Factors associated with childhood chronic malnutrition in West and Central Africa: a scoping review
Pengdewende Maurice Sawadogo, Drissa Sia, Eric Tchouaket Nguemeleu, Jean-François Kobiane, Yentema Onadja, Stephanie Robins
Corresponding author: Pengdewende Maurice Sawadogo, Institut Supérieur des Sciences de la Population (ISSP), Université Joseph Ki-Zerbo, Ouagadougou, Burkina Faso 
Received: 15 Dec 2021 - Accepted: 11 Sep 2022 - Published: 28 Sep 2022
Domain: Child nutrition,Malnutrition,Maternal and child health
Keywords: Chronic malnutrition, child, factors associated, West Africa, Central Africa
©Pengdewende Maurice Sawadogo et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Pengdewende Maurice Sawadogo et al. Factors associated with childhood chronic malnutrition in West and Central Africa: a scoping review. Pan African Medical Journal. 2022;43:45. [doi: 10.11604/pamj.2022.43.45.32820]
Available online at: https://www.panafrican-med-journal.com//content/article/43/45/full
Review 
Factors associated with childhood chronic malnutrition in West and Central Africa: a scoping review
Factors associated with childhood chronic malnutrition in West and Central Africa: a scoping review
![]() Pengdewende Maurice Sawadogo1,&,
Pengdewende Maurice Sawadogo1,&, ![]() Drissa Sia2,3, Eric Tchouaket Nguemeleu2,4, Jean-François Kobiane1, Yentema Onadja1,
Drissa Sia2,3, Eric Tchouaket Nguemeleu2,4, Jean-François Kobiane1, Yentema Onadja1, ![]() Stephanie Robins1
Stephanie Robins1
&Corresponding author
Chronic malnutrition is a major public health concern that is the focus of a large body of scientific research. However, there is no synthesis of knowledge about the factors associated with this disease in West and Central Africa, where its prevalence is particularly high. We conducted a systematic search for scientific articles published between January 1st, 2000, and October 15th, 2020, that focus on chronic malnutrition in children in West and Central Africa. We queried CAIRN, PubMed, CINAHL, MEDLINE, Scopus, and Google Scholar databases for this purpose. The search process followed the recommendations of Arksey and O'Malley. Items reported in this review follow the PRISMA-ScR guidelines. Sixty articles involving children from a total of twenty (20) countries, mainly Ghana and Nigeria, were included in the final analysis. The data used were predominantly cross-sectional and were mainly drawn from demographic and health surveys. The analysis revealed that chronic malnutrition in children is associated with sociocultural, economic, and healthcare factors related to the characteristics of children, mothers, households, and communities. The association with children's vulnerability to disease, maternal education, purchasing power, and autonomy need to be further investigated in West and Central Africa. Further analysis using longitudinal data is also needed to better understand the factors associated with chronic malnutrition in West and Central Africa.
Chronic malnutrition in children is a growth disorder resulting from a long-term deficiency in nutrient intake. The condition brings numerous adverse consequences to health and economic status which are long-lasting and sometimes irreversible [1]. Studies have shown that women who suffered from chronic malnutrition in childhood are more predisposed to complications during childbirth [2,3]. There is also evidence that children who suffered from chronic malnutrition have an increased risk of obesity, high blood pressure, and renal failure in adulthood [3-5]. In addition, chronic malnutrition is associated with reduced physical and intellectual capacity resulting from a long-term deficiency of iodine and iron, an effect that is often irreversible after the child reaches the age of two [6,7]. This reduced cognitive capacity of children -who should become future workers- demonstrates how chronic malnutrition handicaps the development of countries. As such, it is considered "a symptom of past deprivation and a prediction of future poverty" [8].
In sub-Saharan Africa, chronic malnutrition is widespread, affecting one-third of children under the age of five [9]. Evidence-based scientific research will be required to support decision-making to tackle this high level of chronic malnutrition and successfully achieve the goal of eliminating it by 2030, following the Sustainable Development Goals [10].
Given the importance of the subject, several empirical studies have analyzed factors contributing to childhood chronic malnutrition. There are two review articles concerning the whole of sub-Saharan Africa [11,12], which covers all of West and Central Africa. However, one of them does not cover the last four years (2018, 2019, 2020 and 2021) [11]. Also, the most recent review only took into account nationally representative studies [12]. It, therefore, excluded the many studies conducted at the sub-national level. Other research has examined the effect of maternal education on chronic malnutrition in children [13].
To date, there is no article synthesizing knowledge on the factors associated with chronic malnutrition in West and Central Africa, which is the most affected sub-region [9]. The specific health and socio-cultural characteristics of this sub-region support the need for such knowledge synthesis. This article addresses the need for a synthesis of knowledge on the factors associated with chronic malnutrition in West and Central Africa. It is designed as a scoping review, which is an alternative to a classic systematic review when the literature on a subject is extensive [14], which is the case for chronic malnutrition in this setting.
Study design: this scoping review was conducted according to the framework defined by Arksey and O'Malley [14] which is well established and frequently used [15]. The review was written following the recommendations of Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) [16].
Protocol registration: there has been no protocol and registration of this scoping review.
Research question: the scoping review was conducted around the following question: "according to the scientific literature, what are the factors associated with chronic malnutrition in children in West and Central Africa?”.
Search strategy and data source: the search question was analyzed to identify keywords representing population, intervention, comparators, outcomes, timing, and study design (PICOTS), which were then used to build search strategies. These search strategies were then applied to the CAIRN, PubMed, CINAHL, MEDLINE, Scopus, and Google Scholar databases. The keyword searches used included free text and controlled vocabulary. Orthographic variants and synonyms of the keywords were also taken into consideration in the construction of the search equations. These equations enabled a systematic selection of all scientific articles that contained these words in their title, abstract, or keywords. The search equation used was: ("chronic malnutrition" or "growth disorder" or "stunted growth" or stunting or "nutritional status" or undernutrition or malnutrition) and (child* or infant* or under-five or preschool).
Eligibility criteria: eligibility criteria, both inclusion and exclusion, were defined to guide the selection of articles.
