The epidemiological characteristics of COVID-19 in Libya during the ongoing-armed conflict
Mohamed Ali Daw, Abdallah Hussean El-Bouzedi, Mohamed Omar Ahmed, Ali Ali Alejenef
Corresponding author: Mohamed Ali Daw, Department of Medical Microbiology and Immunology, Faculty of Medicine, University of Tripoli, CC 82668, Tripoli, Libya 
Received: 14 Jul 2020 - Accepted: 17 Sep 2020 - Published: 05 Nov 2020
Domain: Epidemiology,Infectious diseases epidemiology
Keywords: Libya, COVID-19, armed conflict
©Mohamed Ali Daw et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mohamed Ali Daw et al. The epidemiological characteristics of COVID-19 in Libya during the ongoing-armed conflict. Pan African Medical Journal. 2020;37:219. [doi: 10.11604/pamj.2020.37.219.24993]
Available online at: https://www.panafrican-med-journal.com//content/article/37/219/full
Outbreak investigation report 
The epidemiological characteristics of COVID-19 in Libya during the ongoing-armed conflict
The epidemiological characteristics of COVID-19 in Libya during the ongoing-armed conflict
Mohamed Ali Daw1,&, Abdallah Hussean El-Bouzedi2, Mohamed Omar Ahmed3, Ali Ali Alejenef4
&Corresponding author
COVID-19 can have even more dire consequences in countries with ongoing armed conflict. Libya, the second largest African country, has been involved in a major conflict since 2011. This study analyzed the epidemiological situation of the COVID-19 pandemic in Libya, examined the impact of the armed conflict in Libya on the spread of the pandemic, and proposes strategies for dealing with the pandemic during this conflict. We collected the available information on all COVID-19 cases in the different regions of Libya, covering the period from March 25th to May 25th 2020. The cumulative number of cases and the daily new cases are presented in a way to illustrate the patterns and trends of COVID-19, and the effect of the ongoing armed conflict was assessed regionally. A total of 698 cases of COVID-19 were reported in Libya within a period of three months. The number of cases varied from one region to another and was affected by the fighting. The largest number of cases were reported in the southern part of the country, which has been severely affected by the conflict in comparison to the eastern and western parts of the country. This study describes the epidemiological pattern of COVID-19 in Libya and how it has been affected by the ongoing-armed conflict. This conflict seems to have hindered access to populations and there by masked he true dimensions of the pandemic. Hence, efforts should be combined to combat these consequences.
Introduction
The COVID-19 pandemic has had major impacts on all aspects of life worldwide. No country can be considered safe, whether rich or poor. COVID-19 is a global concern not only as a huge health problem, but also socially, economically, politically and even ethically [1-3]. COVID-19 has caused huge numbers of deaths even in advanced, economically strong, politically stable countries with the best healthcare services [4, 5]. COVID-19 has also affected most African countries, with over 103,875 cases and 3,184 deaths. The largest number of cases have been recorded in South Africa and 64,388 cases have been reported in the WHO African region [6, 7]. Many African countries suffer from internal conflicts complicated by the emergence of some infectious diseases. One example is the Ebola epidemic in the Democratic Republic of Congo which happened side by side the armed conflict and geopolitical volatility, which led to the displacement of one million people [8, 9]. Libya is the second largest African country which shares its borders with the Mediterranean Sea and possesses huge natural resources. The armed conflict that started in 2011 has continued and became more complicated by April 2019, resulting in extensive mortality, injury and population displacement [10, 11]; then the COVID-19 arrived.
