Multiple meningiomatosis
Inas El Kacemi, Gazzaz Miloudi
Corresponding author: Inas El Kacemi, Service de Neurochirurgie, Hôpital Militaire d'Instruction Mohammed V Rabat, Rabat, Maroc 
Received: 31 May 2021 - Accepted: 22 Aug 2021 - Published: 24 Sep 2021
Domain: Neurosurgery
Keywords: multiple meningiomas, meningiomatosis, MR imaging
©Inas El Kacemi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Inas El Kacemi et al. Multiple meningiomatosis. Pan African Medical Journal. 2021;40:59. [doi: 10.11604/pamj.2021.40.59.30098]
Available online at: https://www.panafrican-med-journal.com//content/article/40/59/full
Multiple meningiomatosis
Inas El Kacemi1,&, Gazzaz Miloudi2
&Corresponding author
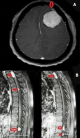
Multiple meningiomas or meningiomatosis are defined by the presence of at least 2 lesions that appear simultaneously or not, at different intracranial locations. Early classification of Cushing and Eisenhardt claimed that a diagnosis of multiple meningioma can only be made if the patient does not suffer neurofibromatosis type I (NF1 is associated with neurofibromin, ras pathway). Majority of multiple meningiomas associate with neurofibromatosis type-II, multiple meningiomatosis refers to the association of at least 2 tumors in two different sites, in a patient who has no evidence of neurofibromatosis. The incidence of this condition varies between series between 1 and 3%, reaching a frequency of 8% with the onset of magnetic resonance imaging (MRI). This entity combines benign tumors of a different histological nature in 30% of cases. A 39-year-old woman patient, with no significant pathological history, who consulted for heaviness in both lower limbs having progressed for 6 months with paresthesias without genitosphincteric disorders, the examination found a spastic paraparesis rated at 3/5. The patient underwent a medullary MRI which revealed 4 lesions, the radiological semiology of which was suggestive of spinal meningiomas, the most compressive projecting in relation to T2. A cerebral computed tomography (CT) was systematically performed and objectified two intra cranial meningiomas, which until then were asymptomatic. Although its incidence is only 1 to 3%, the discovery of multiple meningiomatosis justifies morphological exploration (MRI) of the entire neurax, in which case any symptomatic location should suggest surgical management.
Figure 1: (A,B) brain MRI with contrast axial section showing frontal convexity meningioma, spine MRI on sagittal sections on T1 injection showing 4 lesions, the most compressive meningiomas are projected in T2 whose major axis is 28 mm