Understanding the role of serological and clinical data on assessing the dynamic of malaria transmission: a case study of Bagamoyo district, Tanzania
Tunu Guntram Mwamlima, Solomon Mickson Mwakasungula, Catherine Gerald Mkindi, Mgeni Mohamed Tambwe, Sarah Senyoni Mswata, Stephen Gabriel Mbwambo, Michael Fred Mboya, Simon John Draper, Sarah Elizabeth Silk, Maxmillian Gideon Mpina, John-Mary Vianney and Ally Ibrahim Olotu
Corresponding author: Tunu Guntram Mwamlima, Ifakara Health Institute, Bagamoyo, Tanzania 
Received: 04 Jun 2022 - Accepted: 01 Sep 2022 - Published: 07 Oct 2022
Domain: Public health
Keywords: Total immunoglobulins (IgG), Plasmodium. falciparum, anti-schizont antibodies, infants, clinical malaria, malaria transmission
©Tunu Guntram Mwamlima et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Tunu Guntram Mwamlima et al. Understanding the role of serological and clinical data on assessing the dynamic of malaria transmission: a case study of Bagamoyo district, Tanzania. Pan African Medical Journal. 2022;43:60. [doi: 10.11604/pamj.2022.43.60.35779]
Available online at: https://www.panafrican-med-journal.com//content/article/43/60/full
Research 
Understanding the role of serological and clinical data on assessing the dynamic of malaria transmission: a case study of Bagamoyo district, Tanzania
Understanding the role of serological and clinical data on assessing the dynamic of malaria transmission: a case study of Bagamoyo district, Tanzania
Tunu Guntram Mwamlima1,2,&, Solomon Mickson Mwakasungula1, ![]() Catherine Gerald Mkindi1, Mgeni Mohamed Tambwe1,Sarah Senyoni Mswata1, Stephen Gabriel Mbwambo1, Michael Fred Mboya3,
Catherine Gerald Mkindi1, Mgeni Mohamed Tambwe1,Sarah Senyoni Mswata1, Stephen Gabriel Mbwambo1, Michael Fred Mboya3, ![]() Simon John Draper4,
Simon John Draper4, ![]() Sarah Elizabeth Silk3, Maxmillian Gideon Mpina1,
Sarah Elizabeth Silk3, Maxmillian Gideon Mpina1, ![]() John-Mary Vianney2, Ally Ibrahim Olotu1
John-Mary Vianney2, Ally Ibrahim Olotu1
&Corresponding author
Introduction: naturally acquired blood-stage malaria antibodies and malaria clinical data have been reported to be useful in monitoring malaria change over time and as a marker of malaria exposure. This study assessed the total immunoglobulin G (IgG) levels to Plasmodium falciparum schizont among infants (5-17 months), estimated malaria incidence using routine health facility-based surveillance data and predicted trend relation between anti-schizont antibodies and malaria incidence in Bagamoyo.
Methods: 252 serum samples were used for assessment of total IgG by enzyme-linked immunosorbent assay and results were expressed in arbitrary units (AU). 147/252 samples were collected in 2021 during a blood-stage malaria vaccine trial [ClinicalTrials.gov NCT04318002], and 105/252 were archived samples of malaria vaccine trial conducted in 2012 [ClinicalTrials.gov NCT00866619]. Malaria incidence was calculated from outpatient clinic data of malaria rapid test or blood smear positive results retrieved from District-Health-Information-Software-2 (DHIS2) between 2013 and 2020. Cross-sectional data from both studies were analysed using STATA version 14.
Results: this study demonstrated a decline in total anti-schizont IgG levels from 490.21AU in 2012 to 97.07AU in 2021 which was related to a fall in incidence from 58.25 cases/1000 person-year in 2013 to 14.28 cases/1000 person-year in 2020. We also observed a significant difference in incidence when comparing high and low malaria transmission areas and by gender. However, we did not observe differences when comparing total anti-schizont antibodies by gender and study year.
Conclusion: total anti-schizont antibody levels appear to be an important serological marker of exposure for assessing the dynamic of malaria transmission in infants living in malaria-endemic regions.
