a notable increase in the incidence of H. pylori infection in Moroccan children compared to previous studies, which reported rates of 45% [18] and 53% [5].
These differences in incidence could be probably attributed to the different methods of diagnosis, sample size, and characteristics of patients included in this study. The frequency of H. pylori infection was slightly higher in younger children aged between 2-9 years (83.3%) than in older children aged between 10-17 years (77.3%), which is consistent with the results of a study conducted by Polfan et al. that revealed a high frequency of H. pylori infection in children between 2 to 9 years old (54.5%) [24]. In Vietnam, H. pylori infection was higher in children under the age of 3 years old [25]. Meanwhile, other studies have reported an increase in the frequency of H. pylori infection with age in children [22,24]. Our findings could be explained by the high incidence of H. pylori infection in developing regions and the highest incidence occurs at younger ages, especially in the initial five years of life [26].
The prevalence of H. pylori infection is high in children living in urban areas (80.5%) similar to our results Ravelomanana et al. found that the infection rate is higher in children from urban areas (46.9%) than in rural areas (26.4%) [27]. The high rate could probably be due to municipal water networks as described in the study of Ravelomanana et al. [27] or to mothers' habits of transmitting bacteria to their children, such as the pre-mastication of food. H. pylori infection in pediatric patients may be clinically asymptomatic or associated with non-specific symptoms such as recurrent abdominal pain, epigastric pain, vomiting, and gastroesophageal reflux, which are common to a variety of childhood illnesses [28]. in this study, a significant association was found between H. pylori infection and vomiting (p-value=0.01). These results were consistent with those reported by Dore et al. where diarrhea and nausea/vomiting were significantly associated in children [29]. on the other hand, in Romania, they found that epigastric pain was the most common symptom in infected children [30]. To our knowledge, the antibiotic susceptibility profile of pediatric patients in Morocco has never been reported before. In the course of this study, we examined the metronidazole resistance rate of H. pylori in Moroccan pediatric patients and their association with epidemiologic factors.
Metronidazole is a frequently used first-line treatment to eradicate H. pylori infection. however, its efficacy is undermined by escalating resistance, significantly reducing its therapeutic value [31]. In this study, we found a high metronidazole resistance rate, affecting 70.8% of infected patients. Our result is almost similar to that found in China (68.4%) [32] but much higher than that documented in Vietnam (14.5%) [2], Iran (41.1%) [33], and Jordan (50%) [34], and lower than that found in Egypt (82%) [35]. The high incidence of metronidazole resistance may be attributed to its extensive utilization for parasitic infections in children [12]. A massive national screening is recommended to confirm the results of our study and to make a well-informed decision regarding the use of metronidazole in the treatment of H. pylori in Moroccan children. Analysis of the association of the demographic data and metronidazole resistance demonstrated that patients living in urban areas were at high risk of developing metronidazole-resistant, with a rate of 75.8% compared to patients living in rural areas (40%) (p-value=0.01). In contrast, Nguyen et al. found that metronidazole was significantly higher in rural than urban areas (respectively 74.3%, 57.9%, p-value=0.011) [36]. This difference could be attributed to the higher use of antibiotics in urban areas than in rural areas in our country given the availability and accessibility of antibiotics in urban areas. According to age, we found an upward trend in the resistance rate of metronidazole in older children (80.4%) than in younger children (61.8%) but statistically, the difference was not significant. Oleastro et al. reported in their study that older children aged 11-18 years had the highest rate of metronidazole resistance compared to the youngest children [37]. The possible correlation between the resistance to metronidazole and age could be explained by the increased prescription of this antibiotic for other infections with age for other infections [38].
This study has several limitations. First of all, this study was conducted in a single center and examined a limited number of children; therefore, further multicenter studies should be undertaken. Moreover, the antibiogram method is the reference method for antibiotic susceptibility testing, but we could not use this method because of its high risk of failure given the H. pylori specific growth requirements. In addition, there are other mechanisms of H. pylori resistance to metronidazole, such as mutations in the rdxA and frxA genes, which may also contribute to resistance to metronidazole and future studies will be conducted in this study population to investigate these mechanisms.
In conclusion, our data showed a high incidence of H. pylori among Moroccan children. In addition, we have found that vomiting may be a symptom associated with H. pylori infection in children. Infected children also had an elevated rate of metronidazole resistance, which was higher in those living in urban areas. This study highlights the critical importance of the prevention and eradication of H. pylori. Nevertheless, Given the increasing rate of metronidazole resistance and the limited number of antibiotics available for H. pylori eradication in pediatric patients, it is beneficial to include antimicrobial susceptibility testing in the diagnostic protocol for H. pylori in our country.
