Small bowel obstruction due to congenital adhesion bands during pregnancy: a case report
Sun mi Lee, Jong Chul Baek, Ji Eun Park, Hyen Chul Jo, Jae yoon Jo
Corresponding author: Jong Chul Baek, Department of Obstetrics and Gynecology, Gyeongsang National University Changwon Hospital, Gyeongsang National University, School of Medicine, Changwon, Korea 
Received: 31 Jul 2020 - Accepted: 03 Dec 2020 - Published: 10 Dec 2020
Domain: Obstetrics and gynecology
Keywords: Congenital adhesion band, small bowel obstruction, pregnancy, case report
©Sun mi Lee et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sun mi Lee et al. Small bowel obstruction due to congenital adhesion bands during pregnancy: a case report. Pan African Medical Journal. 2020;37:330. [doi: 10.11604/pamj.2020.37.330.25185]
Available online at: https://www.panafrican-med-journal.com//content/article/37/330/full
Case report 
Small bowel obstruction due to congenital adhesion bands during pregnancy: a case report
Small bowel obstruction due to congenital adhesion bands during pregnancy: a case report
Sun mi Lee1, Jong Chul Baek1,&, Ji Eun Park1, Hyen Chul Jo1, Jae yoon Jo1
&Corresponding author
Small bowel obstruction due to congenital adhesion bands is a very rare occurrence during pregnancy, but is associated with significant fetal and maternal mortality. A 24-year-old primigravida woman, without previous abdominal surgeries, was referred to the emergency department at 35 weeks of gestation with the complaint of sudden abdominal pain. Abdominal magnetic resonance imaging revealed multiple loops of dilated small intestine and adhesion bands in the distal jejunum. The decision was made to proceed with a cesarean delivery and to explore the abdomen to determine the cause of the small bowel obstruction. A 2,680-gram male baby with a 7/9 Apgar score was delivered. A fibrotic band between the jejunal mesentery and distal jejunum caused the small bowel obstruction. After release of the adhesive band, the bowel regained its color and was viable. No adverse event developed in the mother or baby during a 1-year period. Although congenital bands are very rare in pregnant women, they can cause serious maternal and fetal mortality due to the delayed diagnosis and treatment, and physicians should be aware of this clinical condition.
Intestinal obstruction during pregnancy ranges from 1 in 1,500 to 1 in 66,431 deliveries and has been widely reported [1]. It is an uncommon and serious non-obstetric surgical condition associated with serious complications of pregnancy. Postoperative adhesions are the most common cause and are found in 60%-70% of cases, followed by volvulus, which occurs in approximately 25% of cases [1, 2]. In patients without a history of direct abdominal trauma or inflammatory conditions, adhesive bands occur very rarely. Intestinal obstruction due to congenital bands is exceedingly rare, making it difficult to determine the exact incidence. Congenital adhesive bands are an infrequent cause of intestinal obstruction in pregnant women [3, 4]. The fetal mortality rate following maternal bowel obstruction was 20% to 26%, and the maternal mortality rate was between 6% and 20% [1, 5, 6]. Diagnosing a clinical suspicion of congenital bands is challenging due to various clinical presentations and their rarity. However, it should be recognized as a cause of intestinal obstruction because good results can be expected through prompt diagnosis and proper management. Here, we report a case of small bowel obstruction caused by congenital adhesion bands in a 24-year-old primigravida woman at 35 weeks of gestation with no adverse events associated with the patient and fetus.
