Hashimoto's thyroiditis presenting with cardiac tamponade: a case report
Muhammadnur Rachim Enoch, Muhammad Irfan, Rachmad Budianto, Achmad Hardin
Corresponding author: Muhammad Irfan, Cardiology Department, Abdul Aziz Hospital in Singkawang, Kota Singkawang, Kalimantan Barat 79123, Indonesia 
Received: 08 Sep 2023 - Accepted: 07 Oct 2023 - Published: 18 Oct 2023
Domain: Cardiology, Endocrinology
Keywords: Cardiac tamponade, Hashimoto's thyroiditis, hypothyroidism, case report
©Muhammadnur Rachim Enoch et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Muhammadnur Rachim Enoch et al. Hashimoto's thyroiditis presenting with cardiac tamponade: a case report. Pan African Medical Journal. 2023;46:62. [doi: 10.11604/pamj.2023.46.62.41687]
Available online at: https://www.panafrican-med-journal.com//content/article/46/62/full
Hashimoto´s thyroiditis presenting with cardiac tamponade: a case report
Muhammadnur Rachim Enoch1, ![]() Muhammad Irfan1,&, Rachmad Budianto1, Achmad Hardin1
Muhammad Irfan1,&, Rachmad Budianto1, Achmad Hardin1
&Corresponding author
Cardiac tamponade as the initial manifestation of Hashimoto's thyroiditis is an exceedingly uncommon occurrence. We present the case of a 36-year-old female who was admitted due to acute respiratory distress. A cardiac ultrasound revealed a severe pericardial effusion with tamponade signs. Subsequently, percutaneous pericardiocentesis was performed, resulting in a swift clinical improvement. Laboratory examinations confirmed severe hypothyroidism associated with Hashimoto's disease. Despite undergoing hormone replacement therapy, histological analysis of the pericardium revealed a chronic inflammation process. A follow-up cardiac ultrasound conducted six months later indicated the presence of a well-tolerated chronic pericardial effusion. In conclusion, clinicians should consider hypothyroidism as a potential cause when cardiac tamponade is observed, particularly in the absence of tachycardia. The prognosis is generally favorable with hormone replacement therapy, but regular ultrasound monitoring should be maintained until the patient achieves a euthyroid state.
Hashimoto's thyroiditis is an autoimmune disorder that affects the thyroid gland, an important producer of hormones regulating numerous bodily functions. This condition prompts the immune system to attack and destroy the thyroid's hormone-producing cells, typically resulting in decreased hormone production, a condition known as hypothyroidism. Hypothyroidism affects approximately 4% to 10% of the general population [1]. Insufficient thyroid hormones can impact nearly every organ system, leading to a variety of clinical symptoms. Thyroid hormones, particularly triodothyronine (T3), play a crucial role in development and function. Triodothyronine (T3) is responsible for increased tissue oxygen consumption, enhanced systolic contraction force, diastolic relaxation, and an overall reduction in vascular resistance. Hypothyroidism, characterized by a lack of T3, can manifest in cardiovascular issues such as diastolic hypertension, sinus bradycardia, pericarditis, dyslipidemia, and pericardial effusion [2].
Pericardial effusion is a condition characterized by the abnormal accumulation of fluid in the pericardial cavity and can result from various underlying causes such as tumors, uremia, trauma, cardiac surgery, and hypothyroidism. In hypothyroidism, the incidence of pericardial effusion is relatively low, occurring in approximately 3% to 6% of mild cases, and cardiac tamponade as the initial presentation of hypothyroidism is rare [3,4]. The progressive buildup of pericardial fluid can lead to cardiac tamponade. Typical acute cardiac tamponade is clinically diagnosed by observing symptoms like hypotension, jugular vein distention, and muffled heart sounds, collectively known as Beck's triad. In contrast, hypothyroid patients with Hashimoto's disease often present with bradycardia, a normal heart rate, or even high blood pressure [5,6].
In this article, we report a case from Abdul Aziz Hospital in which a patient with Hashimoto's disease developed cardiac tamponade, highlighting a rare occurrence associated with this condition.
Patient information: a 36-year-old female patient hailing from Singkawang City, Indonesia, received an initial diagnosis of primary hypothyroidism secondary to Hashimoto's thyroiditis. She sought medical attention due to a progressive increase in weight, worsening dyspnea, and lower leg edema. According to her statement, there is no history of similar complaints in her family.
Clinical findings: upon admission, the patient was in a state of respiratory distress, seated on her bed, with an oxygen saturation level below 85%, a respiratory rate of 35 breaths per minute, and a blood pressure measuring 84/55 mmHg. Clinical examination revealed a slight goiter upon palpation, without any signs of compression, decreased breath sounds, and pitted edema in both lower legs.