Malaria is one of the vector-borne diseases of public health significance in sub-Saharan Africa, affecting largely under 5 years [1]. Deployment of the malaria control strategies such as insecticide-treated bed nets (ITNs) [2], indoor residual spraying (IRS) [2], artemisinin-based combination therapies (ACTs) [3], and intermittent presumptive treatment (IPT) [4] have all contributed to the 18% and 28% decline in global malaria cases and deaths respectively between 2010 and 2018 [5]. Nevertheless, the Word Malaria Report of 2021 indicated a slight increase in cases and deaths due to the covid-19 pandemic [6]. Although, the control measures played role in reducing malaria burden, those measures becomes vulnerable to parasite resistance [7,3], and vector resistant [7,8]. Therefore, new control interventions such as vaccines are crucial to complement the current strategies. Generally, vaccines are considered one of the most cost-effective public health intervention for diseases, and have contributed to the elimination of smallpox [9] and reduced childhood mortality [10]. The efficacy and immunogenicity of malaria vaccines candidates could be confounded by exposure [10,11] which modify immune responses [10,11]. Therefore, accounting for malaria exposure to an individual especially in randomized clinical trials that assess time to malaria infection [12] is crucial for improving vaccine efficacy [13].
Approaches for estimating malaria exposure to an individual includes entomological inoculation rates [14], prevalence of malaria within a defined radius of the index participant [15]. These approaches are labour intensive compared to the use of antibodies [16] which is less intensive, but could be influence by age [17] and gender [18]. Assessing antibody levels from historical samples alone to characterize the contemporaneous individual malaria exposure could provide imprecise estimates because malaria exposure correlates with antibody responses [19]. The level of accuracy will depend on how distant in time the historical samples came from, and the changes in malaria transmission during that period. This study, aimed to explore the use of serological data from vaccine trials [20] and archived clinical data from DHIS2 [21] in predicting a trend relation of anti-schizont antibody levels and malaria incidence in under five (infants inclusive) over 8 years period in Bagamoyo district.
Study area: serum samples and routine health care data were collected within the Bagamoyo district. According to the 2012 Tanzania National Census, the population of the Bagamoyo district was 311,740 [22].The humid tropical climate district has temperatures of 28�C-30�C, humidity up to 98%, and an average rainfall of 1200-2100 mm per year [23]. Rainy seasons occur between March-May and October-December creating temporary and permanent mosquito breeding water ponds that contribute to high malaria infectivity rates during these periods [22].
Health facility data: in 2014, Tanzania´s Health Management Information Systems (HMIS) under the ministry of health adopted the use of District Health Information Systems 2 (DHIS2) which is an integrated open-source and web-based platform that works to capture routinely collected data from health facilities [24]. Ten health facilities were selected from seven wards of low (Dunda, Magomeni, Zinga and Kisutu) and high (Fukayosi, Makurunge, and Yombo) malaria transmission areas. The characterization into low and high malaria transmission areas was based on both local/traditional categorization and previous epidemiological studies [25]. Simple random sampling was used to select health facilities for clinical data collection from the wards. Using the DHIS2 and register books, malaria data were retrieved for each selected health facility. The data retrieved included monthly malaria cases by age group (<5, >5-59 and 60+ years) and gender. Population size by age and gender for each ward over 8 years of follow-up was extracted from wards´ executive offices. A malaria case was defined as any patient with confirmed malaria, either by malaria rapid diagnostic test (mRDT) or by blood slide (BS). All health facilities were assumed to be operational throughout the period the data were collected. The DHIS2 data were retrieved, verified at the health facilities and any missed or inconsistence data in the DHIS2 were updated with the actual records from the source.
Study design: a cross-sectional study that involved collection of achieved and fresh serum samples from Bagamoyo Clinical Trial Facility of Ifakara Health Institute (BCTF-IHI) and a retrospective data collection from DHIS2.
Sample collection: convenient sampling was used to obtain serum samples for serological and simple random sampling for selecting health facility from which clinical data were retrieved. Serum samples for assessment of total IgGs to schizont were from two malaria vaccine trials that were conducted at two different time point from both low and high malaria transmission areas of Bagamoyo district council. 147 freshly collected infants´ serum samples were obtained during the screening process of a candidate blood-stage malaria vaccine trial (RH5.1/MM) conducted in 2021 [ClinicalTrials.gov NCT04318002] [26] and 105 achieved infants´ serum samples from archived malaria vaccine trial (RTS, S/AS01) conducted in 2012 [ClinicalTrials.gov NCT00866619] were obtained from the BCTF-IHI´s biobank. For assessment of total anti-schizont antibodies, malaria negative by BS or mRDT was an inclusion criterial. All samples were pseudo-anonymized to prevent attribution to participant-specific information. Only gender, age and location were extracted from the individual information.
