AB thymoma revealed by a huge intraparenchymal lung mass: a case report
Btissame Es-sabbahi, Mounia Serraj, Baderdine Alami, Mohammed Elbiaze, Mohammed Chakib Benjelloun, Bouchra Amara
Corresponding author: Btissame Es-sabbahi, Department of Pneumology, University Hospital Center Hassan II, Fes, Morocco 
Received: 25 Jan 2021 - Accepted: 10 Feb 2021 - Published: 18 Feb 2021
Domain: Oncology,Pulmonology
Keywords: Thymoma, ectopics locations, primary intrapulmonary thymoma, case report
©Btissame Es-sabbahi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Btissame Es-sabbahi et al. AB thymoma revealed by a huge intraparenchymal lung mass: a case report. Pan African Medical Journal. 2021;38:189. [doi: 10.11604/pamj.2021.38.189.28041]
Available online at: https://www.panafrican-med-journal.com//content/article/38/189/full
AB thymoma revealed by a huge intraparenchymal lung mass: a case report
![]() Btissame Es-sabbahi1,2,&, Mounia Serraj1,2, Baderdine Alami1,3, Mohammed Elbiaze1,2, Mohammed Chakib Benjelloun1,2, Bouchra Amara1,2
Btissame Es-sabbahi1,2,&, Mounia Serraj1,2, Baderdine Alami1,3, Mohammed Elbiaze1,2, Mohammed Chakib Benjelloun1,2, Bouchra Amara1,2
&Corresponding author
Thymoma is an epithelial neoplasm of the thymus, which commonly lies in the anterior mediastinum. Unusually it can be found in other locations as well. Ectopic thymoma rarely presents as an intrathoracic tumor. We report a case of ectopic thymoma presenting as a giant right intrathoracic tumor, the patient was 51-year-old, and who was presented with heaviness in chest and breathlessness. Detailed investigation including chest computed tomography scan revealed a well-defined large solid tumor in the right thoracic cavity, in this case, immunohistochemical analysis demonstrated a thymome AB. The tumor was metastatic to the lung. Patient received a neoadjuvant chemotherapy, with favorable evolution.
Thymic epithelial tumors are rare tumors with variable evolution and prognosis. These are the most frequent tumors of the anterior mediastinum [1,2]. These tumors develop in more of 90% of cases in the anterior mediastinum [3], and diagnosis is made in 2/3 of cases on the incidental discovery of a mass in the anterior mediastinum [3]. However, ectopic thymoma has been reported in a variety of sites [4,5], such as the neck (ectopic cervical thymoma, ECT), [6,7], middle mediastinum [8], posterior mediastinum, pleura [9], lung [10] and the heart. We report the case of an AB thymoma presenting as a giant intrathoracic tumor.
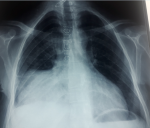
A 51-year-old patient, with a 5-month history off dyspnea, at the physical examination a right basithoracic condensation syndrome was found, radiograph of the chest showed well-defined homogenous lesion in the right hemithorax extending from the hilum to the level of diaphragmatique dome. The medial border merged with the mediastinum with loss of the cardiac silhouette. There was no air bronchogram, calcification, cavitation or rib destruction (Figure 1). Chest computed tomography (Figure 2) showed a solid tumor measuring 120x90x80cm in the right thoracic cavity. The tumor showed a clear limits with polycyclic contours, it occupies the middle lobe and extends to the upper and lower lobes via the splits which have a discontinuous appearance, it comes into contact with the right cardiac cavities without any fatty separation border, with presence of secondary straight pulmonary nodules. Bronchoscopy objectified an aspect of extrinsic compression on the basal pyramid. A primitive bronchial cancer was evoked, as well as a solitary fibrous tumour (polylobate aspect of the mass). The tumour was already metastatic in the lung. An echoguided biopsy of this mass was performed, the anatomopathological examination concluded to a thymoma of type AB, with a positive CD5 and terminal deoxynucleotidyl transferase (TDT). She received chemotherapy according to the College of America Pathologists (CAP) protocol (cisplatin, doxorubicin, cyclophosphamide), a control CT scan after 3 cures showed a discrete decrease in size of the mass, with disappearance of secondary pulmonary nodules, a surgical procedure will be discussed.
