There is an urgent need for a global rural health research agenda
Luchuo Engelbert Bain, Oluwafemi Atanda Adeagbo
Corresponding author: Luchuo Engelbert Bain, International Development Research Centre (IDRC), Ottawa, Canada 
Received: 11 Nov 2022 - Accepted: 17 Nov 2022 - Published: 18 Nov 2022
Domain: Global health,Health Research
Keywords: Rural, health, global, research, agenda
©Luchuo Engelbert Bain et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Luchuo Engelbert Bain et al. There is an urgent need for a global rural health research agenda. Pan African Medical Journal. 2022;43:147. [doi: 10.11604/pamj.2022.43.147.38189]
Available online at: https://www.panafrican-med-journal.com//content/article/43/147/full
There is an urgent need for a global rural health research agenda
&Corresponding author
People living in rural areas generally experience adverse health outcomes compared to their urban counterparts. They experience a greater burden of non-communicable diseases including: diabetes, hypertension, stroke, kidney disease, and chronic obstructive pulmonary disease (COPD), have limited access to healthcare services, and experience scarcity in specialized healthcare services. The disproportionately high all-cause mortality experienced by rural residents has been termed �the rural mortality penalty�. With over 90% of the world�s rural population living in Africa and Asia, we argue that the lack of an authoritative and respected global rural health research agenda contributes to increasing health inequalities, given that many of these people are receiving substandard care. There are differences in how rural and urban resident�s experience healthcare. Living in rural settings might not be systematically connected to adverse health outcomes. It is important to clearly articulate the positive health outcomes associated with living in rural settings (e.g., the positive relationship between mental health and strong social ties/green spaces). Indeed, health policies stand the chance of unconsciously excluding the positive outcomes associated with rurality, as well as the rural experiences of health. Defining rural health remains an issue of controversy with a persistent reality regarding the lack of consensus as to what it means for a region or area to be considered as �rural�. We outline the most common definitions of �rural areas� in the literature, as well as the shortcomings of these definitions. By unpacking the meaning of �rural health�, we aim to foster communication among rural health professionals and researchers locally and internationally, as well as highlight the key research and policy implications that could emanate from a �good� definition of rural health. We agree that context remains key when it comes conceptualizing complex subjects like rurality. However, developing minimum criteria to foster communication among rural health researchers is needed. Systematically providing operational definitions of what authors describe as �rural� in the rural health research and policy literature is of utmost relevance.
Introduction
Place and context affect the overall health status of populations [1-3]. People living in rural settings are increasingly reported to experience a health disadvantage and disparities. They are disproportionately prone to negative health outcomes compared to their urban counterparts [1-5]. Rural populations are more likely to have a poorer quality of life, have a relatively greater number of people without health insurance, limited access to quality healthcare services, have fewer healthcare infrastructures, lower socioeconomic status, and lower life expectancy compared to their urban counterparts [1-6]. These discrepancies in mortality between urban and rural residents have been referred to as the “rural mortality penalty” [4]. Of the over 9.7 million deaths recorded in 2017 in India, three quarters occurred in rural areas [5]. Irrespective of their physical environment or socioeconomic status, rural populations often experience higher burdens of diverse conditions such as obesity, diabetes, cancer, severe acute malnutrition, and injury compared to urban populations [3,4,6]. They are also more likely to engage in risky behaviours such as substance abuse [3,4,6].
Further, the recent coronavirus (COVID-19) pandemic has highlighted the vulnerability of rural communities during an outbreak. In the US per capita, disease burden and health system demand are the highest outside of urban areas [7]. Despite clear inequities existing between rural and urban populations, there has been a lack of political will to address these persistent challenges. Empirical research remains sparse in systematically addressing these inequalities. The Sustainable Development Goals (SDGs), which are an urgent call for action by all countries, recognise that ending poverty and other deprivations must go hand-in-hand with strategies to improve health and education, reduce inequality, and spur economic growth [8]. It is estimated that 76% of the developing world's poor live in rural areas [9]. The ability to recruit and retain a sustainable, skilled workforce to address these inequities and facilitate access to community-relevant care in rural and remote regions is dependent upon evidence-based operational research and situational analysis [10].
