Current self-medication practices in the Kingdom of Saudi Arabia: an observational study
Sameer Al-Ghamdi, Tariq Majed Alfauri, Muath Abdullah Alharbi, Mustafa Mohammed Alsaihati, Muhammad Makki Alshaykh, Almuhanad Abdullah Alharbi, Naif Soud Aljaizani, Ibrahim Aidh Allehiby, Matar Abdullah Alzahrani, Abdulsalam Saud Alharbi
Corresponding author: Sameer Al-Ghamdi, Department of Family Medicine, College of Medicine, Prince Sattam bin Abdulaziz University, Al-Kharj11942, Al-Kharj, Saudi Arabia 
Received: 07 Jun 2020 - Accepted: 23 Aug 2020 - Published: 14 Sep 2020
Domain: Family Medicine
Keywords: Self-medication, nonprescription drugs, over-the-counter drugs, OTC drugs, Saudi Arabia
©Sameer Al-Ghamdi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sameer Al-Ghamdi et al. Current self-medication practices in the Kingdom of Saudi Arabia: an observational study. Pan African Medical Journal. 2020;37:51. [doi: 10.11604/pamj.2020.37.51.24098]
Available online at: https://www.panafrican-med-journal.com//content/article/37/51/full
Current self-medication practices in the Kingdom of Saudi Arabia: an observational study
Sameer Al-Ghamdi1,&, Tariq Majed Alfauri2, Muath Abdullah Alharbi3, Mustafa Mohammed Alsaihati3, Muhammad Makki Alshaykh3, Almuhanad Abdullah Alharbi3, Naif Soud Aljaizani3, Ibrahim Aidh Allehiby3, Matar Abdullah Alzahrani4, Abdulsalam Saud Alharbi5
&Corresponding author
Introduction: medication without prescription is a growing public health concern or phenomenon worldwide. This cross-sectional study was designed to study the trends of self-medication among Saudi population.
Methods: a prospective, cross-sectional study including 2004 participants was carried out from different family clinics across the Kingdom of Saudi Arabia (KSA). The clinicians used a self-designed questionnaire to collect the data, using stringent inclusion criteria and exclusion criteria. The questionnaire recorded participants' demographics and included several closed-ended and open-ended questions with options to choose from. The results were gathered, inserted into an excel spreadsheet and analyzed using SPSS version 23. The analyzed information was presented as frequencies and percentages.
Results: our research showed that 924 respondents (46.1%) found it difficult to reach a hospital. Another 45.2% considered the inefficiency of health centers in providing necessary care as the main reason for self-medication. Other causes of self-medication included a lack of medical insurance, insurance not covering the costs for the drugs, and symptoms of the disease being mild enough for not going to the hospital. Analgesics were the most commonly self-administered drugs (84.58%), followed by antipyretics (71.26%), cough syrups (46.86%), eye drops (35.98%), antibiotics (35.28%), flu medication (32.83%), heartburn medication (23.15%), medicines for joint pain (15.02%), and so on.
Conclusion: the majority of Saudi Arabians engage in self-medication and rely on advice from friends and family most of the time, instead of consulting a health professional.
Self-medication or medication without prescription refers to the use of drugs for self-diagnosed illness without any consultation of a healthcare provider [1,2]. World Health Organization (WHO) refers self-medication to the process of medicating oneself to treat self-recognized disorders or illnesses [3]. Medication without prescription is a growing public health concern or phenomenon worldwide [4]. Over the globe, billions of health conditions are treated with self-medication every year [4]. However, the prevalence of self-medication varies in different regions of the world ranging from 38.5% to 92% [4]. It represents that a large portion of the world population uses drugs without proper consultation from a doctor or healthcare professional. In developing countries, approximately 80% of drugs are purchased without any prescription [5]. In Saudi Arabia, up to 81.4% of the general population has reported to use drugs without prescription at some point of their life [6]. There are many reasons which give rise to self-medication. Some of the important reasons include limited or no excess to healthcare facilities, timesaving, prior good experience, minor or mild illness, emergency conditions, inexpensiveness, suggestions by friends and sufficient knowledge of drugs [7]. In addition, self-medication may also be promoted by social, cultural and economic factors [8]. Self-medication can be responsible as well as irresponsible. Over-the-counter (OTC) drugs are the most frequently used medicines as self-medication. The US Food and Drug Authority (FDA) endorses OTC medicines as safe and effective for the community without consultation [9]. OTC drugs are well-known and well-accepted practice around the globe [10]. Self-medication with OTC drugs is considered responsible or safe self-medication. On the other hand, self-medication with prescription drugs is irresponsible or unsafe self-medication which may give rise to dreadful outcomes [11].