Inclusion criteria: all articles included in this scoping review met the following criteria: i) the study concerned one or more countries in West Africa (Benin, Burkina Faso, Central African Republic, Chad, Ivory Coast, Democratic Republic of Congo, Gambia, Ghana, Guinea, Guinea-Bissau, Liberia, Mali, Mauritania, Niger, Nigeria, Senegal, and Sierra Leone) or Central Africa (Angola, Cameroon, Gabon, Equatorial Guinea, Republic of Congo, Sao Tome and Principe); ii) the study was published between January 1, 2000, and October 15, 2021; iii) the study addressed chronic malnutrition assessed by a height/age ratio; iv) the measurement of height respected the World Health Organization (WHO) standard of measuring height in the supine position for children under two and in the standing position for those aged two and over according to WHO and UNICEF [17]; v) the reference standard used for estimating the nutritional status of children was either the National Center for Health Statistics (NCHS) standard [18] or the new WHO standard [19]; vi) the study assessed the factors associated with chronic malnutrition in children under five years of age; vii) finally, the article was published in French or English.
Exclusion criteria: although meeting the inclusion criteria described above, some articles were excluded for the following reasons: i) the articles were restricted to specific populations such as premature infants, children who were hospitalized or attending a given health service, or children suffering from a particular disease or condition (HIV, congenital pathology, etc.); ii) the articles were methodological guides or handbooks; iii) the data used were collected before January 1, 2000.
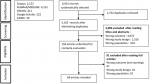
Selection process: the selection of articles was carried out in several steps (Figure 1). It began with the automatic selection of articles by applying search strategies in all databases. References were then exported to Endnote where perfect duplicates were eliminated. Once the duplicates were removed, the remaining references were then exported to the RAYYAN website and screened according to the eligibility criteria. The first screening evaluated the articles by reading titles and abstracts. Following this, the full text of the selected articles was read for final inclusion. Two authors (Pengdewende Maurice Sawadogo and Drissa Sia) separately selected the references by reading the titles and abstracts. The references for which there was a discordance were secondarily examined by a third author (ET). The same process was observed for the complete reading of the articles.
Data extraction from included studies: the data were extracted using a grid designed by the authors. The extraction of data from the first eight (8) articles was done by the whole team of authors during a working meeting. The remaining articles were distributed among the authors for extraction.
Collating, summarizing and reporting the findings: the data extracted from the included articles were designed following the grid. The relevant information obtained includes references of the article, country, age of children, types of study and methods of analysis, and significant risk factors. Subsequently, these data were organized by country and by geographical area.
Applying our search strategy identified a total of 6,915 articles: 2,122 in SCOPUS, 4,131 in PubMed/MEDLINE, 411 in CINAHL, 222 in Google Scholar, and 29 in CAIRN. There were 1,752 duplicates that were removed. Of the 5,163 remaining articles, 4,978 (96.4%) were excluded after reading their titles and abstracts. Also, 40 articles were initially classified as "undecided", they were then re-evaluated, and 26 were excluded and 14 were retained. The 159 articles retained at this stage were read in their entirety and analyzed according to see if they met eligibility criteria. In the end, 68 articles were included. The entire selection process is presented in Figure 1.
Characteristics of the selected studies: four studies [20-23] were published in French and 64 [24-87] in English. The classification of the included articles by country shows that nearly half were conducted in two English-speaking countries, namely Ghana (n=19) and Nigeria (n=13). In French-speaking countries, most studies were conducted in Burkina Faso (n=12), Senegal (n=6), and Democratic Republic of Congo (DRC) (n=4). No study concerning Togo, Cape Verde, Sierra Leone, and Sao Tome and Principe was included.
Methods for identifying factors associated with chronic child malnutrition: the characteristics of the selected studies, including the methods for analyzing the factors associated with chronic child malnutrition, are presented in Table 1, Table 1 (suite), Table 2, Table 2 (suite) and Table 3. The main sources of data were demographic and health surveys (DHS) or multiple indicator cluster surveys (MICS), which were used in 31 studies. Overall there were 63 cross-sectional [20-45,47-55,57-60,62-70,72-84,86,87] and 5 longitudinal study designs [46,56,61,71,85]. Child growth references of the NCHS standard were used in eight studies [22,23,41,54,56,58,68,81]. The new WHO standard was used in the other 60 studies [20,21,24-40,42-53,55,57,59-67,69-80,82-87].
Factors associated with chronic malnutrition in children: the analysis of the 68 selected articles showed that child, maternal, household, and community characteristics are statistically associated with chronic malnutrition in children in West and Central Africa (Table 1, Table 1 (suite), Table 2, Table 2 (suite), Table 3).
Child characteristics associated with chronic malnutrition: child characteristics are those that are the most frequently associated with chronic malnutrition. These include age, sex, twinship, birth weight and height, health status, vaccination status, and dietary intake. The effects of age and sex were the most common across studies. The association with age was reported in 41 studies and indicated an increased risk of chronic malnutrition with increasing age. The effect of sex was found in 30 studies and most of them showed a higher risk in boys than in girls. The effects of twinship (n=7), birth rank (n=3), birth weight (n=6), birth height (n=3), birth interval (n=2), disease frequency (n=13), vaccination status (n=7), breastfeeding (n=3), meal diversification (n=9), meal frequency (n=2), and vitamin A and iron supplementation (n=1) were also found. However, some studies that investigated these factors found that the sex or age of the child was not associated with chronic malnutrition in children. This was the case of two studies conducted in Nigeria [38] and Burkina Faso, Mali, Chad, Senegal, and Mauritania [22] which found no effect on the age of the child. Three studies, conducted in Nigeria, Burkina Faso, and Ghana, concluded that the sex of the child was not statistically associated with his or her nutritional status [21,38,60].
Maternal characteristics associated with childhood chronic malnutrition: significant effects of maternal characteristics, including education, age, mobility, leadership, experience with domestic violence, decision-making autonomy, ethnicity, marital status, and health status were reported in the reviewed studies. The effect of maternal education was reported in 19 studies and showed a reduction in the risk of chronic malnutrition with an increased maternal level of education. These effects of education are particularly apparent when mothers have an education level from secondary school and up [48,49,77,84].
The effects of a mother's purchasing power, as assessed by employment status or income level, were demonstrated in six studies in Angola, Burkina Faso, Cameroon, Ghana (n=2), and Nigeria [21,30,32,57,67,80]. These studies showed that the risk of chronic malnutrition is relatively lower for children of high-income mothers. An association between maternal age and chronic malnutrition in children has also been established in nine studies. They demonstrate that the risk of chronic malnutrition was higher in children of adolescents [36] or relatively younger mothers [24,26,36,54,60,66,74,77].
