Emergency embolization for breast pseudoaneurysm following vacuum-assisted biopsy: a case report
Nguyen Thai Binh, Nguyen Minh Duc, Thieu-Thi Tra My, Le Viet Dung, Doan Tien Luu, Le Tuan Linh
Corresponding author: Nguyen Minh Duc, Department of Radiology, Pham Ngoc Thach University of Medicine, Ho Chi Minh City, Vietnam 
Received: 28 Dec 2020 - Accepted: 01 Feb 2021 - Published: 08 Feb 2021
Domain: Radiology, Oncology, Urgent Care Medicine
Keywords: Vacuum-assisted biopsy, pseudoaneurysm, embolization, case report
©Nguyen Thai Binh et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nguyen Thai Binh et al. Emergency embolization for breast pseudoaneurysm following vacuum-assisted biopsy: a case report. Pan African Medical Journal. 2021;38:135. [doi: 10.11604/pamj.2021.38.135.27619]
Available online at: https://www.panafrican-med-journal.com//content/article/38/135/full
Case report 
Emergency embolization for breast pseudoaneurysm following vacuum-assisted biopsy: a case report
Emergency embolization for breast pseudoaneurysm following vacuum-assisted biopsy: a case report
Nguyen Thai Binh1,2, ![]() Nguyen Minh Duc2,3,4,&, Thieu-Thi Tra My2, Le Viet Dung1, Doan Tien Luu1,2, Le Tuan Linh1,2
Nguyen Minh Duc2,3,4,&, Thieu-Thi Tra My2, Le Viet Dung1, Doan Tien Luu1,2, Le Tuan Linh1,2
&Corresponding author
Vacuum-assisted breast biopsy (VABB) is a minimally invasive procedure and has become an important treatment method. Although VABB is a minimally invasive procedure, it might cause complications, particularly those associated with blood vessels. In this article, we aimed to describe a 35-year-old female who experienced pseudoaneurysm post-VABB and was successfully treated with embolization. She presented to the hospital with a suspected left breast tumor. The pathology report after biopsy confirmed fibroadenoma, and the patient underwent VABB to remove the tumor. One hour after VABB, the patient described pain and swelling at the location of the removed tumor. Breast ultrasound revealed a hematoma and pseudoaneurysm. The bleeding did not stop following the application of manual compression. Breast hemorrhage was controlled by endovascular embolization. Pseudoaneurysm is an uncommon complication of VABB, and embolization represents an effective method for the management of breast pseudoaneurysm.
The introduction of breast cancer screening programs has resulted in the increased detection of benign breast tumors [1]. The definitive management of these benign lesions is preferred by patients [2]. Minimally invasive techniques for the treatment of breast lesions have been found to be effective, safe, and associated with acceptable esthetic outcomes [2]. The vacuum-assisted breast biopsy (VABB) technique can be used for both biopsy and benign tumor removal procedures [3]. VABB is performed under ultrasound guidance and typically lasts from 13-60 minutes [2]. Hematoma and bleeding are the most common complications associated with VABB [4]. The open surgical repair of a hematoma or pseudoaneurysm related to VABB is not necessary in all cases, and other minimally invasive methods, such as manual pressure, or percutaneous embolization, are increasingly utilized [5]. In this report, we present a case of VABB associated with vascular complications that were successfully treated with emergency embolization.