The thymus is located in the upper front part of the chest, in the anterior superior mediastinum, behind the sternum, and infront of the heart. The thymus continues to grow after birth, until it reaches its maximum weight at puberty 20-50 grams. After puberty, the thymus becomes progressively involved. In the adult, the parenchyma is gradually replaced by fatty tissue without disappearing completely. Thymoma is the most common primary mediastinal neoplasm in adults and the most frequent tumor of the anterior mediastinum, originating from the epithelial cells of the thymus. Ninety six percent (96%) of the tumors occurring in the anterior or anterosuperior mediastinum, but ectopic localizations have been described in the literature, mainly involving the neck, middle mediastinum, posterior mediastinum, pleura, lung [4-9]. Primary intrapulmonary thymomas (PIT) are very rare events, and are defined as intrapulmonary tumors without associated mediastinal localization, whose anatomopathological examination reveals a thymoma [11]. There is still a great deal of debate about the pathogenesis of PIT, the most widespread theory being embryologic displacement. The human embryo has five pairs of entobranchial pockets whose entoblastic coating gives rise to different organs. The thymus is derived from the third entoblastic pharyngeal sac. In the 5th week of development, the two thymic blanks appear. Then before the 7th week, they migrate in caudal and medial positions to end up under the thyroid gland in a retro sternal intra thoracic position. Accidently, some islands of thymus tissue may be left in unrelated anatomical regions due to defects during descending of thymic buds. This residual tissue may be the cause of developing some disorders such as thymic cyst, cervical thymoma, and ectopic thymus tissue [12]. Although critics of this theory point out that the respiratory primordium develops several weeks before descent of the thymic primordium [11,13]. The second hypothesis is that thymomas can develop from pluripotent stem cells capable of differentiating and giving different histological types. This theory is supported by the unusual localization of other tumors in the lung, namely meningiomas, salivary gland tumors [11,14].
Cases of PIT are very rare, about thirty observations of primary intra pulmonary thymoma have been published since 1951 [11,15-20]. Most of the cases described in the literature occurred after the 5th decade of life, so for our patient she was 51 years old [11]. A slight female predominance was reported, with a much more frequent localization in the right lung [11]. And this was the case of our patient, whose tumor is located in the middle lobes, and extends to the upper and lower lobes. The majority of these tumors have been discovered on chest X-ray in asynmptomatic patients [11,13]. Presenting symptoms have included cough [11], chest pain, asthenia, hemoptysis [13]. In the case described in the present study, the patient had continuous dyspnea, hence the realization of a chest X-ray, which showed a voluminous right paracardiac mass. A primitive bronchopulmonary cancer was strongly suspected, a solitary fibrous tumor was also evoked because off the polylobate character ofthe mass, a bronchial fibroscopy was performed, which found an aspect of extrinsic compression at the level of the basal pyramid, without detectable endobronchial lesions, and since the tumor was already metastatic, surgical resection was not possible, an echoguided trans parietal biopsy was performed. These tumors have a better prognosis when it is surgically resected [11,20]. For our patient, the tumor was already metastatic in the lung, she received neoadjuvant chemotherapy, with favorable evolution, after 3 cures of chemotherapy according to the CAP protocol a regression of the volume of the tumor mass was noted, with disappearance of the secondary pulmonary localizations, a surgical procedure will be discussed.
Ectopic thymomas, even if it is a very rare event, should always be included in the differential diagnosis whenever a large intra thoracic mass is observed, and the histopathological aspect is not typical of a primitive bronchopulmonary.
The authors declare no competing interests.
Bouchra Amara: aquisition of data, drafting the article. Baderdine Alami: aquisition of data. Mounia Serraj, Mohammed Elbiaze, Mohammed Chakib Benjelloun: revising critically the article. All the authors have read and agreed to the final manuscript.
