Giant hiatal hernia
Danilo Coco, Silvana Leanza
Corresponding author: Danilo Coco, Department of General Surgery, Ospedali Riuniti Marche Nord, Pesaro, Italy 
Received: 18 Sep 2020 - Accepted: 19 Sep 2020 - Published: 24 Sep 2020
Domain: General surgery
Keywords: Giant hiatal hernia, diaphragmatic hernia, volvulus
©Danilo Coco et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Danilo Coco et al. Giant hiatal hernia. Pan African Medical Journal. 2020;37:86. [doi: 10.11604/pamj.2020.37.86.26141]
Available online at: https://www.panafrican-med-journal.com//content/article/37/86/full
Giant hiatal hernia
Danilo Coco1,&, Silvana Leanza2
&Corresponding author
A giant hiatal hernia (GHH) is a type III hernia with a sliding and para esophageal component such as > 30% of the stomach, colon, spleen or pancreas due a chronic positive pressure on the diaphragmatic hiatus. Surgical repair requires hernia sac excision, tension-free repair and Nissen fundoplication. Recurrence rates range between 2% and 12%. A 77 years old Caucasian woman presented to the ED with significant thoracic pain, vomiting and bradycardia (<50 bpm). She presented a medical history of atrial fibrillation and anticoagulant therapy. She reported a traumatic rupture of the sternum 5 years ago. Her vital signs were: blood pressure 130/70 mmHg, respiratory rate 40 breaths/minute, heart rate 129 beats/minute and temperature superior of 36 C. Oxygen saturation was 85% on room air. The abdominal examination was normal. Thoracic examination reported reduced vesicular murmur. Laboratory evaluation revealed high leukocytosis with a white blood cell (WBC) count of 16 per mm3. Arterial blood gases (ABG) demonstrated metabolic acidosis. Computed tomography revealed a giant hiatal hernia with stomach, ileum and colon in thoracic cavity. The patient was immediately started intravenous (IV) fluids of 2l in 6 hours, Foley and jugular catheter vein cannulation to support main arterial pressure and urine output. The patient was discussed for surgical operations.
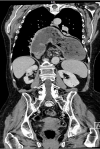
Figure 1: computed tomography revealed a giant hiatal hernia with stomach, ileum and colon in thoracic cavity