The effects of maternal autonomy, including leadership, participation in decision making, experience, or attitude toward violence were highlighted in five studies. They found that children of mothers with decision-making autonomy are less likely to suffer from chronic malnutrition [30,33,41,72,79,84]. Five other studies showed an association between maternal nutritional status and child chronic malnutrition. Usually, the risk was higher for children of mothers with a nutritional deficiency (BMI <18.5) [46,81,83,85,87]. Some studies also reported a higher risk of chronic malnutrition for children of mothers of low height [27,46,78]. The effect of maternal ethnicity was reported in two studies [60,84]. In addition, four studies conducted in Burkina Faso, Ghana and Nigeria have established that children whose delivery occurred in a health center or whose mothers had prenatal consultation(s) were less likely to suffer from chronic malnutrition [21,26,38,80]. Finally, in Burkina Faso, children of mothers with a partner were less likely to suffer from chronic malnutrition than children of non-partnered mothers [47].
Some studies found that maternal and child characteristics are not statistically associated with chronic malnutrition in children. For example, four studies conducted in Ghana, Senegal, and Nigeria concluded that there was no effect of maternal education on chronic child malnutrition [39,45,70,72]. It is the same for purchasing power, in that the absence of its effect has been reported in Nigeria [39].
Household characteristics associated with childhood chronic malnutrition: the analysis of the articles revealed that certain household characteristics are associated with child chronic malnutrition. These characteristics include socioeconomic status, family composition, and access to water and sanitation.
The effect of socioeconomic status was found in ten studies and was assessed by the level of economic well-being [21,26,32,47,59,64,66,80,86] or livestock ownership [63]. These studies show a low propensity for chronic malnutrition in children from households with high socioeconomic status. In rare cases, as in Pikine, Senegal, the effect of household socioeconomic status was not significant [70]. Five studies reported that the household family composition was significantly associated with chronic malnutrition in children. Children from single-parent or monogamous households or those living in a household with relatively few young children were at lower risk of suffering from chronic malnutrition [24,26,47,60,66].
Eight studies conducted in Angola [62], Burkina Faso [46,59], Guinea [34], Niger [48,75], Lubumbashi (DRC) [23], Gambia [48], and Nigeria [32] showed that children living in households with improved drinking water were less likely to suffer from chronic malnutrition than those from households without access to a safe source of drinking water. Furthermore, three studies found that children living in households with access to safe toilets had a lower risk of chronic malnutrition than children without safe toilets [49,62,75]. Similarly, children whose faeces are properly managed are less likely to be stunted [34]. Finally, three studies have documented that urban children are less likely to suffer from chronic malnutrition than rural children [24,40,74]. However, non-significant effects with regards to the place of residence have been reported in Senegal and Burkina Faso [20,47].
Community characteristics associated with childhood chronic malnutrition: community characteristics that were statistically associated with child chronic malnutrition are described in three studies. In Senegal, authors have established that an increase in the percentage of women in the district having decision-making power is statistically associated with reduced childhood chronic malnutrition [20]. In Nigeria, children who came from communities with a low literacy rate were significantly more susceptible to suffer from chronic malnutrition [87]. Finally, researchers in Burkina Faso and Ghana have demonstrated that increasing the immunization coverage of children in a geographical area was associated with a reduction in the prevalence of chronic malnutrition [29,69].
Our discussion first focuses on the methodological aspects of the selected studies. Secondly, it assesses the factors related to childhood chronic malnutrition identified in the selected articles.
Methods used: nearly half of the data collected and analyzed in the studies were from the Demographic and Health/Multiple Indicator Cluster Surveys (DHS/MICS) that provide representative results at the national and regional levels. These surveys use a standardized data collection methodology that ensures the comparability of findings across the time horizon and geographic area.
However, there are weaknesses related to the type of data collected. Almost all (63/68) of the study designs are cross-sectional. Thus, the data collected is not well adapted to examining the effects of ephemeral events such as episodes of disease in children on the onset of chronic malnutrition. Indeed, cross-sectional data do not ensure that the occurrence of the event (e.g. episode of diarrhoea) has preceded the resulting outcome (chronic malnutrition). Therefore, it is difficult to prove that the associations made are not by chance. This is particularly problematic in a condition such as chronic malnutrition, where predisposing damaging factors are slowly and permanently established [54]. Given that some of the factors (diarrhoea, fever) are ephemeral, longitudinal data should have been collected and analyzed to assess their effects on chronic malnutrition in children.
Children's eating practices change dramatically in the first five years of life: from zero to six months, they are almost exclusively breastfed; from 6-23 months, they consume breast milk and light foods; and from 24 months, they share the family meal. Consequently, the factors associated with optimal feeding, a close determinant of chronic malnutrition, may differ according to their age. There is evidence to suggest that there are age-specific factors of malnutrition, as demonstrated by authors [34]. Nevertheless, more than two-thirds of the selected studies did not consider this heterogeneity by analyzing the factors of chronic malnutrition in children aged 0-59 months or 6-59 months as homogeneous groups. Future studies should conduct separate analyses using more discrete age groupings in infants and children (e.g. 0-5 months, 6-23 months, and 24-59 months) in order to highlight the specific determinants in each age group.
Finally, it is important to note that 90% of the studies didn´t use a multilevel model although the theoretical hierarchical structure of malnutrition factors [88,89] argues for this model. The search for contextual factors by using a multilevel model would provide a better understanding of children chronic malnutrition in West and Central Africa.
Associated factors identified: the review of the articles demonstrated that children's characteristics and maternal characteristics are those most frequently associated with chronic malnutrition. This predominance of child and mother-related factors underlines the importance of these proximate determinants in predicting child chronic malnutrition. Our discussion will address the vulnerability of children to disease, maternal education, the purchasing power of parents, and the decision-making autonomy of mothers, which are the main determinants of chronic malnutrition in children highlighted in West and Central Africa.