Armed conflicts cause deaths, injuries, destruction of infrastructures, and physical damage or destruction of healthcare delivery facilities. This facilitates the spread of newly emerging diseases. Hence, conflict zones are more susceptible to the spread of infectious diseases, including COVID-19. Concerns about the impact of the pandemic in countries experiencing armed conflict have been expressed. Such countries include Syria, Libya and Yemen, where the impact may go even beyond the borders of these countries [12, 13]. Many studies have been published on all aspects of COVID-19, but not enough attention has been paid to its epidemiology in conflict zones [14, 15], such as Libya, Sudan and Somalia. This study aimed to examine the status and patterns of COVID-19 in Libya during wartime and the effect of the fighting on its emergence and spread. The study also seeks to highlight potential strategies to minimize the impact of this pandemic on Libyans during the conflict.
Methods
The daily number of new COVID-19 cases was obtained from records made publicly available by national, provincial and municipal authorities throughout Libya and was recorded nationally and regionally. Information on the armed conflict was obtained from the army press offices in Tripoli and Benghazi, from the Ministry of State for families of martyrs, injured and missing persons and as described previously [10, 11]. These data included the number of deaths and injuries. The epidemiological data of all confirmed COVID-19 patients from March 25th 2020 to June 25th 2020 in the centers for COVID-19 diagnosis were collected from all the Libyan regions. Data such as the geographic locations and population densities in the counties and regions are shown in supplement-1 [16]. Laboratory confirmation of COVID-19 in Libya is being done by the National Center for Disease Control. Nasopharyngeal and oropharyngeal swab samples are collected following standard safety procedures. RNA is extracted using QIAamp™ viral RNA mini kit from Qiagen™ according to the manufacturer´s instructions, as previously published [17]. Analysis is done by the real-time reverse transcriptase-polymerase chain reaction (RT-PCR) for all suspected cases following the protocol established by the WHO [18]. Biosafety cabinets are used and the work is done according to laboratory biosafety guidelines.
The geographic distribution of COVID-19 and the mapping of the armed conflict during the pandemic were determined as described [10, 19, 20]. As the armed combat an affect the prevalence of COVID-19 in the surrounding communities, the prevalence of COVID-19 in each city was recorded along with the distance to the fighting on the front lines. Distant cities were defined as those over 100 km away from the fighting area and adjacent cities as those within 100 km. A map of the regional distribution of COVID-19 from March 25th 2020 to June 25th in Libya was made, and the number of confirmed COVID-19 cases were colour coded on the map. Microsoft Excel and SPSS version 12.0 were used for data entry and analysis. The continuous variables included the daily cumulative number of cases, the daily number of newly confirmed cases, the number of deaths and the numbers of severe and recovered cases [21]. The data were summarized as means ± standard deviation or as medians, and the percentage of patients in each group was calculated. The available data were plotted to show the daily number of cumulative cases for each region and province. The geographical distribution of COVID-19 and the status of the war activities were drawn on a map of Libya.
Results
The population in this study consisted of 698 confirmed COVID-19 cases reported from all over the Libyan regions (Table 1). Patients ages ranged from 12 to 74 years, with an average of 43 years. Most of the patients (581, 83.2%) were males. Mortality was low 18 (2.6%). There were 140 recoveries (20.1%), leaving 540 cases still active (77.4%). Of the reported cases, 209 cases (29.9%) were initially imported and the rest were acquired within the Libyan territories. Though the southern region has the smallest population, COVID-19 prevalence was highest in the south 292 (41.8%) of all cases. There were 235 cases (33.7%) in the western region which is the most populous and 171 cases (24.5%) in the eastern region. Figure 1 shows the cumulative numbers of COVID-19 cases in the country from March 25th 2020 to June 25th 2020. Figure 1 shows the total number of cases in the three regions of Libya. The total number of cases continued to increase with time in all parts of the country. Figure 2B shows the daily change in the number of new cases since March 25 th 2020. The daily number of new cases in the three regions showed an increasing trend, particularly in the south. The number of daily cases peaked on May 27th and then declined slightly, particularly in the western and eastern regions.
