Adequacy of blood pressure control and management patterns among hypertensive adult patients attending a sub-county hospital in central Kenya: a cross-sectional study
Eunice Wangechi Muthuki, David Gitonga Nyamu, Peter Ndirangu Karimi, Kefa Ogonyo Bosire
Corresponding author: David Gitonga Nyamu, Department of Pharmaceutics and Pharmacy Practice, School of Pharmacy, University of Nairobi, Nairobi, Kenya 
Received: 05 Aug 2020 - Accepted: 12 Sep 2020 - Published: 07 Dec 2020
Domain: Cardiology,Family Medicine,Internal medicine
Keywords: Blood pressure, antihypertensives, lifestyle activities, sub-county hospital, Kenya
©Eunice Wangechi Muthuki et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Eunice Wangechi Muthuki et al. Adequacy of blood pressure control and management patterns among hypertensive adult patients attending a sub-county hospital in central Kenya: a cross-sectional study. Pan African Medical Journal. 2020;37:325. [doi: 10.11604/pamj.2020.37.325.25366]
Available online at: https://www.panafrican-med-journal.com//content/article/37/325/full
Research 
Adequacy of blood pressure control and management patterns among hypertensive adult patients attending a sub-county hospital in central Kenya: a cross-sectional study
Adequacy of blood pressure control and management patterns among hypertensive adult patients attending a sub-county hospital in central Kenya: a cross-sectional study
Eunice Wangechi Muthuki1, David Gitonga Nyamu2,&, Peter Ndirangu Karimi2, Kefa Ogonyo Bosire3
&Corresponding author
Introduction: there is scarcity of published data on blood pressure (BP) management patterns in rural health facilities in resource constrained settings. The objective was, therefore, to characterize the hypertension management patterns among adult hypertensive outpatients in a sub-county hospital in Kenya.
Methods: cross-sectional study was undertaken among 167 adult patients undergoing hypertension management in Murang'a south sub-county hospital in central Kenya. Patients' sociodemographic characteristics and lifestyles activities were obtained through face-to-face interviews. The level of BP and details of antihypertensive drugs prescribed were acquired from medical files. Statistical associations between adequacy of BP control and sociodemographics as well as management patterns were computed at p≤0.05 using STATA® version 14 software.
Results: adequate blood pressure control was achieved by 40.7% patients. Renin inhibitors (81.5%) and thiazide diuretics (74.3%) were the most prescribed antihypertensive agents, with enalapril-hydrochlorothiazide combination being the preferred dual therapy (34.0%). Adequate BP control was significantly associated with restriction of salt and red meat consumption (p=0.001), living with hypertension for less than five years and use of ≤2 antihypertensives (p=0.05). Patients who restricted salt intake were 2.92 times more likely to have their BP controlled compared to those who did not (AOR=2.92, 95% CI=0.96-8.80), p=0.058) while prescription of a three or more-drug combination reduced the likelihood of BP control by 14% (AOR=0.86, 95% CI=0.69-1.07, p=0.176).
Conclusion: there was poor overall BP control rate among adult outpatients in Murang'a south sub-county hospital. Clinicians should use the fewest number of antihypertensive pharmacotherapies and encourage hypertensive patients to continually engage in lifestyle activities.
Hypertension is the most common modifiable risk factor for cardiovascular diseases, renal failure and premature mortality [1]. It is defined as systolic blood pressure (SBP) of ≥140 mmHg or diastolic blood pressure (DBP) of ≥90 mmHg or both on more than two occasions [1,2]. Hypertension is further defined in different populations: adults aged <60 years, diabetics and patients with chronic kidney disease should have blood pressure (BP) of ≤140/90mmHg while persons aged ≥60 years their BP should not exceed 150/90 [2].
