Stereotactic radiosurgery with Cyberknife®: first case in the United Arab Emirates (a case report)
Nandan Maruti Shanbhag, Christos Antypas, Abdul Karim Msaddi, Teekendra Singh, Sinead Catherine Murphy, Benjie Baguitan
Corresponding author: Nandan Maruti Shanbhag, Neuro Spinal Hospital, Dubai, United Arab Emirates 
Received: 19 Jan 2022 - Accepted: 03 Aug 2022 - Published: 10 Aug 2022
Domain: Oncology
Keywords: Stereotactic radiosurgery, Cyberknife®, precision radiotherapy, case report
©Nandan Maruti Shanbhag et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nandan Maruti Shanbhag et al. Stereotactic radiosurgery with Cyberknife®: first case in the United Arab Emirates (a case report). Pan African Medical Journal. 2022;42:267. [doi: 10.11604/pamj.2022.42.267.33358]
Available online at: https://www.panafrican-med-journal.com//content/article/42/267/full
Case report 
Stereotactic radiosurgery with Cyberknife®: first case in the United Arab Emirates (a case report)
Stereotactic radiosurgery with Cyberknife®: first case in the United Arab Emirates (a case report)
![]() Nandan Maruti Shanbhag1,&, Christos Antypas1, Abdul Karim Msaddi1,
Nandan Maruti Shanbhag1,&, Christos Antypas1, Abdul Karim Msaddi1, ![]() Teekendra Singh1, Sinead Catherine Murphy1, Benjie Baguitan1
Teekendra Singh1, Sinead Catherine Murphy1, Benjie Baguitan1
&Corresponding author
A 64-year-old gentleman was referred to the department of oncology with severe pain in the right ear radiating to the right side of the face. Imaging revealed a large extra-axial expansile lesion, surrounding and encasing the right cavernous sinus extending to the right middle cranial fossa. The patient consulted several neurosurgeons and was recommended stereotactic radiosurgery with Cyberknife® as the best non-invasive modality. The proximity to the critical structures, such as the brainstem, made it challenging for any surgical approach. The patient completed stereotactic radiosurgery with Cyberknife® and is doing well one month after treatment.
With 4807 new cases registered in 2020, cancer is among the leading causes of mortality in the United Arab Emirates [1]. Tumours of the nervous system are a part of new cases being diagnosed every year, with many of them difficult to manage either due to their size or proximity to the critical structures. Cavernous sinus mass has a wide variety of differential diagnoses with meningioma followed by schwannomas of the cranial nerves.
Surgery continues to be the primary modality in many cases but is associated with higher rates of neurovascular damage and sometimes massive bleeding [2]. In such instances, stereotactic radiosurgery has emerged as the primary modality of treatment that can be delivered with precision accuracy and safely utilising machines such as Cyberknife® [3]. Cyberknife® is a non-invasive treatment for benign and malignant conditions where radiation therapy is indicated. The case was reviewed during the multidisciplinary meeting (tumour board), the benefits and risks of the various treatments were discussed and agreed to the treatment plan - stereotactic radiosurgery with Cyberknife®.
The indication for Cyberknife® was two-fold, firstly the proximity of the tumour to the critical structures, secondly, the surgical risks involved. The patient's written informed consent was obtained after discussing the treatment plan, including the treatment safety, adverse effects, and other alternative treatment options. We also considered the patient preference for a non-invasive modality as the patient was sceptical about the surgical interventions due to the risks involved.
The patient was well until six months ago when he developed severe pain in the right ear radiating to the right side of the face. He describes the pain as being "sharp shooting pain" and radiating to the lower part of the face. The pain was a 9/10 on a pain scale [4]. This he noticed was exaggerated after he extracted his last upper molar on the right side. He immediately consulted a neurologist who referred him to a neurosurgeon, and imaging confirmed an extra-axial mass in the proximity of the right cavernous sinus. The patient then was explained that any surgical intervention, including a biopsy, was risky given the proximity of the lesion to the critical structures. The patient has been hypertensive on medications for more than 15 years, related to myocardial infarction with a history of multiple stents. Hyperlipidemia on medications and most recently has recovered from COVID-19. He was incidentally diagnosed with an aortic aneurysm during the workup for SARS-CoV-2 infection. He also has a history of cataracts. He has been treated for prostatitis. He had lower back surgery for a lump excision, probably a lipoma.