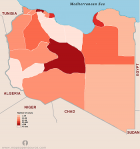
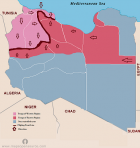
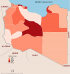
The geographic distribution of the cumulative cases of COVID-19 reported in Libya is shown in Figure 2. The number of cumulative cases is the daily sum of all confirmed cases from March 25th 2020 to June 25th 2020. The regional distribution of COVID-19 is quite obvious with significant spatial agglomeration. The southern region of Sebha had the largest number of cases 292 (41.8%), followed by Tripoli 110 (15.8%) then Musrata 87 (12.5%) in the west and Benghazi 99 (14.2%) in the east. In other Libyan counties such as Gharian, Ojula, Surman, Nalout, Ghat, and Jufra; the number of cases ranged from 10 (1.4%) to 79 (13.3%). No cases were reported in central counties such as Tarhona, Sert and Tawerga. It is evident that regional distribution of the disease varies significantly among the provinces and cities in Libya (p = 0.001). Figure 3 shows the locations of the armed conflict during the emergence of COVID-19. Along the front lines, forces allied with the government located Tripoli (which controls mainly the western region) are pitted against forces allied with the government located in Benghazi (controlling the eastern region). The eastern forces tried to take control of the western region, which led to the spread of the fighting from Jdabia till Tripoli. The cities that are within 100 km of the fighting are the most affected (p< 0.001). These include Sert, Tawerga and Tarhona, which have been devastated by the ongoing conflict and in which no official health authority can work and no cases of COVID-19 have been reported. Distant counties located over 100 km away from the fighting, mainly the southern region, reported large numbers of infections.
Discussion
Based on the 689 cases reported within a three-month period (March 25th till June 25th 2020), we analyzed the epidemiological situation of COVID-19 all over Libya as well as the effect of the ongoing armed conflict on the pandemic patterns. The average age was 43 years and mainly males were affected, with a male-to-female ratio of 4.4:1.0. Of these patients, 540 (77.4%) are still hospitalized, 140 (20.1%) were discharged and 18 (2.6%) died. The number of daily new cases peaked between May 5th and May 7th in the western region, where the first cases were reported. Cases were reported in the eastern region on April 26th and later in the south on May 14th. The total number of cases has started to increase substantially, particularly in the southern region and with no clear sign of declining. This suggests that the epidemic in Libya is not under control and that, strict prevention and control measures have not been adopted. Nevertheless, despite the numerous challenges that the Libyan population has to face since the armed conflict started in 2011, including deaths, injuries and internal displacement of populations; the response to the epidemic and the resilience of the healthcare system has been reasonable [22, 23]. However, the situation remains precarious and a COVID-19 outbreak in this country would overload an already fragile healthcare system and poor baseline health status. Libya was the last country in the MENA region to report the first case of corona virus. However, preliminary epidemiological analysis carried out by Daw indicated that COVID-19 might have arrived in Libya as early as January-February 2020, which has not been reported by the Libyan health authorities [24, 25].
This study investigated the geographic distribution of COVID-19 in Libya and the effect of the ongoing-armed conflict. The number of cases varied greatly from one region to another and the pattern was significantly influenced by the armed conflict. It is worth noting that Sebha in the southern region was the worst-hit city and had the highest number of infected cases. The increase in confirmed cases at any location will inevitably lead to increases in adjacent regions, a positive spillover effect. This was first seen after the first cases were reported in Tripoli and Musrata in the western region, which were followed by spread to Zawia, Surman, Zletan and Alkomas. Likewise, in the eastern region the disease spread from Benghazi to Jalo, Ajdabia, Derna and Tubrak and in the south from Sebha to Murzak, Obari, Wadishati and Ghat. This parallels, to a much smaller extent, the pandemic spread from Wuhan to the neighboring provinces and then all over China and the Italian scenario, where the pandemic started in northern Italy, which at one time accounted for as much as 71.5% of the cases and 81.8% of the deaths and then spread over the rest of Italy [26, 27]. Comparison of the epidemiologic situations in different parts of Libya indicates that the ongoing armed conflict has affected the geographic spread of COVID-19 in two ways. On the one hand, it hindered access to populations and thus masked the actual status of the pandemic, particularly in cities such as Tarhona, Tawerga and Sert. On the other hand, it aggregated the spread of the pandemic to distant cities such as Sebha. Hence, the cross-national variation in the cumulative number of COVID-19 cases due the armed conflict is evident. Intervention strategies should be planned with that in mind [28, 29].