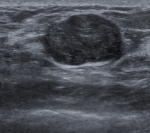
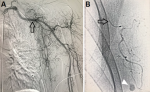
A 35-year-old female underwent a medical check-up due to a painless mass in the left breast, which appeared 2 years prior, without thickening or dimpling of the breast skin, pulling in of the nipple, or bloody nipple discharge. Breast ultrasound revealed a mass at the 3 o´clock position in the left breast, measuring 20mm x 12mm (Figure 1). This mass was oval and hypoechoic, with well-defined borders, oriented parallel to the skin. Pathological findings from a tumor biopsy indicated fibroadenoma. Due to a desire to treat and remove this tumor while maintaining breast esthetics and introducing minimal surgical scars, the patient underwent VABB. After the procedure, a breast ultrasound revealed no hematoma, and manual compression was performed for approximately 10 min, and the patient received a pressure dressing. One hour after VABB, the patient felt pain and swelling in the left breast. Breast ultrasound revealed a large hematoma, measuring 45mm x 30mm at the site of the prior tumor. Although the patient was treated with manual compression and injections of tranexamic acid (Cammic, Vinphaco-Viet Nam), the hematoma continued to increase in size. A pseudoaneurysm was detected on ultrasound. An intervention procedure was conducted using a 5 Fr JB2 (Terumo Corporation, Japan) catheter inserted into the left subclavian artery coronary and left axillary artery, and a selective scan of the left external thoracic artery showed a pseudoaneurysm in the distal branch of this artery (Figure 2). The pseudoaneurysm was successfully embolized using the adhesive N-butyl cyanoacrylate (NBCA) and Lipiodol (Guerbet, France), at a 1:3 ratio. After the intervention, the patient became stabilized, and the hematoma degenerated gradually over 5 days following. A 14 Fr sonde (Bioteq, Taiwan) was inserted to drain the hematoma, and intravenous cefotaxime (Mekophar, Vietnam) was administered at 1 g every 12 hours for 3 days. After 5 days of drainage, ultrasound was used to verify that both the tumor and the hematoma were completely removed. The patient was discharged uneventfully, and at the 2-week and 3-month follow-up appointments, the patient reported no pain and minimal scarring.
The VABB technique, which was developed in late 1995, uses ultrasound guidance to remove samples of breast tissue through a single, small skin incision [6]. Because VABB uses a suction system, a single insertion may be used to obtain larger tissue samples for accurate diagnoses [3]. Additionally, VABB can be used for the treatment and complete removal of benign breast lesions [7]. Complications associated with this procedure may include hematoma; breast vessel injury, which can induce bleeding or pseudoaneurysm; bruises; nipple sensation abnormalities; and pneumothorax, which occurs ata mean rate of 2.5% [7-9]. Most complications are mild to moderate, and severe complications are rare [7] Zheng et al. [10] reported an incidence of hematoma and bleeding after VABB of 11.4% Simon et al. [11] reported that 7% of patients experienced bleeding that could not be controlled by manual compression within 10 minutes post-procedure. A breast pseudoaneurysm is rare, and the first two cases of transcatheter pseudoaneurysm embolization following VABB were reported by Fischman et al. [12]. Following this report, the application of manual compression and pressure bandage was recommended for 48-72 hours following VABB to minimize hematoma occurrence [8]. Multiple factors can contribute to the induction of hematoma following VABB, including nodule size, nodule number, breast shape, menstrual cycle stage, and the efficacy time of bandage less than 12 hours after the operation [13].
Patients with more than two nodules or nodules with a maximum diameter of 25 mm or larger were found to be associated with a significantly increased risk of hematoma after VABB [13]. Hematoma symptoms may occur immediately and present as pulsatile bleeding after VABB [5]. Pseudoaneurysm should be suspected when a patient presents with a rapidly growing breast mass at the previous tumor site after VABB [9]. Cutaneous bruising surrounding the mass may occur [9]. Ultrasound is the most common imaging modality used for the diagnosis of pseudoaneurysm [5]. Grayscale can be used to identify a new cystic mass at the biopsy site, and color Doppler imaging can be used to detect the presence of a swirling flow in the mass [14]. A pseudoaneurysm can also be identified using angiography and computed tomography scans [9]. Breast pseudoaneurysm treatment can be performed using multiple methods, including observation with external pressure dressing; ultrasound-guided, focused compression; thrombin injections; intravascular embolization; and open surgical repair [5,9]. Ultrasound-guided, focused compression is the first-line treatment option and is typically performed using 20 to 30 minutes of direct compression for the treatment of small breast pseudoaneurysms and hematomas [5]. The intravascular embolization of a pseudoaneurysm, using gelfoam, adhesives, or metallic coils, is recommended in cases with significant hemorrhage [9]. Open surgical repair is performed as a last resort when other methods fail [5]. In this case, a complication occurred, despite the tumor not being large. Due to the failure of focused compressions, embolization was required. After successful embolization, the draining of the hematoma facilitated wound healing and reduced infection risk.
This case represents an incident of failure to stop VABB-induced bleeding using focused compression. Although VABB is a safe procedure, associated with a low rate of typically mild to moderate complications, breast vessel injury is always a risk. Patients who present with increasing pain and rapid growth at the tumor site after biopsy must be evaluated for possible pseudoaneurysm. This patient received a prompt diagnosis and was treated successfully with intravascular embolization.