To achieve SDG 10 of bridging existing inequalities among countries, the intricate connections between health, poverty, and wellbeing and the application of health policies that do not fit the contextual needs of rural communities, must be considered if health policies targeting rural populations do not match their needs. Adequate policies should be informed by evidence. We argue that the global rural health research agenda has not been articulated enough. Indeed, a definition of rural health that meets a minimum consensus is required to allow communication among rural health researchers. Defining rural health remains an issue of controversy [11]. In this paper, we report key issues around rural experience of health, and articulate the need for a rural health research agenda, with issues around an 'inclusive' definition for rural health at its core.
Rural experiences of health
The rural setting is very important to rural residents. The rural context must not always be seen in the negative sense [12,13]. The social relations between individuals, family ties, and valued community identities have been reported to be very important considerations for rural residents [14,15]. Disrupting these ties or policies that unintentionally disrupt the will of the rural residents can be detrimental to their wellbeing. Access to green spaces, far more common in rural settings, are increasingly being reported to be associated with better mental health outcomes [16]. What it means to be healthy differs from one rural population to the other [11,17,18]. The extremely rural heterogeneity makes one-size fit-all approaches challenging to implement [19,20]. Engaging communities in the co-creation of health intervention, design and implementation should be prioritized in order provide culturally affirming healthcare services that will improve their health outcomes and overall wellbeing [13,15,21]. These approaches are more likely to provide context-specific solutions to rural health concerns. Framing a rural health research and policy agenda requires a deep understanding of how rural residents perceive and experience health. Table 1 summarizes how rural residents perceive and experience health in the literature.
Why do we need global research agenda for rural health?
In 2018, 3.4 billion (44.7%) of the world´s 7.6 billion inhabitants lived in rural areas, and Africa and Asia are home to 90% of the world´s rural population [22]. There are glaring cultural differences (family, values, relationships, meanings in community) between urban and rural areas. Rural healthcare research and policy are still lagging in these regions of the world [23]. Social and cultural norms have been reported to influence health seeking behaviors [24,25]. Unaddressed rural health challenges might lead to health inequalities. For instance, failure to improve health outcomes in rural areas will indirectly push its residents into the spiral of poverty, ill-health and low economic productivity [26]. In China, dusty lung deaths for men living in rural areas doubled compared to their urban counterparts between 2002 and 2016 [27]. This has been attributed to policies that completely excluded rural communities [27]. Thus, empirical evidence is crucial to make a strong case for rural residents.
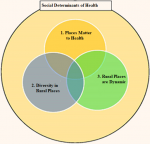
Robust evidence could serve as an important advocacy instrument to bring about change. If rural residents are not properly identified with denominators that capture them appropriately as well as their sociocultural identities, they will be either completely forgotten or at times receive services that do not match their needs and, culture. There are many commonalities as well as differences across rural settings worldwide. However, responding to this challenge needs to be context specific. Responses in land locked areas could differ from responses in areas accessible only by boat, ship, or air. Systematically identifying these differences and commonalities can be helpful in generating local evidence, which could serve as learning grounds for other rural settings. The “rural mortality penalty” is a reality worldwide and has been mostly documented in the US [4,28,29]. There is however a growing body of literature on the heterogeneity in the mortality distribution across rural settings [28,29]. Context and social determinants of health are important considerations when reading mortality rates in rural settings. In 2016, Kulig proposed a rural health framework composed of three core interrelated areas: 'places matter to health', 'diversity in rural places', and 'rural places are dynamic' [30]. She posits that these three areas are interconnected by the social determinants of health (Figure 1). This framework could be empirically tested in diverse rural settings to ascertain its suitability in guiding rural health research and policy.
Gaps in rural health conceptualization and common definitions of rural areas in selected countries
Current perspectives and focus on rural health are fraught with fundamental shortfalls including lack of common definition of rural area and subsequently rural health as well as the weak theoretical framework for implementation of rural health concept. Globally, there is no univocal definition of what area can be considered rural. Most of these definitions have traditionally provided a dichotomous meaning of where to consider rural or urban. In fact, the definitions often differ even within the same country. Population density, travel time to the nearest urban centre, and access to services are mostly used in the definition of rural areas (Table 2).
