Prevalence of precancerous lesions and other cervical abnormalities among internally displaced women in Benue State Nigeria
Atenchong Ngwibete, Olayinka Ogunbode, Laadi Terrumun Swende, Mangalu Mobhe Agbada, Akinyinka Omigbodun
Corresponding author: Atenchong Ngwibete, Pan African University Life and Earth Sciences Institute (including Health and Agriculture)-PAULESI, University of Ibadan, Ibadan, Nigeria 
Received: 18 Mar 2023 - Accepted: 17 Jan 2024 - Published: 07 Feb 2024
Domain: Community health,Health promotion,Maternal and child health
Keywords: Internally displaced persons, precancerous lesions, cervical cancer, Africa
©Atenchong Ngwibete et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Atenchong Ngwibete et al. Prevalence of precancerous lesions and other cervical abnormalities among internally displaced women in Benue State Nigeria. Pan African Medical Journal. 2024;47:50. [doi: 10.11604/pamj.2024.47.50.39721]
Available online at: https://www.panafrican-med-journal.com//content/article/47/50/full
Research 
Prevalence of precancerous lesions and other cervical abnormalities among internally displaced women in Benue State Nigeria
Prevalence of precancerous lesions and other cervical abnormalities among internally displaced women in Benue State Nigeria
![]() Atenchong Ngwibete1,&,
Atenchong Ngwibete1,&, ![]() Olayinka Ogunbode2, Laadi Terrumun Swende3,
Olayinka Ogunbode2, Laadi Terrumun Swende3, ![]() Mangalu Mobhe Agbada4,
Mangalu Mobhe Agbada4, ![]() Akinyinka Omigbodun2
Akinyinka Omigbodun2
&Corresponding author
Introduction: visual inspection is a low-cost screening strategy that can be used to prevent cervical cancer in women. These techniques can improve screening health outcomes for internally displaced women (IDW) who have poor sexual and reproductive health and rights' behaviors and outcomes. This study aimed to determine the prevalence of precancerous lesions and other clinical features using a visual inspection with acetic acid (VIA) technique during a cervical cancer screening campaign in two internally displaced people (IDP) camps in Benue State, Nigeria.
Methods: this was a cross-sectional study of 166 IDW who voluntarily participated in the study during a VIA cervical cancer screening campaign in two IDP camps in Benue State, Nigeria the screening was done by a group of qualified and trained healthcare workers and data was collected using a structured, pretested questionnaire.
Results: a total of 99(60%) of the women had a first sexual experience at 16 years, while 78(47%) had more than 5 full-term pregnancies. Although only 72(43.4%) of the women acknowledged having more than one sexual partner, over 70% of the women stated that their sexual partner had another sexual partner. The prevalence of precancerous lesions among women was 10.8%. Smoking(p=0.003), age at menarche (p≤ 0.001) and sexual behaviors (p=0.009, p=0.004) were factors that had a statistically significant relationship with the presence of a precancerous lesion among the IDW. The study also highlights the high rate (95%) of cervicitis among the women and the relatively high rate (5.4%) of leukoplakia.
Conclusion: the majority of IDW had sociodemographic and lifestyle characteristics that predisposed them to developing cervical cancer More targeted interventions aimed at improving the sociodemographic and lifestyle characteristics of IDW are recommended. In addition, there is a need to create awareness about cervical cancer among IDW and make screening available in camp facilities for early detection and management.
In Africa, cervical cancer is one of the most prevalent cancers among women of reproductive age (15-49 years) [1]. This cancer is caused by two types of human papillomavirus (HPV) strands (16 and 18) that are responsible for over 70% of precancerous lesions [2]. According to the WHO, over 111,632 new cases of cervical cancer were reported in sub-Saharan Africa in 2018. In the same year, cervical cancer was responsible for the deaths of 68% of women [3]. Cervical cancer is preventable and treatable if detected at an early stage, during the pre-cancerous stages. Hence, routine screenings of the cervix with simple and cost-effective procedures like the Visual Inspection with Acetic Acid (VIA) have been recommended for identifying pre-cancerous changes in the cells of the cervix, which can then be treated before they develop into cancer [4]. Visual inspection is able to detect a variety of abnormalities in addition to precancerous lesions and cervical cancer. These abnormalities include cervical inflammation, polyps, and sexually transmitted infections such as genital warts caused by HPV. Although these conditions may not always be precursors to cancer, they still have the potential to have significant clinical implications and may necessitate treatment.