Children's vulnerability to disease: childhood illness is a major contributing factor to chronic malnutrition. Eleven studies describe a statistical association between the occurrence of diarrhoea, fever or anemia and the onset of chronic malnutrition [20,26,34,40,48,53,56,57,62,77,81,86]. By affecting nutritional intake, the illness caused stunted growth. For example, when a child has diarrhoea, a frequent symptom in sick children, a good part of the food intake is eliminated through the stools. The body then draws on its reserves to ensure its functioning, which leads to rapid weight loss. In the days following the remission of the diarrhoea, the nutritional intake is primarily allocated by the body to restore the weight deficit. During this time, the child's growth stagnates, which eventually leads to stunted growth [90]. Most other childhood illnesses are associated with digestive disorders such as anorexia, nausea, and vomiting, creating a deficit in food intake, again resulting in stagnation of growth [62]. For example, researchers have established that a child shows an average growth retardation of 0.002 mm per day during an episode of malaria, due in part to digestive disorders [91]. Although childhood illnesses may affect growth due to dietary intake disturbances, this requires frequent or prolonged bouts of illness [54]. In contrast, some research has shown that recent illness (two weeks) may affect children's growth. Thus, future studies should use longitudinal data to better estimate the effects of episodes of illness on chronic malnutrition in children.
The association between chronic malnutrition and children´s characteristics such as age, sex, twinship, birth size, and vaccination status is related (in part) that these factors (e.g. age, sex, twinship, birth size, and vaccination status) make children vulnerable to disease. Authors have demonstrated that the greater susceptibility of twins to malnutrition is due to a higher frequency of congenital malformations, low birth weight, and cerebral palsy, rendering them more susceptible to disease [24]. Similarly, the increased risk of chronic malnutrition in boys is partly related to a higher frequency of premature births (a major factor of ill health) among males compared to females, or to a higher frequency of disease in boys in infancy [20,62,92]. The frequency of twinship or preterm birth in small birth size children explained their increased risk of malnutrition [93].
The effects of age on chronic malnutrition also express a vulnerability to childhood diseases. Indeed, the risk of chronic malnutrition is increased between 6 and 23 months of age when the child's immune system fails due to the decrease in maternal antibodies [87] and due to an as-yet immature immune system. This immune deficiency makes the child particularly vulnerable to disease, which has an impact on his growth. Similarly, routine immunization of children as part of the Expanded Programme on Immunization (EPI) protects them against major childhood diseases. As a result, vaccinated children are relatively less sick and less likely to suffer from chronic malnutrition [32,48,51,58,69,73,86].
In sum, a greater vulnerability to disease in boys, twins, children born with short stature, and unvaccinated children predisposes them to a greater risk of chronic malnutrition. Given that some of these vulnerability factors such as sex, age, twinship, and birth size are non-modifiable factors, research should be directed toward mitigating the effect of those factors that are most commonly associated with chronic malnutrition in children.
Maternal education: maternal education is commonly associated with chronic malnutrition in children. Its effect has been highlighted in 19 studies, showing a reduction in the risk of chronic malnutrition when the mothers' education level increases. At school, lessons about nursing, biology, food hygiene, enable mothers and caregivers to acquire useful knowledge to care for and feed babies. In addition, educated people have access to more diversified sources of information (newspapers, posters, etc.), which can increase their knowledge. Thus, capitalizing on their schooling and better access to information, educated mothers have higher knowledge of nutrition [45]. Consequently, their children are less likely to suffer from chronic malnutrition than those of uneducated mothers.
The effect of education can also be mediated through a close-to-home diffusion within communities. Uneducated mothers can learn about good hygiene, care, and feeding practices from their educated counterparts, enabling them to overcome their skill deficits. This neighbourhood effect is often so strong that it leads to the elimination of differences in children's nutritional status caused by the individual educational level of their mothers. This could explain why, in communities where the majority of women are educated, maternal education is not a discriminating factor of children's chronic malnutrition [39,72]. Since the examination of this neighbourhood effect of mothers´ education was considered in only one study [86], future research should investigate its relative contribution to chronic malnutrition.
Purchasing power of parents: purchasing power refers to the ability of parents to financially acquire the goods and services necessary for the appropriate growth of children. Some characteristics, such as the mother's employment and income, and the household's economic well-being reflect this effect of parental purchasing power. Women with higher incomes have greater access to food and health services, which is conducive to growth in their children [21,57,67,80]. Similarly, wealthy households have relatively higher incomes that can be used to ensure the successful growth of their children. There is evidence that the purchasing power of mothers has the greatest effect on children's chronic malnutrition, more than that of the father or the whole household [59,64,66,86]. This is explained by the fact that females allocate a larger part of their income to food expenditures [94].
Despite this, some studies have found no effect of purchasing power estimated by the household income level on childhood chronic malnutrition [39,59,64,66,70,86]. This counter-intuitive result may be linked to limitations in the definition of the indicator of purchasing power. In most studies, household income is assessed based on a synthetic index made up of housing characteristics and amenities of the household [95]. This indicator of wealth/poverty may not adequately reflect the true economic status of the household members. Residents of households classified as rich according to this indicator may be poor and vice versa. Moreover, this indicator of relative poverty only assesses differences between extreme classes of socioeconomic levels [96]. Due to these limitations, the use of this indicator to analyze the effects of parental purchasing power on child chronic malnutrition is imperfect.
To be complete, the assessment of parental purchasing power on children's nutritional status must take into account the community income level, as access to goods and services is dependent on it. In fact, food and healthcare are relatively more expensive in upper-income communities found in large urban centers [97,98]. Thus, at equal income levels, people living in an upper-income community may have more limited access to healthcare and food, compared to their peers living in a lower-income community. It is, therefore, appropriate to consider the context of relative wealth in determining the effects of parental income on chronic child malnutrition.
Maternal autonomy: this concept refers to "a woman's ability to influence decisions about family, finances, and spending, work, social outings, health care, travel, family planning, and child care..." [99]. The effects of maternal leadership, participation in decision making, and experience and attitude toward violence highlighted in the selected studies reflect the impact of autonomy [33,41,72,79,84]. For example, a woman who has some leadership can work to increase the share of household resources devoted to food, since they devote a larger share of their income for this purpose [94]. Similarly, a mother who has greater freedom of movement can more easily travel to the health clinic to receive care and advice, which is beneficial for the proper growth of her children. Similarly, women who do not fear violence from their husbands are more likely to follow the nutritional advice they receive than those who do fear them.
In summary, the autonomy of mothers to make decisions concerning the care and feeding of their children is an important determining factor, especially in the contexts of child care and feeding which are almost exclusively their responsibility. Studies on chronic malnutrition should take into account the mothers´ autonomy whose effects have not yet been sufficiently analyzed in West and Central Africa.