Controlling the emergence of infectious diseases in conflict situations is challenging because the fighting creates situations that facilitate the emergence of infectious diseases and enhance their transmission. These may include but are not limited to inadequate surveillance and response systems [30]. However, the Libyan authorities have taken measures to cut off the source of infection, such as lockdown of cities and implementation of isolation procedures but those were mainly restricted to Tripoli and Benghazi. Other regions were not comprehensively or effectively covered. Hence, mapping the disease enables the national authorities to ensure effective implementation of protective infectious disease interventions. This can be achieved by applying internationally accepted standards, guidelines and tools adapted to conflict situations, and this should be supported by specific training of health planners and health facility staff, and rapid mobilization of international experts to provide technical field support as required [30, 31].
Despite the valuable epidemiological information that this study presents, it has several limitations and uncertainties, particularly as it was carried in a conflict-ridden country where security is lacking and collecting accurate information is difficult. First, the number of reported cases is affected by uncertainties due to problems in accuracy in the daily reports of new notifications, particularly from the regions affected by ongoing armed conflict. Furthermore, it refers only to cases confirmed by molecular analysis, which is not feasible in all suspected situations. Daw [25] and Chen et al. advocated that patients are the key cause of COVID-19 infection [32]. Accordingly, patients with mild or less severe symptoms should be taken into account as they may lead to an increase in infectivity and fatality. Secondly, the study did not analyze the medical care resources and healthcare capacities (number of hospital beds and physicians) used to combat the pandemic, especially that the patients are scattered over a very large area. The resources are most likely inadequate for a large influx of patients.
This is one of the first studies to describe the epidemiological status of COVID-19 in an armed conflict area such as Libya and show the effect of the conflict on the epidemiologic pattern. As expected, COVID-19 spread from one region to another, but this spread was influenced by the ongoing battles. By June 2020, the numbers of COVID-19 cases and deaths were still increasing in Libya, but the real situation might have been at least partially masked in communities in close proximity to battle zones and undetected in remote communities in the Sahara area. The ability to contain the spread of infections will depend on the development of enforceable national policies and success ineffective education of the population in the reduction of infection risk according to international standards [33]. At the present time, achievement of such objectives is unpredictable if the ongoing armed conflict is not ended.
The authors declare no competing interests.
Mohamed Ali Daw conceived and designed the study. Mohamed Ali Daw, Abdallah Hussean El-Bouzedi, Mohamed Omar Ahmed and Ali Ali Alejenef participated in the conduct of the study and reviewed the manuscript. All authors read and approved the final version of the manuscript.
We are deeply grateful to the Department of Medical Microbiology and Immunology for their support and courage. Special thanks go to Mr. Ibrahem M Daw, Department of Computer Engineering, Faculty of Engineering, for his great efforts in mapping the results.
