Adolescents´ exposure to secondhand smoke and its association with susceptibility to smoking and mental health in Lagos, Nigeria
Afolabi Oyapero, Olufemi Erinoso, Olubukola Olamide Olatosi
Corresponding author: Afolabi Oyapero, Department of Preventive Dentistry, Lagos State University College of Medicine, Lagos, Nigeria 
Received: 19 Jun 2022 - Accepted: 08 Apr 2023 - Published: 26 Apr 2023
Domain: Environmental health,Non-Communicable diseases epidemiology,Community health
Keywords: Anxiety, depression, secondhand smoke, smoking susceptibility, tobacco
©Afolabi Oyapero et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Afolabi Oyapero et al. Adolescents´ exposure to secondhand smoke and its association with susceptibility to smoking and mental health in Lagos, Nigeria. Pan African Medical Journal. 2023;44:202. [doi: 10.11604/pamj.2023.44.202.35973]
Available online at: https://www.panafrican-med-journal.com//content/article/44/202/full
Research 
Adolescents´ exposure to secondhand smoke and its association with susceptibility to smoking and mental health in Lagos, Nigeria
Adolescents´ exposure to secondhand smoke and its association with susceptibility to smoking and mental health in Lagos, Nigeria
![]() Afolabi Oyapero1,&,
Afolabi Oyapero1,&, ![]() Olufemi Erinoso2,
Olufemi Erinoso2, ![]() Olubukola Olamide Olatosi3
Olubukola Olamide Olatosi3
&Corresponding author
Introduction: this study assessed the relationship between exposure to secondhand smoking (SHS) and its association with self-reported anxiety, depression and susceptibility to smoking among adolescents in Lagos, Nigeria.
Methods: depression among study subjects was determined using the Patient Health Questionnaire-9 (PHQ-9) while the Generalized Anxiety Disorder - 7 (GAD-7) was used to determine anxiety levels. Susceptibility to smoking cigarettes was also determined while the Statistical Package for the Social Science (SPSS) 26.0 software was used for data analysis. Significant associations were determined at P-values <0.05.
Results: of the 300 adolescents surveyed (mean age 12.9±1.43), 7.6 % were regularly exposed to SHS, of which 3.0% were daily exposed to SHS indoors. In multivariable analyses, indoor SHS exposure for ≥ 1 hour daily was associated with increased odds for susceptibility to smoking (AOR=3.793; 95%-CI: 0.98-14.60; p= 0.052) and increased odds for depression (AOR=1.303; 95%-CI: 0.84-2.01; p= 0.228) and slightly reduced odds for anxiety (AOR=0.952; 95%-CI: 0.62-1.47; p=0.822).
Conclusion: secondhand smoking exposure was associated with higher odds of susceptibility to smoking cigarettes and depression among adolescents exposed to SHS, especially among females living in cramped accommodations. Further validation of these findings should however be determined by cohort study designs.
Secondhand smoke (SHS) is the inadvertent inhaling of tobacco smoke by those who are not active smokers. It consists of the mainstream smoke inhaled by a smoker [1] and side stream smoke with a higher concentration of toxins and carcinogens [2]. The noxious chemicals in SHS include polycyclic aromatic hydrocarbons, nitrosamines, tar and carbon monoxide, carbonyls [3]. The harmful effects of SHS on adults, children, pregnant women and their fetuses has been extensively documented by many researchers with sufficient evidence to infer a causal relationship [4-6]. These harmful effects of exposure to SHS [7] include fetal DNA damage, low birth weight, childhood respiratory infections, asthma, lower levels of breast-feeding, poorer academic performance, lung cancer, coronary heart disease and malignancies [8-10]. This range of health consequences can also significantly impact adolescents. Adolescence is a period of significant physical, psychological and social transitions as well as vulnerability to environmental stresses. During this period, the adolescent develops enhanced cognitive functions in areas such as decision-making and impulse control. In addition to tobacco smoke, SHS is one of the potential hazards that could potentially impact on adolescents´ health and well-being. Global reports from tobacco monitoring agencies have documented that 10% of adolescents are exposed to SHS in residential areas and in the public [11]. Similarly, a nationwide survey conducted among adolescents in US in 2017 reported an annual increase in SHS, with over 55% of them being exposed [12]. Thus, the potential adverse effect of SHS on their physical and psychological well-being necessitates adequate investigation. The negative impact of SHS on mental health is postulated to occur through the dopaminergic systems and the initiation of chronic stress [13,14]. Some studies have demonstrated the effects of SHS on the incidence of depressive symptoms [15-18]. While some reported significantly positive associations, [15,16] others observed weak associations [17,18]. Recently, a study of Chinese adolescents documented that SHS exposure for more than 5 days a week doubled the risk of depression among them [19]. These findings are important because depression in childhood predisposes to recurrent depression, alcoholism and suicidal tendencies [20], as well as somatic illnesses [21]. Furthermore, depressive disorders in adolescence is strongly correlated with depression in adulthood [20]. There is also a possibility that adolescents exposed to SHS could initiate the smoking habit since most smokers started the habit during adolescence and became more prone to heavy smoking in adulthood, often finding it difficult to quit [22]. Previous metanalysis have established the association between exposure to secondhand smoking and depressive symptoms among in-school adolescents and also among pregnant women [23,24].
