Determinants of adherence to clinic appointments among tuberculosis and HIV co-infected individuals attending care at Helen Joseph Hospital, Johannesburg, South Africa
Ruvimbo Barbara Claire Nhandara, Birhanu Teshome Ayele, Lovemore Nyasha Sigwadhi, Lovelyn Uzoma Ozougwu, Peter Suwirakwenda Nyasulu
Corresponding author: Peter Suwirakwenda Nyasulu, Division of Epidemiology and Biostatistics, Faculty of Medicine and Health Sciences, Stellenbosch University, Cape Town, South Africa 
Received: 14 May 2020 - Accepted: 23 Jul 2020 - Published: 05 Oct 2020
Domain: Infectious diseases epidemiology
Keywords: Adherence, tuberculosis, HIV/AIDS, co-infection, Johannesburg, South Africa, treatment duration, Helen Joseph Hospital, clinic appointments
©Ruvimbo Barbara Claire Nhandara et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ruvimbo Barbara Claire Nhandara et al. Determinants of adherence to clinic appointments among tuberculosis and HIV co-infected individuals attending care at Helen Joseph Hospital, Johannesburg, South Africa. Pan African Medical Journal. 2020;37:118. [doi: 10.11604/pamj.2020.37.118.23523]
Available online at: https://www.panafrican-med-journal.com//content/article/37/118/full
Research 
Determinants of adherence to clinic appointments among tuberculosis and HIV co-infected individuals attending care at Helen Joseph Hospital, Johannesburg, South Africa
Determinants of adherence to clinic appointments among tuberculosis and HIV co-infected individuals attending care at Helen Joseph Hospital, Johannesburg, South Africa
Ruvimbo Barbara Claire Nhandara1, Birhanu Teshome Ayele1, Lovemore Nyasha Sigwadhi1, Lovelyn Uzoma Ozougwu1, Peter Suwirakwenda Nyasulu1,2,&
&Corresponding author
Introduction: Tuberculosis (TB) is one of the leading causes of morbidity and mortality among people living with HIV/AIDS. The growing burden of TB/HIV co-infection continues to strain the healthcare system due to association with long duration of treatment. This is a catalyst for poor adherence to clinic appointments, which results in poor treatment adherence and patient outcome. This study evaluated the factors associated with adherence to clinic appointments among TB/HIV co-infected patients in Johannesburg, South Africa.
Methods: this was a cross-sectional study that involved 10427 patients ≥18 years of age with HIV infection and co-infected with TB. We used a proxy measure 'md clinic appointments´ to assess adherence, then multivariable logistic regression to evaluate factors associated with adherence.
Results: one thousand, five hundred and twenty eight patients were co-infected with TB, of these 17.4% attained good adherence. Patients with TB/HIV co-infection who were on treatment for a longer period were less likely to adhere to clinic appointments (AOR: 0.98 95% CI: 0.97, 0.99).
Conclusion: duration on treatment among TB/HIV co-infected patients is associated with adherence to clinic appointments. It is therefore vital to reinforce public health interventions that would enhance sustained adherence to clinic appointments and mitigate its impact on treatment adherence and patient outcome.
Tuberculosis (TB) remains a major public health challenge, which has been compounded over the past four decades by the Human Immunodeficiency Virus (HIV) epidemic [1]. As the prevalence of HIV continues to increase, the proportion of individuals in the population with compromised immune system also increased leading to an increase in TB cases [1]. In 2014, TB was the leading infectious cause of death [2] and the most common opportunistic infection among people living with HIV infection (PLWH) [3-5]. Notwithstanding, TB has been over-diagnosed in PLWH due to its close similarity in clinical presentation with other pathogens such as Pneumocystis jirovecii and Norcadia [6]. In the presence of a weakened immune system, Mycobacterium tuberculosis progressively multiplies and causes TB. As such, an individual with TB/HIV co-infection has a higher likelihood of developing active TB [7,8]. The TB/HIV co-infection has significantly increased the burden of infectious diseases worldwide [3].