Cervical cancer progresses slowly from the pre-cancer stage to invasive cancer. Even though the cost of treatment when cancer is detected at its precancerous stage is very low, poor access to preventive screenings and treatment services makes early detection a significant problem [5]. This has been linked to more than 90% of cervical cancer-related deaths [6]. Many factors have been identified as risk factors for cervical cancer. According to the WHO, the risk is higher in women who are: HIV-positive; have had multiple sexual partners; have sex with partners who have had multiple sexual partners; participate in high-risk sexual activity; have not been vaccinated against HPV; have a coinfection involving other sexually transmitted diseases; smoke; engage in long-term use of oral contraceptives; and have not been screened for precancerous lesions [3]. These risk factors are prevalent among displaced persons and puts them at risk of reproductive health issues including cervical cancers [7,8]. However, these women have poor access to reproductive health services and cervical cancer screening services. After a community health intervention to get more IDW in camps in Benue State to use sexual and reproductive health (SRH) services, a researcher found that not enough people knew about or used cervical cancer screening services. Following the health education intervention, women in the camps showed interest in taking up cervical cancer screening. Given that this service is unavailable at camp facilities, a free cervical cancer screening program was offered to the women. Data was collected during the screening services to assess the prevalence of precancerous lesions and associated clinical features among the IDW in two displaced camps in Benue State.
Study design/ procedure: the study was a cross-sectional study undertaken during a cervical screening exercise in an IDP camp. Following a health education intervention to improve the uptake of RH services (HIV/AIDS, family planning, and cervical cancer screening) in Daudu Camps 1 and 2, women showed interest in using cervical cancer screening services. However, this service was unavailable in the camp at the time of the intervention. Based on this, the researcher partnered with other healthcare workers to provide free cervical cancer screenings to the women in these camps.
Study participants: the screening program targeted displaced women between the ages of 18 and 50. Eligibility criteria included being within the age group, being sexually active, having an intact cervix, and not being pregnant. Participation in the screening program was not limited to persons who received the health education.
Study location: the study took place in Daudu, in the Guma local government area (LGA) of Benue State. This community hosts two IDP camps (Daudu Camp 1 and Camp 3). Most of the people living in these camps are indigenous people who had to leave their homes because of violence caused by land disputes between Fulani herders and farmers. Violence caused by land disputes between Fulani herders and farmers. Benue State is said to have over 1.5 million displaced persons, some of whom are in one of the 27 IDP camps [9].
Screening procedure: the screening was carried out by a team of six (6) healthcare professionals and four community healthcare workers. Each woman was given prescreening counseling before the procedure. During this session, data was collected with the consent of the participants. Each screening room had two health professionals. Upon insertion of a sterile Cusco's virginal speculum, 5% acetic acid was applied to the cervix using a spray bottle. Results were read after one minute of application of acetic acid with the aid of a bright touch light. Well-defined, visible acetowhite legions seen in the transformation zone were considered positive. For quality assurance, this was confirmed by a second trained healthcare provider. Acetowhite lesions on the cervix were confirmed using Lugols Iodine. Lesions smaller than 75% were treated with thermal ablation. The team also looked out for other features such as cervical polyps, cervicitis, condyloma or warts, and ectropion or erosion. The team treated people with infections, including cervicitis and precancerous lesion smaller than 75% and referred women with other clinical conditions for specialized care. Following the procedure, appropriate postoperative counseling was provided. All results were also recorded.