Susceptibility to smoking, a tool developed by Pierce et al. [25] has been validated for identifying adolescents who are likely to initiate the smoking habit. Exposure to SHS has been identified as a risk factor that can increase susceptibility to cigarette smoking as well as nicotine dependence [26]. The importance of susceptibility to smoking within the developmental context of adolescence is very noteworthy, because of the role of behavioral intentions in predicting future behavior [27]. Researchers have previously documented that a very high proportion of adolescents who smoke live in low- and middle-income countries (LMICs) [28]. This is troubling, since the initiation of tobacco smoking during early adolescence is strongly correlated with persistent smoking during adulthood [29]. Inadequate attention has been given to the exposure of adolescents to SHS in Nigeria and its effect on their mental health and susceptibility to uptake of the smoking habit [30]. Studies among adolescents are crucial, because the developing brain of adolescents is particularly susceptible to substances found in SHS [31]. Secondly, data from LMICs are scarce. This is omission is not acceptable because the enforcement of tobacco control policy legislation is very weak in LMICs, compared with high-income countries [32]. This study thus aimed to determine the relationship between exposure to SHS and self-reported anxiety, depression and susceptibility to smoking among adolescents in Lagos, Nigeria.
Study design and settings: this descriptive study was conducted between April and July 2021, in Lagos State, Nigeria. The population of Lagos State is about 20 million people, who are widely distributed in several rural and urban communities. It is a densely populated State and almost half of the commercial activities in the country take place in the city. Lagos State has one of the largest private basic education services globally and private schools provide services for almost 60% of the students in the state.
Study participants and sampling method: data were collected using randomly selected sample of Nigerian adolescents aged between 12 to 17 years. A multi-stage random sampling method was utilized to enlist the study participants. A simple random technique by balloting method was used to select 2 LGAs (Ikorodu and Ikeja) in the first stage. At the second stage, a sampling frame of secondary educational institutions was obtained from the Lagos State Ministry of Education website and two schools in each LGA were randomly selected by balloting. The third stage involved selection of eligible classes in the schools by simple random sampling. Children who met the eligibility criteria for the study were enlisted proportionally in each school using a table of random numbers with the class nominal roll serving as a sampling frame.
Sample size calculation: the minimum sample size was obtained using the formula for cross-sectional studies below:
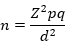
Where: n= minimum sample size for the study; Z= 1.96 at 95% confidence level and p= proportion of adolescents who were exposed to SHS; q= 1-p; and d= acceptable margin of error of 5% precision. Using a prevalence of 15.5% for household exposure to SHS in a previous study [33]. n= (1.96)2 x 0.15 x 0.85= 3.841 x 0.15 x 0.85 =196. Provision for incomplete responses of 20% gave a final sample size of 274 respondents.
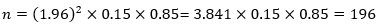
Inclusion criteria: these included students attending junior and senior secondary schools, aged between 12 -17 years, with no history of tobacco use; those who gave their assent (for pupils aged 12 years), gave their consent (for students 13 years and older) and had parental consent (for all students) were selected for the study.
Exclusion criteria: students who were less than 12 years or more than 17 years of age; those that withheld their assent or consent and those without parental consent; physically, mentally or medically challenged pupils, as well as those who had any history of personal tobacco use, were also excluded from the study.