Self-medication has benefits as well as drawbacks at both individual and community levels. Individual benefits of self-medication include time-saving or rapid access to treatment, convenience, cost-effectiveness and self-reliance in managing minor illnesses. At a community level, self-medication offers economic benefits by lowering the burden on healthcare facilities while saving limited resources and making it possible for people living in remote areas to obtain medicine immediately at lower costs. On the other hand, self-medication may cause damages at both individual and community levels. At individual level, medication without any consultation of medical professional may result in wrong self-diagnosis and treatment, failure to reach appropriate healthcare facility, inadequate dose, wrong route of administration, improper timing of medicine, prolonged treatment, drug interaction, drug toxicity, adverse events, drug dependence, microbial resistance and wasted resources of the country [5]. Similarly, at a community level, medication without prescription may result in the loss of resources and drug-induced medical conditions. Surprisingly, it has been reported that self-medication with prescription drugs is the leading cause of misuse among physicians [12]. Therefore, there is utmost need of proper guidelines about self-medication. Literature on trends of self-medication or medication without prescription is lacking from Saudi Arabia in terms of its frequency, reasons, type of self-medication and associated factors. Therefore, this cross-sectional study was designed to study the trends of self-medication among Saudi population.
A prospective, cross-sectional study was carried out on responders from different regions of the Kingdom of Saudi Arabia (KSA) from December 2017 to December 2019. The participants were chosen from patients attending different family clinics across the KSA. The clinicians used a self-designed questionnaire to collect the data. Verbal consent was gained from the participants with an option to decline. The questionnaire was in English, but the questions were translated into Arabic by the clinicians for a better understanding of the participants. The questions were asked in Arabic by the clinicians and the answers were marked by them on the English questionnaire on behalf of the patients. Inclusion criteria included people of all age groups, both genders, residents of KSA who presented to family clinics and provided verbal consent to participate in the study. Patients who denied participation in the study, minors who did not provide legal consent by the guardian, short time visitors to KSA, prisoners, and all cases that needed hospitalization were excluded. The questionnaire recorded participants' demographics and included several closed-ended and open-ended questions with options to choose from. The demographics section recorded participants´ age, gender, educational level, nationality (Saudi vs. non-Saudi), marital status, number of kids, and where they belonged inside the KSA. Other questions included practices regarding self-medication, reasons for self-medication, and the types of medication used. The results were gathered, written on an excel spreadsheet and analyzed using SPSS version 23. The analyzed information was presented as frequencies and percentages. The Chi-square test was used to find the correlation between different factors for using drugs and the types of drugs used against patient demographics as individual variables. P < 0.05 was set as statistical significance for all comparisons.