Quality assurance: the study included a team of six healthcare workers, including two doctors and four nurses, who were trained and experienced in performing cervical cancer screening using the visual inspection under acetic acid (VIA) and visual inspection with lugols iodine (VILI) techniques. These practitioners also had training in the use of the thermal ablator. Each screening room was made up of two healthcare professionals. A second healthcare provider confirmed the screening findings. To ensure that data was collected appropriately, the data collectors were trained in the use of the tool, which was created following a review of the literature with modifications made to suit the study objectives. The instrument was pretested on a group of IDW in another local government area within the State. The data collected used a face-to-face interview approach after verbal consent from the IDW. Just before each woman entered the screening room, she was interviewed for data collection. Women were also given Unique IDs to race data collected. After the screening, the women were given a result sheet which had their unique IDs, this was used to enter the results against the woman previously collected information.
Variables of measure: data collected during face-to-face interview included sociodemographic characteristics, life-style characteristics, and clinical features. These variables were selected following literature review on the subject. Sociodemographic characteristics included participants' age, marital status, educational level, income and age at menarche. Lifestyle characteristics included cigarette smoking, parity, age of first sex, age of first pregnancy, and the total number of pregnancies ever had. Clinical features assessed and recorded in the result sheet included, the presence of precancerous lesions, cervical polyps, cervicitis, condyloma or warts, and ectropion or erosion.
Method data collection: data collection was done with the help of the Kobo collect data collecting software. Four research assistants trained in use of the application collected the data. Each woman was given a unique Identification number which was used as an identifier during data collection.
Method of data analysis: the collected data was entered into SPSS version 23 for data analysis. Results were represented in frequency tables and simple bar charts. Bivariate analysis was done using the chi-squares test of independence to check for association between the presence of precancerous lesions and respondents characteristics.
Ethical consideration: the research emanated as a result of a quasi-experimental PhD intervention carried out to improve the knowledge and use of HIV, family planning, and cervical cancer screening services. Ethical approval for this intervention was obtained from the UI/UCH ethical approval committee. Further approval to conduct the screening activity and research was obtained from the state ministry of health MOH/STA/204/VOL.1/209.
Sociodemographic characteristics of the study participants: as seen in Table 1, the mean age of the women was 31 years ± 9.1 and up to 144 (86.7%) were married or had a live-in partner. A total of 111 (66.9%) had no formal education. Although 137 (82.5%) of the respondents were employed, 138 (83.1%) earned less than 18,000 Naira per month. Up to 95(57%) of women have their first menses at 15 years of age or later.
Lifestyle and behavioral factors of study participants: Table 2 shows that smoking was prevalent among 6(3.6%) of the women. The mean age of first pregnancy was 16.7 years ± 4.4. Most of the women 78(47%) had more than 5 full-term pregnancies with a mean parity of 5±3 pregnancy. The mean age of sexual debut was 16 years ± 2 years of age with a majority 99(60%) having a first sexual experience at 16 years and below. A total of 72(43.4%) of the women had more than one sexual partner with more than three-quarter (72.9%) acknowledging having had a partner who had another sexual partner.
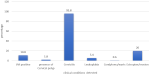
Prevalence of clinical condition detected upon visual inspection: most of the respondents had more than one of the abnormal clinical conditions during the inspection. As demonstrated in Figure 1, the most prevalent clinical condition detected during screening was cervicitis, with a prevalence of 95.9% and cervical ectropion with a prevalence of 20%. Leukoplakia was prevalent in 5.4% of the women. A total of 18 women (10.8%) had precancerous lesions (VIA positive) of which 14(8.4%) occupied less than 75% of the ectocervix.
Association between precancerous lesions with risk factors: according to the Table 3, smoking, age at menarche, having more than one sexual partner, age of first sex and having a sexual partner who had another sexual partner were factors that were significantly associated with the presence of a precancerous lesion among the IDW. Up to 5 of the 6 women had a precancerous lesion where smokers, contributing to 27.8% of those who were VIA-positive (χ²=33.8, p=< 0.001). Those who had more than one sexual partner contributed for up to 7.8% of the positivity (χ²=6.8, p= <0.001), while 10.8% of the positivity were of those who had sexual relationships with partners who had other partners (χ²=7.508, p=0.004). Women who had their first menarche at 14 and bellow had a high prevalence of a precancerous lesion (7.2%) this was statistically significant at χ²=4.7, P=0.003.