Data collection tool: a validated interviewer administered questionnaire which was partly modified from the Global Youth Tobacco Survey (GYTS) version 1.2 2014 was utilised. It obtained sociodemographic information, history of exposure to SHS, assessment of depression with the Patient Health Questionnaire-9 (PHQ-9), assessment of anxiety with the Generalized Anxiety Disorder - 7 (GAD-7) and susceptibility to smoking cigarettes. Section A); determined the socio-demographic characteristics of the participants. Section B); comprised questions about the smoking behaviour of parents and household members as well as the child´s exposure to SHS. The independent variable was SHS exposure, and this was assessed with the following questions: a) ´Within the previous seven days, did someone smoke cigarettes indoors in your home with you present?´ and b) ´Within the previous seven days, did anyone smoke in your presence at any other location apart from your home?´.Those who responded �0 days´ were categorized as unexposed to SHS, while those who responded: ´1-2 days´, ´3-4 days´, ´5-6 days´ and ´all seven days´ were categorized as exposed to SHS. In Section C, the 7-item GAD-7 scale, was used to assess self-reported symptoms and severity of anxiety respectively. The total scores of GAD-7 were categorized as normal (0-5), mild (6-10), moderate to severe (≥11) anxiety. The PHQ-9, a 9-item self-report questionnaire was used to assesses depression symptoms and severity in Section D. The PHQ-9 questionnaire was scored from 0 to 27, with higher scores indicating more severe depressive symptoms. The total score was interpreted as indicating none-minimal depression (score 0-4), mild depression (score 5-9), moderate depression (score 10-14), or moderately severe depression (score 15-19), and severe depression (score 20-27). In Section E; susceptibility to smoking cigarettes, indicated by the lack of a strong choice to abstain from smoking, was assessed using a composite index of three questions: a) if a friends gave you a cigarette, would you smoke it?; b) are you likely to smoke a cigarette at any time within the next year? and c) How likely is it that you will be smoking cigarettes by the time you are 18 years old? Any response other definitely not to any of the three items indicated that the respondent is susceptible.
Statistical analysis: statistical analysis was conducted with SPSS version 26.0 software (Version 26.0. Armonk, NY: IBM Corp). Descriptive statistics were presented as frequencies and percentages while bivariate associations were analyzed using chi-squared and Anova tests. Bivariate and multivariate logistic regression analysis was done using sociodemographic variables and exposure to SHS as the predictor variables to identify outcome variables of interest which were self-reported anxiety, depression and susceptibility to smoking. Statistical significance was determined at p values <0.05.
Ethical aspects: ethical approval was obtained from the Health Research and Ethics Committee of the Lagos State University Teaching Hospital (Approval number: LREC/06/10/1798) and informed assent and consent was obtained from participants.
Characteristics of participants are summarized in Table 1. Of the 300 adolescents surveyed (mean age 12.9±1.43), 66 (22%) were exposed to SHS of which 34 (11.4%) were rarely exposed, 23 (7.6%) were often exposed while 9 (3.0%) of the children were daily exposed to SHS indoors. In the bivariate analysis, females (p=0.022), those living in cramped accommodations (p=0.020), and those <5 years of age when their caregivers started smoking indoors (p=0.001) had significantly higher odds of exposure to SHS (Table 1). Table 2 shows the bivariate association between secondhand smoke exposure, anxiety, depression and susceptibility to smoking among the study participants. The prevalence of self-reported anxiety and depression (from mild to severe) were 29.6% and 11.0% respectively while the prevalence of susceptibility to smoking was 16.2%. Adolescents who were exposed to SHS were significantly more likely to report depressive symptoms (p=0.050), while those who lived in cramped accommodations (p=0.023) and those who were exposed to SHS (p=0.041), were significantly more likely to report susceptibility to smoking. In multivariable analyses, indoor SHS exposure for ≥ 1 hour daily was associated with increased odds for susceptibility to smoking (AOR=3.793; 95%-CI: 0.98-14.60; p= 0.052) and increased odds for anxiety (AOR=1.303; 95%-CI: 0.84-2.01; p= 0.228) and slightly reduced odds for depression (AOR=0.952; 95%-CI: 0.62-1.47; p= 0.822) (Table 3). Table 4 displays the predictors of susceptibility to smoking cigarettes among the sampled adolescents. There was a significant association (p<0.05) between the type of accommodation (AOR: 1.40; CI: 1.037-3.079), severe depression (AOR: 2.7; CI: 1.531-5.473) having a parent that smoke (AOR: 2.76; CI: 2.506- 9.709) and having parents smoking cigarettes indoors (AOR: 4.85; CI: 3.590-21.246) with increased susceptibility to smoking among the adolescents. There were also increased odds of susceptibility to smoking among those whose mother (AOR: 1.30; CI: 0.702-3.824) and father (AOR: 2.12; CI: 0.819- 5.493) had <12 years of formal education, although, the association was not significant.
