Prevalence and determinants of osteoporosis in Congolese patients with axial rheumatism: a cross-sectional hospital-based study
Aldo Mavinga, Jenny Mbuyi, Denis Matanda, Pierrot Lebughe, Jean-Christophe Mulumba, Viviane Nyembue, Adolphe Lukusa, Jean-Paul Divengi, Thierry Lusiensie, Jean-Marie Mbuyi-Muamba, Jean-Jacques Malemba
Corresponding author: Aldo Mavinga, Rheumatology Unit, Kinshasa University Hospital, University of Kinshasa, Kinshasa, Democratic Republic of Congo 
Received: 05 Sep 2021 - Accepted: 06 Jun 2022 - Published: 25 Oct 2022
Domain: Rheumatologist
Keywords: Osteoporosis, axial pain, determinants, Kinshasa
©Aldo Mavinga et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Aldo Mavinga et al. Prevalence and determinants of osteoporosis in Congolese patients with axial rheumatism: a cross-sectional hospital-based study. Pan African Medical Journal. 2022;43:100. [doi: 10.11604/pamj.2022.43.100.31519]
Available online at: https://www.panafrican-med-journal.com//content/article/43/100/full
Research 
Prevalence and determinants of osteoporosis in Congolese patients with axial rheumatism: a cross-sectional hospital-based study
Prevalence and determinants of osteoporosis in Congolese patients with axial rheumatism: a cross-sectional hospital-based study
Aldo Mavinga1,&, ![]() Jenny Mbuyi1, Denis Matanda1,
Jenny Mbuyi1, Denis Matanda1, ![]() Pierrot Lebughe1, Jean-Christophe Mulumba1, Viviane Nyembue2, Adolphe Lukusa3,
Pierrot Lebughe1, Jean-Christophe Mulumba1, Viviane Nyembue2, Adolphe Lukusa3, ![]() Jean-Paul Divengi4, Thierry Lusiensie4, Jean-Marie Mbuyi-Muamba1, Jean-Jacques Malemba1
Jean-Paul Divengi4, Thierry Lusiensie4, Jean-Marie Mbuyi-Muamba1, Jean-Jacques Malemba1
&Corresponding author
Introduction: osteoporosis seems to be uncommon in sub-Saharan Africa. The aim of this study was to determine prevalence and determinants of osteoporosis in Congolese outpatients attending rheumatology consultation for axial rheumatism in Kinshasa, Democratic Republic of the Congo.
Methods: a cross-sectional hospital-based study from January to December 2018 among outpatients received for axial rheumatism in 8 hospitals of Kinshasa. The parameters of interest were age, sex, body mass index (BMI), alcoholism, smoking, physical activity, sunlight exposure, intake of dairy products, the notion of personal or parental fracture, a bone mineral density (BMD) and a phosphocalcic metabolism. The BMD was measured by using the dual energy X-ray absorptiométry. Serum level of calcium, Vitamin D, phosphore and parathormon were determined to assess the phosphocalcic metabolism. Osteoporosis was defined by a T-Score ≤ -2.5 SD. Standard statistical tests were used to analyze the results.
Results: ninety patients (75 women and 15 men) were included. Their mean age was 63.5 ± 12.2 years. Low back pain 71.1% (n=63) was the main symptom. The rate of patients with osteoporosis, osteopenia, and normal bone density was 34.4% (n=31), 43.9% (n=44), and 16.7% (n=15) respectively. Pathological bone fractures were not noted. Ageing (aOR: 1.31, IC95%: 1.11-1.54; p=0.002), smoking (aOR: 14.65, IC95%: 1.38-156.1; p=0.045) and non-obese status (aOR: 32.3, IC95% 1.50-696; p=0.032) were identified as determinants of osteoporosis.
Conclusion: in the present study, osteoporosis is common in Congolese patients with axial pain and is more frequent in women. Its determinants are ageing, smoking and non-obese status.