In 2017, an estimated 10 million people developed active TB of whom 9% were PLWH. The World Health Organization estimates that one third of the estimated 36.9 million PLWH were co-infected with TB. An estimated 1.3 million people died of TB with approximately 300,000 TB related deaths occurring among PLWH [9,10]. This has overstretched the healthcare system due to association with lengthy treatment regimen that prolongs treatment duration. Such a scenario is a precipitating factor for poor treatment adherence, which is a major public health challenge due to its propensity to drive anti-tuberculous drug resistance. This is so because missing scheduled clinic appointments among patients with dual infections is a catalyst for poor treatment adherence and patient outcomes [4,11-13]. This therapeutic challenge has often led to treatment interruption for both HIV/AIDS and TB medication leading to prolonged duration on treatment and occurrences of drug resistance [6,14].
South Africa is among the world´s most affected with TB/HIV co-infection contributing to an estimated 20% of the global burden of TB/HIV co-infections [15]. This has created a scenario where a large proportion of TB/HIV co-infected individuals in South Africa require concurrent treatment for TB and HIV/AIDS [16]. The dual infection has had a compounding effect on sustaining treatment adherence among affected patients. It is common knowledge that where TB treatment adherence is maximally achieved, TB is usually completely cured [17]. The same applies to HIV infection where viral suppression is achieved and sustained with acceptable level of adherence to Antiretroviral Therapy (ART). This fundamental paradigm shift in medication adherence would have a resultant effect in reduction of HIV transmission and would prolong and improve the quality of life of those infected [18,19]. Despite the advances in treatment availability and accessibility, TB/HIV co-infection has remained a compounded public health challenge [20] requiring innovative approach specifically in South Africa, a high burden country. Therefore, assessing the determinants of adherence to clinic appointments among TB/HIV infected patients is critical to help identify effective health system interventions that could be used to support individuals taking both TB medication and ART for improved treatment outcomes.
Study design: the study used a retrospective record review of patients with TB/HIV co-infection to access data on adherence to ART/TB clinic appointments.
Study site: this study was conducted at Themba Lethu Clinic in October 2016. The clinic is located at Helen Joseph Hospital, Westdene, in Johannesburg metropolitan area. It provides HIV/AIDS and TB related treatment, care and support services.
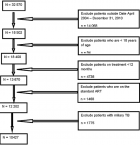
Sampling and sample size: Themba Lethu Clinic had a total population of 32,570 registered patients that were followed up from April 2004 to April 2010. Patients aged ≥18 years, HIV positive, with a TB diagnosis, ART naïve at the time of registration, on standard first line ART, who were within a minimum of 12 months´ follow-up and had initiated treatment between April 2004 and April 2010, were included. Patients with extra-pulmonary TB were excluded from the study. A total of 10,427 individuals met the inclusion criteria, of which 6,781 (65%) were females and 3,646 (35%) were males (Figure 1).
Data collection: data were extracted from ´therapy edge´ database that houses HIV patients´ treatment records at Themba Lethu Clinic. The following variables were extracted: age, sex, education, employment status, alcohol consumption, smoking status, TB co-infection at baseline, baseline CD4 count, haemoglobin level, WHO baseline, BMI, months on individual treatment and months on treatment by co-infection among patients with TB/HIV coinfection.
Variable measurements: adherence was measured by assessing the number of missed clinic appointments. It was categorised into two groups “good adherence”, those who attained greater than 90% of appointment visits and “poor adherence”, those who achieved less than 90% of scheduled clinic appointments [19,20]. The exposure variables were: demographic (sex, age, marital status); socio-economic (source of income, educational level); laboratory (AAFB test, CD4 count); clinical (other opportunistic infections and duration on HIV treatment).
Data management and statistical analysis: data were exported into Stata version 15 (Stata Corp, College Station, TX, USA). Data were checked for errors, outliers and completeness. Frequencies and percentages were used to describe categorical variables while median and inter-quartile ranges (IQR) were used to summarise continuous variables while assuming non-normality. Pearson´s Chi-square test of independence was used to assess presence or otherwise of any significant relationship between exposure variables and outcome variable "level of adherence". Backward elimination model selection method using p<0.10 as a determinant of significant variables was applied. Variables known apriori to be associated with adherence and those with p<0.10 in bivariate analysis were included in the multivariable logistic regression model to determine factors associated with adherence to clinic appointments. Hosmer and Lemeshow test was used to assess the model´s goodness of fit. All variables with p<0.05 in the multivariable analysis, were considered to be statistically significant.
