A retrospective study of 43 cases of fungal malignant external otitis
Chiraz Halwani, Latifa Mtibaa, Moez El Hamdi, Nawel Baccouchi, Rania Benmhamed, Boutheina Jemli, Khemaies Akkari
Corresponding author: Latifa Mtibaa, Laboratory of Parasitology-Mycology, Military Hospital of Tunis, 1008 Monfleury, Tunis, Tunisia 
Received: 29 Apr 2021 - Accepted: 06 Dec 2021 - Published: 08 Apr 2022
Domain: Parasitology,Infectious diseases epidemiology,Infectious disease
Keywords: Malignant, fungal otitis, candida, aspergillus, geotrichum
©Chiraz Halwani et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Chiraz Halwani et al. A retrospective study of 43 cases of fungal malignant external otitis. Pan African Medical Journal. 2022;41:287. [doi: 10.11604/pamj.2022.41.287.29585]
Available online at: https://www.panafrican-med-journal.com//content/article/41/287/full
A retrospective study of 43 cases of fungal malignant external otitis
![]() Chiraz Halwani 1,2,
Chiraz Halwani 1,2,![]() Latifa Mtibaa 2,3,&, Moez El Hamdi1,2,
Latifa Mtibaa 2,3,&, Moez El Hamdi1,2, ![]() Nawel Baccouchi3, Rania Benmhamed1,2, Boutheina Jemli 2 , Khemaies Akkari1,2
Nawel Baccouchi3, Rania Benmhamed1,2, Boutheina Jemli 2 , Khemaies Akkari1,2
&Corresponding author
Malignant external otitis (MEO) has a frequent bacterial origin, but we are currently witnessing the emergence of fungal agents, which poses difficulties in diagnosis and management. The aim of our work is to analyze the epidemiological and clinical profile of fungal MEO and to study the antifungal susceptibility of fungi involved.Our study is retrospective collecting 43 patients treated for fungal MEO between 2010 and 2019.Clinical, biological, and radiological data were collected from patient hospitalization records. Identification of yeasts was done by YST vitek®2 card.The antifungal susceptibility testing was performed for yeasts by the AST vitek® 2 card and for other fungi by the E-test technique. The average age was 66 (± 12) years. We noted a male predominance in 63 % (n=27). Diabetes was found in 86%. Otalgia was a constant symptom. Cranial nerve palsies were observed in 16% (n=7) of cases. CT showed bone lysis in 74% (n=31>) of cases and Tc99 bone scintigraphy revealed hyperfixation in 100%(n=43) of cases. Candida spp (n=21), Aspergillus spp (n=18), and Geotrichum capitatum (n=2) were isolated. No resistance to antifungals has been demonstrated for Candidayeasts. Geotrichumcapitatum isolates were resistant to fluconazole and caspofungin. Aspergillus isolates were resistant to amphotericin B and caspofungin in 50% (n=9) and 72% (n=12) of cases, respectively. Our study proves the predominance of Candida yeasts and Aspergillus as the fungal agents involved in MOE. Mycological diagnosis allows the identification and antifungal susceptibility testing. Thus, it allows usingof the appropriate antifungal treatment and improves the prognosis of the disease.
Malignant external otitis (MEO) corresponds to osteomyelitis of the skull base starting in the external auditory canal [1]. Itis a serious and rare infectious emergency with an overall mortality of around 20% [1]. Its severity is due to the risk of the extension of the infection to the central nervous system or to the deep spaces of the face and its occurrence mostly in elderly diabetic, immunocompromised subjects. It has frequently bacterial origin, but we are currently witnessing the emergence of fungal agents, which poses difficulties in diagnosis and management. Candida yeasts and Aspergillus are the fungal pathogens mainly incriminated [2,3]. The majority of studies found in the literature are case reports or small series. The aim of our workis to analyze the epidemiological and clinical profile of this infection and to study the antifungal susceptibility of fungi involved.
Study design and setting: our study is retrospective collecting 43 patients treated for MEO at the Tunis Military Hospital over a period of 10 years (January 2010 to December 2019).