Assessment of total IgG to schizont: Enzyme-Linked Immunosorbent Assay (ELISA) method described by Miura et al. [27] was used to determine serum antibody levels. Briefly, schizont extract from P. falciparum (3D7 clone produced by Ababacar Diouf, NIH) was used for plate coating as described elsewhere [28]. The stock concentration of 5x108 schizont extract /mL was diluted 1 in 1000 to obtain a working concentration of 5x10² schizont/µl using Dulbecco´s phosphate-buffered saline (DPBS) and 50µl of the mixture used for plate coating. ELISA plates were incubated overnight at 4�C to allow antigen binding, blocked by adding 100µl of 5% milk in DPBS and incubated for 1 hour before adding 50µL/well of serum samples, standards, and controls (diluted in 1% milk) in triplicate, and followed by a 2 hours incubation. Thereafter, 50µL of secondary antibody (goat anti-human IgG (γ-chain)) was added in each well, incubated for 1 hour and developed with 100µL/well of 1mg/ml developer solution (5x diethanolamine buffer in distilled water and 1x 20mg 4-nitrophenyl phosphate tablet). The plates were developed until assigned development endpoint reached. Extensive washing of ELISA plate was done after each incubation phase. To acquire Optical Density (OD), the plates were read on the Bio-Teck microplate ELx 808TM absorbance reader (Agilent Technologies, UK). ODs acquisitions were done using Gen5 software (Agilent Technologies, UK) at Ab405nm wavelength.
Assay quality control: assay control was performed as described by Miura et al. [27]. Positive control reference at 1 in 16000 dilutions with OD readings at Abs405nm threshold of average 0.8 minimum and 1.2 maximum were used. A 2-fold serially diluted standard curve was included in each run. Curve linear portion was Abs405nm threshold of average ~0.4 OD for lower limit and ~2.5 OD for upper limit, R² value was >0.994, coefficient of variation (CV) <20%. Blank wells (1% milk) provided Abs405nm threshold of average < 0.3 OD. Statistical analysis: data were entered in excel 2013 and imported to STATA version 14 (Stata Corp LP, Texas, USA) for analysis. Descriptive analysis presented median and standard deviation. Kruskal Wallis and Mann-Whitney U test compared median AU between the groups. Age was conveniently categorized into 0-5 months, 6-11 months, and 12-19 months groups, box plots were used for AU and line graphs for malaria incidence trend visualization [29].
Malaria incidences was calculated as follows [30]:
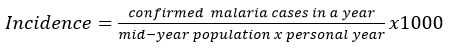
New cases were defined as the sum of all monthly reported cases in each year. Mid-year population size was defined as the annual mean population size in the areas where malaria cases were obtained. Total population in the health facilities catchment areas were considered at risk of clinical malaria and included in the analysis. Personal years were defined as the time each individual data collected in the study year [31].
Ethical considerations: the study received approval from the Ifakara Health Institute-Institutional Review Board (IHI/IRB/No: 49-2020 and 15-2020), National Institute for Medical Research ethical regulatory committee (NIMR/HQ/R.8a/Vol. IX/3537), Oxford Tropical Research Ethics Committee (OxTREC Reference: 9-20), Tanzania Medicines and Medical Devices Authority (Ref. No. TMDA0020/CTR/0005/2) and Local Government Authority (Kumb. Na. JC. 156/254/01).
Sampled population for anti-schizont antibody evaluation and for malaria incidence trend estimation
Samples were collected from infant studies conducted in 2012 and 2021. Table 1, shows the demographic information of the sampled population used for analyzing antibodies to P. falciparum schizont in infants and Table 2 shows distributions of malaria cases and incidence amongst age, gender and transmission variables.
Anti-schizont antibody distribution amongst age, gender and malaria transmission intensity
We showed evidence of a significant difference in levels of anti-schizont antibody when comparing levels by malaria transmission intensity (Figure 1A, p=0.03) and by age (Figure 1B, p=0.02). In addition, a trend positive relation between anti-schizont antibody levels and malaria incidence was observed (Figure 2A). However, there were no significant difference in median (SD) anti-schizont antibody levels during the study period when compared anti-schizont antibody levels by years [33.1AU (829.4) in 2012 and 32 AU (133.1) in 2021] (Figure 1C, p=0.78), and by gender (Figure 1D, p=0.2).
