Multisystemic sarcoidosis revealed by a Heerfordt syndrome: case report
Glad Smart Moussounda Mpika, Paulvon Phérol Koumeka, Lamyae Amro
Corresponding author: Glad Smart Moussounda Mpika, Pneumology Department, Mohammed VI University Hospital, Faculty of Medicine and Pharmacy of Marrakech, Cadi Ayyad University, Marrakech, Morocco 
Received: 01 Mar 2022 - Accepted: 08 Mar 2022 - Published: 29 Jun 2022
Domain: Pulmonology
Keywords: Granulomatosis, anterior uveitis, parotiomegaly, facial paralysis, case report
©Glad Smart Moussounda Mpika et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Glad Smart Moussounda Mpika et al. Multisystemic sarcoidosis revealed by a Heerfordt syndrome: case report. Pan African Medical Journal. 2022;42:159. [doi: 10.11604/pamj.2022.42.159.34073]
Available online at: https://www.panafrican-med-journal.com//content/article/42/159/full
Multisystemic sarcoidosis revealed by a Heerfordt syndrome: case report
![]() Glad Smart Moussounda Mpika1,&, Paulvon Phérol Koumeka1, Lamyae Amro1
Glad Smart Moussounda Mpika1,&, Paulvon Phérol Koumeka1, Lamyae Amro1
&Corresponding author
Heerfordt syndrome is a rare clinical form of sarcoidosis with a favorable evolutionary profile in the majority of cases. In its classical form, it associates uveitis, parotidomegaly, facial paralysis and fever. We report a case of multisystemic sarcoidosis type II revealed by a Heerfordt syndrome in a 51-year-old female patient.
Sarcoidosis is the most common systemic granulomatosis and diffuses infiltrative disease of unknown etiology. It can affect the whole body with pulmonary and lymphatic tropism [1,2]. In 1909, Heerfordt described a syndromic entity associating uveitis, parotitis and facial paralysis in a febrile context [3,4]. Waldenstrom in 1937 had linked this syndrome to sarcoidosis, a rare manifestation of the disease which is easily diagnosed in its complete form [5]. We report a case of Heerfordt syndrome revealing a multisystem sarcoidosis.
Patient information: a 51-year-old woman, housewife, exposed to wood smoke, followed by a visceral surgery for a lithiasis gallbladder and referred to a pneumology consultation in front of a pathological thoracic imaging preceded by a symptomatology evolving for seven months made of a dry cough, a dyspnea stage II of Sadoul associated with a decrease of the bilateral visual acuity with xerophthalmia, xerostomia as well as bilateral polyartralgias of the big joints (knees and ankles).
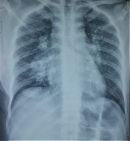
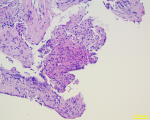
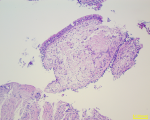
Clinical findings: the clinical examination revealed a preserved general condition with a temperature of 38°C, symmetrical erythematous macules on the lower limbs in connection with erythema nodosum, left facial paralysis and bilateral sequelae of anterior uveitis on ophthalmologic examination. Chest X-ray showed bilateral mediastinopulmonary opacities associated with diffuse micronodular infiltration (Figure 1). The thoracic CT scan showed a magma of bilateral and symmetrical non-compressive medial and para hilar adenopathies, the largest of which measured 60 mm (right para hilar); bilateral para hilar peribronchovascular thickening; nodular thickening of the septal lines, with a pearly appearance of the scissures, more marked at the upper level; bilateral confluent basal sparse micronodules producing the sign of Galaxie (Figure 2). Cervical ultrasonography showed parotitis with swollen, hyper echogenic and heterogeneous glands with thick septa. The radio-clinical picture evoked a Lofgren's syndrome associated with a Heerfordt's syndrome. Further investigations were undertaken as part of a workup for sarcoidosis. Angiotensin-converting enzyme (ACE) was elevated to 104IU/L, phosphocalcic, urinary and serological tests were normal. Inflammation markers were elevated with lymphopenia on the blood count. The flexible bronchoscopy performed found a diffuse 1st degree inflammatory state with no visible buds. A bronchial spur biopsy was performed, which revealed an epithelial-giganto-cellular granuloma without necrosis and no signs of malignancy (Figure 3). The bronchoalveolar lavage showed an inflammatory cytology rich in lymphocytes. Accessory salivary gland biopsy revealed salivary parenchyma without histopathological abnormalities and no evidence of malignancy (Figure 4). The pre-therapeutic work-up revealed normal blood glucose and viral serologies, an electrocardiogram and a transthoracic cardiac echography without abnormalities. Respiratory function tests showed hypoxemia with small airway involvement without carbon monoxide diffusion disorders.
Therapeutic intervention: a corticosteroid therapy 1mg/kg of Prednisolone was instituted with adjuvant measures to the corticosteroid therapy.
Sarcoidosis, also known as Besnier-Boeck-Shaumann disease (BBS), is a rare condition. It represents 5-10% of sarcoidosis and 4.4-5.6% as reported by Fukuhara et al. [6]. Genetically, the HLA-DRB1*04 allele appears to be protective against sarcoidosis and facilitates the occurrence of Heerfordt syndrome [7]. In our study, we reported a case of multi-systemic sarcoidosis in a 51-year-old female patient. This is in agreement with the literature which reveals a female predominance due to a hormonal factor with a second peak of the disease between 45 and 65 years of age corresponding to the peri-menopausal peak incidence [8].