This systematic search and review of the scientific literature have identified child, maternal, household, and community characteristics that are associated with chronic malnutrition in children living in West and Central Africa. Despite the relative abundance of scientific evidence on the subject, the effects of some major factors such as children's vulnerability to disease, maternal education, and maternal autonomy are still poorly defined. Future studies should focus on a deeper investigation of the effects of these factors. In addition, the use of subgroups in analyzing age, and longitudinal data, would provide complete view of childhood chronic malnutrition factors in West and Central Africa.
What is known about this topic
- West and Central Africa, which is the most affected sub-region;
- Factors contributing to childhood chronic malnutrition are studied in several empirical studies.
What this study adds
- It is the first knowledge synthesis of factors associated with childhood stunting in West and Central Africa;
- It shows that there would be a contextual effect of mother's education and purchasing power that must be taken into account in future studies;
- Child´s vulnerability to disease is a factor of childhood chronic malnutrition.
The authors declare no competing interests.
All the authors read and approved the final version of this manuscript.
Table 1: characteristics of selected studies in Ghana and Nigeria
Table 1 (suite): characteristics of selected studies in Ghana and Nigeria
Table 2: characteristics of selected studies in West Africa, excluding Ghana and Nigeria
Table 2 (suite): characteristics of selected studies in West Africa, excluding Ghana and Nigeria
Table 3: characteristics of selected studies in a country in Central Africa or including several countries
Figure 1: flow chart showing the process for selecting the articles
- Stewart CP, Iannotti L, Dewey KG, Michaelsen KF, Onyango AW. Contextualising complementary feeding in a broader framework for stunting prevention: complementary feeding in stunting prevention. Matern Child Nutr. 2013 Sep;9 Suppl 2(Suppl 2):27-45. PubMed | Google Scholar
- Özaltin E, Hill K, Subramanian S. Association of maternal stature with offspring mortality, underweight, and stunting in low-to middle-income countries. JAMA. 2010;303(15):1507-16. PubMed | Google Scholar
- Adair LS, Fall CH, Osmond C, Stein AD, Martorell R, Ramirez-Zea M et al. Associations of linear growth and relative weight gain during early life with adult health and human capital in countries of low and middle income: findings from five birth cohort studies. Lancet. 2013;382(9891):525-34. PubMed | Google Scholar
- Whincup PH, Kaye SJ, Owen CG, Huxley R, Cook DG, Anazawa S et al. Birth weight and risk of type 2 diabetes: a systematic review. JAMA. 2008;300(24):2886-97. PubMed | Google Scholar
- Uauy R, Kain J, Mericq V, Rojas J, Corvalán C. Nutrition, child growth, and chronic disease prevention. Ann Med. 2008;40(1):11-20. PubMed | Google Scholar
- Zimmermann MB. The effects of iodine deficiency in pregnancy and infancy. Paediatr Perinat Epidemiol. 2012 Jul;26 Suppl 1:108-17. PubMed | Google Scholar
- Lukowski AF, Koss M, Burden MJ, Jonides J, Nelson CA, Kaciroti N et al. Iron deficiency in infancy and neurocognitive functioning at 19 years: evidence of long-term deficits in executive function and recognition memory. Nutr Neurosci. 2010;13(2):54-70. PubMed | Google Scholar
- Development Initiatives. The P20 initiative: the gap between the poorest 20% of people and everyone else is getting bigger. 2017. Accessed 15th December, 2021.
- United Nations Children´s Fund, World Health Organization, International Bank for Reconstruction and Development. Levels and trends in child malnutrition: UNICEF/WHO/The World Bank Group joint child malnutrition estimates: key findings of the 2020 edition. 2020. Accessed 15th December, 2021.
- Organisation des Nations Unies. Objectifs de developpement durable. 2015.
- Akombi BJ, Agho K, Hall J, Wali N, Renzaho A, Merom D. Stunting, wasting and underweight in sub-Saharan Africa: a systematic review. Int J Environ Res Public Health. 2017;14(8):863. PubMed | Google Scholar
- Obasohan PE, Walters SJ, Jacques R, Khatab K. Risk factors associated with malnutrition among children under-five years in sub-Saharan African countries: a scoping review. Int J Environ Res Public Health. 2020 Nov 26;17(23):8782. PubMed | Google Scholar
- Mensch BS, Chuang EK, Melnikas AJ, Psaki SR. Evidence for causal links between education and maternal and child health: systematic review. Trop Med Int Health. 2019;24(5):504-22. PubMed | Google Scholar
- Arksey H, O'Malley L. Scoping studies: towards a methodological framework. International Journal of Social Research Methodology. 2005;8(1):19-32. Google Scholar
- Colquhoun HL, Levac D, O'Brien KK, Straus S, Tricco AC, Perrier L et al. Scoping reviews: time for clarity in definition, methods, and reporting. J Clin Epidemiol. 2014;67(12):1291-4. PubMed | Google Scholar
- Tricco AC, Lillie E, Zarin W, O'Brien KK, Colquhoun H, Levac D et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467-73. PubMed | Google Scholar
- World Health Organization. Recommendations for data collection, analysis and reporting on anthropometric indicators in children under 5 years old. 2019. Google Scholar
- de Onis M, Onyango AW, Borghi E, Garza C, Yang H; WHO Multicentre Growth Reference Study Group. Comparison of the World Health Organization (WHO) Child Growth Standards and the National Center for Health Statistics/WHO international growth reference: implications for child health programmes. Public Health Nutr. 2006;9(7):942-7. PubMed | Google Scholar
- de Onis M, Garza C, Onyango AW, Rolland-Cachera MF; le Comité de nutrition de la Société française de pédiatrie. Les standards de croissance de l´Organisation mondiale de la santé pour les nourrissons et les jeunes enfants. Arch Pediatr. 2009 Jan;16(1):47-53. PubMed | Google Scholar
- Berenger V, Vérez J-C. Les déterminants individuels et contextuels de la sous-nutrition des enfants d'âge préscolaire au Sénégal. Journal de Gestion et d'économie de la Santé. 2019;3(3):237-58.