The prevalence of hypertension has been on the rise both globally and locally [3-5] being as high as 56% in some parts of Kenya [6]. The high prevalence rate is characterized by low control rates and poor management [7-9]. In a recent study done in a tertiary referral hospital in Kenya, approximately 30% of the study population had adequate BP control [10]. In another study done in rural Kenya, only 7.3% of participants had adequate BP control [11]. Poorly controlled BP can lead to target organ damage such as the heart; leading to left ventricular hypertrophy, heart failure, coronary heart disease or the brain; leading to cerebral vascular accident. In low resource settings where hypertension specialists are few, the level of blood pressure control remains poor and patients easily progress to end organ damage [12-15]. Hypertension may also cause chronic kidney disease, peripheral artery disease and retinopathy [16].
Studies have revealed varied antihypertensive prescribing patterns and different choices of treatment regimens with poor outcome of therapy [17-19]. In a study done in India, the most frequently prescribed antihypertensive drugs were diuretics followed by angiotensin receptor blockers (ARBs) [17]. Similar regional studies indicated that angiotensin converting enzyme inhibitors (ACEIs) were the most commonly prescribed monotherapy at 20.2% while ACEIs and thiazide diuretic combination was the most commonly prescribed dual therapy at 14.2% [11]. Lifestyle modifications strategies have also been indicated as important in the control of hypertension [20-22]. Although studies have revealed that if the goal BP is not achieved with pharmacological therapies, clinicians should reinforce lifestyle modification and then maximize dosages of drugs or consider adding a third class of drugs, lifestyle modification strategies should be integral from the initial intervention [22]. This present study sought to evaluate the level of BP control and the management patterns among adult outpatients in Murang´a south sub-county hospital. It specifically aimed at describing the prescribing patterns of antihypertensive drugs among clinicians while determining the level of BP control among hypertensive patients with the goal of guiding future management.
Study design and setting: this was a cross-sectional study carried out in Murang´a South sub-county hospital´s medical outpatient clinic (MOPC) in central Kenya. The facility is one of the referral hospitals in rural Kenya and serves outstation hospitals, health centers and dispensaries surrounding it. Interview guide and review of medical records were used to collect data from eligible adult outpatients who attended the clinic. The MOPC had 410 active hypertensive patients who were usually assessed and treated by physicians, medical officers and clinical officers. Their clinical records were kept in the hospital´s record department and retrieved during each patient visit.
Study population: the study population comprised of both males and females aged ≥18 years who had to have attended at least three subsequent clinic visits and prescribed at least one antihypertensive drug in order to assess the course of management. Pregnant mothers and patients with incomplete clinical records were excluded.
Sample size estimation and sampling: the primary outcome variable of this study was adequate BP control among the patients on hypertension management. Similar studies had reported a BP control rate at 30% [10]. Using the prevalence rate of 30% and an equation for calculating sample size for such epidemiological studies [23], a minimum sample of 321 was computed. However, this figure was close to the total clinic population of 410. Therefore, to estimate a representative sample from the total population, the calculated figure was reduced using an equation for correction of sample size for small population to yield the final sample of 167 participants who were used for the study. Simple random sampling using computer generated numbers of the eligible files was used to get the required sample.
Data collection: the study involved extracting relevant information from patients´ medical records using predesigned semi-structured questionnaire. In order to avoid confusion and duplication of enrollment in subsequent clinic appointments, each participant´s file was assigned a unique alphanumeric number to differentiate it from others. The participants were allowed to be reviewed by a clinician which was followed by administration of the questionnaire to capture the sociodemographic characteristics including their age, gender, highest education level, body mass indices, occupation and marital status. The baseline and at least two most recent BP measurements were recorded. The classes and specific types of antihypertensive drugs prescribed were extracted from the patients´ files. Patients were interviewed on lifestyle practices related to the management of hypertension which included salt restriction, dietary approaches to stop hypertension (DASH) diet, moderation of alcohol, regular physical activity and cessation of smoking. The duration that the patient had lived with hypertension was also documented.
Statistical analysis: the collected data was entered into microsoft excel version 2010 spreadsheet to create the database. At the end of data collection and entry period, the data base was checked for errors and then exported to STATA® version 14 statistical software for analysis. Three levels of analysis were carried out: descriptive statistics, bivariate and multivariate analysis. In the first step exploratory data analysis was done to identify unusually entered values and outliers as well as testing the skewness of the data in order to determine the measures of central tendency to be reported. Univariate analysis was done to describe the study population in terms of socio-demographics, clinical characteristics, proportion of patients with adequately controlled BP and the antihypertensives prescribing patterns.