The sociodemographic and lifestyle characteristics of the study population confirm that the majority of women in IDP camps have a live-in partner, low educational attainments, a low level of income, a high parity rate, a late age of menarche, and an early sexual debut. The women had a mean age of menarche of 14 years (2.1), with over 50% having their first menstrual flow at about 15 years or later. In Nigeria, the age of menarche has been reported to range between 12 and 15 years [10,11]. However, studies show that women in low-resource and rural settings who are likely to get poor anthropological measures begin menstruating at a mean age of 14 and above [10]. This may be the same reason for the relatively late menarche age among the women. Furthermore, the majority of the women lived below the poverty line, with a monthly income of less than 18000 Naira. This is indicative of a likelihood of poor living conditions and nutritional capability that may influence individual development and lifestyle choices. The fact that over 40% had more than one sexual partner, of which 72% had partners with another partner, confirms the influence of the women's low income on their lifestyle choices, which indirectly affect their SRHR.
Precancerous lesions were found in 10.8% of the respondents. Although there is a gap in research on the prevalence of precancerous cervical lesions among IDW, studies in Nigeria have found a prevalence rate ranging from 6 to 12% [12,13]. However, the prevalence of 12% was recorded among HIV-positive women, who are known to be at increased risk of developing cervical cancer [13]. Cervicitis was also a condition that was of high prevalence in the population (95.9%). Cervicitis is a cervix infection that manifests as an inflamed cervix with unusual discharge. Studies among the displaced population have proven that there is a high prevalence of reproductive tract infections among displaced women [14,15]. This can be attributed to the cultural, unhealthy sexual and reproductive health and poor hygienic practices among these women. Some of these practices include rape, unprotected sex, having more than one sex partner, unavailability of water and toilet facilities and poor housing conditions [16]. Some of these attributes were seen to be predominant among the women in this study; for example, up to 42% of the women acknowledged having had more than one sexual partner, with more than 70% acknowledging having had a sexual partner who had other partners. Literature has proven that these practices are not uncommon among women in displaced communities due to poverty, hardship, and poor knowledge about sexual health [17,18]. These same reasons may account for the high prevalence of cervicitis in the population.
Leukoplakia was noticed in 5.4% of women. According to Basu and Sankaranarayanan's publication on the WHO's International Agency for Research on Cancer (IARC) website, leukoplakia is a condition that causes white patches visible on the cervical epithelium even before acetic acid application. This patch comes as a result of keratin on the epithelium. Its etiology has been linked to HPV infection or to being idiopathic [19]. This prevalence is relatively high compared to that in the literature, which stated that leukoplakia is seen in 1 in 70 women [20]. This is of primary concern as studies have shown that 27% of cervical leucoplakia cases usually end up as cancer [20].
Bivariate analysis showed that smoking, age at menarche, having more than one sexual partner, and having a sexual partner who had another sexual partner were factors that had a significant associated with the presence of a precancerous lesion in the women. These same factors have been identified in other literature [13,21]. Other factors that have been found to significantly affect the presence of a precancerous lesion in a woman include a history of STIs, age at first sex, parity greater than five, and HIV status [1]. However, these factors were not significant in our study. This may be due to the fact that these characteristics were fairly common among the women in the study. According to the study, over 40% of the IDW had a parity of more than 5, over 90% had a history of STIs, and 60% had sexual intercourse at age 16 or below. Other studies in Nigeria and Africa have found a much lower prevalence of such traits [13,22]. Although there was no significant relationship between women's age and the presence of a precancerous lesion, the majority of the women with a lesion were between 21 and 30 years old (4.8%) and 30 and 40 years old (5.4%), respectively. No lesion was found in women 20 and below. On the contrary, many studies have found a significant relationship between a woman's age and the presence of precancerous lesions [12,23]. However, just like many studies, cervical cancer lesions have been found to exist more among women over 30 and less than 40 [24]. The study also confirms that precancerous lesions are less likely in women under 20 years of age.