Ocular manifestations are constant depending on the series, they are found in 25-60% of cases and are revealing of the disease in 10-20% of cases [9]. It is mainly anterior uveitis, which is quite characteristic as found in our study. All structures of the eyeball may be involved. It is sometimes revealing of the disease. It should be systematically investigated because of its functional prognosis, which requires rapid corticosteroid therapy to avoid sequelae. The involvement of the accessory salivary glands is present in 65% of the cases with a rare involvement of the main salivary glands sometimes resulting in bilateral parotitis (observed in 1-4% of cases) with xerostomia [4,6], as found in the series of Benjelloun H et al. [10]. In our study, the biopsy of the accessory salivary glands was unremarkable.
Neurological manifestations are rare. In our study, it resulted in facial paralysis which, depending on the series, is present in 25 to 50% of cases [4]. It is secondary to the involvement of the epineurium by sarcoid granulomas and to perineural inflammation [4,6]. The patient was treated with long-term corticosteroid therapy. It represents the first-line treatment of Heerfordt syndrome with a dose of 60 mg/day for 3 months followed by a degression of the corticosteroid therapy at a rate of 5 mg every 3 months [4,11].
Heerfordt syndrome is a rare form of sarcoidosis. The diagnosis is simple in its complete form. The evolution is globally favorable under medical treatment with few functional sequelae. Nevertheless, the delay in diagnosis can jeopardize the functional prognosis, which can be responsible in some cases for blindness.
The authors declare no competing interests.
Glad Smart Moussounda Mpika contributed to the design and development of the study, the acquisition of data, the analysis and interpretation of data, the writing of the article and its critical revision leading to important modifications of the intellectual content and the final approval of the version to be published. Paulvon Phérol Koumeka contributed to the acquisition of data, the analysis and interpretation of the data, the writing of the article and its critical revision leading to important modifications of the intellectual content. Lamyae Amro contributed to the final approval of the version to be published. All the authors have read and agreed to the final manuscript.
Figure 1: bilateral mediastino-pulmonary opacities associated with a diffuse micronodular infiltration
Figure 2: (A, B) chest CT axial section (medial and parenchymal window) bilateral and symmetrical non-compressive medial and para hilar adenopathy masses; bilateral para hilar peribronchovascular thickening; nodular thickening of the septal lines; bilateral confluent basal sparse micronodules with Galaxie sign
Figure 3: epithelial-giganto-cellular granuloma without caseous necrosis with no evidence of malignancy on bronchial spur biopsy
Figure 4: salivary parenchyma without abnormality with no sign of malignancy on biopsy of accessory salivary glands
- Statement on sarcoidosis. Joint Statement of the American Thoracic Society (ATS), the European Respiratory Society (ERS) and the World Association of Sarcoidosis and Other Granulomatous Disorders (WASOG) adopted by the ATS Board of Directors and by the ERS Executive Committee, February 1999. Am J Respir Crit Care Med. 1999 Aug;160(2):736-55. PubMed | Google Scholar
- Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007 Nov 22;357(21):2153-65. PubMed
- Heerfordt C. [About a “Febris uveoparotidea subchronica” located on the parotid gland and the uvea of the eye and often complicated with paresis cerebrospinal nerves]. Arch Ophthalmol. 1909;70:254-273 (in German).
- Kharoubi S. Syndrome de Heerfordt: à propos d´une observation et revue de la littérature. Pan Afr Med J. 2020;37:117. PubMed | Google Scholar
- Waldenstrom JG. Some observations of uveoparotitis and allied conditions with special reference to the symptoms from the nervous system. Acta Med Scand. 1937;91(1-2):53-68. Google Scholar
- Fukuhara K, Fukuhara A, Tsugawa J, Oma S, Tsuboi Y. Radiculopathy in patients with Heerfordt´s syndrome: two case presentations and review of the literature. Brain Nerve. 2013 Aug;65(8):989-92. PubMed | Google Scholar
- Darlington P, Tallstedt L, Padyukov L, Kockum I, Cederlund K, Eklund A et al. HLA-DRB1* alleles and symptoms associated with Heerfordt´s syndrome in sarcoidosis. EurRespir J. 2011;38(5):1151-1157. PubMed | Google Scholar
- Cadelis G, Cordel N, Coquart N, Etienne N, Macal M. Incidence de la sarcoidose en Guadeloup: étude rétrospective sur 13ans (1997-2009). Revue des Maladies Respiratoires. January 2012;29(1):13-20. Google Scholar
- Evans M, Sharma O, LaBree L, Smith RE, Rao NA. Differences in clinical findings between Caucasians and African Americans with biopsy-proven sarcoidosis. Ophthalmology. 2007 Feb;114(2):325-33. PubMed | Google Scholar
- Benjelloun H, El Hachimi K, Zagbba N, Bakhatar A, Yassine N, Bahlaoui A. Atteinte ORL au cours de la sarcoïdose thoracique. Revue des Maladies Respiratoires. Janvier 2014;31(Supp 1):A90.
- Nunes H, Uzunhan Y, Freynet O, Naccache JM, Bouvry D, Brillet PY et al. Sarcoïdose médiastinopulmonaire. Presse Med. 2010 Jan;39(1):93-106. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
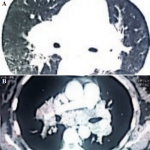 Figure 2: (A, B) chest CT axial section (medial and parenchymal window) bilateral and symmetrical non-compressive medial and para hilar adenopathy masses; bilateral para hilar peribronchovascular thickening; nodular thickening of the septal lines; bilateral confluent basal sparse micronodules with Galaxie sign
Figure 2: (A, B) chest CT axial section (medial and parenchymal window) bilateral and symmetrical non-compressive medial and para hilar adenopathy masses; bilateral para hilar peribronchovascular thickening; nodular thickening of the septal lines; bilateral confluent basal sparse micronodules with Galaxie sign