A case for implementation of adult pneumococcal vaccine program in Africa: review and expert opinion
Reena Shah, Catherine Gathu, Eric Njenga, Jeremiah Chakaya, Elijah Ogola, Omondi Oyoo, Andrew Odhiambo, Benjamin Wambugu, Charles Feldman
Corresponding author: Reena Shah, Aga Khan University Hospital, Nairobi, Kenya 
Received: 02 Oct 2021 - Accepted: 12 Dec 2021 - Published: 19 Jan 2022
Domain: Vaccine logistic,Infectious disease,Immunization
Keywords: Pneumococcal, vaccine, opinion
©Reena Shah et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Reena Shah et al. A case for implementation of adult pneumococcal vaccine program in Africa: review and expert opinion. Pan African Medical Journal. 2022;41:51. [doi: 10.11604/pamj.2022.41.51.31849]
Available online at: https://www.panafrican-med-journal.com//content/article/41/51/full
Opinion 
A case for implementation of adult pneumococcal vaccine program in Africa: review and expert opinion
A case for implementation of adult pneumococcal vaccine program in Africa: review and expert opinion
![]() Reena Shah1,&,
Reena Shah1,&, ![]() Catherine Gathu1, Eric Njenga1,
Catherine Gathu1, Eric Njenga1, ![]() Jeremiah Chakaya2, Elijah Ogola3, Omondi Oyoo3, Andrew Odhiambo3, Benjamin Wambugu4, Charles Feldman5
Jeremiah Chakaya2, Elijah Ogola3, Omondi Oyoo3, Andrew Odhiambo3, Benjamin Wambugu4, Charles Feldman5
&Corresponding author
Vaccines are considered as a therapeutic area for children; the scientific community focuses mainly on managing chronic disease when it comes to adults. There currently is an increase in the burden of vaccine preventable illnesses in adults. Adult vaccination has been shown to dramatically increase the health and quality of life of older populations. Therefore, adult vaccinations need to be approached as a public health issue, similar to smoking cessation programs, for example. According to the Kenya Non-Communicable Diseases and injuries poverty commission report, 2018. Kenya has a high percentage of disability adjusted life years (DALYs) from communicable diseases at 63%, while non-communicable diseases (NCDs) contribute 30% of the DALYs. Specific to pneumococcal pneumonia (PP) in adults, the Global burden of disease (GBD) study in 2016 found that 2,377,697 people of all ages died from lower respiratory tract infections (LRTI) in 2016. Of these, more people died from Streptococcus pneumonia (SP) than from all other studied respiratory pathogens combined. While the incidence of LRTIs in children under five years old was reducing, partly as a result of well-established vaccination programs in children, the incidence, morbidity and mortality of PP was increasing in older populations. The expert recommendations included the following; i) all individuals 65 years of age and above, and individuals with a predisposing comorbidity regardless of age, should receive the pneumococcal vaccine; ii) several systemic modules can be emulated from the successful childhood vaccines programs onto an adult vaccine program; iii) formulation of an effective vaccine program will require collaboration from the public, the government, healthcare providers, and the media, to create awareness; iv) stakeholders who need to be involved in vaccine policy development and implementation include medical professional associations, nurses, pharmacists, clinical officers, payers (private and public insurances), government, medical learning institutions and faith-based medical organizations.
Burden of pneumococcal pneumonia in Kenya: Kenya has a high percentage of disability adjusted life years (DALYs) from communicable diseases at 63%, while non-communicable diseases (NCDs) contribute 30% of the DALYs [1]. The Global Burden of Disease (GBD) study in 2016 found that 2,377,697 people of all ages died from LRTI in 2016. Of these, more people died from SP than by all other studied respiratory pathogens combined [2]. While the incidence in children under five years of age was reducing, the incidence, morbidity and mortality was increasing in older populations. In the United State alone, among adults, invasive pneumococcal disease carries a mortality of approximately 20-30% against an annual incidence of approximately 8700 cases, while non-bacteraemic pneumococcal pneumonia, which is the major burden in the adult population, carries a mortality of approximately 5-7% against an annual incidence of approximately 500,000 cases [2]. Pneumococcal community-acquired pneumonia (CAP) is by far more common in sub-Saharan Africa than in Europe or North America [3]. Lower respiratory infections are still the leading cause of death in low-income countries. A study in Kibra in Nairobi, Kenya and Western Kenya showed that there is a 90% carriage rate of Streptococcus pneumoniae in these populations based on culture from nasopharyngeal swabs [4].