What is known about this topic
- H. pylori infection is a chronic infection that affects more than half of the worldwide population;
- Metronidazole is one of the antibiotics used for the eradication of H. pylori in children.
What this study adds
- The prevalence of H. pylori infection and resistance to metronidazole was high in Moroccan children;
- Children living in urban areas have the highest rate of H. pylori metronidazole resistance;
- Metronidazole should be prescribed based on susceptibility test results.
The authors declare no competing interests.
Conceptualization and study design: Fatima Zahra Kheir, Hasna Boura, and Mariama Lasky. Data curation: Fatima Zahra Kheir, Aicha Baalala, Abdelhak Abkari, Dalal Ben Sabbahia, and Meriem Atrassi. Data analysis: Fatima Zahra Kheir, Ghizlane Bounder, Hasna Boura, and Mariama Lasky. Writing-original draft: Fatima Zahra Kheir. Writing review and editing: Hasna Boura, Mariama Lasky, Ghizlane Bounder, Nourdin Harich, and Halima Rchid. All authors have read and approved the final version of the manuscript.
The authors would like to thank the entire staff of the Gastroenterology unit and Anatomopathology Department of the Hospital Abderrahim Harouchi of the University Hospital Ibn Rochd, Casablanca. we would like to thank all of the participating children and their parents. We are also thankful to Dr. Meriem Khyati from the Laboratory of Onco-Virology, Institut Pasteur du Maroc for her help and support.
Table 1: primer sequences for detection of H. pylori
Table 2: epidemiologic and clinical factors associated with H. pylori infection in children (n=132)
Table 3: epidemiological factors associated with H. pylori resistance to metronidazole in infected children (n=106)
Figure 1: polymerase chain reaction products of the rdxA gene: lane 1 positive control, lane 2 resistant strain mutant gene 650bp, lanes 3 and 4 resistant strains with a wild and mutant gene, lane 6 negative control, lane 7 1Kb DNA ladder
- Malaty HM, El-Kasabany A, Graham DY, Miller CC, Reddy SG, Srinivasan SR et al. Age at acquisition of Helicobacter pylori infection: a follow-up study from infancy to adulthood. The Lancet. 2002;359(9310):931-935. PubMed | Google Scholar
- Van Thieu H, Duc NM, Nghi BTD, Van Bach N, Khoi HH, Tien VNT et al. Antimicrobial Resistance and the Successful Eradication of Helicobacter pylori-Induced Gastroduodenal Ulcers in Vietnamese Children. Med Arch. 2021;75(2):112-115. PubMed | Google Scholar
- Ertem D. Clinical Practice: Helicobacter pylori infection in childhood. Eur J Pediatr. 2013;172(11):1427-1434. PubMed | Google Scholar
- Zamani M, Ebrahimtabar F, Zamani V, Miller WH, Alizadeh-Navaei R, Shokri-Shirvani J et al. Systematic review with meta-analysis: the worldwide prevalence of Helicobacter pylori infection. Alimentary Pharmacology & Therapeutics. 2018;47(7):868-876. PubMed | Google Scholar
- Bouihat N. Epidemiology and Risk Factors of Helicobacter pylori Infection among Moroccan Children: Comparison between Asymptomatic and Symptomatic Children. Age. 1991 May;2:44. Google Scholar
- Jones NL, Koletzko S, Goodman K, Bontems P, Cadranel S, Casswall T et al. Joint ESPGHAN/NASPGHAN Guidelines for the Management of Helicobacter pylori in Children and Adolescents (Update 2016). Journal of Pediatric Gastroenterology & Nutrition. 2017;64(6):991-1003. PubMed | Google Scholar
- Meli LE, Mrginean CO, Ssran MO. The Challenges of Eradicating Pediatric Helicobacter pylori Infection in the Era of Probiotics. Children. 2022;9(6):795. PubMed | Google Scholar
- Suzuki H, Nishizawa T, Hibi T. Helicobacter pylori eradication therapy. Future Microbiology. 2010;5(4):639-648. PubMed | Google Scholar