Osteoporosis is the commonly weakening disease of the skeleton. Because of its frequency as well as the high cost of its management, it constitutes a public health concern in developed countries [1,2]. The International Osteoporosis Foundation claims that at least one in three women and one in five men worldwide will suffer from this disease during their life [3]. The frequency of osteoporosis increases with age, principally over 65 years [4]. Taking into account the increase of life expectancy in developed countries, one can expect an increase in the frequency of osteoporosis and osteoporotic fractures during next decades [5]. The clinical and socio-economic burden of osteoporosis arises from the management of osteoporotic fractures [6]. The later are the basis of the morbidity and mortality due to osteoporosis [7,8].
In sub-Saharan Africa, few studies have been carried out on osteoporosis. This disease appears to be less common according to the literature because black people seem to be genetically protected by a higher bone mass when compared with Caucasian, Asian and Arab population [9]. In the Democratic Republic of Congo, a recent study found that references curves for the lumbar spine and total hip of Congolese patients are significantly different from the Caucasian, Asian or Arab normative data also explaining the low frequency of osteoporosis in our environment [10]. Based on this hypothesis born from the literature on the low frequency of this pathology in the Congolese environment as in sub-Saharan Africa, the aim of the present study was to determine the prevalence and to identify the determinants of osteoporosis in Congolese outpatients attending rheumatology unit for axial rheumatism.
Design, framework and population: a cross-sectional hospital-based study was carried from January to December 2018 on outpatients with axial rheumatism attending the rheumatology units of some hospitals of Kinshasa. These hospitals selected were: Kinshasa Medical Center, University Hospital of Kinshasa, Diamant Clinic, General Provincial Hospital of Kinshasa, HJ Hospital, Monkole Hospital Center, Ngaliema Clinic and Polymedica Center. This selection was based on the organization within them of rheumatology consultations supervised by a rheumatologist. It reliably reflected rheumatological activity throughout Kinshasa, the capital and largest city of the Democratic Republic of the Congo.
Selection and eligibility criteria: patients were recruited comprehensively and consecutively to minimize selection biais and constitute the study population. The inclusion criteria were: any patient aged at least 40 years, consulting for low back pain and/or pelvic pain evolving for at least 3 months, having freely consented to participate in the study and having all our parameters of 'interest. None-inclusion criteria were: using, the last 3 months, drugs that may influence the bone mineral density (BMD), suffering from chronic pathology (hemoglobinopathy, neoplasia, chronic infection, hemopathy, endocrinopathy, nephropathy) that may lead to a secondary osteoporosis, immobilization period of more than 6 weeks during the previous 3 months as well as the presence of skin lesions or skin abrasions at the measurement site.
Data collection: all patients in the present study were examined by a rheumatologist. Lifestyle and physical examination data were recorded. The parameters of interest were age, sex, body mass index, alcoholism, smoking, physical activity, sunlight exposure, intake of dairy products, the notion of personal or parental fracture, a bone mineral density (BMD) and a phosphocalcic metabolism.
Measurement of bone mineral density (BMD): BMD was measured by dual-energy X-ray absorptiometry (DEXA) at HJ Hospital Kinshasa, a private center, the only one with this Hologic Discovery QDR 4500 brand bone densitometry device in the country. Examination carried out in a promotional context with the installation of this device. BMD was assessed at the lumbar column and hips for about 20 minutes. In case of contraindication for one of the 2 regions, the examination was performed at the distal region of the radius. BMD was expressed as absolute values (g/cm²) and as T- score. As per with the WHO recommendations, normal BMD, osteopenia, osteoporosis, and severe osteoporosis was a T-score >-1, -2.5 < T-score ≤ -1, T-score ≤ -2.5 and T-score ≤ -2.5 with pathological fractures respectively.
Phosphocalcic metabolism assessment: to assess phosphocalcic metabolism, two milliliters of blood were used for subsequent analysis of total serum calcium, phosphoremia, plasma vitamin D (25 OH Vitamin D), and parathyroid hormone using a SHIMADZU UV 1900 brand spectrophotometer at HJ Hospital on the same day of the bone densitometry making the possibility of missing data almost nil.