- Bougma S, Garanet F, Sawadogo N, Savadogo A. Facteurs associés au retard de croissance dans un contexte de supplémentation alimentaire au Burkina Faso. Cahiers de Nutrition et de Diététique. 2019;54(2):108-15. Google Scholar
- Garenne M. Tendances de l´état nutritionnel des jeunes enfants dans les pays francophones du Sahel: 1990-2015. 2019. Google Scholar
- Mukatay AW, Kalenga PM, Dramaix M, Hennart P, Schirvel C, Kabamba LM et al. Facteurs prédictifs de la malnutrition chez les enfants âgés de moins de cinq ans à Lubumbashi (RDC). Sante Publique. 2010 Sep-Oct;22(5):541-50. PubMed | Google Scholar
- Yaya S, Oladimeji O, Odusina EK, Bishwajit G. Household structure, maternal characteristics and children's stunting in sub-Saharan Africa: evidence from 35 countries. Int Health. 2020;14(4):381-9. PubMed | Google Scholar
- de Wit M, Cairns M, Compaoré YD, Sagara I, Kuepfer I, Zongo I et al. Nutritional status in young children prior to the malaria transmission season in Burkina Faso and Mali, and its impact on the incidence of clinical malaria. Malar J. 2021 Jun 22;20(1):274. PubMed | Google Scholar
- Aheto JMK. Simultaneous quantile regression and determinants of under-five severe chronic malnutrition in Ghana. BMC Public Health. 2020;20(1):644. PubMed | Google Scholar
- Anin SK, Saaka M, Fischer F, Kraemer A. Association between Infant and Young Child Feeding (IYCF) indicators and the nutritional status of children (6-23 months) in Northern Ghana. Nutrients. 2020;12(9):2565. PubMed | Google Scholar
- Appiah CA, Mensah FO, Hayford FEA, Awuuh VA, Kpewou DE. Predictors of undernutrition and anemia among children aged 6-24 months in a low-resourced setting of Ghana: a baseline survey. Journal of Health Research. 2021;35(1):27-37. Google Scholar
- de Groot R, Handa S, Ragno LP, Spadafora T. Child malnutrition, consumption growth, maternal care and price shocks: new evidence from Northern Ghana. Development Studies Research. 2020;7(1):18-30. Google Scholar
- Essilfie G, Sebu J, Annim SK. Women's empowerment and child health outcomes in Ghana. African Development Review. 2020;32(2):200-15. Google Scholar
- Mank I, Vandormael A, Traoré I, Ouédraogo WA, Sauerborn R, Danquah I. Dietary habits associated with growth development of children aged <5 years in the Nouna health and demographic surveillance system, Burkina Faso. Nutr J. 2020;19(1):81. PubMed | Google Scholar
- Obayelu OA, Adeleye OR. Explaining child nutritional status in rural Nigeria: socioeconomic dimensions. Journal of Hunger and Environmental Nutrition. 2020;829-846. Google Scholar
- Yaya S, Odusina EK, Uthman OA, Bishwajit G. What does women's empowerment have to do with malnutrition in sub-Saharan Africa: evidence from demographic and health surveys from 30 countries. Glob Health Res Policy. 2020;5:1. PubMed | Google Scholar
- Woodruff BA, Wirth JP, Ngnie-Teta I, Beaulière JM, Mamady D, Ayoya MA et al. Determinants of stunting, wasting, and anemia in Guinean preschool-age children: an analysis of DHS data from 1999, 2005, and 2012. Food Nutr Bull. 2018;39(1):39-53. PubMed | Google Scholar
- Wemakor A, Mensah KA. Association between maternal depression and child stunting in Northern Ghana: a cross-sectional study. BMC Public Health. 2016;16(1):869. PubMed | Google Scholar
- Wemakor A, Garti H, Azongo T, Garti H, Atosona A. Young maternal age is a risk factor for child undernutrition in Tamale Metropolis, Ghana. BMC Res Notes. 2018;11(1):877. PubMed | Google Scholar
- Vonaesch P, Tondeur L, Breurec S, Bata P, Nguyen LBL, Frank T et al. Factors associated with stunting in healthy children aged 5 years and less living in Bangui (RCA). PloS One. 2017;12(8):e0182363. PubMed | Google Scholar
- Uthman OA. A multilevel analysis of individual and community effect on chronic childhood malnutrition in rural Nigeria. J Trop Pediatr. 2009;55(2):109-15. PubMed | Google Scholar
- Udoh EE, Amodu OK. Complementary feeding practices among mothers and nutritional status of infants in Akpabuyo Area, Cross River State Nigeria. Springerplus. 2016;5(1):2073. PubMed | Google Scholar
- Thorne CJ, Roberts LM, Edwards DR, Haque MS, Cumbassa A, Last AR. Anaemia and malnutrition in children aged 0-59 months on the Bijagós Archipelago, Guinea-Bissau, West Africa: a cross-sectional, population-based study. Paediatr Int Child Health. 2013;33(3):151-60. PubMed | Google Scholar
- Sobkoviak RM, Yount KM, Halim N. Domestic violence and child nutrition in Liberia. Soc Sci Med. 2012;74(2):103-11. PubMed | Google Scholar
- Sié A, Tapsoba C, Dah C, Ouermi L, Zabre P, Bärnighausen T et al. Dietary diversity and nutritional status among children in rural Burkina Faso. Int Health. 2018;10(3):157-62. PubMed | Google Scholar
- Sawadogo PS, Martin-Prével Y, Savy M, Kameli Y, Traissac P, Traoré AS et al. An infant and child feeding index is associated with the nutritional status of 6- to 23-month-old children in rural Burkina Faso. J Nutr. 2006;136(3):656-63. PubMed | Google Scholar
- Saaka M, Wemakor A, Abizari AR, Aryee P. How well do WHO complementary feeding indicators relate to nutritional status of children aged 6-23 months in rural Northern Ghana. BMC Public Health. 2015;15:1157. PubMed | Google Scholar
- Saaka M. Relationship between mothers' nutritional knowledge in childcare practices and the growth of children living in impoverished rural communities. J Health Popul Nutr. 2014;32(2):237-48. PubMed | Google Scholar
- Prado EL, Yakes Jimenez E, Vosti S, Stewart R, Stewart CP, Somé J et al. Path analyses of risk factors for linear growth faltering in four prospective cohorts of young children in Ghana, Malawi and Burkina Faso. BMJ Glob Health. 2019 Jan 13;4(1):e001155. PubMed | Google Scholar
- Poda GG, Chien-Yeh H, Chao JC-J. Factors associated with malnutrition among children <5 years old in Burkina Faso: evidence from the demographic and health surveys IV 2010. Int J Qual Health Care. 2017;29(7):901-8. PubMed | Google Scholar
- Oyekale AS, Oyekale TO. Do mothers' educational levels matter in child malnutrition and health outcomes in Gambia and Niger. Social Sciences. 2009;4(1):118-27.