The research conducted substantiates the high occurrence of sociodemographic and lifestyle attributes among Internally Displaced Women (IDW) that make them susceptible to precancerous lesions. This investigation contributes to the existing literature by providing further evidence on the prevalence of precancerous lesions and other associated factors among IDW. In addition to the relatively high incidence of precancerous lesions, the study underscores the prevalence of related clinical conditions and lifestyle factors that suggest suboptimal sexual and reproductive health practices among this population. It highlights factors such as smoking, multiple sexual partners, early age of menarche, and having a sexual partner who is non-monogamous to significantly influence the occurrence of precancerous lesions among these women. Given the sociodemographic and lifestyle attributes of the IDW, it is imperative to raise awareness about cervical cancer within this group and ensure the availability of screening services in camp facilities for early detection and intervention. The study does have certain limitations. The sample was selected for convenience from the population, and data collection was restricted to only two IDP camps out of the 14 present in the study area, thereby limiting the number of women who could participate in the screening process. Despite these limitations, the study's strength lies in the expertise of the screening team.
What is known about this topic
- Internally displaced women have poor sexual and reproductive healthcare practices and access to sexual and reproductive rights services are poor;
- VIA technology is a cost-effective procedure that could be used for screening of cervical cancer in resource-limited and humanitarian settings.
What this study adds
- IDW of the study population have high risk characteristics that predisposes them to cervical cancer;
- The prevalence of precancerous lesions among the IDW in the study population is high;
- Conditions such as cervicitis and leukoplakia also have a high prevalence in the study population.
The authors declare no competing interests.
Conception and study design: Atenchong Ngwibete, Laadi Terrumun Swende. Data analysis and interpretation: Atenchong Ngwibete, Olayinka Ogunbode, and Mangalu Mobhe Agbada: manuscript drafting Atenchong Ngwibete Manuscript revision: Atenchong Ngwibete, Olayinka Ogunbode, Mangalu Mobhe Agbada, and Akinyinka Omigbodun. All authors read and approved the final version of the manuscript.
We like to acknowledge the support of Mr. Moses Ede and members of the Nigerian Medical Women Association in Makurdi for their collaboration in making this screening exercise possible. We also acknowledge the camp managers of Daudu camp 1 and camp 3 for assisting with coordination of the screening activity.
Table 1: sociodemographic characteristics of the study participants
Table 2: lifestyle and behavioral factors of study participants
Table 3: bivariate association of precancerous lesions with risk factors
Figure 1: prevalence of clinical condition detected upon visual inspection
- Jedy-Agba E, Joko WY, Liu B, Buziba NG, Borok M, Korir A et al. Cervical cancer screening behaviours and challenges: A sub-Saharan Africa perspective. Br J Cancer. 2020 Jun 16;36:97. PubMed | Google Scholar
- Fiander A. The prevention of cervical cancer in Africa. Womens Heal. 2011 Jan;7(1):121-32. PubMed | Google Scholar
- WHO, FMoH. Costing the National Strategic Plan on Prevention and Control of Cervical Cancer: Nigeria, 2017-2021. 2021;(November 2020):5-6.
- Tchounga BK, Jaquet A, Coffie PA, Horo A, Sauvaget C, Adoubi I et al. Cervical cancer prevention in reproductive health services: Knowledge, attitudes and practices of midwives in Côte d´Ivoire, West Africa. BMC Health Services Research. 2014 Apr 11:14:165. PubMed | Google Scholar
- Lauren J, Allison A, Caroline, MJ, Anne, MT, Alison MB. Implementation strategies to improve cervical cancer prevention in sub-Saharan Africa: a systematic review. Implement Sci. 2018 Feb 9;13(1):28. PubMed | Google Scholar
- Adoch W, Garimoi CO, Scott SE, Okeny GG, Moodley J, Komakech H et al. Knowledge of cervical cancer risk factors and symptoms among women in a refugee settlement: a cross-sectional study in northern Uganda. Confl Heal. 2020 Dec 3;14(1):85. PubMed | Google Scholar
- Women Refugee Commission. Inter-Agency Working Group on Reproductive Health in Refugee Situations. 2010;2.