Table 1: demographic features of the patients infected with COVID-19 in Libya
Figure 1: map of Libya showing the geographic area controlled by each fighting group during the emergence of COVID-19
Figure 2: geographic distribution of the reported cases of COVID-19 in Libya
Figure 3: A) the graph shows the data of the number of confirmed cases in Libya between March 25th and June 25 th 2020; B) the cumulative number of COVID-19 cases in each Libyan region during the study period; the number of daily increased confirmed COVID-19 cases in each region
- Hartley DM, Perencevich EN. Public health interventions for COVID-19: emerging evidence and implications for an evolving public health crisis. JAMA. 2020 May 19;323(19):1908-9. PubMed | Google Scholar
- Lewnard JA, Lo NC. Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet Infect Dis. 2020 Jun;20(6):631-633. PubMed | Google Scholar
- Yancy CW. COVID-19 and African Americans. JAMA. 2020 May 19;323(19):1891-1892. PubMed | Google Scholar
- Onder G, Rezza G, Brusaferro S. Case-fatality rate and characteristics of patients dying in relation to COVID-19 in Italy. JAMA. 2020 May 12;323(18):1775-6. PubMed | Google Scholar
- Legido-Quigley H, Mateos-García JT, Campos VR, Gea-Sánchez M, Muntaner C, McKee M. The resilience of the Spanish health system against the COVID-19 pandemic. The lancet public health. 2020 May 1;5(5):e251-2. PubMed | Google Scholar
- Mehtar S, Preiser W, Lakhe NA, Bousso A, TamFum JJ, Kallay O et al. Limiting the spread of COVID-19 in Africa:one size mitigation strategies do not fit all countries. The Lancet Global Health. 2020 Apr 28. PubMed | Google Scholar
- Tadesse DB, Gebremeskel GG, Asefa GG, Abay M, Demoz GT. The burden, admission, and outcome of COVID-19 in Africa: protocol for a systematic review and meta-analysis. Emerg Microbes Infect. 2020 Dec;9(1):1372-1378. PubMed | Google Scholar
- Gostin LO, Kavanagh MM, Cameron E. Ebola and war in the Democratic Republic of Congo: avoiding failure and thinking ahead. JAMA. 2019 Jan 22;321(3):243-4. PubMed | Google Scholar
- Nachega JB, Mbala-Kingebeni P, Otshudiema J, Mobula LM, Preiser W, Kallay O et al. Responding to the Challenge of the Dual COVID-19 and Ebola Epidemics in the Democratic Republic of Congo-Priorities for Achieving Control. Am J Trop Med Hyg. 2020 Jun 19. PubMed | Google Scholar
- Daw MA, El-Bouzedi A, Dau AA. Libyan armed conflict 2011: mortality, injury and population displacement. Afr J Emerg Med. 2015 Sep 1;5(3):101-7. Google Scholar
- Daw MA, El-Bouzedi AH, Dau AA. Trends and patterns of deaths, injuries and intentional disabilities within the Libyan armed conflict: 2012-2017. PloS one. 2019 May 10;14(5):e0216061. PubMed | Google Scholar
- Daw MA. Corona virus infection in Syria, Libya and Yemen; an alarming devastating threat. Trav Med Infect Dis. 2020 Apr 2;101652. PubMed | Google Scholar
- Elhadi M, Msherghi A, Alkeelani M, Alsuyihili A, Khaled A, Buzreg A et al. Concerns for low-resource countries, with under-prepared intensive care units, facing the COVID-19 pandemic. Infect Dis Health. 2020 Jun 5. pii: S2468-0451(20)30035-3. PubMed | Google Scholar
- Letendre K, Fincher CL, Thornhill R. Does infectious disease cause global variation in the frequency of intrastate armed conflict and civil war? Biol Rev CambPhilosSoc. 2010 Aug;85(3):669-83. PubMed | Google Scholar
- Sartin JS. Infectious diseases during the Civil War: the triumph of the “Third Army”. Clinical Infectious Diseases.Clin Infect Dis. 1993 Apr;16(4):580-4. PubMed | Google Scholar
- Daw MA, El-Bouzedi AH. Trends and projection of demographic indices of the Libyan population using a fifty-year census data 1954-20 African Population Studies. 2019 Aug 6;33(2). Google Scholar
- World Health Organization. Laboratory testing for coronavirus disease 2019 (COVID-19) in suspected human cases: interim guidance, 2 March 2020. Accessed on 4thApril 2020.