Secondhand smoke contains the same injurious chemicals inhaled by active smokers, thus those who are exposed to it encounter a comparable hazard [33,34]. Of the 300 adolescents surveyed in this study, 22% were exposed to SHS of which 11.4% were rarely exposed, 7.6% were often exposed while 3.0% of the adolescents were daily exposed to SHS indoors. This finding is comparable to the figures presented by Centers for Disease Control and Prevention (CDC) which showed that almost 50% of young adolescents are exposed to SHS at home [35]. Of the six WHO regions, the European Region (77.8%) had the highest level of exposure to SHS while the African region (27.6%) had the lowest. The prevalence of self-reported anxiety and depression (from mild to severe) among the adolescents was 29.6% and 11.0% respectively. Depression is one of the most common mental health problems, with an estimated 350 million people affected globally [36]. The findings from this study agrees with that reported by the World Health Organization which documented the prevalence of depression among adolescents around the world as between 5-10% [37]. Furthermore, the prevalence of susceptibility to smoking was 16.2%. This figure is slightly lower than that obtained from that of a US National survey of teens which obtained a prevalence of 22% for females and 23% for males [38]. In the non-smoking population, susceptibility is an initial phase in a sequence of cognitive changes, which ultimately progresses into experimentation with cigarettes, steady smoking, and eventually addiction to tobacco. Hence, any intervention that addresses this crucial first stage of susceptibility, will likely result in a reduction in the uptake of cigarettes by a significant proportion of youth [38]. In the bivariate analysis, females, those living in cramped accommodations and those who were less than 5 years of age when their caregivers started smoking indoors had significantly higher levels of exposure to SHS. The intensity of exposure to SHS and the number of individuals residing in an accommodation have a direct dose-response relationship [39]. The primary source of exposure to SHS for children living with adult smokers in cramped households is the mainstream and side stream smoke [39]. Secondhand smoke exposure was associated with slightly reduced odds for anxiety in this study but 1.3 increased odds for depression. Some authors have observed an augmented risk for anxiety with tobacco smoking [40] while quitting smoking was associated with a reduction in this risk [41]. In a study conducted by Amering et al., it was reported that 72% of panic disorder patients stated that they were regular smokers at the onset of their condition [42]. A previous study using US National Health and Nutrition Examination Survey data reported that SHS exposure was positively associated with major depressive disorder, generalized anxiety disorder and attention-deficit/hyperactivity disorder in adolescents [43]. Adolescents with higher frequency of SHS have also been found to be more likely to report depressive symptoms [19]. In addition, a 12-year population-based follow-up study observed that suicide mortality was higher in adolescents exposed to secondhand smoke, even with mild exposure [44].
There are numerous likely mechanisms for the association of SHS exposure with depressive symptoms even though the direction of the association and potential underlying mechanisms are not fully understood. SHS comprises electrophiles, free radicals, and metal ions that act as oxidizing or reducing agents that alter the body´s pro- anti-oxidant balance, leading to potential damage in biological molecules. Free radicals in tar such as hydroquinone and catechol can also induce oxidative stress in cells. SHS exposure also elevates the levels of adrenocorticotropic hormones which are related to mood and behavior [45-47]. Exposure to SHS in stressful states is likewise associated with an increased risk for negative lifestyle and behavioral problems such as emotional disorders at a young age [46]. Adolescent depression is an antecedent of many adverse outcomes in adulthood, and globally imposes a significant economic burden not only on individuals with the condition, but also on their families and communities [48]. Those who were exposed to SHS, were also significantly more likely to report susceptibility to smoking. Also, there was a significant association between living in a cramped accommodation, severe depression, having a parent that smokes and having parents smoking cigarettes indoors with increased susceptibility to smoking among the adolescents. In multivariable analyses, indoor SHS exposure for ≥ 1 hour daily was associated with 3.79 increased odds for susceptibility to smoking. A review of research has found that children exposed to smoking are significantly more likely to take up smoking themselves [49]. This was in agreement with a previous study that documented that children whose parents smoked were at a three-fold increased risk of smoking uptake. Children were further found to be over 70% more likely to start smoking if just one parent smoked, and over twice as likely if that parent was the mother [50].