Eight-year trend analysis of malaria incidence
Overall, we demonstrated a significant decline in malaria incidence in both females and males from year 2015 (78.78 malaria incidence per 1000-person years) to 2020 (42.08 malaria incidence per 1000-person years) (Figure 2B). When categorizing data by age groups, we demonstrated a similar trend of decline in malaria incidence in patients under 5 years and those above 60 years old between 2015 and 2020. However, malaria incidence in patients aged 5-59 years did not change much between the follow-up period (Figure 2C). The current study also showed that, despite starting slightly high in 2013, there was a significant decline in malaria incidence in those under 5 years old from (598.30 malaria incidence per 1000-person years in 2015 to 75.56 malaria incidence per 1000-person years in 2020) in the low malaria transmission area. In high transmission areas, the incidence dropped from 891.30 (in 2015) to 249.89 malaria incidence per 1000-person years (in 2017), followed by a rebound of incidence up to 538.55 malaria incidence per 1000-person years in 2020 (Figure 2D). When comparing anti-schizont antibodies in under 5 patients, we showed a decrease in antibodies against P. falciparum anti-schizont was related to a decreased incidence in the respective group (Figure 2A).
We have demonstrated that the level of antibodies to P. falciparum schizont in under 5 years depending on the intensity of malaria transmission in Bagamoyo district, Tanzania. In general, we showed that waning in antibodies to P. falciparum schizont extract was reflected by a decrease in malaria incidence in under 5 years population, similar to the findings demonstrated in study conducted in Kenya [32]. This study also reported more incidence of malaria in males as compared to females despite, through the follow-up period (year 2013-2020) we observed a decrease in malaria incidence in both groups. The difference in incidence between males and females could be attributed to socioeconomic activities that led to more man exposed to mosquitos when spending time outside their home at night compare to females [33]. In addition, the acceptability of the use of malaria interventions such as treated bed nets has shown to be low in the male population compared to females [34].
Both antibodies and clinical malaria data have widely been used in studies to determine the malaria burden and monitor the impact of interventions over some time [35]. Using serological markers, a robust information on exposure over time and availability of long-lasting antibodies to Plasmodium spp can be obtained [35]. Serological data can further provide more insights into malaria epidemiology and help identify hotspots that need targeted interventions [36]. Moreover, the retrospective serological data and clinical data are important and can complement each other in explaining malaria status in malaria-endemic areas [37].
The current study neither observed a general difference in the median anti-schizont antibodies between the infants nor differences when categorized data by gender. This concurs with other studies that have shown no association between gender and malaria antibodies [38]. Previous study have also suggested that antibody distribution in infants may vary according to the level of malaria exposure [39], and/or vary due to level of antibodies they acquired from their mothers while in-utero [40], which is reported to last up to 6 months [41]. A change in anti-schizont antibody levels observed between the years of study samples might be allied to malaria control measures that have been implemented in recent years [42].
Interestingly, the clinical data demonstrated a significant reduction in malaria incidence among those under 5 years over the past 8 years. The outstanding reduction in malaria incidence observed in those under 5 years might also be related to control measures that the National Malaria Control Programs (NMCP) has implemented focusing on this age group [42]. Less malaria incidence seen in the >5-59 years age group, could be due to naturally acquired malaria immunity following several exposures to asymptomatic and symptomatic infections [43]. The >5-59 years age group includes adults that are more active and engage in social activities that put them at risk of contracting malaria parasites [44] resulting in a higher rate of acquisition of naturally acquired immunity [43]. High incidence observed in 60+years age group, could be resulted from the age-related immune compromise [45], thus making them susceptible to infectious diseases including malaria infection [46].
The observed fluctuation in malaria incidence over time in areas of high malaria transmission could be due to unstable implementation of malaria control measures in the region secondary to increased settlements [38]. Additionally, over the last 8 years, there has been a continuous improvement in the access to malaria diagnostic tests and reporting through HMIS providing a more realistic picture of malaria burden in rural Bagamoyo, an area regarded to have high malaria transmission [47]. Furthermore, possible factors that could determine the difference in malaria incidences between areas could be malaria species variation [48], resistance to interventions or efficiency and coverage of interventions [48] as well as social-economic activities [49], host and vector characteristics [49]. A slight trend increase in malaria incidence in 2020 could be a blip or a true increase as a result of the Covid-19 pandemic that might have negatively impacted malaria control programs such as clinical care provision and bed net distribution [6]. However, further studies are required to provide evidence of the impact of Covid-19 on malaria incidence.