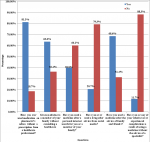
Our study included a total of 2,004 participants who attended family clinics across the KSA. Most of the responders were Saudis (94%) and females (63%). Most of the patients belonged to the age bracket 20-29 (61.5%). Most of the respondents were University graduates (69.0%) and 50% of them belonged to the central KSA region. As for marital status, a substantial proportion was single (75.6%). Out of the married couples, 81.9% had no kids. A detailed description of the participants´ demographics is given in Table 1. Assessing the trends for self-medication, a substantial 1,630 (81.3%) participants responded to having used medication on pharmacist´s advice without a prescription from a healthcare professional. Furthermore, 63.6% of participants gave medications to their family members without consulting a qualified clinician. Advice from friends and family appeared to be the main stimulus for self-medication in 68.6% of cases, followed by information gathered from internet research (39.9%). A detailed analysis of self-medication practices is shown in Figure 1. Our research showed that 924 respondents (46.1%) found it difficult to reach a hospital. Another 45.2% considered the inefficiency of health centers in providing necessary care to be the main reason for self-medication. This is followed by a lack of medical insurance, insurance not covering the costs for the drugs, and symptoms of the disease being mild enough for not going to the hospital as the main triggers in 22.8%, 9.3% and 3.8% cases respectively. Figure 2 analyzes in detail the reasons for self-medication among the participants. Analgesics were the most commonly self-administered drugs (84.58%), followed by antipyretics (71.26%), cough syrups (46.86%), eye drops (35.98%), antibiotics (35.28%), flu medication (32.83%), heartburn medication (23.15%), medicines for joint pain (15.02%), and so on (Figure 3).
Statistical significance was seen between gender (p = 0.001) and different reasons for self-administration with females more likely to self-administer compared to males. Statistical significance was also seen between age (p=0.001), marital status (p=0.001), and the number of kids (p=0.006). No statistical significance was achieved for education level and nationality (Table 2). As for assessing the correlation between different reasons for self-medication, statistical significance was achieved for lack of medical insurance (p=0.05), mild severity of symptoms (p=0.028), ignorance (p=0.000), not having time to go to the doctor (p=0.008), and not liking going to the hospital (p=0.000) only (Table 3). When different medications used were assessed against individual demographic variables, statistical significance was achieved between analgesics, laxatives, food supplements, and educational level with people with university-level education most likely to self-medicate (Table 4). Females were statistically more likely to use antipyretics, cough syrups, antibiotics, medications for joint pain, laxatives, diarrhea medication, and vitamins (Table 5). People between the 20-29 age bracket and singles were more likely to self-medicate as shown by Table 6 and Table 7 respectively.
Several themes can be delineated from the results of our study. First, the demographic details of self-medicators are not in keeping with what is reported by other studies which contend with the same topic. Indeed, two studies which were conducted in Ethiopia found that the majority of self-medicators belonged to the 25-44 and 30-45 age brackets respectively [5,13]. However, results from our study are in keeping with Saudi Arabian studies; one 2015 study found that most self-medicators were in the 23-33 age bracket [14]. These figures may reflect cultural differences between KSA and Ethiopia which account for the observation that self-medicators in KSA are generally younger. Another explanation for this observation is that the purchasing power amongst younger Saudi Arabians may be higher compared to their Ethiopian counterparts, as the former is more developed and has a more robust economy. As regards the reasons for self-medication, almost half of our participants faced challenges in access to healthcare and perceived health care delivery mechanisms as inefficient. This contrasts with the Ethiopian study mentioned previously, which found that the most commonly cited reason for self-medication was that the illness was perceived to be minor. In fact, only 5.1% of the participants in this study felt that healthcare institutions had no value to add, were too far or were inefficient [5]. In a society that more resembles the KSA closely, one study that was scoped towards Indians who lived in urban areas, found that participants most frequently self-medicated because they perceived that their illness was mild, or because they had time constraints which precluded seeking a consultation from a healthcare provider [15].