- Nwosu EO, Orji A. A Comparative analysis of socioeconomic indicators and child nutritional status in Nigeria´s geopolitical zones. Child Indicators Research. 2018;11(5):1677-98. Google Scholar
- Ntab B, Simondon KB, Milet J, Cissé B, Sokhna C, Boulanger D et al. A young child feeding index is not associated with either height-for-age or height velocity in rural Senegalese children. J Nutr. 2005;135(3):457-64. PubMed | Google Scholar
- Nikoi E, Anthamatten P. An examination of environmental correlates with childhood height-for-age in Ghana. Public Health Nutr. 2013;16(1):46-53. PubMed | Google Scholar
- Gupta N, Gehri M, Stettler N. Early introduction of water and complementary feeding and nutritional status of children in northern Senegal. Public Health Nutr. 2007 Nov;10(11):1299-304. PubMed | Google Scholar
- Makamto Sobgui C, Kamedjie Fezeu L, Diawara F, Diarra H, Afari-Sefa V, Tenkouano A. Predictors of poor nutritional status among children aged 6-24 months in agricultural regions of Mali: a cross-sectional study. BMC Nutr. 2018;4:18. PubMed | Google Scholar
- Kobelembi F. La malnutrition chronique chez les enfants de moins de cinq ans. L'enfant en Centrafrique. 2004:157.
- Kismul H, Acharya P, Mapatano MA, Hatløy A. Determinants of childhood stunting in the Democratic Republic of Congo: further analysis of demographic and health survey 2013-14. BMC Public Health. 2017;18(1):74. PubMed | Google Scholar
- Kang H, Kreuels B, Adjei O, Krumkamp R, May J, Small DS. The causal effect of malaria on stunting: a Mendelian randomization and matching approach. Int J Epidemiol. 2013;42(5):1390-8. PubMed | Google Scholar
- Humbwavali JB, Giugliani C, Nunes LN, Dalcastagnê SV, Duncan BB. Malnutrition and its associated factors: a cross-sectional study with children under 2 years in a suburban area in Angola. BMC Public Health. 2019;19(1):220. PubMed | Google Scholar
- Hong R. Effect of economic inequality on chronic childhood undernutrition in Ghana. Public Health Nutr. 2007;10(4):371-8. PubMed | Google Scholar
- Gelli A, Headey D, Becquey E, Ganaba R, Huybregts L, Pedehombga A et al. Poultry husbandry, water, sanitation, and hygiene practices, and child anthropometry in rural Burkina Faso. Matern Child Nutr. 2019 Oct;15(4):e12818. PubMed | Google Scholar
- Frempong RB, Annim SK. Dietary diversity and child malnutrition in Ghana. Heliyon. 2017;3(5):e00298. PubMed | Google Scholar
- Fregonese F, Siekmans K, Kouanda S, Druetz T, Ly A, Diabaté S et al. Impact of contaminated household environment on stunting in children aged 12-59 months in Burkina Faso. J Epidemiol Community Health. 2017;71(4):356-63. PubMed | Google Scholar
- Fernandes ECB, de Castro TG, Sartorelli DS. Associated factors of malnutrition among African children under five years old, Bom Jesus, Angola. Revista de Nutricao. 2017;30(1):33-44. Google Scholar
- Fadare O, Mavrotas G, Akerele D, Oyeyemi M. Micronutrient-rich food consumption, intra-household food allocation and child stunting in rural Nigeria. Public Health Nutr. 2019;22(3):444-54. PubMed | Google Scholar
- Fadare O, Amare M, Mavrotas G, Akerele D, Ogunniyi A. Mother's nutrition-related knowledge and child nutrition outcomes: empirical evidence from Nigeria. PloS One. 2019;14(2):e0212775. PubMed | Google Scholar
- Ewusie J, Beyene J, Ahiadeke C, Hamid J. Malnutrition in pre-school children across different geographic areas and socio-demographic groups in Ghana. Matern Child Health J. 2017;21(4):797-808. PubMed | Google Scholar
- Darteh EKM, Acquah E, Kumi-Kyereme A. Correlates of stunting among children in Ghana. BMC Public Health. 2014;14:504. PubMed | Google Scholar
- Dapi Nzefa L, Monebenimp F, Äng C. Undernutrition among children under five in the Bandja village of Cameroon, Africa. South African Journal of Clinical Nutrition. 2019;32(2):46-50. Google Scholar
- Custodio E, Descalzo MA, Roche J, Sánchez I, Molina L, Lwanga M et al. Nutritional status and its correlates in Equatorial Guinean preschool children: results from a nationally representative survey. Food Nutr Bull. 2008;29(1):49-58. PubMed | Google Scholar
- Chuang Y-C, Chuang T-W, Chao HJ, Tseng K-C, Nkoka O, Sunaringsih S et al. Contextual factors and spatial patterns of childhood malnutrition in provinces of Burkina Faso. J Trop Pediatr. 2020;66(1):66-74. PubMed | Google Scholar
- Buttarelli E, Chapuis-Lucciani N, Badiane NS, Gueye L. Nutritional status among young children (0-3 years) in the Pikine-Dagoudane urban area in Senegal. Bulletins et Memoires de la Societe d'Anthropologie de Paris. 2013;25(1):83-98.