The limitations of this study include the availability of a small sample size in a high transmission area for antibody analysis, the use of retrospective hospital data for incidence estimation, and inadequate longitudinal antibody data to conduct a statistical correlation between antibodies levels and malaria incidence. This was due to reliance on cross-sectional samples derived from studies that had different study objectives and the use of secondary clinical malaria data from health care facilities. Further, errors in measurement and reporting from secondary data obtained from health facilities might have reduced data quality [50]. Moreover, meteorological information such as rainfall, temperature, and relative humidity was not included in the analysis. However, serological and clinical results reported by this study are in agreement with findings from other studies, an indication that the above factors did not play a great role in the modification of the current findings [37].
The present study supports the evidence that the total anti-schizont antibody (IgG) levels depend on malaria transmission intensity in infants of 5-17 months and are positively related to malaria incidence. The use of archived clinical data from DHIS2 and serological data from vaccines or epidemiological studies can potential provide insight into the status of current malaria exposure in areas where proper incidence studies are unavailable.
What is known about this topic
- Association of antibodies to malaria blood-stage antigens and malaria exposure;
- Use of anti-malaria antibodies to blood-stage antigens in monitoring changes in malaria transmission over time.
What this study adds
- Further demonstration that total IgG antibody levels to P. falciparum schizont in infants of 5-17 months are related to malaria transmission intensity;
- Assessment of total IgG antibody levels to P. falciparum schizont in infants using both achieved and freshly collected serum samples to understand the change in malaria immunity over time;
- Demonstrate the potential of using antibodies data established from archive samples and hospital data from DHIS to give an insight into malaria exposure that would help better planning of clinical trial studies of malaria vaccine-induced responses in malaria-endemic communities.
The authors declare no competing interests.
Conception and study design: Tunu Guntram Mwamlima, John-Mary Vianney, Sarah Elizabeth Silk, Simon John Draper and Ally Ibrahim Olotu. Data collection: Tunu Guntram Mwamlima, Sarah Elizabeth Silk and Sarah Senyoni Mswata. Data analysis and interpretation: Tunu Guntram Mwamlima, Stephen Gabriel Mbwambo, Michael Fred Mboya and Ally Ibrahim Olotu. Manuscript drafting: Tunu Guntram Mwamlima. Manuscript revision: Ally Ibrahim Olotu, John-Mary Vianney, Maxmillian Gedion Mpina, Solomon Mickson Mwakasungula, Catherine Gerald Mkindi, Mgeni Mohamed Tambwe, Stephen Gabriel Mbwambo, Simon John Draper and Sarah Elizabeth Silk. All read and approved the final version of the manuscript.
This study was part of the EDCTP2 funding programme supported by the European Union (grant number RIA2016V-1649-MMVC). Thanks to Ifakara Health Institute who provided archived samples from which the antibody data were analysed.
Table 1: the demographic characteristics of the sampled population used for analyzing antibodies to P. falciparum schizont in infants
Table 2: the demographic characteristics, malaria cases and malaria incidence of the study population over the 8 years of follow-up
Figure 1: total immunoglobulins G against P. falciparum schizont among infants of Bagamoyo in 2012 versus 2021. (A) by study year, (B) by gender, (C) by age group and (D) by transmission areas; total IgG against P. falciparum schizont (Pf3D7) as measured by standardized enzyme-linked immunosorbent assay
Figure 2: trend of malaria incidence in Bagamoyo for the year 2013-2020, (A) males versus females, (B) by age groups, and (C) by transmission areas, the vertical (y) axis representing malaria incidence and the horizontal (x) axis representing years of follow-up, panel (D) showing the trend of malaria anti-schizont antibodies relative to malaria incidence in under 5 years; M=male, F=female, High trans=high transmission area and Low trans=low transmission area
- Press W, Geneva S. World malaria report 2014. 2014. Accessed 7 January 2022.
- Okumu FO, Moore SJ. Combining indoor residual spraying and insecticide-treated nets for malaria control in Africa: a review of possible outcomes and an outline of suggestions for the future. Malaria Journal. 2011;10(1):208. PubMed | Google Scholar
- Eastman RT, Fidock DA. Artemisinin-based combination therapies: a vital tool in efforts to eliminate malaria. Nat Rev Microbiol. 2009;7(12):864-874. PubMed | Google Scholar
- Gosling RD, Cairns ME, Chico RM, Chandramohan D. Intermittent preventive treatment against malaria: an update. Expert Review of Anti-infective Therapy. 2010;8(5):589-606. PubMed | Google Scholar
- WHO. Malaria. 2018.
- WHO. World malaria report 2021. 2021. Accessed 30 December 2021.