A rise in the aging population in Kenya is increasing the need for pneumococcal adult vaccination in Kenya. Following an episode of pneumococcal pneumonia, the mortality is increased for up to 10 years, compared to the expected 10 year survival of an average 63-year-old American male [5]. The most common risk factors for acquiring CAP and invasive pneumococcal disease (IPD) included age 6 years, Diabetes mellitus, alcohol misuse disorders, chronic obstructive pulmonary disease (COPD), asthma, smoking, cancer, cerebrovascular disease, chronic kidney disease and HIV [6]. These comorbidities and risk factors are on the rise in the Kenyan adult population. Having two or more comorbid conditions drastically increases the incidence of pneumococcal CAP. In addition, in one study, there was a reciprocal relationship between pneumococcal CAP and comorbid conditions, with patients reporting worsening of their comorbid conditions following an episode of pneumococcal CAP [7]. The morbidity and mortality rate of CAP in adults is possibly greatly underestimated in the Kenyan context due to insufficient research and data
Impact of adult pneumococcal vaccination: the community-acquired pneumonia immunization trial in adults (CAPiTA) study was a phase 4, randomized, placebo-controlled clinical trial of the 13-valent pneumococcal conjugate vaccine efficacy in prevention of vaccine-serotype pneumococcal community-acquired pneumonia and invasive pneumococcal disease, which yielded the following results: 46% efficacy in prevention of vaccine-type (VT) CAP, and 75% efficacy in prevention of VT IPD [8]. Post hoc analysis of CAPiTA showed significant and persistent efficacy of PCV13 against VT-CAP in at-risk older adults [9]. Furthermore, COPD exacerbations were reduced, as was risk of hospital admission among COPD patients in vaccinated cases [9]. There is high vaccine coverage of children of nearly 100% by pneumococcal vaccines as a result of initiatives from the Ministry of Health, Kenya (MOH), which has reduced the incidence of CAP in children, as evidenced by a demographic health Survey in Kilifi, 2011 whereby IPD sharply declined both in vaccinated and unvaccinated children following introduction of PCV 10 [10].
Challenges in attaining adequate adult vaccination coverage for pneumococcal pneumonia in Kenya: vaccination advice for adults is hereditary coproporphyria (HCP) initiated. The majority of the HCPs are under-informed or uninformed of the existence and indications of PP vaccines for adults. The existing policies and protocols from the Ministry of Health are non-specific, not recently updated, and not widely disseminated to the HCPs. There are no local studies illustrating the burden of non-vaccination in adults or the benefits of vaccination. Members of the public are not aware of the huge impact of adult pneumococcal vaccinations, with the belief that vaccines “only exist” for children. In addition, the “anti-vaxxer” movements have gained momentum in causing pensiveness towards vaccines, making uptake of vaccines in general challenging. Adult pneumococcal vaccines are costly, making them inaccessible to a great majority of the population. There are no programs in Kenya that provide finance or reimbursements for adult vaccines (i.e. NHIF/private insurances/government or nongovernmental reimbursement schemes). The vaccines are not freely available in the government-run health facilities, which is where the majority of patients are treated. There is insufficient infrastructure in the country to reliably maintain the cold chain required of vaccines. Poor inventory management leads to regular stock-outs of vaccines in the country. There is no national registry for adult vaccinations in Kenya at the moment.
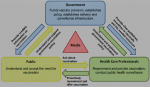
Recommendations/framework for developing and implementing pneumococcal adult vaccine program in Kenya: all key stakeholders must be involved in the process of developing and implementing the pneumococcal vaccine program in Kenya as illustrated in Figure 1 [11]. Other stakeholders not captured in the Figure 1 are: bodies involved in accessibility of the vaccines (NHIF and private insurers), religious organizations which run several major health facilities christian health association of Kenya (CHAK) and council of catholic bishops and medical learning institutions. Under HCPs, professional associations are to be involved; notably the nursing Council, the clinical officers´ council, pharmacy and poisons board, paediatrician associations, infectious disease experts, family medicine associations, physician associations, pulmonology associations, rheumatology associations, oncology associations and other specialist organizations with specialists that cater to the at-risk populations. With regard to government, both local county and national government representatives should be involved. National government is to be represented by the Ministry of Health, with inclusion of the non-communicable disease department in the Ministry of Health. Local government is to be represented by the association of County Executive Committee Members for Health. The public is to be involved directly, via media campaigns and through patient groups.