Bivariate analysis was performed to examine the relationship between the outcome variable (adequacy of blood pressure control) and the predictor variables including sociodemographics, duration of hypertension, number of antihypertensives prescribed and lifestyle modifications strategies. Pearson´s Chi square test or Fisher´s exact test was used to compare distribution across arms of categorical variables of controlled and uncontrolled BP.
The results at bivariate analysis informed the multivariable analyses. Predictor variables that statistically significantly impacted on the adequate level of BP at bivariate analysis were subjected to multivariate analysis using stepwise forward logistic regression model in order to adjust for potential confounders impacting on the outcome variable and to identify the correlates of adequate BP control. P-values, 95% confidence interval (CI), crude odds ratios (CORs) and adjusted odds ratios (AOR) were used to estimate the association between predictor and outcome variables and the threshold for statistical significance was set at P≤0.05.
Ethical considerations: ethical approval was sought from Kenyatta National Hospital/University of Nairobi-Ethics and Research Committee (KNH/UoN-ERC) and approved through the reference number KNH-ERC/A/150. Approval from Murang´a south sub-county hospital management team was also sought prior to commencement of the study. All medical requirements and ethical standards relating to research were observed at all times throughout the study.
Social demographic and clinical characteristics of participants: Table 1 shows the sociodemographics and clinical characteristics of the respondents. The female to male ratio was approximately 3:1 and patients were generally old (63.0±12.1 years), married (96.4%), with at least a primary level of education. Over 80% had suffered from hypertension for more than a year. Adequate blood pressure control was found among 40.7% patients (Table 1).
Prescription patterns of antihypertensives among the participants: the frequency of the antihypertensive agents prescribed is shown in Table 2. Renin inhibitors (81.5%) and thiazide diuretics (74.3%) were the most preferred antihypertensive agents among the study population, while the centrally acting antiadrenergics were the least used at 1.2% (Table 2). The participants were either on monotherapy, duo therapy, triple therapy or quadruple drug combinations. The prevalence of these drug combinations are shown in Table 3.
The most commonly prescribed monotherapy was ACEI (16, 51.6%), followed by a CCB (6, 19.4%) and diuretic. Majority of participants (93, 56.9%) were on two drugs (93, 55.6%). Among those on two drugs combination, the most common regimen was diuretic plus an ACEI (33, 34.0%) followed by diuretic plus CCB at 21(22.0%). The most frequent trio therapy was diuretic, BB and ACEI at 12(28.0%), followed by a combination of diuretic, CCB and ACEI (11, 26.0%) (Table 3).
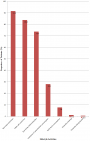
Lifestyle activities for the management of hypertension: the lifestyles practices for the management of hypertension are shown in the Figure 1. Almost all patients avoided alcohol consumption and tobacco smoking. Over 80% of the participants restricted salt and red meat consumption. Almost three-quarters of participants (123, 73.7%) regularly performed some exercise (Figure 1).
Bivariate analysis to determine factors associated with adequate BP control: the associations between patients´ characteristics as well as hypertension management strategies and the level of blood control are presented in Table 4. Patients who restricted salt and red meat consumption had their BP significantly controlled (p=0.001). A significant proportion of patients who had suffered from hypertension for less than 5 years or using ≤2 drugs had better controlled BP (p=0.05) (Table 4).
Correlates of adequacy of blood pressure control: bivariate analysis revealed that salt restriction (p=0.001), limitation of red meat consumption (p=0.001), duration of HTN (p=0.05) and the number of antihypertensives prescribed (p=0.05) significantly impacted on the levels of BP control. These variables were subjected to multivariate analysis using stepwise forward logistic regression to identify the correlates of adequate BP control. Participants who restricted salt in their diet were 2.92 times more likely to have their BP controlled compared to those who did not (AOR=2.92, 95% CI=0.96-8.80), p=0.058). Additionally, prescription of a three or more-drug combination reduced the likelihood of BP control by 14% (AOR=0.86, 95% CI=0.69-1.07, P=0.176) (Table 5).