Timeline: the patient was admitted to the hospital on January 26, 2023, due to dyspnea, hypotension, and swelling in both legs, with a normal heart rate. Upon admission, the chest X-ray showed a "water bottle-shaped" image of the heart, and the echocardiography revealed the presence of pericardial fluid and a collapsed right ventricle. Emergency pericardiocentesis was performed, and 1000 ml of fluid was drained using a pigtail drain. One day later, an additional 500 ml of fluid was drained. Two days later, 500-800 ml of fluid was drained until the fifth day. On the fifth day, the patient no longer experienced dyspnea, and a repeat echocardiography showed minimal pericardial fluid. The patient was discharged with a prescription for 75 �g of levothyroxine tablet therapy. Six months later, the patient came to control with no complaints, a repeat echocardiography showed a well-tolerated chronic pericardial effusion and thyroid hormone was in the normal range.
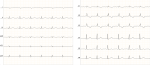
Diagnostic assessment: an electrocardiogram (ECG) indicated low-voltage ECG complexes, right axis deviation, incomplete right bundle branch block, and sinus rhythm, with a heart rate of approximately 80 beats per minute (Figure 1). A chest X-ray displayed a characteristic "water bottle-shaped" sign, suggesting the presence of pericardial effusion (Figure 2). Further assessment through transthoracic cardiac echocardiography (TTE) unveiled circumferential fibrinous pericardial effusion, along with signs of right ventricular collapse, while the left ventricular ejection fraction remained within the normal range (Figure 3). The laboratory test results revealed significant indicators of severe hypothyroidism, including a thyroid-stimulating hormone (TSH) level of 14.45 �U/mL, low FT4 at 1.46 ng/dL, TSH receptor antibody levels were measured at 5.13 IU/L, and highly elevated anti-thyroid peroxidase antibodies at 31.74 IU/mL, all indicative of Hashimoto's thyroiditis. Renal function parameters, including creatinine at 0.59 mg/dL and urea concentration at 13 mg/dL, were within the normal range. There is no evidence of tuberculosis, cancer, or lupus in the patient. The sputum test of tuberculosis, antinuclear antibody test, and pathological anatomic measure were all negative. Additionally, cytological analysis of the pericardial fluid revealed an inflammatory response with no presence of malignant cells.
Therapeutic intervention: to alleviate the condition, a percutaneous pericardiocentesis procedure was carried out through subxiphoid access with a pericardiocentesis kit, guided by echocardiographic. Approximately 3000 ml of pale red fluid was successfully drained slowly at a rate of 500-1000 cc per day for five days, leading to improvement in the patient's clinical condition. The echocardiography follow-up after pericardiocentesis showed improvement in the right ventricle, and there was only a mild pericardial fluid (Figure 4). The patient was also given levothyroxine 75 μg tablets for her hypothyroidism therapy. A follow-up echocardiography six months later indicated the presence of a well-tolerated chronic pericardial effusion.
Follow-up and outcomes: the patient showed significant improvement after undergoing pericardiocentesis and receiving levothyroxine hormone therapy.
Patient perspective: the patient expressed immense satisfaction and gratitude, as after one week of hospital treatment, their initial severe shortness of breath complaint disappeared. Additionally, the pericardial fluid has significantly reduced, and the patient's thyroid hormone levels are now well-regulated with the prescribed medications.
Informed consent: a written informed consent was obtained from the patient for the publication of patient data and accompanying images.
Hashimoto's thyroiditis, an autoimmune thyroid disorder, often leads to gradual and nonspecific symptoms of hypothyroidism, which can go unnoticed for an extended time. Diagnosis may be delayed, and in rare cases, patients can experience life-threatening emergencies like cardiac tamponade. Although mild pericardial effusion is common in hypothyroidism, moderate to severe cases are rare, and cardiac tamponade due to pericardial effusion is extremely uncommon. Prompt recognition of hypothyroidism and the initiation of levothyroxine treatment are crucial for effective management [7].
Hypothyroidism affects various organ systems with varying manifestations depending on factors like its cause, duration, and extent. It primarily impacts the cardiovascular system, leading to bradycardia, diastolic hypertension, a narrow pulse pressure, and reduced pericardial activity. While ventricular arrhythmias are common, heart failure is rare due to the generally lowered cardiac output meeting reduced oxygen demands [8].
The incidence of pericardial effusion in hypothyroidism varies from 3% in mild cases to 80% in severe cases [3]. It results from increased capillary permeability, reduced lymphatic clearance, and enhanced salt and water retention. Cardiac tamponade, a rare complication of hypothyroidism, typically occurs in severe and long-standing cases. Although most patients seek medical attention before this stage, in rare instances, hypothyroidism can initially present with cardiac tamponade. Diagnosis is confirmed through echocardiography, and treatment involves pericardiocentesis and levothyroxine replacement therapy [9,10].