Study population: this study included all patients who had been treated in the ENT department for MEO, in whom the fungus was identified on a mycological sample and/or on a positive Aspergillus antigenemia. Patients with unusable medical records were excluded from the study, in particular when the course under treatment was not well detailed or was lost to follow-up. The ear sample was taken by swabbing the external auditory canal under otoscopic examination. The identification of the yeasts was carried out using the YST vitek®2 card (Biomérieux). The identification of Aspergillus relied on their macroscopic and microscopic characters. The antifungal susceptibility testing was performed for yeasts by the AST vitek®2 (Biomérieux) card and for Aspergillus and Geotrichumcapitatum, by the E-test technique with reference to the EUCAST recommendations. Aspergillus serology and antigenemia were performed using the PLATELIA™AspergillusIg G (Biorad) and PLATELIA™Aspergillus Ag (Biorad) respectively.
Data collection: clinical, biological and radiological data were collected from patient hospitalization records and laboratory records.
Statistical analysis: data were entered using Excel software and analyzed using SPSS version 20 software. We calculated simple frequencies and relative frequencies (percentages) for the categorical variables. We calculated averages; medians and standard deviations and determined the extreme values (minimum and maximum) for the quantitative variables.
Ethical consideration: the global rules of ethics relating to respect for confidentiality and the protection of patient-specific data were taken into account during this work. We obtained the informed consent from patients and the authorization of the Ethical Committee of the Military Hospital of Tunis.
Sociodemographic characteristics: the diagnosis of MEO was confirmed in 43 patients, including 41 cases with mycological confirmation and 2 cases through positive antigenemia. The average age of our patients was 66 (± 12) years with extremes from 37 to 89 years. The proportion of males was 63 % (n=27). Diabetes was found in 86%(n=37).
Clinical features: Otalgia was the main reason for consultation (100%, n=43) followed by otorrhea (81%, n=35).Cranial palsies were observed in 16%(n=7) of cases. Computed tomography of the rocks was performed in all patients and showed bone lysis in 74%(n=31) of cases (Table 1). Technetium-99 bone scintigraphywas performed for 37 patients (86%, n=37) and showed bone hyperfixation in all cases. Table 1 summarizes Clinical, biological and radiological data of patients.
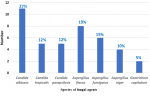
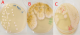
Mycologic features: the isolated fungi were: yeasts genus Candida (n=21), Aspergillus (n=18) and Geotrichum capitatum(n=2). Candida albicans was the most implicated strain in 11 patients (27%, n=11) followed by Aspergillus flavus in 8 patients (19%, n=8) and Aspergillus fumigatus in 6 patients (15%, n=6) (Figure 1). The three genera of isolated fungi are photographed and illustrated in Figure 2. Serology and antigenemiawere performed in 18 cases. Serology was positive in 10 patients (55%, n=10). Aspergillus antigenemia was positive in only 2 patients (11%, n=2) having negative mycological cultures. No resistance to antifungals was demonstrated for yeasts of the Candidagenus. All Candida yeasts were sensitive to Fluconazole and Voriconazole. C. parapsilosis isolates (n=5) were intermediate to Micafungin in 80% of cases (n=4). The results of the susceptibility of Candida yeasts to antifungals are shown in Table 2.
For the genera Aspergillus and Geotrichum, Antifungal susceptibility was interpreted referring to EUCAST recommandations. The MICs found for all isolates are shown in Table 3. The two isolates of Geotrichum capitatum had low MICs for amphotericin B and voriconazole (<1µg/ml) and were resistant to fluconazole and caspofungin. Aspergillus isolates were all susceptible to voriconazole. Resistance to amphotericin B and caspofungin was reported in 50% (n=9)and 72% (n=13) of cases, respectively. Antifungal treatment consisted of fluconazole (49%, n=21) and voriconazole (51%, n=22) in case of MEO due to Candida yeasts and to Geotrichum/Aspergillus respectively. The duration of antifungal treatment varied between 3 and 7 months, with an average of 90 days. Other therapies were used such as surgery and hyperbaric oxygen therapy performed in 5 cases (12%) and 12 cases (28%) respectively.The evolution of our patients under treatment was favorable in 39 cases (91%, n=39) with a total cure of the disease without recurrencewith an average follow-up of 2 years.
