The impact of COVID-19 lockdown on acute trauma patients seen at the National Hospital Trauma Centre Abuja, Nigeria
Onyedika Godfrey Okoye, Oluwole Olayemi Olaomi, Usman Adamu Gwaram, Kanati Dennis Apollo
Corresponding author: Onyedika Godfrey Okoye, Trauma Centre, National Hospital Abuja, Abuja, Nigeria 
Received: 17 Feb 2021 - Accepted: 19 Apr 2021 - Published: 30 Apr 2021
Domain: Emergency medicine,General surgery
Keywords: COVID-19, lockdown, acute, trauma
©Onyedika Godfrey Okoye et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Onyedika Godfrey Okoye et al. The impact of COVID-19 lockdown on acute trauma patients seen at the National Hospital Trauma Centre Abuja, Nigeria. Pan African Medical Journal. 2021;38:414. [doi: 10.11604/pamj.2021.38.414.28431]
Available online at: https://www.panafrican-med-journal.com//content/article/38/414/full
Research 
The impact of COVID-19 lockdown on acute trauma patients seen at the National Hospital Trauma Centre Abuja, Nigeria
The impact of COVID-19 lockdown on acute trauma patients seen at the National Hospital Trauma Centre Abuja, Nigeria
![]() Onyedika Godfrey Okoye1,&,
Onyedika Godfrey Okoye1,&, ![]() Oluwole Olayemi Olaomi1,
Oluwole Olayemi Olaomi1, ![]() Usman Adamu Gwaram1, Kanati Dennis Apollo1
Usman Adamu Gwaram1, Kanati Dennis Apollo1
&Corresponding author
Introduction: trauma is the leading cause of mortality in individuals less than 45 years. The principles of Advanced Trauma Life Support (ATLS) which is used around the world in resuscitation of trauma patients have been considered to be safe. However, the outbreak of corona virus disease 2019 (COVID-19) has affected the processes and characteristics of acute trauma patients seen around the world. This study is intended to determine the impact of COVID-19 lockdown on the acute trauma patients seen in a Nigerian trauma centre.
Methods: this is a cross-sectional observational study of trauma patients seen in the resuscitation room of the National Hospital trauma centre in Abuja, Nigeria, from 24th February,2020 to 3rd May, 2020. The participants were consecutive acute trauma patients who were grouped into two: five weeks preceding total lockdown and five weeks of total lockdown. Statistical analysis was done using the statistical package for social sciences (SPSS) version 24.0 while results were presented in tables and a figure.
Results: a total of 229 patients were recruited into the study with age range 1 to 62 years, mean age of 28 ± 13 and male to female ratio of 3.87. The patient volume reduced by 41.31% during the lockdown. Though motor vehicular crash (MVC) was the predominant mechanism of injury in both groups making up 37.65% and 23.88% respectively, penetrating assault was more during the lockdown period (17.91% versus 6.17%). The lockdown was further associated with more delayed presentation (52.24% versus 48.15%), more referrals (53.73% versus 32.72%), less severe injury score (29.6% versus 56.7%) and no death in the resuscitation room (0% versus 1.85%).
Conclusion: despite the reduction in the volume of trauma presentations by 41.31%, patients got the required care with less mortality. Efforts should be directed at sustaining access to acute trauma care in all circumstances to reduce preventable trauma deaths.
Trauma remains the leading cause of death in individuals less than 45 years [1]. It is still a public health issue currently accounting for up to 18% of the global burden of diseases [2, 3]. Management of major trauma is protocol driven around the world. Most protocols are in line with the popular Advanced Trauma Life Support (ATLS) principles [4]. These principles have been adjudged to be safe and consistent even in the presence of infectious diseases while employing standard precautions. Recall that the novel corona virus disease (COVID-19) outbreak was first reported in December 2019 with the first patient hospitalized in the city of Wuhan, China [5]. It was further declared a public health emergency of international concern [6] on January 30th, 2020 and a pandemic [7] on March 11th, 2020 by the World Health Organization (WHO). Cases continue to be reported in varying proportions in different parts of the world with attendant mortalities.
COVID-19 is caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The microbial pathogenesis results from host-microbial interaction with attendant host damage from microbial trait or the host immune response or both [8]. Clinical symptoms range from a mild upper respiratory tract-like illness to a life threatening acute respiratory acute respiratory syndrome [9], leading to compromised oxygenation by pulmonary inflammation. The virus damages the infected cells and triggers the production of proinflammatory cytokines which elicit inflammation that damages host cells and tissues locally and at a distance [10]. Neurological mechanisms and thromboembolism are also contributory factors [11, 12].