- Roux AT, Maharaj L, Oyegoke O, Akoniyon OP, Adeleke MA, Maharaj R et al. Chloroquine and Sulfadoxine-Pyrimethamine Resistance in Sub-Saharan Africa-A Review. Front Genet. 2021;0. doi:10.3389/fgene.2021.668574. PubMed | Google Scholar
- Toé KH, Jones CM, N´Fale S, Ismail HM, Dabiré RK, Ranson H. Increased Pyrethroid Resistance in Malaria Vectors and Decreased Bed Net Effectiveness, Burkina Faso. Emerg Infect Dis. 2014;20(10):1691-1696. Google Scholar
- Rémy V, Z�llner Y, Heckmann U. Vaccination: the cornerstone of an efficient healthcare system. Journal of Market Access & Health Policy. 2015;3. doi:10.3402/jmahp.v3.27041. Google Scholar
- Bobo FT, Asante A, Woldie M, Dawson A, Hayen A. Child vaccination in sub-Saharan Africa: Increasing coverage addresses inequalities. Vaccine. 2022;40(1):141-150. PubMed | Google Scholar
- Sánchez L, Vidal M, Jairoce C, Aguilar R, Ubillos I, Cuamba I et al. Antibody responses to the RTS,S/AS01E vaccine and Plasmodium falciparum antigens after a booster dose within the phase 3 trial in Mozambique. npj Vaccines. 2020;5(1):1-16. Google Scholar
- Valmaseda A, Macete E, Nhabomba A, Guinovart C, Aide P, Bardají A et al. Identifying Immune Correlates of Protection Against Plasmodium falciparum Through a Novel Approach to Account for Heterogeneity in Malaria Exposure. Clinical Infectious Diseases. 2018;66(4):586-593. PubMed | Google Scholar
- Schwartz L, Brown GV, Genton B, Moorthy VS. A review of malaria vaccine clinical projects based on the WHO rainbow table. Malaria journal. 2012;Vol. 11, 11. doi:info:doi/10.1186/1475-2875-11-11. PubMed | Google Scholar
- Kilama M, Smith DL, Hutchinson R, Kigozi R, Yeka A, Lavoy G et al. Estimating the annual entomological inoculation rate for Plasmodium falciparum transmitted by Anopheles gambiae s.l. using three sampling methods in three sites in Uganda. Malaria journal. 2014;13:111. PubMed | Google Scholar
- Olotu A, Fegan G, Wambua J, Nyangweso G, Ogada E, Drakeley C et al. Estimating Individual Exposure to Malaria Using Local Prevalence of Malaria Infection in the Field. PLOS ONE. 2012;7(3):e32929. PubMed | Google Scholar
- Baidjoe AY, Stevenson J, Knight P, Stone W, Stresman G, Osoti V et al. Factors associated with high heterogeneity of malaria at fine spatial scale in the Western Kenyan highlands. Malaria Journal. 2016;15(1):307. PubMed | Google Scholar
- White MT, Verity R, Griffin JT, Asante KP, Owusu-Agyei S, Greenwood B et al. Immunogenicity of the RTS,S/AS01 malaria vaccine and implications for duration of vaccine efficacy: secondary analysis of data from a phase 3 randomised controlled trial. The Lancet Infectious Diseases. 2015;15(12):1450-1458. Google Scholar
- Drakeley CJ, Corran PH, Coleman PG, Tongren JE, McDonald SLR, Carneiro I et al. Estimating medium- and long-term trends in malaria transmission by using serological markers of malaria exposure. PNAS. 2005;102(14):5108-5113. Google Scholar
- Olotu A, Fegan G, Wambua J, Nyangweso G, Awuondo KO, Leach A et al. Four-Year Efficacy of RTS,S/AS01E and Its Interaction with Malaria Exposure. New England Journal of Medicine. 2013;368(12):1111-1120. PubMed | Google Scholar
- Simmons RA, Mboera L, Miranda ML, Morris A, Stresman G, Turner EL et al. A longitudinal cohort study of malaria exposure and changing serostatus in a malaria endemic area of rural Tanzania. Malaria Journal. 2017;16(1):309. PubMed | Google Scholar
- Ashton RA, Bennett A, Al-Mafazy A-W, Abass AK, Msellem MI, McElroy P et al. Use of Routine Health Information System Data to Evaluate Impact of Malaria Control Interventions in Zanzibar, Tanzania from 2000 to 2015. EClinicalMedicine. 2019;12:11-19. PubMed | Google Scholar
- NBS. 2012 Population and housing census population distribution by administrative areas. 2013. Ministry of Finance Dar es Salaam.