Previous review studies have demonstrated an association between SHS exposure and smoking uptake [51]. Prior research has indicated that smoking susceptibility is a significant independent predictor of future initiation into tobacco use and that SHS could influence tobacco use and smoking behaviors [52]. Secondhand Smoke, through repeated nicotine exposure, can induce tolerance to nicotine´s adverse effects, resulting in nicotine-induced behavioral changes [53]. Close to a hundred thousand young people commence the smoking habit daily and most of them are from LMICs and pre-adolescent [54]. Adolescents who smoke are 3 times more like than nonsmokers to use alcohol, 8 times more likely to use marijuana and 22 times more likely to use cocaine. The present study suggests a positive association between SHS exposure with increased susceptibility to smoking, slightly reduced odds for anxiety but increased odds for depression. Evidence shows that smoking cessation is associated with reduction in depression, anxiety and stress and improved quality of life for people with mental health conditions and those without [55]. Cigarette smoke contains many substances that may either directly (free radicals) or indirectly (metals) exert negative effects on stress pathways, immune and mitochondrial functions, and also possibly influence neurodevelopmental and subsequent anxiety risk. Anti-tobacco messages (ATM) have primarily communicated the physical risks of smoking [56] and further cohort studies on this crucial research question may confirm the need to expand these messages to include the mental health risks of tobacco use, such as “SHS exposure is associated with increased risk of anxiety”. There are however some limitations associated with this study. Firstly, access to direct measures and biological indicators such as serum cotinine, urinary cotinine, serum carboxyhemoglobin or household air nicotine levels could have provided more valid evidence of levels of SHS exposure. Secondly, we are unable to determine the direction of the association since some parents who are smokers may have higher rates of depression, triggering indirect psychological impacts on their children who were similarly exposed to SHS. Moreover, other confounding indicators that could be associated with anxiety, depression and susceptibility to smoking such as alcohol consumption, illicit drug use, and intrapersonal factors such as stress were not determined. This baseline study however provides very important baseline data for further analytical studies.
Secondhand smoke exposure in this study was associated with higher odds of susceptibility to smoking cigarettes and depression among adolescents exposed to SHS, especially among females, those living in cramped accommodations, having parents smoking cigarettes indoors and having poorly educated parents. Further validation of this findings should however be determined by cohort study designs.
What is known about this topic
- Secondhand smoke (SHS) exposure is one of the important risk factors that might increase susceptibility to smoking and nicotine dependence among those who have begun smoking; the importance of susceptibility to smoking within the developmental context of adolescence is significant given the role of behavioural intentions in predicting future behaviour;
- Previous research has shown that a disproportionate number of those aged 15 years and over who smoke (approximately 80%) live in LMICs.
What this study adds
- This article scientifically presents data on the prevalence of mental health problems associated with SHS exposure;
- Secondhand smoke exposure in this study was associated with slightly reduced odds for anxiety in this study but 1.3-fold increased odds for depression;
- Those who were exposed to SHS, were also significantly more likely to report susceptibility to smoking; also there was a significant association between living in a cramped accommodation, having a parent that smokes and having parents smoking cigarettes indoors with increased susceptibility to smoking among the adolescents.
The authors declare no competing interests.
All the authors have read and agreed to the final version of this manuscript.
Table 1: association between secondhand smoke exposure and socio-demographic characteristics of respondents
Table 2: association between anxiety, depression, susceptibility to smoking and the socio-demographic characteristics of respondents
Table 3: multivariable association between secondhand smoke exposure, anxiety, depression and susceptibility to smoking
- United States Environmental Protection Agency. Respiratory health effects of passive smoking; lung cancer and other disorders. EPA. 1992.