The COVID surge collaborative recommended thresholds for surgery should be heightened after analyzing an international multi centre cohort of patients who had any kind of surgery with a perioperative diagnosis of COVID-19 [13]. As cases of COVID-19 begin to surge at different trauma centres; changes in the delivery of direct patient care to injured patients require modification [14]. Many trauma centres have adopted more restrictive transfusion practices [15]. Some centres have limited the use of emergency department resuscitative thoracotomy, departing from standard indications [16]. Many hospitals are restricting early tracheostomy due to the perceived risk of incidental viral transmission [17]. Trauma experts believe that all efforts should be made to prevent trauma centres from becoming collateral damage in the fight against COVID-19 [18]. Introduction of lockdown measures in the United Kingdom led to a reported fall of 30 percent in overall emergency admissions [19]. A fall in trauma volume was also observed in Italy but with higher injury severity [20]. In general, the surge in acute ill patients from COVID-19 infections put a significant stress on the already overwhelmed health care system globally [21]. For purpose of emphasis, it is imperative that local acute trauma resuscitation protocols are modified to reflect the changes brought about by this pandemic [22]. This study is intended to compare the pattern of acute trauma patients seen in a dedicated Nigerian trauma centre before and during COVID-19 total lockdown in the country with a view of ascertaining the influence of the lockdown, if any on the patient characteristics.
Study design: this is a cross-sectional observational study of patients seen in the resuscitation room of the trauma centre of National Hospital Abuja.
Setting: the study was done in national trauma centre, a level 1 dedicated trauma centre located in National Hospital Abuja, Nigeria. This centre is a referral centre for major trauma patients within and outside Abuja and serves a population of over three million people.
Participants: all acute trauma patients (presenting within the first 72 hours of their injury as per our existing trauma protocol) who were seen in the resuscitation room during the study period were recruited. The participants were divided into two groups: group A were patients seen in the five weeks period preceding the national total lockdown in Nigeria from 24th February to 29th March 2020 while group B were patients seen during the five weeks period of total lockdown from 30th March to 3rd May 2020.
Variables: information on their demographics including age and sex; mechanism of injury, mode of transportation, accompanying person, referral status, revised trauma score, injury severity score, diagnosis, disposition from the resuscitation room and final outcome were retrieved and subsequently analyzed.
Data sources: data comprising variables mentioned above was retrieved from the trauma registry kept by the trauma centre. Our trauma registry is 32 parameters excel spreadsheet with drop down options where all trauma patients´ information is recorded and updated every 24 hours. Some specific missing information in some cases was completed from the patient case note. Patients with incomplete data despite case notes information were excluded from the study.
Bias: potential sources of bias were addressed by ensuring equal duration of study for both groups of participants and involving an independent statistician for data analysis.
Study size/sampling technique: a total of 229 patients were recruited into the study using consecutive sampling method. These patients included 162 and 67 from group A and B periods respectively. The sample size was a reflection of all eligible patients (injuries 72 hours duration or less) who presented within the study period while the study period was determined by the period of government imposed total lock down in Nigeria.
Statistical methods: data recording, processing and analysis were done using statistical package for social sciences (SPSS) version 24.0. Univariate analysis of data on socio-demographic characteristics and functional outcomes was presented by use of measures of distribution, like frequency distribution tables, central tendency (mean, median and mode) and dispersions (range and standard deviation). As part of baseline analysis, the findings in group A and B patients were compared and subjected to statistical analysis including test of significance. Chi Square test (x²) and likelihood ratios (LR) were used to test the statistical association between/among the distribution on both sides of the study group. A value of P < 0.05 was considered significant. Frequency tables and charts were used where necessary to present the results.
Ethical consideration: ethical clearance was obtained from the institution review board of National Hospital Abuja, Nigeria.
A total of 229 patients were recruited into this study; 162 in the first five weeks preceding total lockdown and 67 in the second five weeks during the total lockdown, representing a 41.35% reduction in the patient volume during the lockdown period. Males were more affected than females in both periods with male to female ratio of 3.87. The mean age of the patients was 28 ± 13. The most frequent age groups were 21-30 years (38.27%), 31-40 years (22.84%) and 11-20 years (16.67%) before the lockdown; and 21-30 years, 31-40 years both accounting for 28.36% and less than 10 years (17.91%) during the lockdown. The least involved age group in both periods was more than 50 years group accounting for only 3.70% and 5.97% respectively (Table 1). While slightly more patients (51.85%) presented in less than two hours before the lockdown, slightly more patients (52.39%) presented after two hours during the lockdown.