We observed a similar breakdown in the types of medications which were self-administered by our participants. Including our study, studies scoped to self-medicating behavior in various countries have found that analgesics are the most commonly self-administered drugs, followed by antipyretics and medications which provided symptomatic relief for upper respiratory tract symptoms (e.g. cough syrups) [12,16]. Several correlations were observed in our study. First, there was a statistically significant association between female gender and self-medication. Several studies have found that the prevalence of self-medication amongst women is moderate to high [17]. One study observed that the prevalence of self-medication amongst women may even increase during pregnancy [18]. Second, we also observed that participants with university-level education were more likely to self-medicate. The evidence regarding associations between self-medicating behavior and educational level is conflicted. In the study which looked at self-medication amongst pregnant women, the authors also observed that the odds-ratio of self-medication in women with secondary education was almost three-fold that of women with a high educational level [18]. In a similar Saudi Arabian study, the researchers observed that educational level was significantly associated with the mean knowledge score of medications [14]. It could be posited that participants with a higher degree of education, and therefore, knowledge of medications, could be more inclined to self-medicate as opposed to seeking professional advice from a physician. Similarly, statistically significant correlations were observed between self-medicating behavior and marital status as well as the number of children. This observation could be accounted for by the fact that young children frequently contract viral illnesses and upper respiratory tract infections which warrant symptomatic treatment with over-the-counter medications [19].
This prospective cross-sectional study aimed to delineate current self-medication practices in KSA. The results suggest that the majority of Saudi Arabians engage in self-medicating behavior and rely on advice from friends and family most of the time, instead of consulting a health professional. Self-medication in KSA is associated with female gender, higher education level, being married and having children. These trends could be useful for Saudi health policymakers who seek to educate the public on self-medication in an attempt to mitigate adverse drug reactions and drug-drug interactions, especially amongst vulnerable populations such as children.
What is known about this topic
- Self-medication is one of the major public health concerns worldwide, adopted by billions of people around the globe;
- Over-the-counter (OTC) drugs are the most frequently used medicines as self-medication;
- In Saudi Arabia, up to 81.4% of the general population has reported to use drugs without prescription at some point of their life.
What this study adds
- Like other countries, analgesics, antipyretics and drugs for symptomatic relief for upper respiratory tract symptoms were among the most common self-medications in Saudi Arabia;
- In Saudi Arabia, top five causes of self-medication were difficulty to reach a hospital, inefficiency of health centers in providing necessary care, lack of medical insurance, insurance not covering the costs for the drugs, and symptoms of the disease being mild enough for not going to the hospital;
- The study findings are useful for Saudi health policy makers who seek to educate the public on self-medication in an attempt to mitigate adverse drug reactions and drug-drug interactions, especially among vulnerable populations such as children.
The authors declare no competing interest.
All the authors contributed equally in the study and manuscript preparation. They have also read and agreed to the final manuscript.
This publication was supported by the Deanship of Scientific Research at Prince Sattam bin Abdulaziz University, Alkharj, Saudi Arabia.
Table 1: descriptive statistics
Table 2: correlation between different factors and use of medication without prescription from a healthcare professional
Table 3: correlation between different reasons and use of medication without prescription from a healthcare professional
Table 4: correlation between education level and type of medications used without prescription from a healthcare professional
Table 5: correlation between gender and type of medications used without prescription from a healthcare professional
Table 6: correlation between age groups and type of medications used without prescription from a healthcare professional
Table 7: correlation between marital status and type of medications used without prescription from a healthcare professional
Figure 1: distribution of practices about medication without prescription from a healthcare professional
Figure 2: reasons for using medications without prescription
Figure 3: distribution of the type of medication used without prescription from a healthcare professional
- Jamshed SQ, Wong PS, Yi HC, Yun GS, Khan MU, Ahmad A. Self-medication practices among female students of higher educational institutions in Selangor, Malaysia: A quantitative insight. J Pharm Bioallied Sci. 2016;8(3):217-222. PubMed | Google Scholar
- Kassie AD, Bifftu BB, Mekonnen HS. Self-medication practice and associated factors among adult household members in Meket district, Northeast Ethiopia. BMC PharmacolToxicol. 2018;19(1):15. PubMed | Google Scholar
- World Health Organization. The role of pharmacist in self-care and self-medication. Report of the 4th WHO Consultative Group on the role of pharmacist: Geneva (CH): 1998. Google Scholar
- Abdi A, Faraji A, Dehghan F, Khatony A. Prevalence of self-medication practice among health sciences students in Kermanshah, Iran. BMC PharmacolToxicol. 2018;19(1):36. PubMed | Google Scholar
- Shafie M, Eyasu M, Muzeyin K, Worku Y, Martin-Aragon S. Prevalence and determinants of self-medication practice among selected households in Addis Ababa community. PLoS One. 2018;13(3):e0194122. PubMed | Google Scholar
- Mahzari YI, Aldhfyan YM, Aldossary AM, Alghamdi EA, Alsubaie ML, Abdullah M. Self-medication in Saudi Arabia-a cross sectional study. Int J Med Search. 2019;8(2):79-85.