Clinical findings: there were no significant clinical findings on examination and no neurological deficits.
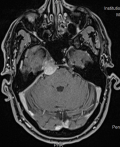
Diagnostic assessment: a well-defined extra-axial soft tissue lesion measuring 26 x 20 x 24 mm is seen around the right cavernous sinus encasing the vessels without affecting its lumen. It is seen paralleling the grey matter intensity signal, relatively effacing the right side of the pons with diffuse homogeneous post gadolinium enhancement and dural tail enhancement extending overlying the right side of the clivus bone. There is no extension within the right internal auditory canal (yet just reaching its outer edge) (Figure 1).
Diagnosis: probable differentials include meningioma (most probable), schwannoma of the cranial nerves and very unlikely a carcinoma, inflammation, or a hemorrhagic process.
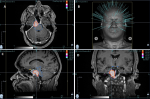
Therapeutic interventions: the treatment included simulation, contouring, plan generation, plan quality assurance plan approval and treatment delivery. During simulation, the patient was immobilized with a customized, non-invasive 2.4 mm thermoplastic mask formed over the face and affixed to an acrylic baseplate frame attached directly to the cyberknife® couch. For patient comfort, a custom-formed pillow (AccuForm™, Civco Medical Systems, Orange City, USA) was used and shaped around the base of the head to hold its shape indefinitely. The non-contrast computed tomography (CT) scan was fused with contrast-enhanced CT and the T1 weighted magnetic resonance imaging (MRI), both with 1 mm slice thickness, to delineate the target and the organs at risk. Plan evaluation was done with a close observation of the Isodose distribution and the dose volume histogram and approved after the set parameters were met (Figure 2).
For treatment delivery with image guidance, 6D skull tracking mode was used. At the same time, the patient was positioned on the treatment Robo-couch in the same position as during simulation, using in-room lasers. For initial patient alignment, orthogonal kV X-ray pairs were acquired using an in-room imaging system and compared with the planning digitally reconstructed radiographs (DRR) using the 2D-3D image registration method [5]. Initial set-up errors were detected and corrected by Robo-couch movement, thus bringing the patient to the treatment position. After the treatment started, real-time deviations were continuously recorded and adjusted by the robotic arm. The robot can automatically correct up to ±10 mm in all translational axes and up to ±1.5 degrees in all rotational axes without moving the patient [6,7]. Imaging interval varied between 20 seconds up to 45 seconds depending on the patient´s movement, minimizing intrafraction inaccuracy. A dose of 14Gy (80%) was delivered in a single fraction.
Follow-up and outcome of interventions: the patient was followed up in 3 weeks and is doing well with no adverse reactions, and the pain has significantly subsided.
Patient perspective: “I have been diagnosed as a patient with a benign brain tumour, and all the neurosurgeons that i have met advised of stereotactic radiation surgery as the most suitable treatment in such case. I got treatment by the cyber-knife robotic radiation surgery which is a very advanced technique in such a case. During the procedure, I felt no pain nothing just lying down with no movement until they told me that it is finished, for me, it is an amazing treatment as I didn't expect it to be such easy, and after the treatment, I walked normally and even my family when I met them and saw me walking normally and talking to them, they didn't believe it. Now, after the treatment, I practice my life normally, and no side effects are observed. My perspective about the treatment is positive, and the most important for me is that it is safe and with no risk”.
Informed consent: the patient signed a written informed consent.
The clinical management of a patient with central nervous tumours is challenging. This is primarily due to the proximity to the critical structures. In cases such as those close to or involving the cavernous sinus, there is fear of causing massive bleeding in addition to the damage caused to the nerve structures leading to permanent morbidity. With excision being risky, stereotactic radiation techniques - stereotactic radiosurgery (SRS) and stereotactic radiotherapy (SRT) - have emerged as safe modalities, either adjuvant or in some instances as the primary modality with 5-yr progression-free survival rates close to 90% [8]. More importantly, post-treatment neurological deficits have been low, and preservation rates close to 100% [9].