Figure 1: homogenous
lesion in the right hemithorax extending from the hilum to the level
of diaphragmatic dome; the medial border merged with the mediastinum
with loss of the cardiac
silhouette
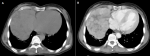
Figure 2: A) non-contrast
CT chest and B) contrast-enhanced CT chest: heterogeneously enhancing mass in
the right thoracic cavity; it showed a clear limits with polycyclic contours,
and it occupies the middle lobe and extends to the upper and lower lobes
- Thomas V, Montpréville De. Thymomes et carcinomes thymiques. Rev mal resp. 2010;27:1281-7. Google Scholar
- Gaubert JY, Cohen F, Vidal V, Louis G, Moulin G, Bartoli JM et al. Imagerie des tumeurs du médiastin. Rev pneumol clin. 2010 Feb;66(1):17-27. PubMed | Google Scholar
- Srirajaskanthan R, Toubanakis C, Dusmet M, Caplin ME. A review of thymic tumors. lung cancer. Elsevier BV. 2008;60:4-13. Google Scholar
- Fukai I, Funato Y, Mizuno T, Hashimoto T, Masaoka A. Distribution of thymic tissue in the mediastinal adipose tissue. J Thorac Cardiovasc Surg. 1991 Jun;101(6):1099-102. PubMed | Google Scholar
- Den Bakker MA, Roden AC, Marx A, Marino M. Histologic classification of thymoma: a practical guide for routine cases. J Thorac Oncol. 2014 Sep;9(Suppl 2):S125-30. PubMed | Google Scholar
- Baek C, Ryu J, Yun J, Chu K. Aberrant cervical thymus: a case report and review of literature. Int J Pediatr Otorhinolarngol. 1997;41:215-222. Google Scholar
- Loney DA, Bauman NM. Ectopic cervical thymic masses in infants: case report and review of literature. Int J Pediatr Otorhinolarngol. 1998 Feb;43(1):77-84. PubMed | Google Scholar
- Minniti S, Valentini M, Pinali L, Malag� R, Lestani M, Procacci C et al. Thymic masses of the middle mediastinum: report of 2 cases and review of the literature. J Thorac Imaging. 1992 Feb;16(2):138-44. Google Scholar
- Moran CA, Travis WD, Rosado-de-Christenson M, Koss MN, Rosai J. Thymomas presenting as pleural tumors: report of eight cases. Am J Surg Pathol. 1992;16:138-44. Google Scholar
- Moran CA, Suster S, Fishback NF, Koss MN. Primary intrapulmonary thymoma: a clinicopathologic and immunohistochemical study of eight cases. Am J Surg Pathol. 1995 Mar;19(3):304-12. PubMed | Google Scholar
- Gong L, Li YH, He XL, Wang Q, Yao L, Zhu SJ et al. Primary intrapulmonary thymomas: case report and review of the literature. J Int Med Res. Jul-Aug 2009;37(4):1252-7. PubMed | Google Scholar
- Sanei B, Tabatabie SA, Bigdelian H, Hashemi SM, Davarpanah AH, Jafari HR et al. Distribution of mediastinal ectopic thymic tissue in patients without thymic disease. Adv Biomed Res. 2015 Jan 30;4:18. PubMed | Google Scholar
- Veynovich B, Masetti P, Kaplan PD, Jasnosz KM, Yousem SA, Landreneau RJ et al. Primary pulmonary thymoma. Ann Thorac Surg. 1997 Nov;64(5):1471-3. PubMed | Google Scholar
- Marchevsky AM. Lung tumors derived from ectopic tissues. Semin Diagn Pathol. 1995 May;12(2):172-84. PubMed | Google Scholar
- Ishibashi H, Takahashi S, Tomoko H, Jotaro S, Satoshi S, Masashi H et al. Primary intrapulmonary thymoma successfully resected with vascular reconstruction. Ann Thorac Surg. 2003 Nov;76(5):1735-7. PubMed | Google Scholar
- Srivastava A, Padilla O, Alroy J, Angelo U, Monika P, Benedict D et al. Primary intrapulmonary spindle cell thymoma with marked granulomatous reaction: report of a case with review of literature. Int J Surg Pathol. 2003 Oct;11(4):353-6. PubMed | Google Scholar
- Moran CA, Suster S, Fishback NF, Koss MN. Primary intrapulmonary thymoma: a clinicopathologic and immunohistochemical study of eight cases. Am J Surg Pathol. 1995 Mar;19(3):304-12. PubMed | Google Scholar
- McBurney RP, Clagett OT, McDonald JR. Primary intrapulmonary neoplasm (thymoma) associated with myasthenia gravis: report of case. Mayo Clin Proc. 1951 Sep 12;26(19):345-53. PubMed | Google Scholar
- Stefani A, Boulenger E, Mehaut S, Adrian C, Marco A. Primary intrapulmonary thymoma associated with congenital hyperhomocysteinemia. J Thorac Cardiovasc Surg. 2007 Sep;134(3):799-801. PubMed | Google Scholar
- Dashottar S, Singh AK, Suhag V, Sunita BS. Ectopic thymoma presenting as a large intrathoracic mass. J Can Res Ther. Oct-Dec 2015;11(4):1033. PubMed | Google Scholar