In our study, fungal MEO diagnosis was confirmed in 41 cases with mycological examination and in 2 cases with positive Aspergillus antigenemia. Candida spp (n=21), Aspergillus spp (n=18), and Geotrichum capitatum (n=2) were isolated. All Candida yeasts were sensitive to fluconazole and voriconazole. Both isolates of Geotrichum capitatum had low MICs for amphotericin B and voriconazole. The Aspergillus isolates were all sensitive to voriconazole. Fungal MEO is a potentially serious and fatal disease that typically affects older people. The infection is favored by an imbalance of local and general defense mechanisms, in addition to virulence factors of fungal agents [1,4]. Diabetes mellitus is usually reported in 75 to 100%of patients with fungal MEO [5,6]. In our study, the patients were diabetic in 86% (n=37) of cases. Other immunosuppressive factors such as chronic renal failure, anti-cancer chemotherapy, hematologic malignancies and acquired immune deficiency syndrome (AIDS) have been reported [7,8]. Otalgia is the most reported symptom with nocturnal exacerbation as described in our study for all patients. Otorrhea is the second frequent symptom in 81% (n=35). Other functional signs can be seen such as trismus, dizziness, tinnitus and fever [6,9]. The fungus makes the infection more invasive which explains the higher number of cranial nerve palsies in patients with Fungal MEO[3,6].This complicationwas observed in 16%of our patients (n=7).
The most fungus incriminated in MEO is genus Aspergillus with predominance of A. fumigatus followed by A. Flavus [10,11]. In our study Aspergillus MEO was diagnosed in 20 cases including 18 cases of positive cultures and 2 cases with positive Aspergillusantigenemia. In addition, our series shows the predominance of A. flavusspecies. Aspergillus secrete several proteolytic enzymes that facilitate tissue invasion [10,11]. Furthermore, Susceptibility testing is helpful in defining the activity spectrum of antifungals and determining the appropriate drug for treatment. All strains of Aspergillus isolated were sensitive to voriconazole. Resistance to amphotericin B and caspofunginwas reported in 50% (n=9)and 72% (n=13)of our isolates, respectively. The second fungal agent frequently responsible for MEO is Candida yeasts. However, in our series, they represent the most frequent isolate in 49% of cases (n=21).These yeastsproduce a biofilm forming a barrier to the host's defence mechanisms and to the passage of antifungals [12]. Mycological examination allows identification of yeasts and antifungal susceptibility testing. In our study, no resistance to antifungals was demonstrated for the Candida yeasts. C. parapsilosis isolates were intermediate to Micafungin in 80% of cases (n=4).In fact, elevated MICs were founded of echinocandin for C. parapsilosis.