- Hoffmann D, Hoffmann I. Significance of exposure to sidestream tobacco smoke. IARC Sci Publ. 1987;(81):3-10. PubMed | Google Scholar
- Raghuveer G, White DA, Hayman LL, Woo JG, Villafane J, Celermajer D et al. Cardiovascular consequences of childhood secondhand tobacco smoke exposure: Prevailing evidence, burden, and racial and socioeconomic disparities: A scientific statement from the American Heart Association. Circulation. 2016 Oct 18;134(16):e336-e359. PubMed | Google Scholar
- Besaratinia A, Pfeifer GP. Second-hand smoke and human lung cancer. Lancet Oncol. 2008 Jul;9(7):657-66. PubMed | Google Scholar
- Bloch M, Althabe F, Onyamboko M, Kaseba-Sata C, Castilla EE, Freire S et al. Tobacco use and secondhand smoke exposure during pregnancy: an investigative survey of women in 9 developing nations. Am J Public Health. 2008 Oct;98(10):1833-40. PubMed | Google Scholar
- Herrmann M, King K, Weitzman M. Prenatal tobacco smoke and postnatal secondhand smoke exposure and child neurodevelopment. Curr Opin Pediatr. 2008 Apr;20(2):184-90 PubMed | Google Scholar
- Department of Health, Human Services. The health consequences of involuntary exposure to tobacco smoke: a report of the surgeon general. Atlanta GA USA; HHS, CDC, CCHP, NCCDPHP, OSH. 2006. Google Scholar
- Chou SY, Hsu HH, Kuo HH, Kuo HW. Association between exposure to environmental tobacco smoke (ETS) and breastfeeding behaviour. Acta Paediatr. 2008 Jan;97(1):76-80. PubMed | Google Scholar
- Collins BN, Wileyto EP, Murphy MF, Munaf� MR. Adolescent environmental tobacco smoke exposure predicts academic achievement test failure. J Adolesc Health. 2007 Oct;41(4):363-70. PubMed | Google Scholar
- Cutler-Triggs C, Fryer GE, Miyoshi TJ, Weitzman M. Increased rates and severity of child and adult food insecurity in households with adult smokers. Arch Pediatr Adolesc Med. 2008 Nov;162(11):1056-62. PubMed | Google Scholar
- Chen PL, Weigang Huang, Chuang YL, Warren CW, Jones NR, Lee J et al. Exposure to and attitudes regarding secondhand smoke among secondary students in Taiwan. Asia Pac J Public Health. 2009 Jul;21(3):259-67. PubMed | Google Scholar
- Gentzke AS, Wang TW, Marynak KL, Trivers KF, King BA. Exposure to secondhand smoke and secondhand e-cigarette aerosol among middle and high school students. Prev Chronic Dis. 2019 Apr 4;16:E42. PubMed | Google Scholar
- Serafini G, Hayley S, Pompili M, Dwivedi Y, Brahmachari G, Girardi P et al. Hippocampal neurogenesis, neurotrophic factors and depression: Possible therapeutic targets? CNS Neurol Disord Drug Targets. 2014;13(10):1708-21. PubMed | Google Scholar
- Iñiguez SD, Warren BL, Parise EM, Alcantara LF, Schuh B, Maffeo ML et al. Nicotine exposure during adolescence induces a depression-like state in adulthood. Neuropsychopharmacology. 2009 May;34(6):1609-24. PubMed | Google Scholar
- Ye X, Li L, Gao Y, Zhou S, Yang Y, Chen S. Dose-response relations between second-hand smoke exposure and depressive symptoms among middle-aged women. Psychiatry Res. 2015 Sep 30;229(1-2):533-8. PubMed | Google Scholar
- Huang J, Wen G, Yang W, Yao Z, Wu C, Ye X. The association between second-hand smoke exposure and depressive symptoms among pregnant women. Psychiatry Res . 2017 Oct;256:469-474. PubMed | Google Scholar
- Bauer NS, Anand V, Carroll AE, Downs SM. Secondhand smoke exposure, parental depressive symptoms and preschool behavioral outcomes. J Pediatr Nurs . 2015 Jan-Feb;30(1):227-35. PubMed | Google Scholar
- Michal M, Wiltink J, Reiner I, Kirschner Y, Wild PS, Schulz A et al. Association of mental distress with smoking status in the community: Results from the Gutenberg Health Study. J Affect Disord. 2013 Apr 25;146(3):355-60. PubMed | Google Scholar