- Jenks PJ, Edwards DI. Metronidazole resistance in Helicobacter pylori. International Journal of Antimicrobial Agents. 2002;19(1):1-7. PubMed | Google Scholar
- Hanafi A, Lee WC, Loke MF, Teh X, Shaari A, Dinarvand M et al. Molecular and Proteomic Analysis of Levofloxacin and Metronidazole Resistant Helicobacter pylori. Frontiers in Microbiology. Front Microbiol. 2016 Dec 15;7:2015. PubMed | Google Scholar
- Amin M, Shayesteh AA, Serajian A, Goodarzi H. Assessment of metronidazole and clarithromycin resistance among Helicobacter pyloriisolates of Ahvaz (southwest of Iran) during 2015-2016 by phenotypic and molecular methods. Jundishapur Journal of Microbiology. 2019 Apr 30;12(4). Google Scholar
- Borka Balas R, Meli LE, Mrginean CO. Current Worldwide Trends in Pediatric Helicobacter pylori Antimicrobial Resistance. Children. 2023;10(2):403. PubMed | Google Scholar
- Essaidi I, Bounder G, Jouimyi R, Boura H, Elyounsi I, Kheir FZ et al. Comparative Study of Helicobacter pylori Resistance to Clarithromycin and Metronidazole and Its Association with Epidemiological Factors in A Moroccan Population. Asian Pac J Cancer Prev. 2022;23(8):2755-2761. PubMed | Google Scholar
- Stolte M, Meining A. The updated Sydney system: classification and grading of gastritis as the basis of diagnosis and treatment. Canadian Journal of Gastroenterology and Hepatology. 2001;15(9):591-8. PubMed | Google Scholar
- Lu J-J, Perng CL, Shyu RY, Chen CH, Lou Q, Chong SKF et al. Comparison of Five PCR Methods for Detection of Helicobacter pylori DNA in Gastric Tissues. J Clin Microbiol. 1999;37(3):772-774. PubMed | Google Scholar
- Debets-Ossenkopp YJ, Pot RGJ, van Westerloo DJ, Goodwin A, Vandenbroucke-Grauls CMJE, Berg DE et al. Insertion of Mini-IS605 and Deletion of Adjacent Sequences in the Nitroreductase (rdxA) Gene Cause Metronidazole Resistance in Helicobacter pylori NCTC11637. Antimicrob Agents Chemother. 1999;43(11):2657-2662. PubMed | Google Scholar
- Wani FA, Bashir G, Khan MA, Zargar SA, Rasool Z, Qadri Q. Antibiotic Resistance in Helicobacter pylori: A Mutational Analysis from a Tertiary Care Hospital in Kashmir, India. Indian Journal of Medical Microbiology. 2018;36(2):265-272. PubMed | Google Scholar
- Hibaoui L, Massik A, Yahyaoui G, Mahmoud M, Hmass N, Chbani L et al. Moroccan Children With Helicobacter pylori Infection: Demographics, Clinical Features, and Histological Findings. Cureus. 2023 Jun 21;15(6):e40740. PubMed | Google Scholar
- Bounder G, Boura H, Nadifiyine S, Jouimyi MR, Bensassi M, Kadi M, Eljihad M, Badre W, Benomar H, Kettani A, Lebrazi H. Epidemiology of Helicobacter pylori infection and related gastric pathologies in Moroccan population. J Life Sci. 2017;11(5):211-8. Google Scholar
- Siai K, Ghozzi M, Ezzine H, Medjahed N, Azzouz MM. Prevalence and risk factors of Helicobacter pylori infection in Tunisian children: 1055 children in Cap-Bon (northeastern Tunisia). Gastroentérologie Clinique et Biologique. 2008;32(11):881-886. PubMed | Google Scholar
- Naficy AB, Frenck RW, Abu-Elyazeed R, Kim Y, Rao MR, Savarino SJ et al. Seroepidemiology of Helicobacter pylori infection in a population of Egyptian children. International Journal of Epidemiology. 2000;29(5):928-932. PubMed | Google Scholar
- Emerenini F, Nwolisa E, Iregbu F, Eke C, Ikefuna A Emerenini FC, Nwolisa EC et al. Prevalence and risk factors for Helicobacter pylori infection among children in Owerri, Nigeria. Nigerian Journal of clinical practice. 2021 Aug 1;24(8):1188-93. Google Scholar
- Che TH, Nguyen TC, Ngo DTT, Nguyen HT, Vo KT, Ngo XM et al. High Prevalence of Helicobacter pylori Infection Among School-Aged Children in Ho Chi Minh City, VietNam. Int J Public Health. 2022;67:1605354. PubMed | Google Scholar