The most frequent mechanisms of injury were motor vehicular crash (MVC) (37.65%), motor bike crash (MBC) (19.75%) and domestic accident (8.64%) before the lockdown while MVC (23.88%), penetrating assault (17.91%) and MBC (13.43%) were more frequent during the lockdown. The least frequent mechanism of trauma was pedestrian vehicular crash (PVC) representing 5.56 and 4.48% respectively. The proportion of patients who were referred before the lockdown (32.64%) were nearly half of those who were not referred (67.28%); while in the lockdown period, slightly more patients (53.73%) were referred. Majority of injuries occurred in both the city and suburb at equal amount (43.83%) before the lockdown while most of them occurred in the suburb (52.24%) during the lockdown period (Table 2).
Soft tissue injuries (26.54%) followed by traumatic brain injury (25.92%) and fractures/dislocations (14.20%) constituted most of the diagnoses before the lockdown while traumatic brain injury (25.37%) followed by fractures/dislocations (16.42%) and polytrauma (16.42%) were the commonest diagnoses during the total lockdown. Majority of the injuries felt into the revised trauma score (RTS) of 12; both before (80.25%) and during (67.16%) the lockdown. Injury severity score (ISS) of 75 was recorded only in two patients before the lockdown and none of the patients during the lockdown era (Table 3).
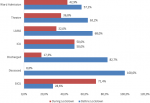
Figure 1 which compared the disposition of the patients from the resuscitation room revealed higher percentages for ward admissions, operating theatre cases, those who left against medical advice (LAMA) and those who died before the lockdown. However, there was equal intensive care unit (ICU) admission and more burns ICU admission during the lockdown. In all, the differences seen among the distribution of the variables before and during lockdown are statistically significant (P=0.001).
Patient volume: a total of 229 patients were seen in the trauma resuscitation room over the study period of ten weeks, 162 patients in the first five weeks before total lockdown and 67 patients during the five weeks of total lockdown. This represents 41.35% reduction in the patient volume during the total lockdown. This reduction in the number of patients is expected in view of the restriction of movement imposed by the Nigerian government to curtail the spread of COVID-19. This is very similar to the findings in the United Kingdom where there was observed reduction of emergency department presentations by up to 30% [19] and acute orthopaedic trauma referrals by up to 34% [23]. This is also similar to other studies in Europe [20] and in Asia where a tremendous reduction of 75% in trauma emergency department footfall was reported [24].
Socio-demographic characteristics: males suffered more injuries than females during both periods of the study. This is a general pattern of trauma epidemiology globally and was not affected by the lockdown. The modal age group among the studied population during the two periods was 21 to 30 years followed by 31 to 40 years. These age groups represent the most active age groups who are more frequently involved in trauma. This is in line with the known fact that trauma most frequently affects the younger population and has remained the commonest cause of death in the same group [1].
Duration and mechanism of injury: more patients presented within two hours before lockdown while more patients presented after two hours during the lockdown period. This delayed presentation during the lockdown period may be due to multiple security check points in an attempt to enforce movement restriction. This observed difference is however, not statistically significant. The predominant mechanism of injury before and during total lockdown remained motor vehicular crash (MVC). This is followed by motorbike crash (MBC) before lockdown and penetrating assault during the total lockdown. MVC reduced from 37.65% before lockdown to 23.88% during the lockdown. The reason is obvious as fewer vehicles were allowed to move during the lockdown. This reduction in MVC was also reported in the Spanish association of surgeons´ document [25]. The proportion of penetrating assault increased from 6.2% before lockdown to 17.9% during lockdown. This higher prevalence of penetrating assault during the total lockdown may be partly due to the relative increase in crime rate occasioned by economic downturn during the lockdown.