Electrocardiogram (ECG) findings can aid in diagnosis, with hypothyroidism commonly showing sinus bradycardia and prolonged QTc intervals. In contrast, cardiac tamponade often presents with sinus tachycardia, electrical alternans, and low-voltage QRS complexes. The presence of bradycardia or normal heart rate in cardiac tamponade suggests hypothyroidism as a potential cause. Chest radiogram showed cardiomegaly with globular enlargement of the cardiac silhouette with a “water bottle-shaped” configuration. Echocardiographic findings in cardiac tamponade include massive pericardial effusion and chamber collapse. Pericardial fluid in hypothyroidism is typically golden-colored, exudative with a high protein content, and predominantly contains lymphocytes [5]. Emergency pericardiocentesis is required for patients with cardiac tamponade, along with levothyroxine replacement therapy. Pericardial effusion typically resolves over 3 to 6 months with treatment [4].
Severe hypothyroidism can cause pericardial effusion, but it is a rare cause of massive pericardial effusion leading to tamponade. Therefore, it is important to monitor the heart condition of patients with hypothyroidism continuously using echocardiography until they have euthyroid.
The authors declare no competing interests.
Patient management: Muhammadnur Rachim Enoch and Rachmad Budianto. Data collection: Muhammadnur Rachim Enoch and Muhammad Irfan. Manuscript drafting: Muhammad Irfan. Manuscript revision: Muhammadnur Rachim Enoch, Muhammad Irfan, Rachmad Budianto and Achmad Hardin. All the authors have read and agreed to the final manuscript.
Figure 1: the ECG showing normal sinus rhythm with low voltage, right axis deviation (RAD), and incomplete right bundle branch block (RBBB)
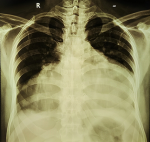
Figure 2: chest radiogram showing cardiomegaly with globular enlargement of the cardiac silhouette with “water bottle” configuration
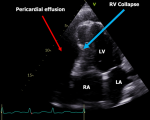
Figure 3: a two-dimensional transthoracic echocardiography reveals a significant pericardial effusion surrounding the heart; the red arrow indicates the effusion, while the blue arrow indicates right ventricular (RV) collapse; (LV: left ventricular, LA: left atrium, RA: right atrium)
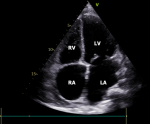
Figure 4: the follow-up echocardiography after pericardiocentesis
- Udovcic M, Pena RH, Patham B, Tabatabai L, Kansara A. Hypothyroidism And The Heart. Meth Deb Car J. 2017 Apr-Jun;13(2):55-59. PubMed | Google Scholar
- Chiu MH, Sharma NC. A case of hypertensive emergency, primary hypothyroidism and large pericardial effusion with early tamponade. J Cardiol Cases. 2018 Apr 26;18(1):29-32. PubMed | Google Scholar
- Sinha A, Yeruva SLH, Kumar R, Curry BH. Early cardiac tamponade in a patient with postsurgical hypothyroidism. Case Rep Cardiol. 2015:2015:310350. PubMed | Google Scholar
- Bajaj R, Mehrzad R, Singh K, Gupta JP. Cardiac tamponade in hypothyroidism. BMJ Case Rep. 2014 May 26:2014:bcr2014204076. PubMed | Google Scholar
- Baldwin C, Newman JD, Vallejo F, Peck V, Greene LW, Goldberg IJ. Myxedema heart and pseudotamponade. J Endocr Soc. 2020 Aug 27;5(1):bvaa125. PubMed | Google Scholar
- Butala A, Chaudhari S, Sacerdote A. Cardiac tamponade as a presenting manifestation of severe hypothyroidism. BMJ Case Rep. 2013 Feb 5:2013:bcr2012005281. PubMed | Google Scholar
- Chahine J, Ala CK, Gentry JL, Pantalone KM, Klein AL. Pericardial diseases in patients with hypothyroidism. Heart. 2019 Jul;105(13):1027-1033. PubMed | Google Scholar
- Layal C, Antonio CB, Jacqueline J, Peeters RP. Hypothyroidism. Lancet. 2017 Sep 23;390(10101):1550-1562. PubMed
- Maddali VR, Miryala S, Bellamkonda YS, Nagula P. Cardiac tamponade due to primary hypothyroidism: Acute management and approach to prevent recurrence - A case report. Eur Heart J Case Rep. 2020 May 3;4(3):1-5. PubMed | Google Scholar
- Bahrani S, Emami SA, Vakhshoori M, Siavash M, Kiani K, Mahmoudi F et al. Primary hypothyroidism leading to massive pericardial effusion and diastolic right ventricular compression: A case report SN Compr Clin Med. 2019;1:924-927. Google Scholar