This study demonstrates the adequacy of blood pressure control and management patterns among 167 adults visiting a rural health facility in central Kenya. Blood pressure control rate was poor at 40.7% which is comparable to available local studies which have revealed that <50% of the patients with hypertension are adequately controlled [11,21]. Furthermore, the local study which showed highest proportion of patients with controlled hypertension was at 49% [7]. Previous studies recorded lower rates. For instance, a study done in a regional referral hospital in central Kenya in 2013 had control rate at 33% [8]. Patients were generally of older age and obese. Although studies have shown positive relationships between obesity and hypertension [13,15,24], it is not known whether they were obese before the diagnosis of hypertension because this was beyond the scope of the present study.
Thiazide diuretics were commonly used agents at 74.3%, comparing well with a study done in a referral hospital in Nigeria that found them being the commonly preferred prescription at 89% [25]. Other related studies have revealed that thiazide diuretics are the most widely prescribed antihypertensive agents [8,11,25]. Though the findings are in line with current guidelines which advocate for a thiazide diuretic as the first line drug for the black population [2], these agents could have been preferred because they are cheap and readily available locally compared to other antihypertensive medications. A combination of ACEI and a diuretic was the most commonly prescribed dual therapy. Similar local studies have demonstrated consistent findings [8,10,11]. ACEIs and diuretics, in addition to being effective in reducing BP, are readily available in most of Kenyan public hospitals. They are relatively cheap and the preferred dual therapies especially in patients presenting with elevated blood pressure which is not responding to a single agent.
In other parts of the world, antihypertensive prescribing patterns differ markedly. For instance, a study done in Bangladesh on patterns of drugs prescribed for hypertension treatment found that most patients were on monotherapy at 62% and ARBs were the most common at 37% followed by CCBs at 33% and diuretics at 1.5% [26]. The discrepancies could be attributed to differences in guideline recommendations and populations studied [23] or different economic status which affect the affordability and hence the choice of drugs.
The present study revealed that having three or more drugs in the regimen significantly reduced the odds of having controlled BP as has been revealed in related studies [8,11]. This is, however, contrary to the expectations. Obviously, adequate BP control would be expected from patients on two or three drugs regimen. Perhaps the contrary observations could be due to refractory hypertension, inadequate dosing and non-adherence to medications because of increased pill burden or white coat hypertension. Related studies have indicated different and conflicting findings. A study done in a regional referral hospital in central Kenya attributed better control of hypertension to old age, having diabetes and being on three or more drugs [8].
This present study demonstrated that the lifestyle modification strategies that were significant to BP control were restricting salt in the diet, limiting red meat in take, quitting smoking and moderation in alcohol consumption which were comparable to other studies [27,28]. The overall effects of lifestyle modifications on BP reduction and in prevention of cardiovascular events cannot be underestimated as outlined in the guidelines and demonstrated by the studies [23,24]. A randomized trial conducted on the effects of lifestyle modifications on BP found that weight loss, restriction of salt intake, increased physical activity and observing DASH diet lowered BP [29]. Observing healthy lifestyle was also found to have an impact on all-cause and cardiovascular mortality after stroke in a study done in USA, where abstaining from smoking and exercising regularly had independent association on all-cause mortality reduction [30]. There is a possibility that the clinicians had already informed patients the importance of lifestyle activities in blood pressure management at the time of diagnosis.
While the study provides some useful insights for future management of hypertensive patients in rural settings in Kenya, the main limitation patients could have over-rated or under-rated their experiences by the virtue of the nature of the face to face interview. In addition, the findings may not be reflective of what was occurring over a prolonged period of time but will provide some direction for the future management of hypertension in rural resource limited settings.