The authors declare no competing interests.
NTB and NMD contributed equally to this article as co-first authors. All the authors have read and agreed to the final manuscript.
Figure 1: fibroadenoma at the 3 o'clock position in the left breast, measuring 20mm x 12mm
Figure 2: A) the left subclavian artery angiogram (arrow); B) a large pseudoaneurysm (arrowhead) in the distal branch of the left external thoracic artery (black arrow)
- Tsai H, Chao M, Ou-Yang F, Jung-Yu K, Jui-Sheng H, Ming-Feng H et al. Accuracy and outcomes of stereotactic vacuum-assisted breast biopsy for diagnosis and management of nonpalpable breast lesions. Kaohsiung J Med Sci. 2019 Oct;35(10):640-645. PubMed | Google Scholar
- Lakoma A, Kim ES. Minimally invasive surgical management of benign breast lesions. Gland Surg. 2014 May;3(2):142-8. PubMed | Google Scholar
- Nakano S, Imawari Y, Mibu A, Otsuka M, Oinuma T. Differentiating vacuum-assisted breast biopsy from core needle biopsy: is it necessary? Br J Radiol. 2018 Dec;91(1092):20180250. PubMed | Google Scholar
- Fu SM, Wang XM, Yin CY, Song H. Effectiveness of hemostasis with Foley catheter after vacuum-assisted breast biopsy. J Thorac Dis. 2015 Jul;7(7):1213-20. PubMed | Google Scholar
- Adler K, Samreen N, Glazebrook KN, Bhatt AA. Imaging features and treatment options for breast pseudoaneurysms after biopsy: a case-based pictorial review. J Ultrasound Med. 2020 Jan;39(1):181-190. PubMed | Google Scholar
- Parker SH, Dennis MA, Stavros AT, Johnson KK. Ultrasound-guided mamtmeotomoy: a new breast biopsy technique. J Diagn Med Sonogr. 1996;12(3):113-118. Google Scholar
- Park H-L, Kim LS. The Current Role of Vacuum assisted breast biopsy system in breast disease. J Breast Cancer. 2011 Mar;14(1):1-7. PubMed | Google Scholar
- Qu S, Zhang W, Li S, Weili H, Lu R, Qing Z et al. The Vacuum-assisted breast biopsy system is an effective strategy for the treatment of gynecomastia. Aesthetic Plast Surg. 2020 Sep 4. PubMed | Google Scholar
- Ingram AD, Mahoney MC. An overview of breast emergencies and guide to management by interventional radiologists. Tech Vasc Interv Radiol. 2014 Mar;17(1):55-63. PubMed | Google Scholar
- Zheng J, Cai S, Song H, Yunlei W, Xiaofeng H, Gang H et al. Prediction of postoperative hematoma occurrence after ultrasound-guided vacuum-assisted breast biopsy in minimally invasive surgery for percutaneous removal of benign breast lesions. Gland Surg. 2020 Oct;9(5):1346-1353. PubMed | Google Scholar
- Simon JR, Kalbhen CL, Cooper RA, Flisak ME. Accuracy and complication rates of US-guided vacuum-assisted core breast biopsy: initial results. Radiology. 2000 Jun;215(3):694-7. PubMed | Google Scholar
- Fischman AM, Epelboym Y, Siegelbaum RH, Joshua LW, Edward K, Francis SN et al. Emergent embolization of arterial bleeding after vacuum-assisted breast biopsy. Cardiovasc Intervent Radiol. 2012 Feb;35(1):194-7. PubMed | Google Scholar
- Huo H, Wan W, Wang Z, Li H, Li J. Percutaneous removal of benign breast lesions with an ultrasound-guided vacuum-assisted system: influence factors in the hematoma formation. Chin Med Sci J. 2016 Mar 20;31(1):31-36. PubMed | Google Scholar
- Bazzocchi M, Francescutti GE, Zuiani C, Del Frate C, Londero V. Breast pseudoaneurysm in a woman after core biopsy: percutaneous treatment with alcohol. Am J Roentgenol. 2002 Sep;179(3):696-8. PubMed | Google Scholar