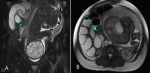
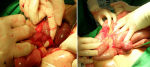
A 24-year-old primigravida woman was referred to the emergency department at 35 weeks of gestation with a complaint of sudden abdominal pain. Perinatal examination was unremarkable. The patient had no history of abdominal surgeries, trauma or pelvic inflammatory diseases. The uterus was nearly term sized, and the fetal heart sounded normal. Physical examination revealed a distended abdomen with decreased bowel sounds. Additionally, the abdomen was tympanic to percussion with right upper quadrant tenderness. Vaginal examination revealed a closed cervical opening. The patient´s blood pressure was 130/90mmHg, the pulse rate was 84/min, and the body temperature was 37.3°C. Fetal ultrasound (USG) showed no abnormalities in the fetus or the placenta. Biometric measurements were compatible with 35 gestational weeks, and the estimated body weight was 2.5 kg. A nonstress test showed reactive patterns, and no uterine contraction was observed. Plain abdominal X-ray showed mechanical obstruction of the small intestine. Abdominal magnetic resonance imaging (MRI) revealed multiple loops of dilated small intestine of the distal jejunum. The point of transition was identified in the distal jejunum. T2-weighted images identified dilated loops of jejunum, and extraluminal compression of the bowel caused by a visible adhesive band (Figure 1). The patient´s symptoms did not improve after over an hour of observation, and the well-being of the fetus could not be guaranteed. The decision was made to proceed with a Cesarean delivery and to explore the abdomen to determine the cause of the small bowel obstruction. Cesarean section began with a lower midline laparotomy incision. A 2,680-gram male baby with a 7/9 Apgar score was delivered. Following repair of the uterine incision, abdominal exploration was performed. One adhesive band was identified in the distal jejunum. Occlusion due to these bands resulted from the trapping of the intestines between the band and mesentery. A fibrotic band between the jejunal mesentery and the distal jejunum caused the small bowel obstruction (Figure 2A). The constricted portion of the bowel appeared dark and congested initially. Meticulous adhesiolysis was performed to free the bowel loops. After release of the adhesive band, the bowel regained its color and was viable (Figure 2B). Mesenteric artery pulsations were palpable, and bowel peristalsis was also observed. The patient was discharged 7 days postoperatively. After 1 week in the neonatal intensive care unit, the male baby (now 2,700 grams) returned home with the mother. No adverse event developed in the mother or baby during a 1-year period.
The reported incidence of acute abdominal pain during pregnancy occurs in 1 in 500-635 pregnancies. Appendicitis is the most common cause of acute abdominal pain during pregnancy, accounting for about a quarter of operative indications for a non-obstetric surgery [7]. Other surgical conditions observed in pregnancy include cholecystitis, pancreatitis and bowel obstruction [8]. For pregnant women, preoperative determination of the cause of acute abdomen may be difficult and inaccurate because of various confounding factors found in normal pregnancy. Additionally, diagnostic radiography is performed less frequently than in the general population due to concerns about radiation exposure. Intestinal obstruction during pregnancy ranges from 1 in 1,500 to 1 in 66,431 deliveries [1]. It is a serious non-obstetric surgical condition that causes serious complications during pregnancy. Postoperative adhesions are the most common cause of this, accounting for nearly 80% of cases, followed by volvulus [1, 2]. When the size of the uterus changes rapidly, especially in the 16th to 20th weeks, the 36th week, and the immediate puerperium, the risk of intestinal obstruction increases. Adhesive bands from previous abdominal surgeries are a causative factor for intestinal obstruction [6].
The congenital adhesion band, previously called an anomalous congenital band, is one of the rarest causes of intestinal obstruction. Congenital bands are considered to have congenitally formed in the abdominal cavity, regardless of previous laparotomy, inflammatory diseases or embryonic remnants [9]. These disease entities may induce intestinal obstruction at any age, but occur more frequently in childhood than in adults [3,4]. Congenital bands that cause bowel obstruction are extremely rare in pregnant women; however, if it is not identified and diagnosed early, it can endanger the fetus and mother and often leads to life-threatening situations [4]. These bands can be found anywhere in the gastrointestinal tract, such as the ascending colon, ileum, and jejunum. The most common site of occurrence of congenital adhesive bands is around the terminal ileum, in the order of the mesentery root, jejunum, liver, and omentum [9]. Importantly, even without a history of abdominal trauma or without previous surgical procedures, intestinal obstruction due to a band cannot be ruled out.
Fetal mortality increases dramatically as the number of gestations increases, and the mortality rate of bowel obstruction is much higher in pregnant women than in the general population. The fetal mortality rate following maternal bowel obstruction was 20% to 26%, and the maternal mortality rate was between 6% and 20% [1, 5]. Typical symptoms of intestinal obstruction during pregnancy are abdominal pain and vomiting [10]. A clinical diagnosis is often difficult in these patients due to nonspecific symptoms associated with pregnancy and the pregnant uterus limiting the effectiveness of physical examinations [6]. Various symptoms of pregnancy itself can be confused on the symptoms of intestinal obstruction, and the ambiguity of symptoms due to pregnancy delays diagnosis and increases complications. Physical examination may not be typical of pain patterns due to the increased abdominal wall due to pregnancy. The abdomen is usually distended and tender on examination. The likelihood of strangulation of the intestine increases with fever, leukocytes, and electrolyte abnormalities [10].