As depicted in Table 1, there were 10,427 participants that were involved in this study. Of these, 1,559 (15%) showed good adherence to clinic appointments while 8,868 (85%) adhered poorly. Participants who were co-infected showed poor adherence to clinic appointments 14.2% (p<0.001) with median month on treatment of 39.4 (23.8-60.4). Adherence to clinic appointments decreased with increasing age of the individuals (from 49% in the age group 35-50 to 8.7% in 50+ years), however, this was not statistically significant (p=0.07). Those who were employed had poor level of adherence to clinic appointments, whilst smokers and former smokers had a good level of adherence. There was a significant association between adherence to clinic appointments and WHO stage of HIV diseases at baseline (p<0.001). Adherence to clinic appointments decreased as HIV disease progressed. Individuals with haemoglobin level >11mg/dl adhered more compared to individuals with haemoglobin concentration of <11mg/dl. On univariate analysis, we found that there was a significant association between (being co-infected at baseline, history of alcohol consumption, employment status, history of smoking, haemoglobin level, WHO stage 2, BMI <18, months on treatment, months on treatment by co-infection) and adherence to clinic appointments (Table 2).
Individuals co-infected at baseline were less likely to adhere to clinic appointments compared to those who were not co-infected at baseline (OR: 0.78, 95% CI: 0.68-0.91). There was also an association between duration in months on treatment and adherence to scheduled clinic appointments among co-infected patients (OR: 0.97, 95%CI: 0.97-0.98). This shows that adherence to clinic appointments decreased by 2% for every single month that the patient stayed on treatment. On multivariable logistic regression factors associated with adherence to clinic appointments were 'alcohol consumption, age group, employment, baseline CD4 count, months on treatment and months on treatment by co-infection'. Patients co-infected with TB had 21% reduced odds of adherence to clinic appointments compared with patients living with HIV only (AOR: 0.79, 95% CI: 0.68, 0.91). Those who consumed alcohol were 19% less likely to adhere to clinic appointments compared with the non-alcoholics (AOR: 0.81, 95% CI: 0.68, 0.97).
Patients with a previous history of alcohol consumption were approximately 1.3 times more likely to adhere to clinic appointments than patients who were using alcohol (AOR: 1.29, 95% CI: 1.02, 1.62). The odds of adherence to clinic appointments were higher among patients aged 35-50 years compared with patients who were ≥50 years of age (AOR: 1.29, 95% CI: 1.04, 1.59). Patients with employment were less likely to adhere to clinic appointments compared with patients who were unemployed (AOR: 0.61, 95% CI: 0.55, 0.69). Furthermore, patients with much lower immune status as evidenced by a CD4 count of less than 350cell/ml3 had increased odds of good adherence to clinic appointments (AOR: 1.48 95% CI: 1.20, 1.82). This is a demonstration of a willpower to recover. In addition, patients who were on treatment for a longer period had decreased odds of adherence to clinic appointments compared with patients who had been on treatment for a shorter period.
This study evaluated determinants of adherence to clinic appointments among patients with TB/HIV co-infection. We found that the longer a patient was on treatment the lower the likelihood of adhering to clinic appointments (AOR: 0.98, 95% CI: 0.97, 0.98). This is essential as it provides a platform for continued adherence counselling among patients on treatment specifically those who have been on treatment for a lengthy period. Our findings are similar to other studies that showed long term treatment compromised patients´ will to keep up with scheduled clinic appointments [21-23]. Missed appointments are a catalyst for poor treatment adherence because patients would have no pills as they missed their pill collection time [13,24,25]. Thus, it would be a catalyst to poor treatment outcomes as their attending physician would be unaware of any ailments the patient could be having as they missed their review date. Proper follow up for clinical assessment as scheduled is an important component of the patient´s rigorous assessment to ascertain if the patients have no underlying illness requiring a different type of medication. Furthermore, patients are assessed on any side effect they might be having, to warrant treatment discontinuation or change of treatment regimen to a different type. All these are best carried out if patients maintained their regular follow up visits as scheduled [5,26]. However, a study of two regional cohorts: sub-Saharan Africa and Asia reported different findings. The longer a patient was on ART, the higher the chances of good adherence. This could have been due to patients´ self-reported adherence being high [27].