Referral status, mode of transportation and location of injury: in the pre-lockdown period, only about 32.72% of patients were referred while in the lockdown period, more patients (53.72%) were referred. This may be related to increased presentation to nearby local health facilities due to restriction of movement. The predominant modes of transportation during both periods under study were private and security vehicles while commercial vehicles were least used. However, the proportion of patients who were transported in ambulance was significantly higher during the total lockdown period. This may not be unconnected to easy access at multiple security check points during the total lockdown. While majority of the injuries happened in the Abuja city before the lockdown, more occurred in the suburb during the total lockdown. This is understandable since majority of the population reside in the suburb where relative activities continued coupled with inadequate enforcement in those areas during the lockdown. The injuries that happened outside Abuja were minimal due to the interstate travel ban in place. When road related injuries are excluded, majority of the injuries (25%) happened at home during the lockdown due to sit at home orders, none happened in recreation centres which were closed during this period and only about 7% happened at workplace due to work from home order for non-essential workers.
Diagnosis and injury severity: in the pre-lockdown period, the most frequent diagnoses were soft tissue injuries, traumatic brain injuries and fractures/dislocations. During the lockdown, they were traumatic brain injuries, fractures/dislocations and polytrauma. This finding relatively reflects the usual injuries and was most likely not impacted by the lockdown. However, more severe injuries were seen before the lockdown than during the total lockdown. This observed difference in severity is statistically significant and may be attributed to more busy roads with no restrictions in the pre-lockdown era.
Disposition from the resuscitation room: the observed reduction of ward admissions, surgical interventions and patients leaving against medical advice (LAMA) from the resuscitation room during the lockdown probably mirrored the differences in the patient volume. While equal proportion of patients was admitted into the intensive care unit in both periods, more patients were admitted into the burns unit during the lockdown period. This later finding was due to burns from cooking gas and scald heightened by stay-at-home order. Finally, no patient died in the resuscitation room during the lockdown period. All the deaths recorded over the study period occurred before the lockdown period. This reflects the severity of injuries which were more in the pre lockdown period as discussed earlier.
Limitations: small sample size due to limited period of the lockdown is seen as one of the major limitations of this study. In addition, comparing the lockdown period with a similar calendar period in the previous year would have given a more objective analysis.
The COVID-19 lockdown in Abuja Nigeria significantly reduced the total volume of acute trauma patients. There was a noticeable increase in referred cases and penetrating assault during the lockdown. Reduction in causes of severe injuries translated to reduced mortality in our centre. Efforts should be directed at sustaining access to acute trauma care in all circumstances to reduce preventable trauma deaths.
What is known about this topic
- COVID-19 pandemic has affected the processes and the procedures in the management of acute trauma patients;
- COVID-19 lockdown was associated with reduction in trauma volume in different parts of the world.
What this study adds
- Despite reduction in the overall acute trauma volume, COVID-19 lockdown was associated with a relative increase in subset of acute trauma patients referred to the trauma centre; in a setting with a hitherto poor referral system;
- COVID-19 lockdown in Abuja Nigeria was associated with less severe injuries and less mortality in the emergency room among acute trauma patients;
- The study will serve as a background knowledge in this subject matter, to stimulate further research in the future.
The authors declare no competing interests.
Drafting of manuscript, study conception and design with the analysis and interpretation of data was done by Onyedika Godfrey Okoye. Acquisition of data: Onyedika Godfrey Okoye, Oluwole Olayemi Olaomi, Usman Adamu Gwaram, Kanati Dennis Apollo. Critical revision: Oluwole Olayemi Olaomi and Usman Adamu Gwaram. All authors read and approved the final version of this manuscript and equally contributed to its content.
Table 1: socio-demographic characteristics of the respondents presenting before and during the lockdown
Table 2: conditions surrounding the injuries of respondents who presented before and during the lockdown
Table 3: diagnosis and severity grading of respondents who presented before and during the lockdown
Figure 1: disposition from the resuscitation room among patients presenting before and during the lockdown
- Sauaia A, Moore FA, Moore EE, Moser KS, Brennan R, Read RA et al. Epidemiology of trauma deaths: a reassessment. J Trauma. 1995 Feb;38(2):185-93. PubMed | Google Scholar
- Krug E. Injury: A leading cause of the burden of disease (WHO/HSC/PV1/99.11) Geneva: world Health Organization; 1999. Google Scholar
- Global burden of diseases, World Health Organization, 2010.
- Committee on trauma, American College of Surgeons´ Advanced Trauma Life Support (ATLS) 10th edition, 2018.