Stereotactic radiosurgery (SRS) delivers a high radiation dose in a single sitting. At the same time, stereotactic radiotherapy (SRT) or hypofractionated stereotactic radiotherapy refers to the delivery of radiation (usually more than 5Gy) in divided doses [10]. SRS is either delivered as adjuvant therapy or even as a primary modality in early grade or benign World Health Organization (WHO) tumours, including meningiomas, as the local control is similar. There is no standard grading system to guide a clinician for treatment selection as either SRS or SRT. This largely depends on the size of the tumour, location, and proximity to critical structures. In general, a cavernous sinus meningioma, well contained within the region and size not exceeding 3cm, SRS is preferred and safely delivered. For a larger tumour enclosing the eloquent structures, SRT is preferable [11]. The dose delivered with SRS ranges from 11Gy - 19Gy for WHO grade 1 meningiomas, and some studies have supported lower marginal doses of 12Gy for benign cavernous sinus tumours [12,13].
Cavernous sinus meningiomas larger in size, hypofractionated stereotactic radiotherapy is preferred as it provides equivalent tumour control and lesser side effects than SRS [14-16]. The ideal follow-up and response time for the cavernous sinus meningiomas has been a matter of debate. Some of the tumours have been known to remain stable for almost two years before regression. As a general clinical practice, the patient is followed up three weeks after the treatment and then every three months for the first year and every six months for the following two years and then once a year for regular follow-up. Imaging studies are done three months after the treatment and at the end of 1 year to assess response to treatment [17,18]. Radiological and clinical examinations, including neurological and ophthalmological assessments, could be extended to a longer time interval depending on the initial follow-up results and patient symptoms.
Central nervous tumours provide a comprehensive set of challenges for treatment due to the presence of critical structures in proximity. Often, surgery risks damaging these structures and may lead to permanent morbidity. Novel treatment techniques like stereotactic radiosurgery with the Cyberknife® robotic system are emerging as primary treatment modalities and must be explored further. This is the first case treated with stereotactic radiosurgery with Cyberknife® in the United Arab Emirates and demonstrates that such treatments can be delivered with safety and precision.
The authors declare no competing interest.
NMS wrote the manuscript draft; CA wrote the physics and treatment plan; TS and SCM gave details about the treatment delivery; BB helped format the manuscript and wrote references for the introduction; AKM notes were utilized. All the authors have read and agreed to the final manuscript.
We want to thank the other therapists, Mr. Nikhil Jose, Ms. Muriel Burke, and admin staff Ms. Viktoria Kmetyk for helping with records.
Figure 1: T1 MRI with contrast (coronal) showing the mass near the right cavernous sinus
Figure 2: (A,B,C,D) the Cyberknife® Accuray® precision plan, isodose and dose volume histogram
- Al-Shamsi H, Darr H, Abu-Gheida I, Ansari J, McManus MC, Jaafar H et al. The state of cancer care in the United Arab Emirates in 2020: challenges and recommendations, a report by the United Arab Emirates oncology task force. Gulf J Oncolog. 2020 Jan;1(32):71-87. PubMed | Google Scholar
- Raheja A, Couldwell WT. Cavernous sinus meningioma. Handb Clin Neurol. 2020;170:69-85. PubMed | Google Scholar
- Lee CC, Trifiletti DM, Sahgal A, DeSalles A, Fariselli L, Hayashi M et al. Stereotactic radiosurgery for benign (World Health Organization grade I) cavernous sinus meningiomas-International Stereotactic Radiosurgery Society (ISRS) practice guideline: a systematic review. Neurosurgery. 2018;83(6):1128-42. PubMed | Google Scholar
- Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: visual analog scale for pain (vas pain), numeric rating scale for pain (nrs pain), mcgill pain questionnaire (mpq), short-form mcgill pain questionnaire (sf-mpq), chronic pain grade scale (cpgs), short form-36 bodily pain scale (sf-36 bps), and measure of intermittent and constant osteoarthritis pain (ICOAP). Arthritis Care Res (Hoboken). 2011;63(S11):S240-S52. PubMed | Google Scholar
- Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET et al. Toxicity and response criteria of the eastern cooperative oncology group. Am J Clin Oncol. 1982;5(6):649-55. PubMed | Google Scholar
- Fu D, Kuduvalli G. A fast, accurate, and automatic 2D-3D image registration for image-guided cranial radiosurgery. Med Phys. 2008;35(5):2180-94. PubMed | Google Scholar
- Li G, Ballangrud A, Chan M, Ma R, Beal K, Yamada Y et al. Clinical experience with two frameless stereotactic radiosurgery (fSRS) systems using optical surface imaging for motion monitoring. J Appl Clin Med Phys. 2015;16(4):149-62. PubMed | Google Scholar
- De Jesús O, Sekhar LN, Parikh HK, Wright DC, Wagner DP. Long-term follow-up of patients with meningiomas involving the cavernous sinus: recurrence, progression, and quality of life. Neurosurgery. 1996;39(5):915-20. PubMed | Google Scholar
- Hasegawa T, Kida Y, Yoshimoto M, Koike J, Iizuka H, Ishii D. Long-term outcomes of gamma knife surgery for cavernous sinus meningioma. J Neurosurg. 2007;107(4):745-51. PubMed | Google Scholar
- Solberg TD, Balter JM, Benedict SH, Fraass BA, Kavanagh B, Miyamoto C et al. Quality and safety considerations in stereotactic radiosurgery and stereotactic body radiation therapy: executive summary. Pract Radiat Oncol. 2012;2(1):2-9. PubMed | Google Scholar
- De Salles AA, Frighetto L, Grande CV, Solberg TD, Cabatan-Awang C, Selch MT et al. Radiosurgery and stereotactic radiation therapy of skull base meningiomas: proposal of a grading system. Stereotact Funct Neurosurg. 2001;76(3-4):218-29. PubMed | Google Scholar
- Kreil W, Luggin J, Fuchs I, Weigl V, Eustacchio S, Papaefthymiou G. Long term experience of gamma knife radiosurgery for benign skull base meningiomas. J Neurol Neurosurg Psychiatry. 2005;76(10):1425-30. PubMed | Google Scholar
- Pollock BE, Stafford SL, Link MJ. Stereotactic radiosurgery of intracranial meningiomas. Neurosurg Clin N Am. 2013 Oct;24(4):499-507. PubMed | Google Scholar
- Manabe Y, Murai T, Ogino H, Tamura T, Iwabuchi M, Mori Y et al. CyberKnife stereotactic radiosurgery and hypofractionated stereotactic radiotherapy as first-line treatments for imaging-diagnosed intracranial meningiomas. Neurol Med Chir (Tokyo). 2017;57(12):627-633. PubMed | Google Scholar
- Alfredo C, Carolin S, Güliz A, Anne K, Antonio P, Alberto C et al. Normofractionated stereotactic radiotherapy versus CyberKnife-based hypofractionation in skull base meningioma: a German and Italian pooled cohort analysis. Radiat Oncol. 2019;14(1):201. PubMed | Google Scholar
- Nguyen EK, Nguyen TK, Boldt G, Louie AV, Bauman GS. Hypofractionated stereotactic radiotherapy for intracranial meningioma: a systematic review. Neurooncol Pract. 2019;6(5):346-53. PubMed | Google Scholar
- Nguyen EK, Pond GR, Greenspoon JN, Whitton AC, Hann C. Hypofractionated stereotactic radiotherapy for the treatment of benign intracranial meningiomas: long-term safety and efficacy. Curr Oncol. 2021;28(5):3683-91. PubMed | Google Scholar
- Rogers L, Barani I, Chamberlain M, Kaley TJ, McDermott M, Raizer J et al. Meningiomas: knowledge base, treatment outcomes, and uncertainties. A RANO review. J Neurosurg. 2015;122(1):4-23. PubMed | Google Scholar