Overall, HIV/TB co-infected patients had poor adherence to clinic appointments. A study conducted in South Africa reported similar findings [28]. The reasons for this could be patient related such as high pill burden, adverse reactions and fear of not being able to tolerate both ART and anti-tuberculosis medication [19,28-30]. The site of the TB infection was also associated with adherence. Patients with pulmonary TB were less likely to adhere to clinic visits compared with those with extra pulmonary TB [28]. Our study found that patients who consume alcohol have poor adherence. Similar findings were reported where consumption of alcohol resulted in missed clinic visits and in turn poor medication adherence [5,31]. Shumba et al. analysed factors associated with missing ART doses and noted that missing clinic appointments was linked to missing doses [32]. Alcohol consumption may cause cognitive impairment which could result in patients failing to make it for their clinic appointments or forget to take their pills, leading to poor adherence [21,32,33]. Patients with a history of alcohol consumption had good adherence than those who did not consume alcohol. Research conducted in Thailand reported good adherence in former drinkers as well and concluded that the good adherence among former drinkers could possibly be due to patients following the health care workers guidelines on lowering or stopping alcohol consumption to improve treatment outcome [33].
Patients 35-50 years of age had good adherence compared with those aged 50 years and older. Financial constraints could have been a potential reason for the older individuals missing their clinic appointments as noted by another study conducted in South Africa [24]. Patients with employment history adhered poorly compared with the unemployed. This is different from another study that noted employment as having a positive influence on attendance to scheduled clinic visits. Being employed offered individuals financial means to visit the clinic [34]. Our results could be different due to missing data as employment status was not available for all participants. Patients with low clinical values of CD4 count <350 had nearly 1.5 times the odds of good adherence (AOR: 1.48 95% CI: 1.20, 1.82). This could have been due to a clear understanding of the risk associated with low CD4 in HIV infection. This is however in contrast with a study conducted in America which noted that individuals that were very ill were possibly less mobile and thus miss the scheduled clinic visit [35]. Another possible reason for our findings could be that patients with clinically normal values felt healthier and thus less inclined to take their medication [36].
Duration on treatment had a negative influence on adherence to clinic appointments among HIV/TB co-infected patients in this study. Long term treatment appears to compromise an individual´s will to keep up with scheduled clinic appointments. This is problematic among patients with TB/HIV co-infection as missing appointments can result in poor treatment adherence and in turn poor outcomes.
What is known about this topic
- Tuberculosis remains the leading opportunistic infection among HIV infected individuals thus the continued rampage of TB/HIV co-infection;
- Adherence to TB/HIV co-infection is still a challenge despite the advances in accessibility of ART;
- Good adherence among TB/HIV co-infected individuals results in a reduction of new HIV cases, decreases occurrences of drug resistance and improves the individuals´ quality of life.
What this study adds
- Adherence to ART was poor in this study: the longer a patient stayed on treatment, adherence became poor whereas previous studies reported good adherence overtime;
- Factors that influenced adherence negatively among the TB/HIV co-infected patients included 'co-infection at baseline, alcohol consumption, employment status, baseline CD4 count, months on treatment and months on treatment by co-infection';
- Further research needs to be conducted regarding duration on treatment as a negative influence on adherence.
The authors declare no competing interests.
RN and PN conceived and designed the study; RN, BA and PN analysed and interpreted the data; RN, LO and PN drafted the manuscript; RN, BA, LO, LS and PN reviewed the manuscript for critical intellectual content and approved final revision. All the authors have read and agreed to the final manuscript.
The authors would like to acknowledge Dr. Samson Muyanga for his input in editing the manuscript and ´Right to Care´ for the provision of dataset.