Concepts' definitions: the axial rheumatism was defined by the presence of low back pain or pelvic pain evolving for at least 3 months without any major trauma. Physical activities were considered as low if any physical activity was mentioned, moderate if physical activity duration was less than an hour per week and intense for vigorous practice that causes breath shortness, rapid heartbeat once or twice a week [11]. The frequency of milk intake by patients during the past 3 months was precised. It was considered as sufficient, or insufficient when taking milk at least twice a week and less than 2 times a week respectively [12]. It was considered as null when the patient did not take milk. Exposure to sunlight was assessed by the frequency of going outside the home over a period of a week and during the past 3 months. Going out of his home every day, at least three times a week, and less than 3 times a week was considered strong, moderate, and weak exposure to sunlight respectively [13]. Consuming at least 20 and 30g of alcohol a day defined alcoholism in women and in men respectively. Moderate drinkers were defined as people drinking less than 30g of ethanol a day for men and less than 20g for women, while heavier drinkers were defined as people drinking more than 30g of ethanol a day for men and more than 20g for women [14]. Smoking ≤ 5 and >5 packet-years (PUA) was considered as lower and heavier smoking respectively [15]. The body mass index (BMI) was measured and classified as needed using WHO recommendations; spinal deformities and fractures were looked for in the patients and their first-degree relatives.
Statistical analyzes: analyzes were performed using SPSS version 21.0 software. Data were presented as average ± standard deviations for continuous quantitative data, and as absolute or relative frequency for categorical variables. The Student's t-test was used to compare means and the Pearson's Chi-squared or Fisher's exact test as appropriate for proportions. Binary logistic regression was used to identify possible determinants of osteoporosis. The adjusted odd ratio values and 95% of confidence interval have been reported. The significant level was set at P-value < 0.05.
Ethical considerations: the data was collected anonymously and confidentially after the free and informed consent of each patient. The present study was approved by the national health ethical committee (CNES) of Democratic Republic of Congo with as approval number 361/CNES/BN/PMMF/2022.
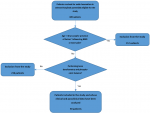
General characteristics: of the 685 patients with axial rheumatism recruited in the different selected hospitals (Figure 1), ninety patients (women: 83.3%, average age: 63.5 ± 12.2 years) were included in the present study and their general characteristics have been described in Table 1. The majority (52.2%) of them were recruited from the rheumatology unit of the University Hospital of Kinshasa. Overall prevalence of alcoholism, smoking, low activity, and overweight/obesity was 43.3%, 27.8%, 62.2%, and 74.6% respectively. The sunlight exposure was good for all the patients (Table 2).
Clinical and densitometric's characteristics: lumbar spine was the principal site (67.7%) of osteoporosis (Table 3). A normal t-score was noted in 15 patients (16.7%), an osteopenia in 44 patients (48.9%) and osteoporosis in 31 patients (34.4%). Osteoporosis was diagnosed in 29 women (38.7% of women and 93.5% of osteoporosis cases) and 2 men (13.3% of men and 6.5% of osteoporosis cases). So, the frequency of osteoporosis was 3 times higher in women than in men. One of ten patients reported a hip fracture in 1st degree relative while none of them presented an osteoporotic fracture in the present study. Low back pain was the foremost symptom (71.1%). Osteoporosis was not an isolated condition in the present study; it was associated with osteoarthritis in 59 patients (Table 4).
Phosphocalcic metabolism and osteoporosis associated factors: the mean level of calcium, phosphore, vitamin D and parathormon were normal, while a deficiency of vitamin D was noted in one third of patients (Table 5). In the univariable analysis, ageing, smoking, non-obese status, menopause duration ≥ 20 years, parent's fractures were associated with osteoporosis. In the multivariable analysis, ageing (aOR: 1.31, IC95%: 1.11-1.54; p = 0.002), smoking (aOR: 14.65, IC95%: 1.38-156.1; p = 0.045) and the non-obese status (aOR: 32.3, IC95% 1.50-696; p = 0.032) were identified as independent determinants of osteoporosis in the present study (Table 6).