- Tunçalp Ö, Fall IS, Phillips SJ, Williams I, Sacko M, Touré OB et al. Conflict, displacement and sexual and reproductive health services in Mali: Analysis of 2013 health resources availability mapping system (HeRAMS) survey. Confl Health. 2015 Sep 14;9:28. PubMed | Google Scholar
- BENSEMA. Benue Displaced Population Statistics. Benue State Emergency Management Agency. 2021.
- Adinma JIB-D, Egeonu RO, Adinma-Obiajulu ND, Emeka EA. Menarcheal Age and Nutritional Status of Secondary School Adolescent Girls in Nnewi, South-East Nigeria. Advances in Reproductive Sciences. 2021;09(02):139-148. Google Scholar
- Anikwe CC, Mamah JE, Okorochukwu BC, Nnadozie UU, Obarezi CH, Ekwedigwe KC. Age at menarche, menstrual characteristics, and its associated morbidities among secondary school students in Abakaliki, southeast Nigeria. Heliyon. 2020 May 26;6(5):e04018. PubMed | Google Scholar
- Bakari F, Abdul M, Ahmed S. The prevalence and course of preinvasive cervical lesions during pregnancy in a Northern Nigerian Teaching Hospital. Annals of African Medicine. 2017 Apr-Jun;16(2):74-80. PubMed | Google Scholar
- Daniel GO, Musa J, Akindigh TM, Shinku F, Shuaibu SI, Kwaghe B et al. Prevalence and predictors of precancerous cervical lesions among HIV-positive women in Jos, north-central Nigeria. Int J Gynecol Obstet. 2020 Nov;151(2):253-259. PubMed | Google Scholar
- Isah B saidu. Reproductive health challenges among internally displaced persons in abuja. 2015.
- Odo ANA, Musa K, Oladugba AVA. Sexual and reproductive health needs and problems of internally displaced adolescents (IDAs) in Borno State, Nigeria: A mixed method approach. Afr J Reprod Health. 2020 Mar;24(1):87-96. PubMed | Google Scholar
- Fatemi F, Moslehi S. Challenges of Reproductive Health Management in the Camps of Internally Displaced Persons: A Systematic Review. Ethiop J Health Sci. 2021 Jan;31(1):179-188. PubMed | Google Scholar
- Amodu OC, Salami BO, Richter S, Okeke-Ihejirika P. Reproductive healthcare for women in IDP camps in Nigeria: An analysis of structural gaps. Global Public Health. 2021 Apr;16(4):563-577 Epub 2020 Sep 22. PubMed | Google Scholar
- Ivanova O, Rai M, Kemigisha E. A Systematic Review of Sexual and Reproductive Health Knowledge, Experiences and Access to Services among Refugee, Migrant and Displaced Girls and Young Women in Africa. Int J Environ Res Public Health. 2018 Jul 26;15(8):1583. PubMed | Google Scholar
- Basu DP, Sankaranarayanan DR. Colposcopy Digital Atlas. Scr Publications. 2017. Accessed on 18 March 2023.
- Lebherz TB, Charles RB. Cervical Leukoplakia Its Significance. Postgraduate Medicine. 2016;38(3):327-30. Google Scholar
- Wabo B, Nsagha DS, Nana TN, Assob CJN. Prevalence and risk factors associated with precancerous cervical lesions among women in two cities in Cameroon. Pan Afr Med J. 2022 Apr 6;41:276. PubMed | Google Scholar
- Gedefaw A, Astatkie A, Tessema GA. The prevalence of precancerous cervical cancer lesion among HIV-infected women in Southern Ethiopia: A cross-sectional study. PLoS ONE. 2013 Dec 20;8(12):e84519. PubMed | Google Scholar
- Campos NG, Lince-Deroche N, Chibwesha CJ, Firnhaber C, Smith JS, Michelow P et al. Cost-effectiveness of cervical cancer screening in women living with HIV in South Africa: A mathematical modeling study. Journal of Acquired Immune Deficiency Syndromes. 2018 Oct 1;79(2):195-205. PubMed | Google Scholar
- Jedy-Agba E, Joko WY, Liu B, Buziba NG, Borok M, Korir A et al. Trends in cervical cancer incidence in sub-Saharan Africa. Br J Cancer. 2020 Jul;123(1):148-154. PubMed | Google Scholar