- Odufuwa OG, Ross A, Mlacha YP, Juma O, Mmbaga S, Msellemu D et al. Household factors associated with access to insecticide-treated nets and house modification in Bagamoyo and Ulanga districts, Tanzania. Malar J. 2020;19:220. PubMed | Google Scholar
- Begum T, Khan SM, Adamou B, Ferdous J, Parvez MM, Islam MS et al. Perceptions and experiences with district health information system software to collect and utilize health data in Bangladesh: a qualitative exploratory study. BMC Health Services Research. 2020;20(1):465. PubMed | Google Scholar
- Salim N, Knopp S, Lweno O, Abdul U, Mohamed A, Schindler T et al. Distribution and Risk Factors for Plasmodium and Helminth Co-infections: A Cross-Sectional Survey among Children in Bagamoyo District, Coastal Region of Tanzania. PLOS Neglected Tropical Diseases. 2015;9(4):e0003660. PubMed | Google Scholar
- University of Oxford. Safety and Immunogenicity of ChAd63 RH5 and MVA RH5 in Adults, Young Children and Infants Living in Tanzania . 2019. Accessed 28 September 2021.
- Miura K, Orcutt AC, Muratova OV, Miller LH, Saul A, Long CA. Development and characterization of a standardized ELISA including a reference serum on each plate to detect antibodies induced by experimental malaria vaccines. Vaccine. 2008;26(2):193-200. PubMed | Google Scholar
- Kapulu MC, Kimani D, Njuguna P, Hamaluba M, Otieno E, Kimathi R et al. Controlled human malaria infection (CHMI) outcomes in Kenyan adults is associated with prior history of malaria exposure and anti-schizont antibody response. BMC Infect Dis. 2022;22:86. PubMed | Google Scholar
- Batwala V, Magnussen P, Nuwaha F. Are rapid diagnostic tests more accurate in diagnosis of Plasmodium falciparum malaria compared to microscopy at rural health centres? Malaria Journal. 2010;9(1):349. Google Scholar
- Battle KE, Guerra CA, Golding N, Duda KA, Cameron E, Howes RE et al. Global database of matched Plasmodium falciparum and P. vivax incidence and prevalence records from 1985-2013. Sci Data. 2015;2:150012. PubMed | Google Scholar
- Castro MC, Maheu-Giroux M, Chiyaka C, Singer BH. Malaria Incidence Rates from Time Series of 2-Wave Panel Surveys. PLoS Comput Biol. 2016;12(8):e1005065. PubMed | Google Scholar
- Ondigo BN, Hamre KES, Frosch AEP, Ayodo G, White MT, John CC. Antibody Profiles to P. falciparum Antigens Over Time Characterize Acute and Long-Term Malaria Exposure in an Area of Low and Unstable Transmission. Am J Trop Med Hyg. 2020;103(6):2189-2197. PubMed | Google Scholar
- Rodríguez-Rodríguez D, Katusele M, Auwun A, Marem M, Robinson LJ, Laman M et al. Human Behavior, Livelihood, and Malaria Transmission in Two Sites of Papua New Guinea. The Journal of Infectious Diseases. 2021;223(Supplement_2):S171-S186. Google Scholar
- Garley AE, Ivanovich E, Eckert E, Negroustoueva S, Ye Y. Gender differences in the use of insecticide-treated nets after a universal free distribution campaign in Kano State, Nigeria: post-campaign survey results. Malaria Journal. 2013;12(1):119. PubMed | Google Scholar
- Wong J, Hamel MJ, Drakeley CJ, Kariuki S, Shi YP, Lal AA et al. Serological markers for monitoring historical changes in malaria transmission intensity in a highly endemic region of Western Kenya, 1994-2009. Malaria Journal. 2014;13(1):451. PubMed | Google Scholar
- Surendra H, Supargiyono, Ahmad RA, Kusumasari RA, Rahayujati TB, Damayanti SY et al. Using health facility-based serological surveillance to predict receptive areas at risk of malaria outbreaks in elimination areas. BMC Medicine. 2020;18(1):9. PubMed | Google Scholar
- Keffale M, Shumie G, Behaksra SW, Chali W, Hoogen LL van den, Hailemeskel E et al. Serological evidence for a decline in malaria transmission following major scale-up of control efforts in a setting selected for Plasmodium vivax and Plasmodium falciparum malaria elimination in Babile district, Oromia, Ethiopia. Transactions of The Royal Society of Tropical Medicine and Hygiene. 2019;113(6):305-311. PubMed | Google Scholar
- Kabaria CW, Gilbert M, Noor AM, Snow RW, Linard C. The impact of urbanization and population density on childhood Plasmodium falciparum parasite prevalence rates in Africa. Malaria Journal. 2017;16(1):49. PubMed | Google Scholar
- Leoratti FM, Durlacher RR, Lacerda MV, Alecrim MG, Ferreira AW, Sanchez MC et al. Pattern of humoral immune response to Plasmodium falciparum blood stages in individuals presenting different clinical expressions of malaria. Malaria Journal. 2008;7(1):186. PubMed | Google Scholar
- Kurtis JD, Raj DK, Michelow IC, Park S, Nixon CE, McDonald EA et al. Maternally-derived Antibodies to Schizont Egress Antigen-1 and Protection of Infants From Severe Malaria. Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America. 2019;68(10):1718. PubMed | Google Scholar
- Stewart L, Gosling R, Griffin J, Gesase S, Campo J, Hashim R et al. Rapid Assessment of Malaria Transmission Using Age-Specific Sero-Conversion Rates. PLOS ONE. 2009;4(6):e6083. Google Scholar
- Everett S, deChambeau A. UL Strategic Plan 2018-2020 . 2018.