- Huang J, Xu B, Guo D, Jiang T, Huang W, Liu G et al. Dose-response relationships between second-hand smoke exposure and depressive symptoms among adolescents in Guangzhou, China. Int J Environ Res Public Health. 2018 May 14;15(5):985. PubMed | Google Scholar
- Mullen S. Major depressive disorder in children and adolescents. Ment Health Clin. 2018 Nov 1;8(6):275-283. PubMed | Google Scholar
- Thapar A, Collishaw S, Pine DS, Thapar AK. Depression in adolescence. Lancet. 2012 Mar 17;379(9820):1056-67. PubMed | Google Scholar
- Yang X, Yan Z, Xu G, Tan Y, Zhu J. How secondhand smoke exposure affects tobacco use and smoking susceptibility of adolescents: Sex and school differences. Tob Induc Dis . 2021 Sep 1;19:68. PubMed | Google Scholar
- Suzuki D, Wariki WMV, Suto M, Yamaji N, Takemoto Y, Rahman MM et al. Association of secondhand smoke and depressive symptoms in nonsmoking pregnant Women: A systematic review and meta-analysis. J Affect Disord. 2019 Feb 15;245:918-927. PubMed | Google Scholar
- Jacob L, Smith L, Jackson SE, Haro JM, Shin JI, Koyanagi A. Secondhand smoking and depressive symptoms among in-school adolescents. Am J Prev Med. 2020 May;58(5):613-621. PubMed | Google Scholar
- Pierce JP, Choi WS, Gilpin EA, Farkas AJ, Merritt RK. Validation of susceptibility as a predictor of which adolescents take up smoking in the United States. Health Psychol. 1996 Sep;15(5):355-61. PubMed | Google Scholar
- Carey FR, Wilkinson AV, Harrell MB, Cohn EA, Perry CL. Measurement and predictive value of susceptibility to cigarettes, e-cigarettes, cigars, and hookah among Texas adolescents. Addict Behav Rep. 2018 Aug 18;8:95-101. PubMed | Google Scholar
- Albarracin D, Ajzen I. Predicting and changing behavior: A reasoned action approach. Prediction and Change of Health Behavior: Applying the Reasoned Action Approach. Lawrence Erlbaum Associates, Mahwah, NJ. 2007:3-21. Google Scholar
- Action on Smoking and Health. ASH fact sheet: tobacco and the developing world. ASH. Accessed on 22nd October, 2022.
- Reidpath DD, Davey TM, Kadirvelu A, Soyiri IN, Allotey P. Does one cigarette make an adolescent smoker, and is it influenced by age and age of smoking initiation? Evidence of association from the U.S. Youth Risk Behavior Surveillance System (2011). Prev Med. 2014 Feb;59:37-41. PubMed | Google Scholar
- Han C, Liu Y, Gong X, Ye X, Zhou J. Relationship between secondhand smoke exposure and depressive symptoms: a systematic review and dose-response meta- analysis. Int J Environ Res Public Health. 2019 Apr 15;16(8):1356. PubMed | Google Scholar
- Yuan M, Cross SJ, Loughlin SE, Leslie FM. Nicotine and the adolescent brain. J Physiol. 2015;593(16):3397-3412. PubMed | Google Scholar
- Stone E, Peters M. Young low and middle-income country (LMIC) smokers-implications for global tobacco control. Transl Lung Cancer Res. 2017 Dec;6(Suppl 1):S44-S46. PubMed | Google Scholar
- Oyapero A, Erinoso O, Olatosi OO. Second-Hand Tobacco Smoke Exposure in Children: A Neglected Driver of Health Disparities and Social Injustice in Nigeria. West Afr J Med. 2021 Dec 30;38(12):1216-1223. PubMed | Google Scholar
- Kim SJ, Han KT, Lee SY, Chun SY, Park EC. Is secondhand smoke associated with stress in smokers and non-smokers? BMC Public Health. 2015 Dec 17;15:1249. PubMed | Google Scholar
- Centers for Disease Control and Prevention. Global Youth Tobacco Surveillance, 2000-2007. MMWR Surveill Summ. 2008 Jan 25;57(1):1-28. PubMed | Google Scholar
- Yolton K, Xu Y, Khoury J, Succop P, Lanphear B, Beebe DW et al. Associations between secondhand smoke exposure and sleep patterns in children. Pediatrics. 2010 Feb;125(2):e261-8. PubMed | Google Scholar
- World Federation for Mental Health. Depression: a global crisis. WFHM. 2012.