- Wu F, Zhao S, Yu B, Chen YM, Wang W, Song ZG et al. A new coronavirus associated with human respiratory disease in China. Nature. 2020 Mar;579(7798):265-269. PubMed | Google Scholar
- World Health Organization (WHO) Corona virus Disease (COVID 19) Dashboard, January 30, 2020.
- World Health Organization (WHO) Corona virus Disease (COVID 19) Dashboard, March 11th, 2020.
- Casadevall A, Pirofski L. Host pathogen interactions: redefining the basic concepts of virulence and pathogenicity. Infect Immun. 1999 Aug;67(8):3703-13. PubMed | Google Scholar
- Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med. 2020 Apr 30;382(18):1708-1720. PubMed | Google Scholar
- Giamarellos-Bourboulis EJ, Netea MG, Rovina N, Akinosoglou K, Antoniadou A, Antonakos N et al. Complex immune dysregulation in COVID-19 patients with severe respiratory failure. Cell Host Microbe. 2020 Jun 10;27(6):992-1000.e3. PubMed | Google Scholar
- Li YC, Bai WZ, Hashikawa T. The neuroinvasive potential of SARS-CoV2 may play a role in the respiratory failure of COVID-19 patients. J Med Virol. 2020 Jun;92(6):552-555. PubMed | Google Scholar
- Cui S, Chen S, Li X, Liu S, Wang F. Prevalence of venous thromboembolism in patients with severe novel coronavirus pneumonia. J Thromb Haemost. 2020 Jun;18(6):1421-1424. PubMed | Google Scholar
- Royal college of surgeons. Recovery of surgical services during and after COVID-19. Accessed 17th February 2021.
- Coleman JR, Burlew CC, Platnick KB, Campion E, Pieracci F, Lawless R et al. Maintaining trauma care access during the COVID-19 pandemic: an urban level-1 trauma centre´s experience. Ann Surg. 2020 Aug;272(2):e58-e60. PubMed | Google Scholar
- Vanderbilt University Medical Centre. Blood conservation strategies during COVID-19. Accessed 17th February 2021.
- Seamon MJ, Haut ER, Arendonk KV, Barbosa RR, Chiu WC, Dente CJ et al. An evidence based approach to patient selection for emergency department thoracotomy. J Trauma Acute Care Surg. 2015 Jul;79(1):159-73. PubMed | Google Scholar
- Chao TN, Harbison SP, Braslow BM, Hutchinson CT, Rajasekaran K, Go BC et al. Tracheostomy in ventilated patients with COVID-19. Guidelines from the COVID-19 tracheostomy task force, a working group of the airway safety committee of the university of Pennsylvania Health System. Ann Surg. 2020 Sep 1;272(3):e181-e186. PubMed | Google Scholar
- Haut ER, Leeds IL, Livingston DH. The effect on trauma care secondary to the COVID-19 pandemic collateral damage from diversion of resources. Ann Surg. 2020 Sep 1;272(3):e204-e207. PubMed | Google Scholar
- Appleby J. What is happening to non - covid deaths? BMJ. 2020 Apr 24;369:m1607. PubMed | Google Scholar
- Robert Fojut. How coronavirus is affecting trauma systems in Italy. Accessed 17th February 2021.
- Paules CI, Marston HD, Fauci AS. Coronavirus infections - more than just the common cold. JAMA. 2020 Feb 25;323(8):707-708. PubMed | Google Scholar
- Okoye OG. Implementing trauma resuscitation protocol in COVID 19 era: our modifications at the national trauma centre, Abuja, Nigeria. Niger J Clin Pract. 2021 Jan;24(1):138-141. PubMed | Google Scholar
- Kapil Sugand, COVERT Collaborative. The impact of COVID-19 on acute trauma and orthopaedic referrals and surgery in the UK: the �golden peak weeks´of the first national multi-centre observational study. COVERT collaborative. Google Scholar
- Siawhney C, Singh Y, Jain K, Sawhney R, Trikha A. Trauma care and COVID-19 pandemic. J Anaesthesiol Clin Pharmacol. 2020 Aug; 36(suppl 1): s115 - s120. PubMed | Google Scholar
- Aranda-Narváez JM, Tallón-Aguilar I, Pareja-Ciuró F, Martín-Martín G, Gonzálenz-Sánchez AJ, Rey-Simó I et al. Emergency surgery and trauma care during COVID 19 pandemic. Recommendations of the Spanish association of surgeons. Cir Esp. 2020 Oct;98(8):433-441. PubMed | Google Scholar