Cervical Pott's disease: case report and review of the literature
Dognon Kossi François de Paule Adjiou, Michèle Yolande Moune, Fresnel Lutèce Ontsi Obame, José Dimbi Makoso, Nourou Dine Adeniran Bankole, Mustapha Hemama, Nizare El Fatemi, Mouley Rachid El Maaqili
Corresponding author: Dognon Kossi François de Paule Adjiou, Faculty of Medicine and Pharmacy, Mohamed V University of Rabat, Rabat, Morocco 
Received: 22 Feb 2022 - Accepted: 21 Jun 2022 - Published: 22 Aug 2022
Domain: Neuroradiology,Head, Neck and Reconstructive Surgery,Neurosurgery
Keywords: Tuberculosis, spinal, management, case report
©Dognon Kossi François de Paule Adjiou et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Dognon Kossi François de Paule Adjiou et al. Cervical Pott's disease: case report and review of the literature. Pan African Medical Journal. 2022;42:299. [doi: 10.11604/pamj.2022.42.299.33951]
Available online at: https://www.panafrican-med-journal.com//content/article/42/299/full
Cervical Pott's disease: case report and review of the literature
![]() Dognon Kossi François de Paule Adjiou1,2,&, Michèle Yolande Moune1,2,
Dognon Kossi François de Paule Adjiou1,2,&, Michèle Yolande Moune1,2, ![]() Fresnel Lutèce Ontsi Obame1,2, José Dimbi Makoso1,2, Nourou Dine Adeniran Bankole1,2,
Fresnel Lutèce Ontsi Obame1,2, José Dimbi Makoso1,2, Nourou Dine Adeniran Bankole1,2, ![]() Mustapha Hemama1,2, Nizare El Fatemi1,2, Mouley Rachid El Maaqili1,2
Mustapha Hemama1,2, Nizare El Fatemi1,2, Mouley Rachid El Maaqili1,2
&Corresponding author
Tuberculosis is a major public health problem in the world. Spinal tuberculosis (Pott disease) is a frequently encountered extrapulmonary form of the disease. Cervical spinal tuberculosis is relatively rare. We report the case of a 66-year-old patient admitted for cervical Pott's disease managed surgically and the positive outcome. A patient with a history of pulmonary tuberculosis present 3 months ago persistent neck pain with tingling and heaviness in both upper limbs. The neurological examination was normal without any sensory or motor deficit. Spinal cord magnetic resonance imaging (MRI) showed a lesion centered on the vertebral body of C4 with spinal cord compression and epiduritis without signs of spinal cord injury. The patient underwent a corpectomy of C3 and C4 with an iliac graft and anterior cervical plate. The anatomopathological examination revealed a Pott disease. He was therefore put on antituberculous chemotherapy for 12 months. Three months later the neck pain and tingling disappeared in the upper limbs. Cervical Pott's disease is relatively rare. Surgical management is indicated in the case of spinal instability or spinal cord compression.
Tuberculosis is a major public health problem in the world. Spinal tuberculosis (TB) is the most common musculoskeletal manifestation, affecting about 1 to 2% of all cases of TB [1]. Cervical spinal tuberculosis (Pott's disease) is relatively rare, and its incidence varies from 2% to 12% [2]. The treatment approaches to cervical spine tuberculosis fluctuated between conservative therapy and surgery [3]. We report a case of cervical Pott's disease managed surgically and the positive outcome in the light of previous literature.
Clinical presentation: a 66-year-old patient with a history of pulmonary tuberculosis treated in 1997, declared cured, and high blood pressure present three months ago persistent neck pain with tingling and heaviness in both upper limbs. At the neurological examination, the muscular testing was normal and no sensory deficit. The American Spinal Injury Association (ASIA) score was graduated E.
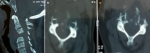
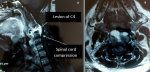
Diagnosis assessment: cervical spine computed tomography (CT) showed a lytic process centered on C4 with posterior wall recession and anterior epiduritis (Figure 1). Spinal cord magnetic resonance imaging (MRI) showed a cervical lytic lesion centered on the vertebral body of C4 with spinal cord compression and epiduritis without signs of spinal cord injury (Figure 2).