Table 1: summary of baseline characteristics of patients by adherence to clinic appointments
Table 2: univariable and multivariable analysis of factors associated with adherence
Figure 1: flow diagram showing number included in the final analysis
- Mulongeni P, Hermans S, Caldwell J, Bekker L-G, Wood R, Kaplan R. HIV prevalence and determinants of loss-to-follow-up in adolescents and young adults with tuberculosis in Cape Town. PLoS One. 2019 Feb 5;14(2):e0210937. PubMed | Google Scholar
- Pathmanathan I, Pasipamire M, Pals S, Dokubo EK, Preko P, Ao T et al. High uptake of antiretroviral therapy among HIV-positive TB patients receiving co-located services in Swaziland. PLoS One. 2018 May 16;13(5):e0196831. PubMed | Google Scholar
- Adeiza MA, Abba AA, Okpapi JU. HIV-associated tuberculosis: a sub-Saharan African perspective. Sub-Sahar Afr J Med. 2014;1(1):1-14. Google Scholar
- Manosuthi W, Wiboonchutikul S, Sungkanuparph S. Integrated therapy for HIV and tuberculosis. AIDS Res Ther. 2016 Dec;13:22. PubMed | Google Scholar
- Naidoo K, Dookie N, Naidoo K, Yende-Zuma N, Chimukangara B, Bhushan A et al. Recurrent tuberculosis among HIV-coinfected patients: a case series from KwaZulu-Natal. Infect Drug Resist. 2018 Sep;11:1413-21. PubMed | Google Scholar
- Narendran G, Swaminathan S. TB-HIV co-infection: a catastrophic comradeship. Oral Dis. 2016 Apr;22 Suppl 1:46-52. PubMed | Google Scholar
- Shankar EM, Vignesh R, Ellegard R, Barathan M, Chong YK, Bador MK et al. HIV-mycobacterium tuberculosis co-infection: a 'danger-couple model' of disease pathogenesis. Pathog Dis. 2014 Mar;70(2):110-8. PubMed | Google Scholar
- Yusria A, Rintiswati N, Sumardi S. Factors associated with tuberculosis treatment success among Human Immunodeficiency Virus-Tuberculosis (HIV-TB) in H Adam Malik General Hospital, Medan. J Trop Med. 2017;4(1):9. Google Scholar
- World Health Organization. HIV-associated Tuberculosis. World Health Organization. 2018.
- World Health Organization. Global Tuberculosis report 2019. World Health Organization. 2019.
- Rossetto M, Brand ÉM, Rodrigues RM, Serrant L, Teixeira LB. Factors associated with hospitalization and death among TB/HIV co-infected persons in Porto Alegre, Brazil. PLoS One. 2019 Jan 2;14(1):e0209174. PubMed | Google Scholar
- Sinshaw Y, Alemu S, Fekadu A, Gizachew M. Successful TB treatment outcome and its associated factors among TB/HIV co-infected patients attending Gondar University Referral Hospital, Northwest Ethiopia: an institution based cross-sectional study. BMC Infect Dis. 2017 Dec;17(1):132. PubMed | Google Scholar
- Kimeu M, Burmen B, Audi B, Adega A, Owuor K, Arodi S et al. The relationship between adherence to clinic appointments and year-one mortality for newly enrolled HIV infected patients at a regional referral hospital in Western Kenya, January 2011-December 2012. AIDS care. 2016 Apr 2;28(4):409-15. PubMed | Google Scholar
- Abdool Karim SS, Naidoo K, Grobler A, Padayatchi N, Baxter C, Gray AL et al. Integration of antiretroviral therapy with Tuberculosis treatment. N Engl J Med. 2011 Oct 20;365(16):1492-501. PubMed | Google Scholar
- Shamu S, Kuwanda L, Farirai T, Guloba G, Slabbert J, Nkhwashu N. Study on knowledge about associated factors of Tuberculosis (TB) and TB/HIV co-infection among young adults in two districts of South Africa. PLoS One. 2019 Jun 6;14(6):e0217836. PubMed | Google Scholar
- Mazinyo EW, Kim L, Masuku S, Lancaster JL, Odendaal R, Uys M et al. Adherence to concurrent Tuberculosis treatment and antiretroviral treatment among co-infected persons in South Africa, 2008-2010. PLoS One. 2016 Jul 21;11(7):e0159317. PubMed | Google Scholar