An accurate diagnosis and proper treatment are essential to minimize the morbidity and mortality of pregnant women and fetuses. An imaging study is usually required to clarify the vague clinical situation of pregnant women. Due to concerns about the fetus due to radiation exposure, USG and MRI are the most recommended imaging studies for acute abdomen in pregnant women [10]. USG can be used as the primary imaging technique because of its portability and lack of radiation. However, it may have limited value due to the narrow field of view, changes in the body habitus due to pregnancy, and the presence of fetal structures that interfere with ultrasound. MRI is extremely accurate for the differential diagnosis of both obstetric and non-obstetric pain causes. MRI provides additional definite information when the USG findings are non-diagnostic or equivocal [10]. Treatment of intestinal obstruction in pregnant women is the same as that in the non-pregnant state, although the fetal condition affects this treatment policy. Treatment is first performed with medical management, such as fluid and electrolyte replacement and intestinal decompression through the nasogastric tube. If symptoms are aggravated with fever, tachycardia, and progressive leukocytosis despite medical treatment, early surgical exploration is indicated [7, 10]. If surgery is required in a pregnant woman, an enlarged uterus occupies an intraperitoneal space; thus, a midline vertical incision is recommended for adequate abdominal exposure. Intestinal exposure may be difficult due to pregnancy; in the third trimester of pregnancy when fetal lung maturation is achieved, cesarean section may be performed first to ensure visibility. Because more than one disorder may be indicated, the entire intestine should be examined carefully. Bowel viability should be assessed carefully by an experienced colorectal surgeon in the management of necrotic bowels [10].
Due to various clinical presentations, no history of prior abdominal surgery, and no specific findings on the physical examination or the imaging study, it is difficult to have a clinical suspicion of bowel obstruction caused by a congenital adhesive band in pregnant women. However, the possibility of a congenital adhesion band should be considered as a possible cause of intestinal obstruction, even in the absence of abdominal trauma or previous surgical procedures. An accurate diagnosis and proper treatment can increase the survival rate of the fetus and mother. Treatment of intestinal obstruction in pregnant women is the same as the treatment for women in a non-pregnant state, although the gestational age and lung maturation of the fetus affect this treatment policy. Our patient had a favorable outcome without complications due to the early diagnosis, prompt cesarean section, and exploro-laparotomy.
The authors declare no competing interests.
SM Lee and JC Baek contributed to the diagnosis, surgical treatment and follow-up of the patient as well as the writing and revision of this manuscript. All the authors have read and agreed to the final manuscript.
Figure 1: coronal (A) and axial (B) T2-weighted images identify dilated loops of the jejunum and extraluminal compression of the bowel caused by an adhesive band visible at the transition zone (blue arrow)
Figure 2: operative findings show a fibrotic band between the jejunum mesentery and distal jejunum causing small bowel obstruction (A); after release of the adhesive band, the constricted portion of the bowel appears viable: only band release without segmental resection was performed (B)
- Perdue PW, Johnson Jr HW, Stafford. Intestinal obstruction complicating pregnancy. Am J Surg. 1992 Oct;164(4):384-8. PubMed | Google Scholar
- Ballantyne GH, Brandner MD, Beart Jr RW, Ilstrup DM. Volvulus of the colon: incidence and mortality. Ann Surg. 1985 Jul;202(1):83-9. PubMed | Google Scholar
- Nicolas G, Kfoury T, Shimlati R, Koury E, Tohmeh M, Gharios E, Wakim R. Diagnosis and Treatment of Small Bowel Strangulation Due To Congenital Band: Three Cases of Congenital Band in Adults Lacking a History of Trauma or Surgery. Am J Case Rep. 2016 Oct 7;17:712-719. PubMed | Google Scholar
- Habib E, Elhadad A. Small bowel obstruction by a congenital band in 16 adults. Ann Chir. 2003 Mar;128(2):94-7. PubMed | Google Scholar
- Connolly MM, Unti JA, Nora PF. Bowel obstruction in pregnancy. Surg Clin North Am. 1995 Feb;75(1):101-13. PubMed | Google Scholar
- Zachariah SK, Fenn MG. Acute intestinal obstruction complicating pregnancy: diagnosis and surgical management. BMJ Case Rep. 2014 Mar 6;2014. PubMed | Google Scholar
- Augustin G, Majerovic M. Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol. 2007 Mar;131(1):4-12. PubMed | Google Scholar
- Coleman MT, Trianfo VA, Rund DA. Nonobstetric emergencies in pregnancy: trauma and surgical conditions. Am J Obstet Gynecol. 1997 Sep;177(3):497-502. PubMed | Google Scholar
- Yang KH, Lee TB, Lee SH, Kim SH, Cho YH, Kim HY. Congenital adhesion band causing small bowel obstruction: What's the difference in various age groups, pediatric and adult patients? BMC Surg. 2016 Dec 7;16(1):7. Google Scholar
- Sharp HT. The acute abdomen during pregnancy. Clin Obstet Gynecol. 2002 Jun; 45(2):405-13. PubMed | Google Scholar