- Bork K, Cames C, Barigou S, Cournil A, Diallo A. A summary index of feeding practices is positively associated with height-for-age, but only marginally with linear growth, in rural senegalese infants and toddlers. J Nutr. 2012;142(6):1116-22. PubMed | Google Scholar
- Boah M, Azupogo F, Amporfro DA, Abada LA. The epidemiology of undernutrition and its determinants in children under five years in Ghana. PloS One. 2019;14(7):e0219665. PubMed | Google Scholar
- Balogun TB, Yakubu AM. Recent illness, feeding practices and father's education as determinants of nutritional status among preschool children in a rural Nigerian community. J Trop Pediatr. 2015;61(2):92-9. PubMed | Google Scholar
- Annim SK, Ausabo-Asare K, Amo-Adjei J. Household nucelation, dependency and child health outcomes in Ghana. J Biosoc Sci. 2015;47(5):565-92. PubMed | Google Scholar
- Anand A, Roy N. Transitioning toward sustainable development goals: the role of household environment in influencing child health in sub-Saharan Africa and South Asia using recent demographic health surveys. Front Public Health. 2016;4:87. PubMed | Google Scholar
- Amugsi DA, Dimbuene ZT, Kimani-Murage EW, Mberu B, Ezeh AC. Differential effects of dietary diversity and maternal characteristics on linear growth of children aged 6-59 months in sub-Saharan Africa: a multi-country analysis. Public Health Nutr. 2017;20(6):1029-45. PubMed | Google Scholar
- Amare M, Benson T, Fadare O, Oyeyemi M. Study of the determinants of chronic malnutrition in Northern Nigeria: quantitative evidence from the Nigeria demographic and health surveys International Food Policy Research Institute (IFPRI) working paper 45 (September 2017). Food Nutr Bull. 2018;39(2):296-314. PubMed | Google Scholar
- Ali Z, Saaka M, Adams A-G, Kamwininaang SK, Abizari A-R. The effect of maternal and child factors on stunting, wasting and underweight among preschool children in Northern Ghana. BMC Nutr. 2017;3:31. PubMed | Google Scholar
- Alaofè H, Zhu M, Burney J, Naylor R, Douglas T. Association between women's empowerment and maternal and child nutrition in Kalalé District of Northern Benin. Food Nutr Bull. 2017;38(3):302-18. PubMed | Google Scholar
- Akombi BJ, Agho KE, Hall JJ, Merom D, Astell-Burt T, Renzaho AMN. Stunting and severe stunting among children under-5 years in Nigeria: a multilevel analysis. BMC Pediatr. 2017 Jan 13;17(1):15. PubMed | Google Scholar
- Aké-Tano O, Tiembré I, Konan YE, Donnen P, N'Cho Dagnan S, Dramaix M et al. Chronic malnutrition among children under five years of age in the northern part of Côte d'Ivoire. Sante Publique. 2010;22(2):213-20. PubMed | Google Scholar
- Ajao KO, Ojofeitimi EO, Adebayo AA, Fatusi AO, Afolabi OT. Influence of family size, household food security status, and child care practices on the nutritional status of under-five children in lle-lfe, Nigeria. Afr J Reprod Health. 2010 Dec;14(4 Spec no.):117-26. PubMed | Google Scholar
- Aheto JMK, Keegan TJ, Taylor BM, Diggle PJ. Childhood malnutrition and its determinants among under-five children in Ghana. Paediatr Perinat Epidemiol. 2015;29(6):552-61. PubMed | Google Scholar
- Agu N, Emechebe N, Yusuf K, Falope O, Kirby RS. Predictors of early childhood undernutrition in Nigeria: the role of maternal autonomy. Public Health Nutr. 2019;22(12):2279-89. PubMed | Google Scholar
- Agbota G, Fievet N, Heude B, Accrombessi M, Ahouayito U, Yovo E et al. Poor maternal anthropometric status before conception is associated with a deleterious infant growth during the first year of life: a longitudinal preconceptional cohort. Pediatr Obes. 2020 Jan;15(1):e12573. PubMed | Google Scholar
- Adeyemi RA, Zewotir T, Ramroop S. Joint spatial mapping of childhood anemia and malnutrition in sub-Saharan Africa: a cross-sectional study of small-scale geographical disparities. Afr Health Sci. 2019;19(3):2692-712. PubMed | Google Scholar
- Adekanmbi VT, Kayode GA, Uthman OA. Individual and contextual factors associated with childhood stunting in Nigeria: a multilevel analysis. Matern Child Nutr. 2013;9(2):244-59. PubMed | Google Scholar
- Hien NN, Hoa NN. Nutritional status and determinants of malnutrition in children under three years of age in Nghean, Vietnam. Pakistan Journal of Nutrition. 2009;8:958-64. Google Scholar
- United Nations Children's Fund. Strategy for improved nutrition of children and women in the developing countries. 1992:13-24.
- Richard SA, Black RE, Gilman RH, Guerrant RL, Kang G, Lanata CF et al. Diarrhea in early childhood: short-term association with weight and long-term association with length. Am J Epidemiol. 2013;178(7):1129-38. PubMed | Google Scholar
- Oldenburg CE, Guerin PJ, Berthé F, Grais RF, Isanaka S. Malaria and nutritional status among children with severe acute malnutrition in Niger: a prospective cohort study. in Infect Dis. 2018;67(7):1027-34. PubMed | Google Scholar
- Wamani H, Åstrøm AN, Peterson S, Tumwine JK, Tylleskär T. Boys are more stunted than girls in sub-Saharan Africa: a meta-analysis of 16 demographic and health surveys. BMC Pediatr. 2007 Apr 10;7:17. PubMed | Google Scholar
- Mieth RA. Les jumeaux sous le signe du conflit: le point de vue du néonatologue. Revue de Médecine Périnatale. 2015;7(1):16-20. Google Scholar
- Lachaud JP. Gains féminins, allocation des biens et statut nutritionnel des enfants au Burkina Faso. Revue d'économie du développement. 1998;6(2):3-53. Google Scholar
- Croft TN, Aileen MJM, Courtney KA. Guide to DHS statistics DHS-7: the demographic and health surveys program. Rockville, Maryland, USA: ICF. 2018.
- Kobiané JF. Habitat et biens d´équipement comme indicateurs de niveau de vie des ménages: bilan méthodologique et application à l´analyse de la relation pauvretéscolarisation. 2004. Google Scholar
- Ministère de la Santé. Cartographie de l'offre de services de santé dans la région du centre. In: Direction générale de l'information et des statistiques sectorielles /ministère de la santé, editor. Ouagadougou/Burkina Faso. 2010.
- Ball K, Timperio A, Crawford D. Neighbourhood socioeconomic inequalities in food access and affordability. Health Place. 2009;15(2):578-85. PubMed | Google Scholar
- Carlson GJ, Kordas K, Murray-Kolb LE. Associations between women's autonomy and child nutritional status: a review of the literature. Matern Child Nutr. 2015;11(4):452-82. PubMed | Google Scholar