The overall BP control rate among adult patients in Murang´a sub county was low. Adequate BP control was correlated with patient reported restriction in the use of salt, red meat and the use of one or two drugs. Clinicians should aim at prescribing the fewest number of different classes of antihypertensives and encourage patients to continually engage in lifestyle activities. Future studies should find out why the large proportion of patients had uncontrolled BP.
What is known about this topic
- The prevalence of hypertension has been on the rise both globally and locally being as high as 56% in some parts of Kenya;
- There is poor control of BP among hypertensive adult outpatients in Kenyan health facilities;
- The most recommended antihypertensives for the Kenyan population are thiazide diuretics and calcium channel blockers.
What this study adds
- Hypertensive patients followed up in rural Kenyan health facilities are generally of older age and obese;
- The most preferred antihypertensive therapies in rural health facilities are renin inhibitors and thiazide diuretics;
- Lifestyle modification strategies and use of 2 antihypertensive drugs are correlated with adequate BP control.
The authors declare no competing interests.
EWM and DGN conceptualized the idea; EWM wrote the concept and collected the data; DGN and PNK assisted data analysis and interpretation; DGN drafted the manuscript; KOB reviewed the manuscript. All the authors have read and agreed to the final manuscript.
The authors wish to thank all staff and patients at Murang´a sub-county hospital MOPC clinic for the support during the study.
Table 1: sociodemographic and clinical characteristics of the study population (N=167)
Table 2: specific antihypertensive drugs prescribed
Table 3: specific types of antihypertensive therapies prescribed
Table 4: relationship between blood pressure control and other study variables
Table 5: correlates of adequate BP control among the study participants
Figure 1: lifestyle behavior among hypertensive patients
- World Health Organization. A global brief on hypertension. WHO press. 2013;40(27):1-40.
- Hernandez-Vila E. A review of the JNC 8 blood pressure guideline. Tex Heart Inst J. 2015;42(3):226-228. PubMed | Google Scholar
- Adeloye D, Basquill C. Estimating the prevalence and awareness rates of hypertension in Africa: a systematic analysis. PLoS One. 2014;9(8):e104300. PubMed | Google Scholar
- World Health Organization. Global health observatory data: raised blood pressure. WHO press. 2016;39-40.
- World Health Organization. World health statistics: a snapshot of global health. WHO press. 2012;(2):33-46. Google Scholar
- Ministry of Health NCD. Kenya stepwise survey for non communicable disease risk factors 2015 report. KNBS J. 2015;2-12.
- Joshi MD, Ayah R, Njau EK, Wanjiru R, Kayima JK, Njeru EK et al. Prevalence of hypertension and associated cardiovascular risk factors in an urban slum in Nairobi, Kenya: a population-based survey. BMC Public Health. 2014;14:1177. PubMed | Google Scholar
- Mutua EM, Gitonga MM, Mbuthia B, Muiruri N, Cheptum JJ, Maingi T. Level of blood pressure control among hypertensive patients on follow-up in a regional referral hospital in central Kenya. Pan African Medical Journal. 2014;18:278. PubMed | Google Scholar
- van de Vijver SJM, Oti SO, Agyemang C, Gomez GB, Kyobutungi C. Prevalence, awareness, treatment and control of hypertension among slum dwellers in Nairobi, Kenya. J Hypertens. 2013;31(5):1018-24. PubMed | Google Scholar
- Mongi A, Nyamu D, Karimi P, Maru S. Evaluation of the management of hypertension among diabetic and non-diabetic adult outpatients at a referral hospital in Kenya. AJPT Journal. 2016;5(2):93-99. Google Scholar
- Mbui JM, Oluka MN, Guantai EM, Sinei KA, Achieng OL, Jande M et al. Prescription patterns and adequacy of blood pressure control among adult hypertensive patients in Kenya: findings and implications. Expert Rev Clin Pharmacol. 2017;10(11):1263-71. PubMed | Google Scholar
- Stanifer JW, Jing B, Tolan S, Helmke N, Mukerjee R, Naicker S et al. The epidemiology of chronic kidney disease in sub-Saharan Africa. Lancet Glob Health. 2014;2(3):174-81. PubMed | Google Scholar
- Papazafiropoulou A, Skliros E, Sotiropoulos A, Papafragos C, Gikas A, Apostolou O et al. Prevalence of target organ damage in hypertensive subjects attending primary care: CVPC study (epidemiological cardio-vascular study in primary care). BMC Fam Pract. 2011;12:75. PubMed | Google Scholar
- Tiwaskar M. End organ protection. Medicine Update J. 2012;22:157-63.