The present study aim was to determine prevalence of osteoporosis and its determinants in Congolese patients followed for axial pain. Results show that osteoporosis is common in these patients and is more frequent in women. Its determinants are ageing, smoking and non-obese status. The female predominance of osteoporosis is in agreement with the literature [16]. Since osteoporosis affects mostly women, several studies have been conducted only on women [17]. This female predominance might be explained by estrogen deprivation that occurs during menopause [18]. Two-thirds of the patients were at least 60 years-old. This is in line with the studies by Ka et al. [19] in Senegal, and Haouichat et al. [20] in Algeria who reported a average age over 60. Ageing is involved in the occurrence of osteoporosis through reactive hyperparathyroidism often due to a deficiency in calcium and vitamin D. This deficiency is due to an insufficient consumption of calcium and vitamin D, a lack of exposure to solar rays or even reduction of nephronic mass [21].
BMI is strongly associated to the occurrence of osteoporosis and osteoporotic fractures [22]. Indeed, the relative risk of occurrence of osteoporosis and osteoporotic fractures increases with a BMI ≤ 20 kg/m² and tends to decrease with a BMI ≥ 30 kg/m². The role of leptin in osteoblasts differentiation and estrogens aromatization that takes place in adipocytes may protect people with a high BMI from osteoporosis [23]. At least a third of the patients suffered from osteoporosis. This is the same as the studies by Aspray et al. [24] in Gambia (28.2%), Ka et al. [19] in Senegal (41.7%) and Ngandeu et al. [25] in Cameroon (13.6%). Contrastingly to our study, Tozin et al. [26] observed that postmenopausal Congolese women lost less bone mass per decade than Caucasian women. Kabeya-Kabenkama et al. [27] suggested that Congolese women attempted their peak of bone density later than Caucasians. These authors explained that this scarcity would be linked to a genetic protection which make that blacks would have a higher bone mass than other races. The African ancestral style of life, characterized by intense physical activity and significant exposure to sunlight, would also contribute to this protection [28]. The 27.7% smoking prevalence increased considerably the risk of osteoporosis. Tobacco decreases the half-life of circulating estrogens and impairs its release from adipose tissue. Ngandeu et al. [25] in Cameroon, also described an association between smoking and osteoporosis.
A third of our patients had vitamin D deficiency. This is in vein with the results by Ntyonga-Pono et al. [29] in Gabon (43.2% of patients) and Maataoui et al. [30] in Morocco (77.4% of patients). The vitamin D deficiency may be explained by the shelter effect of black skin which is rich in melanin, the clothing habits covering almost all from the body and an insufficient consumption of calcium and vitamin D. Concerning consumption of dairy products for example, 57.7% of patients reported having little or no milk consumption. No association has been found between the level of physical activity or alcohol consumption and osteoporosis.
The small size of the sample in the present study may explain the lack of association between other risk factors that are well known and closely linked to the occurrence of osteoporosis. The hospital nature of the study does not allow its results to be extrapolated to the general population. The credit for this study, however, is that it investigated osteoporosis using the benchmark tool and provided data showing that patients with axial rheumatism are candidates for osteoporosis.
The present study suggests that osteoporosis is frequent in Congolese patients suffering from axial rheumatic disorders, with a strong female predominance. Severe osteoporosis was not observed among these patients. Ageing, smoking and non-obese status were retained as the determinants of osteoporosis.
What is known about this topic
- Osteoporosis is a public health problem in developed countries because of its high frequency and the exorbitant cost of its management; in sub-Saharan Africa, Osteoporosis seems infrequent because Black Africans seem genetically protected by a high bone mass;
- The axial skeleton is a common site of osteoporotic fractures; the later are associated to a worsening mortality and morbidity in osteoporosis;
- The principals' determinants of osteoporosis are genetic factors, menopause, advanced age, sedentary life style, calcium and vitamin D deficiency.