In two of our patients, Geotrichum capitatum (Saprochaete capitata) was isolated. We didn´t found in literature any cases of MEO caused by this fungus. Itis rarely responsible for deep invasive infections in patients with hematological malignancies and transplant subjects [13]. Regarding antifungal susceptibility, the two isolates had a low MICs for amphotericin B and voriconazole (<1µg / ml) and were resistant to fluconazole and caspofungin. In fact, data on its antifungal susceptibilities are limited; however amphotericin B and voriconazole appeared to be the more active drugs. Yenizehirli et al. proved in a series of 96 fungal isolates taken from 92 patients suspected of otomycosis, the efficacy of voriconazole [14]. In fact, the mean MICs of voriconazole for A. fumigatus, A. niger, A. flavus and C. albicans were significantly lower than those of itraconazole for the same pathogens [14]. Candida yeasts are frequently sensitive to all triazole derivatives. For MEO due to Candida, fluconazole may be prescribed as the first line [14]. Voriconazole is also effective with even greater efficacy than fluconazole [15-17]. The antifungal treatment must be prolonged with a total duration of three to six months [15,17]. In our series, 49% (n=21) of our patients were treated with fluconazole and 51% (n=22)with voriconazole in case of MEO due to Candida yeasts and to Geotrichum / Aspergillus respectively. Other therapies were used such as surgery and hyperbaric oxygen therapy performed in 5 cases (12%) and 12 cases (28%) respectively. Hyperbaric oxygen therapy promotes healing, angiogenesis, and phagocytosis, by increasing the partial pressure of oxygen [18]. Good outcome was noted in 91% (n=39) of our patients with an average follow-up of 2 years. Fungal MEO is an opportunistic infection increasingly described in the literature but the majority of authors report case studies or series of around ten cases. The strength of our work is the large number of cases collected (n=43), appearing among the largest studies in the literature, which offers reliability to our epidemiological data. However, it should be noted that this study has certain limitations, such as the absence of a standard inter-department protocol which codifies the treatment of this disease which allows reliable comparative statistical studies. Prospective studies are to be carried out in the future in order to resolve the problems of management of this invasive infection.
Our study proves the predominance of Candida yeasts and Aspergillus as the fungal agents involved in MEO and reports the first cases due to Geotrichum capitatum. Mycological diagnosis allows the identification and antifungal susceptibility testing. Thus, it allows to use the appropriate antifungal treatment and to improve the prognosis of the disease. The antifungal susceptibility testing performed of all our isolates proves the effectiveness of Voriconazole with low MICs. Management of this fungal invasive infection often requires prolonged antifungal treatment and in some cases the need for surgical procedures or hyperbaric oxygen therapy following surgery.
What is known about this topic
- Malignant external otitis is a serious and rare infectious emergency with a high mortality and morbidity rate;
- It has frequently bacterial origin, but we are currently witnessing the emergence of fungal agents which poses difficulties in diagnosis and management;
- Candida yeasts and Aspergillus are the fungal pathogens mainly incriminated.
What this study adds
- Our study allowed the analyse of clinical profile of this fungal infection in Tunisian population;
- We report here the first cases of malignant external otitis due to Geotrichum capitatum;
- Antifungal susceptibility testing of fungi involved in this infection was performed and proves the effectiveness of Voriconazole for all isolates.
The authors declare no competing interests.
Conception and study design: Latifa Mtibaa and Chiraz Halwani. Data collection: Chiraz Halwani, Latifa Mtibaa and Moez El Hamdi. Data analysis and interpretation: Latifa Mtibaa and Chiraz Halwani. Manuscript drafting: Chiraz Halwani, Latifa Mtibaa, Moez El Hamdi and Nawel Baccouchi. Manuscript revision: Latifa Mtibaa, Nawel Baccouchi and Rania Benmhamed. All authors approved final version of the manuscript. Guarantor of the study: Khémaies Akkari and Boutheina Jemli.
Table 1: clinical, biological and radiological characteristics of patients with fungal malignant external otitis
Table 2: antifungal sensitivity of Candida yeasts
Table 3: in vitro sensitivity of Geotrichum capitatum and Aspergillus by the E-test technique
Figure 1: species of fungal agents isolated in culture
Figure 2: macroscopic aspect of cultures on sabouraud medium, A) candida ablicans; B) aspergillus flavus; C) geotritchum capitatum
- Marina S, Goutham MK, Rajeshwary A, Vadisha B, Devika T. A retrospective review of 14 cases of malignant otitis externa. J Otol. 2019;14(2):63-66. PubMed | Google Scholar
- Bechraoui R, Dhaha M, Chahed H, Ksentini A, Zainine R, Amor MB et al. Epi-demiology and predictive factors of fungal malignant otitis externa. Indian J Otol. 2019;25:1. Google Scholar
- Mion M, Bovo R, Marchese-ragonaR, Martini A. Outcome predictors of treatment effectiveness for fungal malignant external otitis: a systematic review. ActaOtorhinolaryngol Ital. 2015;35(5):307-13. PubMed | Google Scholar
- Rubin Grandis J, Branstetter BF, Yu VL. The changing face of malignant (necrotising) external otitis: clinical, radiological, and anatomic correlations. Lancet Infect Dis. 2004;4(1):34-9. PubMed | Google Scholar
- Schultz P, Riehm S, Carpentier A-S, Boivin G, Schlienger J-L. Otite externe nécrosante (otite maligne externe) et diabète. Encycl Med Chir (Elsevier Masson, Paris), médecine des maladies métaboliques.2011; 1(5):53-4.