- Leatherdale ST, McDonald PW, Cameron R, Jolin MA, Brown KS. A multi-level analysis examining how smoking friends, parents, and older students in the school environment are risk factor for susceptibility to smoking among non-smoking elementary school youth. Prev Sci. 2006 Dec;7(4):397-402. PubMed | Google Scholar
- Patra J, Bhatia M, Suraweera W, Morris SK, Patra C, Gupta PC et al. Exposure to second-hand smoke and the risk of Tuberculosis in children and adults: a systematic review and meta-analysis of 18 observational studies. PLoS Med. 2015 Jun 2;12(6):e1001835. PubMed | Google Scholar
- Erinoso O, Oyapero A, Osoba M, Amure M, Osibogun O, Wright K et al. Association between anxiety, alcohol, poly-tobacco use and waterpipe smoking: A cross-sectional study in Lagos, Nigeria. Niger Postgrad Med J. 2021 Apr-Jun;28(2):117-125. PubMed | Google Scholar
- Bakhshaie J, Zvolensky MJ, Goodwin RD. Cigarette smoking and the onset and persistence of depression among adults in the United States: 1994-2005. Compr Psychiatry. 2015 Jul;60:142-8. PubMed | Google Scholar
- Amering M, Bankier B, Berger P, Griengl H, Windhaber J, Katschnig H et al. Panic disorder and cigarette smoking behavior. Compr Psychiatry. 1999 Jan-Feb;40(1):35-8. PubMed | Google Scholar
- Bandiera FC, Richardson AK, Lee DJ, He J-P, Merikangas KR. Secondhand smoke exposure and mental health among children and adolescents. Arch Pediatr Adolesc Med. 2011 Apr;165(4):332-8. PubMed | Google Scholar
- Chen VC, Kuo CJ, Wang TN, Lee WC, Chen WJ, Ferri CP et al. Suicide and other-cause mortality after early exposure to smoking and second-hand smoking: a 12-year population-based follow-up study. PLoS On. 2015 Jul 29;10(7):e0130044. PubMed | Google Scholar
- Wang R, Zhang P, Lv X, Gao C, Song Y, Li Z et al. Association between passive smoking and mental distress in adult never-smokers: A cross-sectional study. BMJ Open. 2016 Jul 29;6(7):e011671. PubMed | Google Scholar
- Tweed JO, Hsia SH, Lutfy K, Friedman TC. The endocrine effects of nicotine and cigarette smoke. Trends Endocrinol Metab. 2012 Jul;23(7):334-42. PubMed | Google Scholar
- Gim W, Yoo J-H, Shin J-Y, Goo A-J. Relationship between Secondhand Smoking with Depressive Symptom and Suicidal Ideation in Korean Non-Smoker Adults: The Korean National Health and Nutrition Examination Survey 2010-2012.Korean J Fam Med. 2016 Mar;37(2):97-104. PubMed | Google Scholar
- Fergusson DM, Woodward LJ. Mental health, educational, and social role outcomes of adolescents with depression. Arch Gen Psychiatry. 2002 Mar;59(3):225-31. PubMed | Google Scholar
- Leonardi-Bee J, Jere ML, Britton J. Exposure to parental and sibling smoking and the risk of smoking uptake in childhood and adolescence: a systematic review and meta-analysis. Thorax. 2011 Oct;66(10):847-55. . PubMed | Google Scholar
- Wilkinson AV, Shete S, Prokhorov AV. The moderating role of parental smoking on their children's attitudes toward smoking among a predominantly minority sample: a cross-sectional analysis. Subst Abuse Treat Prev Policy. 2008 Jul 14;3:18. PubMed | Google Scholar
- Okoli CT, Kodet J. A systematic review of secondhand tobacco smoke exposure and smoking behaviors: Smoking status, susceptibility, initiation, dependence, and cessation. Addict Behav. 2015 Aug;47:22-32. PubMed | Google Scholar
- Lessov-Schlaggar CN, Wahlgren DR, Liles S, Ji M, Hughes SC, Winickoff JP et al. Sensitivity to secondhand smoke exposure predicts future smoking susceptibility. Pediatrics. 2011 Aug;128(2):254-62. PubMed | Google Scholar
- Solomon RL, Corbit JD. An opponent-process theory of motivation. II. Cigarette addiction. J Abnorm Psychol. 1973 Apr;81(2):158-71. PubMed | Google Scholar
- Lando HA, Hipple BJ, Muramoto M, Klein JD, Prokhorov AV, Ossip DJ et al. Tobacco is a global paediatric concern. Bull World Health Organ. 2010 Jan;88(1):2. PubMed | Google Scholar
- Taylor G, McNeill A, Girling A, Farley A, Lindson-Hawley N, Aveyard P. Change in mental health after smoking cessation: systematic review and meta-analysis. BMJ. 2014 Feb 13;348:g1151. PubMed | Google Scholar
- Oyapero A, Erinoso O, Osoba M, Amure M, Osibogun O, Wright KI et al. Exposure to Anti-Tobacco Messaging and Quit Attempts among Adolescent and Young Adult in Lagos, Nigeria: A Population-based Study. West Afr J Med. 2021 Nov 30;Vol. 38(11):1058-1064. PubMed | Google Scholar