Development of the vaccines program could borrow from the already established and successful paediatric vaccination program. Local data should be collected via surveys, research and interventional studies to determine the burden of PP in Kenya, the burden of non-vaccination of PP and the benefit of adult vaccination in Kenya. This data should be shared with the intended financiers and reimbursement bodies to illustrate the need for adult PP vaccination programs in the country. With involvement of the MOH and the named stakeholders, the existing guidelines on pneumococcal vaccination need to be updated, approved and disseminated to all relevant HCPs and the public. HCPs, directly and through the respective associations, need to be trained on the significance and administration of the PP vaccine. Training should be conducted directly to all the aforementioned HCP cadres via seminars, conferences, advisory boards and dissemination of education material on the subject matter. There should be an establishment of an electronic medical register by the ministry of health recording pneumococcal adult vaccinations in Kenya.
All the authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Medical triting support was provided by Dr Martin Makau at the Manor Health Services, Nairobi, Kenya, funded by Pfizer laboratories Ltd, Vienna Court, State House crescent road, Nairobi, Kenya
Figure 1: stakeholder involvement in adult vaccine program implementation
- Ministry of Health. The Kenya non-communicable diseases & injuries poverty commission report, July 2018. May 13th, 2021.
- Christopher T, Mohammad F, Puja RC, Ibrahim K, Alexandria B, Scott S et al. Estimates of the global, regional, and national mortality, and aetiologies of lower respiratory tract infections in 195 countries, 1990-2016: a systematic analysis for the Global burden of disease study 2016. Lancet Infect Dis. 2018 Nov;18(11):1191-1210. PubMed | Google Scholar
- Susan SH, Kristen MJ, Thomas RG, Peter W, Tracy AL, Matthew RM et al. Healthcare utilization and cost of pneumococcal disease in the United States. Vaccine. 2011 Apr 18;29(18):3398-412. PubMed | Google Scholar
- Miwako K, Laura MC, Godfrey B, Geofrey J, Lee H, Fleming-Dutra KE et al. Pneumococcal carriage and antibiotic susceptibility patterns from two cross-sectional colonization surveys among children aged <5 years prior to the introduction of 10-valent pneumococcal conjugate vaccine - Kenya, 2009-2010. BMC Infect Dis . 2017 Jan 5;17(1):25. PubMed| Google Scholar
- Barcleigh S, Adriana MR, Musher DM. Long-term survival following pneumococcal pneumonia. Clin Infect Dis. 2013 Apr;56(8):1145-6. PubMed | Google Scholar
- Moe HK, Charles ER, Alicia MF, James AS, Zack M, Elizabeth RZ et al. The influence of chronic illness on the incidence of invasive pneumococcal disease in adults. J Infect Dis. 2005 Aug 1;192(3):377-86. PubMed | Google Scholar
- Kathleen WW, Holly Y, Reiko S, David S, John HP. Community-acquired pneumonia: symptoms and burden of illness at diagnosis among us adults aged 50 years and older. Patient. 2013;6(2):125-34. PubMed | Google Scholar
- Marc JMB, Susanne MH, Marieke B, Chris W, Scott P, Samantha G et al. Polysaccharide conjugate vaccine against pneumococcal pneumonia in adults. N Engl J Med. 2015 Mar 19;372(12):1114-25. PubMed | Google Scholar
- José AS, Qin J, Daniel AS, William CG, Chris W, Schmoele-Thoma B et al. Post hoc analysis of the efficacy of the 13-valent pneumococcal conjugate vaccine against vaccine-type community-acquired pneumonia in at-risk older adults. Vaccine. 2018 Mar 7;36(11):1477-1483. PubMed | Google Scholar
- Micah S, Michael O, Christian B, Joyce S, Rachel B, Kate Park et al. Effect of 10-valent pneumococcal conjugate vaccine on the incidence of radiologically-confirmed pneumonia and clinically-defined pneumonia in Kenyan children: an interrupted time-series analysis. Lancet Glob Health. 2019 Mar;7(3):e337-e346. PubMed | Google Scholar
- Mark DT, Mark PC, Giuseppe DG, Johan F, Jorg JG, Grubeck-Loebenstein B et al. Vaccination programs for older adults in an era of demographic change. Eur Geriatr Med. 2018;9(3):289-300. PubMed | Google Scholar