- Hariga I, Mardassi A, Belhaj Younes F, Ben Amor M, Zribi S, BenGamra O et al. Necrotizing otitis externa: 19 cases report. Eur Arch Oto-Rhino-Laryngol Off. 2010; 267(8):1193-8. PubMed | Google Scholar
- Hamzany Y, Soudry E, Preis M, Hadar T, Hilly O, Bishara J et al. Fungal malignant external otitis. J Infect. 2011;62(3):226-31. PubMed | Google Scholar
- Liu X-L, Peng H, Mo T-T, Liang Y. Malignant otitis externa in a healthy non-diabetic patient. Eur Arch Oto-Rhino-LaryngolOff J. 2016; 273(8):2261-5. PubMed | Google Scholar
- Mediouni A, Chahed H, Yassine Y, Mellouli Y, Bechraoui R, Beltaief N et al. Les otitis externs nécrosantes d´origine fongique: à propos de 11 cas. Ann Froto-Rhino-Laryngol Pathol Cervico-Faciale. 2013;130:A141.
- Gangneux JP, Bouchara JP. Aspergillose et résistance aux antifongiques. Encycl Med Chir (Elsevier Masson, Paris), Biologie médicale. 2016; 90-35-0055-A: 8.
- Caillot D, Chretien ML, Legouge C, Roques M, Newinger M, Favennec C et al. Aspergillose invasive. Encycl Med Chir (Elsevier Masson, Paris), Maladies infectieuses.2014; 8-600-A-20:6.
- Develoux M, Bretagne S. Candidoses et autres levuroses. Encycl Med Chir (Elsevier Masson, Paris) Maladies infectieuses.2014; 8-602-A-10: 13.
- Bonhomme J. Infections dues à Trichosporon spp et à Geotrichum spp. Encycl Med Chir (Elsevier Masson, Paris) Maladies infectieuses.2015; 8-601-A-10: 6.
- Yenişehirli G, Bulut Y, Güven M, Günday E. In vitro activities of fluconazole, itraconazole and voriconazole against otomycotic fungal pathogens. J LaryngolOtol. 2009; 123(9):978-81. PubMed | Google Scholar
- Marchionni E, Parize P, Lefèvre A, Vironneau P, Bougnoux ME, Poiree S et al. Aspergillus spp invasive external otitis: favorable outcome with a medical approach. ClinMicrobiol Infect. 2016; 22(5):434-37. PubMed | Google Scholar
- Parize P, Chandesris M-O, Lanternier F, Poirée S, Viard J-P, Bienvenu B et al. Antifungal therapy of Aspergillus invasive otitis externa: efficacy of voriconazole and review. Antimicrob Agents Chemother. 2009; 53(3):1048-53. PubMed | Google Scholar
- Hasibi M, Ashtiani MK, Motassadi Zarandi M, Yazdani N, Borghei P, Kuhi A et al. A treatment protocol for management of bacterial and fungal malignant external otitis: a large cohort in Tehran, Iran. Ann OtolRhinol Laryngol. 2017; 126(7):561-7. PubMed | Google Scholar
- Mathieu D, Marroni A, Kot J. Tenth European Consensus Conference on Hyperbaric Medicine: recommendations for accepted and non-accepted clinical indications and practice of hyperbaric oxygen treatment. Diving and Hyperbaric Medicine. 2017 March;47(1):24-32. PubMed | Google Scholar