Management: the patient underwent corpectomy of C3 and C4 with iliac graft and anterior cervical plate (Figure 3). Then a reinforced neck brace was applied 2 weeks after the surgery to enable consolidation. The anatomopathological examination revealed a Pott disease. The patient was put on antituberculosis chemotherapy treatment for 12 months: 2 months of Rifampicin - Isoniazid - Pyrazinamid - Ethambutol (RHZE) followed by 10 months of Rifampicin-Isoniazid (RH).
Outcomes: at discharge, 2 weeks after surgery, the patient presented the same neurological state as at admission.
Follow up: the patient was seen in outpatient three months later. No complaint was noted, and neurological examination was normal.
Declaration of patient consent: the authors certify that they have obtained all appropriate patient consent.
We report the case of a 66-year-old patient with a history of treated pulmonary tuberculosis in 1997, admitted for cervical pains and heaviness of the upper limbs, ASIA E, and in whom the explorations came back in favour of a cervical Pott's disease that we managed surgically by an anterior approach. The management of stable cervical spine Pott's disease was previously controversial. The surgical treatment of cervical spine Pott�s disease is practiced worldwide. However, its indications are well described in literature [4] and they are based on results of clinical and radiologic investigations.
The clinical presentation of cervical spine Pott�s disease is not specific. The average time between the onset of symptoms and diagnosis is highly variable from one to several months (Table 1, Table 1 (suite)). The clinical signs can range from isolated neck pain to a sensitivo-motor deficit whoever the main symptoms at onset are neck pain and restricted neck movement. The smaller canal dimension, proximity to vertebral artery and other vital structures, unique facetal architecture, higher mobility and lordotic alignment make the cervical spine vulnerable to greater neuro-deterioration, instability, and progressive mal-alignment [5]. Our patient presented persistent neck pain with tingling and heaviness in both upper limbs. The average time from symptom onset to diagnosis was 3 months.
Because of the high risk of neurological deficits due to epidural compression of the cervical spine or spinal instability, the diagnosis should be made at the first symptoms and investigations should be done accordingly. Magnetic resonance imaging is considered the investigation of choice in spinal infection because it has high sensitivity and satisfactory specificity. The advantages of CT over MRI are that CT offer more reliable detection of calcified foci and they also provide guidance on the need for interventional procedures. Anterior approach is the gold standard in surgical management because lesions are located predominantly on the anterior column [2]. Performing anterior debridement and bone grafting fusion with instrumentation, has the advantages of direct access to the focus of the disease, bony union, and stabilization of the spine. Anti-TB treatments are systematic as soon as the bacteriological examination confirms the presence of mycobacterium tuberculosis.
Surgery and conservative management are treatment options of spinal TB. Surgical procedure should be considered in patients with extensive spine involvement, severe deformity, vertebral body collapse, prevertebral cervical abscess, advanced neurological involvement, and any sign of progressive recovery despite of conservative therapy [6]. Our patient underwent a corpectomy of C3 and C4 with iliac graft and anterior cervical plate. Then a reinforced neck brace was applied for 3 months. The evolution is often favorable when patients are managed as soon as the first symptoms appear.
The anterior approach is the most used. Most patients showed an improvement of the neurological status in case of preoperative neurological deficit. In our case, the patient benefited from an anterior approach with improvement of neurological status 3 months after surgery. Table 1 and Table 1 (suite) summarizes the data from the literature review [2,7-15].
Tuberculosis is an empirical but still prevalent infectious disease. It is a real public health problem. Cervical vertebral localizations, although rare, can always occur in patients treated for pulmonary tuberculosis. The management is based on anti-tuberculosis treatments and surgery by posterior, anterior or combined approaches is indicated on a case-by-case basis if spinal instability or spinal cord compression.
Disclosures: the authors did not receive any funding for the preparation of this case report. This article is an original work that is not being considered or reviewed by any other publication and has not been published elsewhere in the same or a similar form. All authors of the manuscript have read and agreed to its content and are accountable for all aspects of the accuracy and integrity of the manuscript.
The authors declare no competing interests.
Dognon Kossi François de Paule Adjiou, Michele Yolande Moune, and Fresnel Lutèce Ontsi Obame: conceptualisation, and writing original draft-editing. Nourou Dine Adeniran Bankole: writing, review, editing and supervision; José Dimbi Makoso: supervision; Mustapha Hemama, Nizare El Fatemi, Mouley Rachid El Maaqili: supervision and validation. All the authors have read and agreed to the final manuscript.