What this study adds
- Osteoporosis is frequent in Congolese patients with axial skeleton pain but fracture risk may be low;
- The use of DEXA highlighted the true extent of osteoporosis in the Congolese environment;
- Ageing, non-obese status and smoking are associated to osteoporosis in Congolese patients.
The authors declare no competing interests.
Aldo Mavinga conceived the study, collected and interpreted data and wrote the article. Jenny Mbuyi, Denis Matanda, Pierrot Lebughe, Jean-Christophe Mulumba, Viviane Nyembue, Adolphe Lukusa, Jean-Paul Divengi and Thierry Lusiensie collected data. Jean-Marie Mbuyi-Muamba collected, interpreted data and revised the manuscript. Jean-Jacques Malemba has a substantial contribution in the conception of the study, the acquisition of the data and the revision of the article. All authors read and approved the final version of the manuscript.
Table 1: general characteristics of patients (n=90)
Table 2: patients' antecedents and life habits (n=90)
Table 3: patients' densitometric characteristics (n=90)
Table 4: patients' clinical feature
Table 5: parameters of phosphocalcic metabolism
Table 6: determinants of osteoporosis
Figure 1: flow diagram showing numbers of patients at each stage of study
- Haute autorité de santé. Recommandations sur la prévention, le diagnostic et le traitement de l'ostéoporose: notes de synthèse. Septembre, 2006.
- Funck-Brentano T, Cohen-Solal M. Le vieillissement osseux: les nouveaux acteurs de communication intercellulaire. Médecine et Longévité. 2010;2:200-4. Google Scholar
- Francis C, Tafforeau J, Herman VO. Ostéoporose et fractures de la hanche: état des connaissances en Belgique et apport d'éléments pour l'élaboration d'une politique de santé. Institut de santé publique centre de recherche opérationnelle en santé publique. Novembre, 1999.
- Valentine M. Ostéoporose: état des lieux, perspectives et rôle du pharmacien d'officine dans sa prise en charge. Sciences pharmaceutiques. 2012;47:20-4.
- Malemba JJ, Mbuyi-Muamba JM. Clinical and epidemiological features of rheumatic diseases in patients attending the university hospital in Kinshasa. Clin Rheumatol. 2008 Jan;27(1):47-54. PubMed | Google Scholar
- Laffargue AL. Validation d'un score de risque de fracture ostéoporotique: étude sur une population du bassin nancéen. Thèse de doctorat en médecine. Université de Nancy, 2009. Google Scholar
- Ferrari SL, Deutsch S, Choudhury U, Chevalley T, Bonjour JP, Dermitzakis ET et al. Polymorphisms in the low-density lipoprotein receptor-related protein 5 (LRP5) gene are associated with variation in vertebral bone mass, vertebral bone size, and stature in whites. Am J Hum Genet 2004; 74(5): 866-75. Google Scholar
- Chen P, Li Z, Hu Y. Prevalence of osteoporosis in China: a meta-analysis and systematic review. BMC Public Health. 2016;16(1):1039-42. PubMed | Google Scholar
- Organisation Mondiale de la Santé. Normes de croissance de l'enfant: cours de formation sur l'évaluation de la croissance de l'enfant. Genève, OMS, 2008. Google Scholar
- Garner P. Nouveaux marqueurs biologiques du remodelage osseux dans l'ostéoporose. Médecine nucléaire. 2009;33(1):17-27. Google Scholar
- Organisation Mondiale de la Santé. Stratégie mondiale pour l'alimentation, l'exercice physique et la santé: recommandations mondiales en matière d'activité physique pour la santé. Genève, 2019.
- Fardellone P, Cotté FE, Roux C, Lespessailles E, Merciere F, Gaudinf AF. Apport de calcium et risque d'ostéoporose et de fractures chez les femmes françaises. Revue du rhumatisme. 2010;77(2):182-7. Google Scholar
- Parfitt AM. Trabecular bone architecture in the pathogenesis and prevention of fracture. Am J Med. 1987 Jan 26;82(1B):68-72. PubMed | Google Scholar
- Favrod TC, Guessous I. L'alcool en médecine de premier recours. Département de médecine communautaire, de premier recours et des urgences. Hôpitaux Universitaires de Genève, 2017.