Given these definitions differ considerably across geographies, this renders cross-country comparisons problematic. For instance, an area with a population of less than 400 persons in New Zealand is considered rural; whilst an area with less than 10,000 persons in the UK is rural. Population density on its own becomes an empty concept if the context is not specified. Accessibility to services, for instance, healthcare services, also carries some shortcomings. In New Zealand for instance, 40% of people using rural healthcare facilities are classified as urban by Statistics New Zealand greatly contributing to the difficulties in demonstrating the differences between rural and urban healthcare services [17]. The rural-urban dichotomous definitions have been reported to propagate the heterogeneity among rural areas especially when it comes to access to healthcare services [31-34]. Failure to recognize this reality means health policy research recommendations might miss the intended beneficiaries. Inequalities in healthcare, a critical issue in health policy, might persist due to the inability to correctly identify who is a rural or urban resident, as well as correctly identifying the usage patterns of the healthcare services at their disposal. Poor definitions can drive health inequalities since those in need can either be missed/misclassified or received inappropriate healthcare interventions or funding. To mitigate this bias, it is plausible to rethink the definition of 'rural health' that captures the key healthcare challenges or priorities of areas considered as rural. Definitions mainly based on geographical considerations (population density for instance) are inadequate to capture the healthcare needs of rural populations [23].
Identifying a consensus definition for urban areas is also a daunting exercise. In a literature review and expert survey of the European Union member states for the European Urban Health Indicator System (EURO-URHIS) project, no unique definition for urban areas was found [25]. Sociocultural differences between urban and rural areas suggest that residents´ views regarding the meaning of being healthy or quality healthcare might be different. Rural residents have been reported to have distinct views on how they conceptualize and define health [11]. The researchers however highlight in their systematic review the scarcity of corresponding comparative definitions of health from urban residents. Capturing a definition for rural health that is relevant to a specific context stands to benefit from including rural residents´ views. Indeed, whenever possible, and depending on the research subject of interest, co-creating a definition of 'rural' stands to provide findings and policy recommendations that better capture the populations that stands to benefit, as well as reflect the reality of the setting in question. Empirical rural-urban comparative health research is sparse and increasingly being required to provide context relevant healthcare. This is relevant in not only properly ascertaining the real burden of disease in rural and urban areas, but also allows identification of unique healthcare challenges associated with being a rural or urban resident. These high-quality findings can be a strong advocacy tool in pushing policy makers to respond adequately to the needs of the disadvantaged rural residents [24,35].
The need for an inclusive definition for rural health
Theoretical imperative
Bourke and colleagues argue that developing a theoretical framework on how to approach rural health has relevance both at intellectual and policy levels [36]. They put forward five main reasons for this: i) theory provides logical guidance to study a subject; (ii) it helps in challenging assumptions in the knowledge generation process; (iii) permits a structured analysis which is a relevant predictor of knowledge transferability; (iv) theory provides predictability; and (v) theory allows for a holistic understanding of concepts studied. Complexities around the definitions of rural health across the world compel researchers to speak a common language. Theoretically, it is imperative to allow for peers to learn from experiences elsewhere and apply it locally [14]. This is helpful in not repeating the same conceptual and methodological mistakes committed elsewhere. An international rural health research agenda will highlight how rural healthcare provision is different and constitute a great avenue for policy makers to make context specific relevant and appropriate policies.
There is a need for best-practice guidelines to direct researchers on which urban/rural definition is appropriate for which situations. There are cultural differences between rural communities and urban centres in many countries including significant cultural differences as one moves from rural community to the other. Sociologists describe this quality as 'gemeinschaft' (social relations between individuals, based on close personal and family ties; community) [12,26]. Indeed, through a social lens, the construct of rurality should reflect local understandings, history, lifestyle, and institutions. Most rural populations in the world are from low- and middle-income countries (LMICs) while rural health research centres and researchers are rare in these countries. Most research in rural health has explored rural areas mainly in Western countries, with very limited data on rural health in LMICs.
We can hypothesize that these health policies, generally urban-centric might be neither relevant, nor appropriate, for rural settings. Inequalities in the provision of, and access to healthcare, are prone to persist, or be exacerbated in some instances in these rural settings. The rural populations can be be trapped in the vicious cycle of disease and poverty, which negates the core objective of global health (equity in healthcare access) as well as the World Health Organization's (WHO) “Health for All' campaign.