- Corman VM, Landt O, Kaiser M, Molenkamp R, Meijer A, Chu DK et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill. 2020;25(3):2000045. PubMed | Google Scholar
- Daw MA, Daw AM, Sifennasr NE, Draha A, Daw A, Daw A et al. The epidemiological characterization and geographic distribution of Hepatitis D virus infection in Libya. Pan Afr Med J. 2020 Apr 14;35:120. PubMed | Google Scholar
- Daw MA, Ali LA, Daw AM, Sifennasr NE, Dau AA, Agnan MM et al. The geographic variation and spatiotemporal distribution of hepatitis C virus infection in Libya: 2007-2016. BMC Infect Dis. 2018 Nov 22;18(1):594. PubMed | Google Scholar
- Daw MA, Daw AM, Sifennasr NE, Draha AM, Daw AA, Daw AA et al. Spatiotemporal analysis and epidemiological characterization of the human immunodeficiency virus (HIV) in Libya within a twenty five year period: 1993-2017. AIDS Res Ther. 2019 Jun 25;16(1):1-14. PubMed | Google Scholar
- Daw MA. Libyan healthcare system during the armed conflict: Challenges and restoration. Afr J Emerg Med. 2017 Jun;7(2):47-50. PubMed | Google Scholar
- Daw MA, El-Bouzedi A, Dau AA. The assessment of efficiency and coordination within the Libyan health care system during the armed conflict-2011. Clin Epidemiol Glob Health. 2016 Sep 1;4(3):120-7. Google Scholar
- Daw MA, El-Bouzedi AH. Modelling the epidemic spread of COVID-19 virus infection in Northern African countries. Travel Med Infect Dis. 2020 May - Jun;35:101671. PubMed | Google Scholar
- Daw MA. Preliminary epidemiological analysis of suspected cases of corona virus infection in Libya. Travel Med Infect Dis. 2020 May-Jun;35:101634. PubMed | Google Scholar
- Kang D, Choi H, Kim JH, Choi J. Spatial epidemic dynamics of the COVID-19 outbreak in China. Int J Infect Dis. 2020 May;94:96-102. PubMed | Google Scholar
- La Maestra S, Abbondandolo A, De Flora S. Epidemiological trends of COVID?19 epidemic in Italy over March 2020: From 1000 to 100 000 cases. J Med Virol. 2020 Apr 21;10.1002/jmv.25908. PubMed | Google Scholar
- Matua GA, Van der Wal DM, Locsin RC. Ebola hemorrhagic fever outbreaks: strategies for effective epidemic management, containment and control. The Brazilian Journal of Infectious Diseases. 2015 May 1;19(3):308-13. PubMed | Google Scholar
- Gayer M, Legros D, Formenty P, Connolly MA. Conflict and emerging infectious diseases. Emerg Infect Dis. 2007 Nov;13(11):1625-31. PubMed | Google Scholar
- Hay SI, Battle KE, Pigott DM, Smith DL, Moyes CL, Bhatt S et al. Global mapping of infectious disease. Philos Trans R Soc Lond B Biol Sci. 2013 Feb 4;368(1614):20120250. PubMed | Google Scholar
- World Health Organization. WHO interim guidance note: health system response to COVID-19 in the context of internally displaced persons, refugees, migrants and returnees in the Eastern Mediterranean Region: 7 April 2020. World Health Organization. Regional Office for the Eastern Mediterranean; 2020. Google Scholar
- Chen D, Xu W, Lei Z, Huang Z, Liu J, Gao Z et al. Recurrence of positive SARS-CoV-2 RNA in COVID-19: a case report. Int J Infect Dis. 2020;93:297-9. PubMed | Google Scholar
- Gostin LO, Abubakar I, Guerra R, Rashid SF, Friedman EA, Jakab Z. WHO takes action to promote the health of refugees and migrants. Lancet. 2019 May 18;393(10185):2016-2018. PubMed | Google Scholar