- Addo J, Smeeth L, Leon DA. Hypertensive target organ damage in Ghanaian civil servants with hypertension. PLoS One. 2009;4(8):e6672. PubMed | Google Scholar
- National High Blood Pressure Education Program. The seventh report of the joint national committee on prevention, detection, evaluation and treatment of high blood pressure. Bethesda (MD): National Heart, Lung, and Blood Institute (US). 2004 Aug;04-5230. PubMed | Google Scholar
- Bajaj JK, Sood M, Singh SJ, Jerath P. Prescription patterns of antihypertensive drugs and adherence to JNC VII guidelines in a tertiary care hospital in north India. Int J Medicine and clinical research. 2012;3(2):118-20.
- Alba-Leonel A, Carvajal A, Fierro I, Castillo-Najera F, Campos-Ramos O, Villa-Romero A et al. Prescription patterns of antihypertensives in a community health centre in Mexico City: a drug utilization study. Fundam Clin Pharmacol. 2016;30(3):276-81. PubMed | Google Scholar
- Gu Q, Burt VL, Dillon CF, Yoon S. Trends in antihypertensive medication use and blood pressure control among united states adults with hypertension: the national health and nutrition 2001 to 2010. Circulation. 2012;126(17):2105-14. PubMed | Google Scholar
- Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5):487-97. PubMed | Google Scholar
- Gosmanova EO, Kovesdy CP. Adherence to antihypertensive medications: is prescribing the right pill enough. Nephrol Dial Transplant. 2015;30(10):1649-56. PubMed | Google Scholar
- James PA, Ortiz E. JNC 8 hypertension guideline algorithm. JAMA. 2014;311(5):507-20.
- Kasiulevicius V, Šapoka V, Filipavičiūtė R. Sample size calculation in epidemiological studies. Gerontologija J. 2006;7(4):225-31. Google Scholar
- Tesema S, Disasa B, Kebamo S, Kadi E. Primary health care: open access: knowledge, attitude and Ppractice regarding lifestyle modification of hypertensive patients at Jimma University Specialized Hospital, Ethiopia. Primary Health Care J. 2016;6(1):1-4. Google Scholar
- Etuk E, Isezuo SA, Chika A, Akuche J, Ali M. prescription pattern of anti-hypertensive drugs in a tertiary health institution. Ann Afr Med. 2008;7(3):128-32. PubMed | Google Scholar
- Hasan J. Pattern of drugs prescribed for treatment of hypertensive patients: Bangladesh. Academic Journals. 2016;10(25):521-5. Google Scholar
- Marfo AFA, Mercy FTO, Addo O, Saana II. Ghanaian hypertensive patients understanding of their medicines and life style modification for managing hypertension. International Journal of Pharmacy and Pharmaceutical Sciences. 2014;6(4):165-170. Google Scholar
- Durai V, Muthuthandavan AR. Knowledge and practice on lifestyle modifications among males with hypertension. Indian Journal of Community Health. 2015;27(01):142-149. Google Scholar
- Svetkey LP, Erlinger TP, Vollmer WM, Feldstein A, Cooper LS, Appel LJ et al. Effect of lifestyle modifications on blood pressure by race, sex, hypertension status and age. J Hum Hypertens. 2005;19(1):21-31. PubMed | Google Scholar
- Towfighi A, Markovic D, Ovbiagele B. Impact of a healthy lifestyle on all-cause and cardiovascular mortality after stroke in the USA. J Neurol Neurosurg Psychiatry. 2012;83(2):146-151. PubMed | Google Scholar