- Martine Y, Bohadana A. Tabagisme: de la prévention au sevrage. 1ère édition. Masson, Paris, 1997.
- Luckey M, Wallenstrein S, Lapinski R, Meier DE. A prospective study, of bone loss in African American and white woman; a clinical research center study. J Clin Endocrinol Metab. 1996 Aug;81(8):2948-56. PubMed | Google Scholar
- Dibba B, Prentice A, Laskey MA, Stirling DM, Cole TJ. An investigation of ethnic differences in bone mineral, hip axis, length, calcium metabolism and bone turnover between West African and Caucasian adults living in the United Kingdom. Ann Hum Biol. 1999 May-Jun;26(3):229-42. PubMed | Google Scholar
- Knobel J, Pick G, Burger H. No osteoporosis detected by quantitative computed tomography in post-menopausal black females. South African medical journal. 1992;82(3):184-5. Google Scholar
- Ka O, Miryem E, Faye A, Leye MMM, Ndongo S. How bone densitometry contributes to the diagnosis of osteoporosis at Ouaka's gerontology and geriatrics center in Dakar City: A study based on the observation of 102 cases. Mali Med. 2016;31(4):37-47. PubMed | Google Scholar
- Haouichat C, Hammoumraoui N, Lehtihet S. Prevalence of postmenauposal osteoporosis in Algerian women. Ann rheum dis. 2014;73:760-760.
- Carmen GV. The activity of a Spanish bone densitometry unit revisited under the point of view of FRAX. Reumatol Clin. 2012;8(4):179-83. PubMed | Google Scholar
- Haugeberg G, Uhlig T, Falch JA, Halse JI, Kvien TK. Bone mineral density and frequency of osteoporosis in female patients with rheumatoid arthritis: results from 394 patients in the Oslo County Rheumatoid Arthritis register. Arthritis Rheum. 2000 Mar;43(3):522-30. PubMed | Google Scholar
- Ruhl CE, Everhart JE. Relationship of serum leptin concentration with bone mineral density in the United States population. J Bone Miner Res. 2002;17(10):1896-903. PubMed | Google Scholar
- Aspray TJ, Prentice A, Cole TJ, Sawo Y, Reeve J, Francis RM. Low bone mineral content is common but osteoporotic fractures are rare in elderly Gambian women. J Bone Miner Res. 1996;11:1019-1025. PubMed | Google Scholar
- Ngandeu S, Nko'o A. Densité minérale osseuse de la femme camerounaise à Yaoundé: une étude échographique. Mali medical. 2008;1:22-6. Google Scholar
- Tozin R. Contribution à l'étude de la pathologie de l'ostéoporose post-ménopausique chez la femme congolaise. Thèse d'agrégation à l'enseignement supérieur en médecine. Université de Kinshasa, 2000.
- Kabeya-Kabenkama JM, Tshibola JM, Tshikwela ML, Rahma T, Malemba JJ, Westhovens R et al. Ultrasound assessment of bone mass in central Africans population. Research in Health Science. 2017;2(4):323-4. Google Scholar
- El Maataoui A, Biaz A, El Boukhrissi F, El Machtani S, Dami A, Bouhsain S et al. Association between sex hormones, bone remodeling markers and bone mineral density in postmenopausal women of Moroccan origin. Pan Afr Med J. 2015;22:106. PubMed | Google Scholar
- Ntyonga-Pono MP. Vitamin D deficiency in adults in Gabon: isolated case or unrecognized problem? Pan Afr Med J. 2014;19:183. PubMed | Google Scholar
- El Maataoui A, Biaz A, El Machtani S, Bouhsain S, Dami A, El Maghraoui A et al. Vitamin D status in healthy Moroccan men and women aged 50 years and older: a cross-sectional study. Arch Osteoporos. 2016 Dec;11(1):24. PubMed | Google Scholar