Worrisome evidence indicates that the gap in mortality rates between rural and urban settings is increasing as the years go by [37]. If ´rural health´ continues to be poorly defined, the over 3.4 billion persons in the world living in these areas (90% in Africa and Asia) might be receiving inadequate and inappropriate healthcare. Indeed, no clear definition of rural areas was found from developing countries. Heterogeneity is a constant reality worth considering in rural health research and policy making. We agree that context remains key when it comes conceptualizing complex subjects like rurality. However, developing minimum criteria to foster communication among rural health researchers is need. Systematically providing operational definitions of what authors describe as “rural” in the rural health research and policy literature is of utmost relevance. With the current trends where rural populations are left behind, attaining the sustainable development goal 10 on health and inequalities remains a mirage [8]. Not all is bad regarding health outcomes when it comes to living in rural areas. Articulating “rurality associated health advantages”, and how these could be enhanced will stand to benefit a huge portion of the world's population which is predominantly "rural".
The authors declare no competing interests.
Luchuo Engelbert Bain conceived and drafted the initial draft of the manuscript. Oluwafemi Atanda Adeagbo contributed in reviewing the literature, and providing significant intellectual input in restructuring the manuscript. Both authors have read and agreed to the final version of the manuscript.
Table 1: rural perception and experience of health
Table 2: examples of common definitions of 'rural areas' in selected countries
Figure 1: a general rural health research framework
- Scheil-Adlung X; ILO | Social Protection Platform. Global evidence on inequities in rural health protection. New data on rural deficits in health coverage for 174 countries. World; 2015. Accessed Aug 4, 2020.
- Richman L, Pearson J, Beasley C, Stanifer J. Addressing health inequalities in diverse, rural communities: An unmet need. SSM Popul Health. 2019 Apr 9;7:100398. PubMed | Google Scholar
- Mainous AG, Kohrs FP. A comparison of health status between rural and urban adults. J Community Health. 1995 Oct;20(5):423-31. PubMed | Google Scholar
- Cosby AG, Neaves TT, Cossman RE, Cossman JS, James WL, Feierabend N et al. Preliminary Evidence for an Emerging Nonmetropolitan Mortality Penalty in the United States. Am J Public Health. 2008 Aug;98(8):1470-2. PubMed | Google Scholar
- Menon GR, Singh L, Sharma P, Yadav P, Sharma S, Kalaskar S et al. National Burden Estimates of healthy life lost in India, 2017: an analysis using direct mortality data and indirect disability data. Lancet Glob Health. 2019 Dec;7(12):e1675-84. PubMed | Google Scholar
- Fagbamigbe AF, Kandala NB, Uthman AO. Demystifying the factors associated with rural-urban gaps in severe acute malnutrition among under-five children in low- and middle-income countries: a decomposition analysis. Sci Rep. 2020 Jul 7;10(1):11172. PubMed | Google Scholar
- Miller IF, Becker AD, Grenfell BT, Metcalf CJE. Disease and healthcare burden of COVID-19 in the United States. Nat Med. 2020 Aug;26(8):1212-1217. PubMed | Google Scholar
- United Nations | Department of Economic and Social Affairs: Sustainable Development. Sustainable Development Goals. Accessed August 11, 2020.
- Ravallion M, Chen S, Sangraula P. New Evidence on the Urbanization of Global Poverty. Development Research Group, World Bank; March 2007. Accessed 11, Aug 2020.
- Deblonde M. Responsible research and innovation: Building knowledge arenas for glocal sustainability research. Journal of Responsible Innovation. 2015 Jan 2;2(1):20-38. Google Scholar
- Gessert C, Waring S, Bailey-Davis L, Conway P, Roberts M, VanWormer J. Rural definition of health: a systematic literature review. BMC Public Health. 2015 Apr 14;15(1):378. PubMed | Google Scholar
- Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. Am J Public Health. 2005 Jul;95(7):1149-55. PubMed | Google Scholar
- Thurston WE, Meadows LM. Rurality and health: perspectives of mid-life women. Rural Remote Health. 2003 Oct-Dec;3(3):219. PubMed | Google Scholar
- Farmer J, Clark A, Munoz S-A. Is a global rural and remote health research agenda desirable or is context supreme? Australian Journal of Rural Health. 2010;18(3):96-101. PubMed | Google Scholar