- Selvaraj K, Kumar SG, Ramalingam A. Prevalence of self-medication practices and its associated factors in Urban Puducherry, India. Perspect Clin Res. 2014;5(1):32-36. PubMed | Google Scholar
- Araia ZZ, Gebregziabher NK, Mesfun AB. Self medication practice and associated factors among students of Asmara College of Health Sciences, Eritrea: a cross sectional study. J Pharmeceut Policy Pract. 2019;12:3. PubMed | Google Scholar
- Chang J, Lizer A, Patel I, Bhatia D, Tan X, Balkrishnan R. Prescription to over-the-counter switches in the United States. J Res Pharm Pract. 2016;5(3):149-154. PubMed | Google Scholar
- Seam OR, Bhatta R, Saha BL, Das A, Hossain M, Naim Uddin SM et al. Assessing the perceptions and practice of self-medication among Bangladeshi undergraduate pharmacy students. Pharmacy (Basel). 2018;6(1):6. PubMed | Google Scholar
- Aljadhey H, Assiri GA, Mahmoud MA, Al-Aqeel S, Murray M. Self-medication in Central Saudi Arabia: Community pharmacy consumers´ perspectives. Saudi Med J. 2015;36(3):328-334. PubMed | Google Scholar
- Kumar R, Goyal A, Padhy BM, Gupta YK. Self-medication practice and factors influencing it among medical and paramedical students in India: A two-period comparative cross-sectional study. J Nat Sci Biol Med. 2016;7(2):143-148. PubMed | Google Scholar
- Jember E, Feleke A, Debie A, Asrade G. Self-medication practices and associated factors among households at Gondar town, Northwest Ethiopia: a cross-sectional study. BMC Research Notes. 2019;12(1):153. PubMed | Google Scholar
- Aljadhey H, Assiri GA, Mahmoud MA, Al-Aqeel S, Murray M. Self-medication in Central Saudi Arabia. Community pharmacy consumers' perspectives. Saudi Med J. 2036(3):328-334. PubMed | Google Scholar
- Selvaraj K, Kumar SG, Ramalingam A. Prevalence of self-medication practices and its associated factors in Urban Puducherry, India. Perspect Clin Res. 2014;5(1):32-36. PubMed | Google Scholar
- Bennadi D. Self-medication: A current challenge. J Basic Clin Pharm. 2013;5(1):19-23. PubMed | Google Scholar
- Karimy M, Rezaee-Momtaz M, Tavousi M, Montazeri A, Araban M. Risk factors associated with self-medication among women in Iran. BMC Public Health. 2019;19(1):1033. PubMed | Google Scholar
- Ebrahimi H, Atashsokhan G, Amanpour F, Hamidzadeh A. Self-medication and its risk factors among women before and during pregnancy. Pan Afr Med J. 2017;27:183. PubMed | Google Scholar
- Escourrou B, Bouville B, Bismuth M, Durrieu G, Oustric S. Self-medication in children by parents: a real risk? A cross-sectional descriptive study. Rev Prat. 2010;60(6 Suppl):27-34. PubMed | Google Scholar