- Polfan M, Pratita W, Siregar GA, Yanni GN, Sianturi P. Risk Factors Associated with Helicobacter pylori Infection in Children with Gastrointestinal Symptoms. International Journal of Research Publications. 2021 Jun 20;78(1):9. Google Scholar
- Langner M, Machado RS, Patrício FRS, Kawakami E. Evaluation of gastric histology in children and adolescents with Helicobacter pylori gastritis using the Update Sydney System. Arq Gastroenterol. 2009;46(4):328-332. PubMed | Google Scholar
- Khalifa MM, Sharaf RR, Aziz RK. Helicobacter pylori: a poor man´s gut pathogen. Gut Pathogens. 2010;2(1):2. PubMed | Google Scholar
- Ravelomanana L, Imbert P, Kalach N, Ramarovavy G, Richard V, Carod JF et al. Helicobacter pylori infection in children in Madagascar: risk factors for acquisition. Trop Gastroenterol. 2013 Oct-Dec;34(4):244-51. PubMed | Google Scholar
- Sabbagh P, Javanian M, Koppolu V, Vasigala VR, Ebrahimpour S. Helicobacter pylori infection in children: an overview of diagnostic methods. Eur J Clin Microbiol Infect Dis. 2019;38(6):1035-1045. PubMed | Google Scholar
- Dore MP, Fanciulli G, Tomasi PA, Realdi G, Delitala G, Graham DY et al. Gastrointestinal Symptoms and Helicobacter pylori Infection in School-Age Children Residing in Porto Torres, Sardinia, Italy. Helicobacter. 2012;17(5):369-373. PubMed | Google Scholar
- Rosu OM, Gimiga N, Stefanescu G, Anton C, Paduraru G, Tataranu E et al. Helicobacter pylori Infection in a Pediatric Population from Romania: Risk Factors, Clinical and Endoscopic Features and Treatment Compliance. J Clin Med. 2022;11(9):2432. PubMed | Google Scholar
- Lin Y, Shao Y, Yan J, Ye G. Antibiotic resistance in Helicobacter pylori: From potential biomolecular mechanisms to clinical practice. Journal of Clinical Laboratory Analysis. 2023;37(7):e24885. PubMed | Google Scholar
- Zhang Y, Wen Y, Xiao Q, Zheng W, Long G, Chen B et al. Mutations in the Antibiotic Target Genes Related to Clarithromycin, Metronidazole and Levofloxacin Resistance inHelicobacter pylori Strains from Children in China. Infect Drug Resist. 2020 Jan 30;13:311-322. PubMed | Google Scholar
- Haghighi MB, Dara N, Mansour Ghanaie R, Azimi L, Hosseini A et al. Evaluation of clarithromycin and metronidazole resistance of Helicobacter pylori infection in symptomatic Iranian children. International Journal of Pediatrics. 2019 Feb 1;7(2):8925-33. PubMed | Google Scholar
- Burayzat S, Al-Tamimi M, Barqawi M, Massadi MS, Abu-Raideh J, Albalawi H et al. Antimicrobial Resistance Molecular Mechanisms of Helicobacter pylori in Jordanian Children: A Cross-Sectional Observational Study. Antibiotics. 2023;12(3):618. PubMed | Google Scholar
- Awad YM, Eldeeb MT, Fathi MS, Mahmoud N, Morsy RM. Helicobacter pylori Antibiotic resistance patterns among Egyptian children and predictors of resistance. QJM: An International Journal of Medicine. 2020 Mar 1;113(Supplement_1):hcaa063-021. Google Scholar
- Nguyen TVH, Bengtsson C, Yin L, Nguyen GK, Hoang TTH, Phung DC et al. Eradication of Helicobacter pylori in Children in Vietnam in Relation to Antibiotic Resistance. Helicobacter. 2012;17(4):319-325. PubMed | Google Scholar
- Oleastro M, Cabral J, Ramalho PM, Lemos PS, Paixao E, Benoliel J et al. Primary antibiotic resistance of Helicobacter pylori strains isolated from Portuguese children: a prospective multicentre study over a 10 year period. Journal of Antimicrobial Chemotherapy. 2011;66(10):2308-2311. PubMed | Google Scholar
- Li L, Ke Y, Yu C, Li G, Yang N, Zhang J et al. Antibiotic resistance of Helicobacter pylori in Chinese children: A multicenter retrospective study over 7 years. Helicobacter. 2017;22(3):e12373. PubMed | Google Scholar