- Rawolle TA, Sadauskas D, van Kessel G, Dollman J. Farmers´ perceptions of health in the Riverland region of South Australia: �If it´s broke, fix it´. Aust J Rural Health. 2016 Oct;24(5):312-6. PubMed | Google Scholar
- Houlden V, Weich S, Porto de Albuquerque J, Jarvis S, Rees K. The relationship between greenspace and the mental wellbeing of adults: A systematic review. PLoS One. 2018 Sep 12;13(9):e0203000. PubMed | Google Scholar
- Fearnley D, Lawrenson R, Nixon G. �Poorly defined´: unknown unknowns in New Zealand Rural Health. N Z Med J. 2016 Aug 5;129(1439):77-81. PubMed | Google Scholar
- Levesque J-F, Harris MF, Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. International Journal for Equity in Health. 2013 Mar 11;12(1):18. PubMed | Google Scholar
- Kenny A, Hyett N, Sawtell J, Dickson-Swift V, Farmer J, O´Meara P. Community participation in rural health: a scoping review. BMC Health Serv Res. 2013 Feb 18;13:64. PubMed | Google Scholar
- Harvey DJ. Understanding Australian rural women´s ways of achieving health and wellbeing - a metasynthesis of the literature. Rural Remote Health. 2007 Oct-Dec;7(4):823. PubMed | Google Scholar
- Bennett KJ, Borders TF, Holmes GM, Kozhimannil KB, Ziller E. What Is Rural? Challenges And Implications Of Definitions That Inadequately Encompass Rural People And Places. Health Aff (Millwood). 2019 Dec;38(12):1985-92. PubMed | Google Scholar
- United Nations | Department of Economic and Social Affairs. 68% of the world population projected to live in urban areas by 2050, says UN. New York: UN DESA; 16 May 2018. Accessed Mar 29, 2021.
- Smith ML, Dickerson JB, Wendel ML, Ahn S, Pulczinski JC, Drake KN et al. The utility of rural and underserved designations in geospatial assessments of distance traveled to healthcare services: implications for public health research and practice. Int J Environ Res. 2013 Jun 13;2013. Google Scholar
- Lourenço AEP. The meaning of �rural´ in rural health: a review and case study from Brazil. Glob Public Health. 2012;7(1):1-13. PubMed | Google Scholar
- Breckenkamp J, Patterson L, Scharlach M, Hellmeier W, Verma A. Definitions of urban areas feasible for examining urban health in the European Union. Eur J Public Health. 2017 May 1;27(suppl_2):19-24. PubMed | Google Scholar
- Strasser R. Rural health around the world: challenges and solutions. Fam Pract. 2003 Aug;20(4):457-63. PubMed | Google Scholar
- Liu L. China´s dusty lung crisis: Rural-urban health inequity as social and spatial injustice. Soc Sci Med. 2019 Jul;233:218-28. PubMed | Google Scholar
- James WL. All rural places are not created equal: revisiting the rural mortality penalty in the United States. Am J Public Health. 2014 Nov;104(11):2122-9. PubMed | Google Scholar
- Miller CE, Vasan RS. The southern rural health and mortality penalty: A review of regional health inequities in the United States. Soc Sci Med. 2021 Jan;268:113443.. PubMed | Google Scholar
- Kulig J. The time is now: setting a rural health research agenda. Rural Remote Health. 2016 Oct-Dec;16(4):4201. PubMed | Google Scholar
- Snyder JE, Jensen M, Nguyen NX, Filice CE, Joynt KE. Defining Rurality in Medicare Administrative Data. Med Care. 2017 Dec;55(12):e164-e169. PubMed | Google Scholar
- Vanderboom CP, Madigan EA. Federal definitions of rurality and the impact on nursing research. Res Nurs Health. 2007 Apr;30(2):175-84. PubMed | Google Scholar
- Lim A, Asher MI, Ellwood E, Ellwood P, Exeter DJ. How are 'urban' and 'rural' defined in publications regarding asthma and related diseases? Allergol Immunopathol (Madr). 2014 Mar-Apr;42(2):157-61. PubMed | Google Scholar
- Roberts ME, Doogan NJ, Tanenbaum E, Stillman FA, Mumford EA, Chelluri D et al. How should we define 'rural' when investigating rural tobacco use in the United States? Subst Abus. 2021;42(4):788-795. PubMed | Google Scholar
- du Plessis V, Beshiri R, Bollman RD, Clemenson H. Rural and Small Town Canada Analysis Bulletin: Catalogue no. 21-006-XIEVol. November 2001;3(3).
- Bourke L, Humphreys JS, Wakerman J, Taylor J. Understanding rural and remote health: a framework for analysis in Australia. Health Place. 2012 May;18(3):496-503. PubMed | Google Scholar
- Canadian Institute for Health Information. Rural Health Systems Model. Accessed Mar 1, 2021.