- Doolan DL, Dobaño C, Baird JK. Acquired Immunity to Malaria. Clinical Microbiology Reviews. 2009;22(1):13-36. Google Scholar
- Bizimana J-P, Twarabamenye E, Kienberger S. Assessing the social vulnerability to malaria in Rwanda. Malaria Journal. 2015;14(1):2. PubMed | Google Scholar
- Sadighi Akha AA. Aging and the immune system: An overview. Journal of Immunological Methods. 2018;463:21-26. PubMed | Google Scholar
- Oni T, Unwin N. Why the communicable/non-communicable disease dichotomy is problematic for public health control strategies: implications of multimorbidity for health systems in an era of health transition. International Health. 2015;7(6):390. PubMed | Google Scholar
- Renggli S, Mayumana I, Mboya D, Charles C, Mshana C, Kessy F et al. Towards improved health service quality in Tanzania: contribution of a supportive supervision approach to increased quality of primary healthcare. BMC Health Services Research. 2019;19(1):848. PubMed | Google Scholar
- Mboera LEG, Makundi EA, Kitua AY. Uncertainty in Malaria Control in Tanzania: Crossroads and Challenges for Future Interventions. 2007. American Society of Tropical Medicine and Hygiene. Accessed 23 October 2021.
- Tatem AJ, Gething PW, Smith DL, Hay SI. Urbanization and the global malaria recession. Malaria Journal. 2013;12(1):133. PubMed | Google Scholar
- Endriyas M, Alano A, Mekonnen E, Ayele S, Kelaye T, Shiferaw M et al. Understanding performance data: health management information system data accuracy in Southern Nations Nationalities and People´s Region, Ethiopia. BMC Health Services Research. 2019;19(1):175. Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
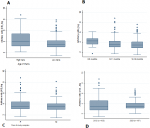 Figure 1: total immunoglobulins G against P. falciparum schizont among infants of Bagamoyo in 2012 versus 2021. (1A) by study year, (1B) by gender, (1C) by age group and (1D) by transmission areas. Total IgG against P. falciparum schizont (Pf3D7) as measured by standardized enzyme-linked immunosorbent assay
Figure 1: total immunoglobulins G against P. falciparum schizont among infants of Bagamoyo in 2012 versus 2021. (1A) by study year, (1B) by gender, (1C) by age group and (1D) by transmission areas. Total IgG against P. falciparum schizont (Pf3D7) as measured by standardized enzyme-linked immunosorbent assay
 Figure 2: trend of malaria incidence in Bagamoyo for the year 2013-2020, (A) males versus females, (B) by age groups, and (C) by transmission areas, the vertical (y) axis representing malaria incidence and the horizontal (x) axis representing years of follow-up, panel (D) showing the trend of malaria anti-schizont antibodies relative to malaria incidence in under 5 years; M=male, F=female, High trans=high transmission area and Low trans=low transmission area
Figure 2: trend of malaria incidence in Bagamoyo for the year 2013-2020, (A) males versus females, (B) by age groups, and (C) by transmission areas, the vertical (y) axis representing malaria incidence and the horizontal (x) axis representing years of follow-up, panel (D) showing the trend of malaria anti-schizont antibodies relative to malaria incidence in under 5 years; M=male, F=female, High trans=high transmission area and Low trans=low transmission area