Table 1: review of literature on cervical spine Pott disease
Table 1 (suite): review of literature on cervical spine Pott disease
Figure 1: (A,B,C) cervical spine CT, lytic process centered on C4 with posterior wall recession
Figure 2: (A,B) spinal cord MRI, cervical lytic lesion on the vertebral body of C4 with spinal cord compression and epiduritis
Figure 3: (A,B) corpectomy of C3 and C4 with iliac graft and anterior cervical plate
- Dunn RN, Ben Husien M. Spinal tuberculosis: review of current management. Bone Jt J. 2018;100-B(4):425-31. PubMed | Google Scholar
- Yin XH, He BR, Liu ZK, Hao DJ. The clinical outcomes and surgical strategy for cervical spine tuberculosis: a retrospective study in 78 cases. Medicine (Baltimore). 2018;97(27):e11401. PubMed | Google Scholar
- Bhandari A, Garg RK, Malhotra HS, Verma R, Singh MK, Jain A et al. Outcome assessment in conservatively managed patients with cervical spine tuberculosis. Spinal Cord. 2014;52(6):489-93. PubMed | Google Scholar
- Ali A, Musbahi O, White VLC, Montgomery AS. Spinal tuberculosis: a literature review. JBJS Rev. 2019;7(1):e9. PubMed | Google Scholar
- Shetty AP, Viswanathan VK, Rajasekaran S. Cervical spine TB - current concepts in management. J Orthop Surg. 2021;29(1_suppl):23094990211006936. PubMed | Google Scholar
- Alam MS, Phan K, Karim R, Jonayed SA, Munir HK, Chakraborty S et al. Surgery for spinal tuberculosis: a multi-center experience of 582 cases. J Spine Surg. 2015;1(1):65-71. PubMed | Google Scholar
- He M, Xu H, Zhao J, Wang Z. Anterior debridement, decompression, bone grafting, and instrumentation for lower cervical spine tuberculosis. Spine J. 2014;14(4):619-27. PubMed | Google Scholar
- Wu W, Li Z, Lin R, Zhang H, Lin J. Anterior debridement, decompression, fusion and instrumentation for lower cervical spine tuberculosis. J Orthop Sci. 2020;25(3):400-4. PubMed | Google Scholar
- Bunmaprasert T, Dongsang K. Cervical spinal tuberculosis: a preliminary study of clinical diagnosis and management. J Med Assoc Thai. 2015;98(1):33-8. PubMed | Google Scholar
- Xing S, Gao Y, Gao K, Zhang G, Yu Z. Anterior cervical retropharyngeal debridement combined with occipital cervical fusion to upper cervical tuberculosis. Spine (Phila Pa 1976). 2016;41(2):104-10. PubMed | Google Scholar
- Mao N, Shi Z, Ni H, Zhao Y, Tang H, Liu D et al. Long-term outcomes of one-stage anterior debridement, bone grafting, and internal fixation for the treatment of lower cervical tuberculosis with kyphosis. Br J Neurosurg. 2013;27(2):160-6. PubMed | Google Scholar
- Elsawaf A. Outcome of surgical versus conservative management of cervical spine myelopathy secondary to cervical tuberculosis. Neurosurg Rev. 2013;36(4):621-8; discussion 628. PubMed | Google Scholar
- Koptan W, Elmiligui Y, Elsharkawi M. Single stage anterior reconstruction using titanium mesh cages in neglected kyphotic tuberculous spondylodiscitis of the cervical spine. Eur Spine J. 2011;20(2):308-13. PubMed | Google Scholar
- Raja RA, Sheikh AD, Hussain M, Agani SA. Early recovery and stabilisation with instrumentation in anterior cervical spine tuberculosis. J Ayub Med Coll Abbottabad. 2012;24(3-4):93-6. PubMed | Google Scholar
- Wang X-Y, Luo CK, Li W-W, Wu P, Pang XY, Xu ZQ et al. A practical therapeutic protocol for cervical tuberculosis. Eur J Trauma Emerg Surg. 2013;39(1):93-9. PubMed | Google Scholar