- Akanbi K, Ajayi I, Fayemiwo S, Gidado S, Oladimeji A, Nsubuga P. Predictors of tuberculosis treatment success among HIV-TB co-infected patients attending major tuberculosis treatment sites in Abeokuta, Ogun State, Nigeria. Pan African Medical Journal. 2019 Jan 22;32(Suppl 1):7. PubMed | Google Scholar
- Altice F, Evuarherhe O, Shina S, Carter G, Beaubrun AC. Adherence to HIV treatment regimens: systematic literature review and meta-analysis. Patient Prefer Adher. 2019 Apr;13:475-90. PubMed | Google Scholar
- Zhu Y, Wu J, Feng X, Chen H, Lu H, Chen L et al. Patient characteristics and perceived health status of individuals with HIV and tuberculosis coinfection in Guangxi, China. Medicine (Baltimore). 2017 Apr;96(14):e6475. PubMed | Google Scholar
- Schechter MC, Bizune D, Kagei M, Holland DP, Del Rio C, Yamin A et al. Challenges across the HIV care continuum for patients with HIV/TB co-infection in Atlanta, GA. Open forum Infect Dis. 2018 Apr 1;5(4):ofy063. PubMed | Google Scholar
- Heestermans T, Browne JL, Aitken SC, Vervoort SC, Klipstein-Grobusch K. Determinants of adherence to antiretroviral therapy among HIV-positive adults in sub-Saharan Africa: a systematic review. BMJ Glob Health. 2016 Dec 1;1(4):e000125. PubMed | Google Scholar
- Mugavero MJ, Lin HY, Willig JH, Westfall AO, Ulett KB, Routman JS et al. Missed visits and mortality among patients establishing initial outpatient HIV treatment. Clin Infect Dis. 2009 Jan 15;48(2):248-56. PubMed | Google Scholar
- Mugavero MJ, Westfall AO, Cole SR, Geng EH, Crane HM, Kitahata MM et al. Beyond core indicators of retention in HIV care: missed clinic visits are independently associated with all-cause mortality. Clin Infect Dis. 2014 Nov 15;59(10):1471-9. PubMed | Google Scholar
- Barry A, Ford N, El-Khatib Z. Factors for incomplete adherence to antiretroviral therapy including drug refill and clinic visits among older adults living with human immunodeficiency virus-cross: sectional study in South Africa. Trop Med Int Health. 2018;23(3):270-8. PubMed | Google Scholar
- Tweya H, Oboho IK, Gugsa ST, Phiri S, Rambiki E, Banda R et al. Loss to follow-up before and after initiation of antiretroviral therapy in HIV facilities in Lilongwe, Malawi. PloS One. 2018;13(1):e0188488. PubMed | Google Scholar
- Lemos LD, Fiuza ML, Reis RK, Ferrer AC, Gir E, Galvao MT. Adherence to antiretrovirals in people coinfected with the human immunodeficiency virus and tuberculosis. Rev Lat Am Enfermagem. 2016;24:e2691. PubMed | Google Scholar
- Bijker R, Jiamsakul A, Kityo C, Kiertiburanakul S, Siwale M, Phanuphak P et al. Adherence to antiretroviral therapy for HIV in sub-Saharan Africa and Asia: a comparative analysis of two regional cohorts. J Int Aids Soc. 2017;20(1):21218. PubMed | Google Scholar
- Gajee R, Schnippel K, Mthupha N, Muzah B, Berhanu RH. Missed appointments among rifampicin-resistant tuberculosis (RR-TB) patients at a decentralised RRTB outpatient clinic in Johannesburg, South Africa. SAMJ. 2016;106(9):912-7. PubMed | Google Scholar
- Ghatage S, Anurupa MS, Aithal SS, Shubha DB, Angadi N. A study on reasons for nonadherence to 99DOTS among HIV-tuberculosis coinfected patients in Davanagere district, Karnataka. Int J Med Sci Public Health. 2018;7(11):805. Google Scholar
- Kigozi G, Heunis C, Chikobvu P, Botha S, van Rensburg D. Factors influencing treatment default among tuberculosis patients in a high burden province of South Africa. Int J Infect Dis. 2017 Jan;54:95-102. PubMed | Google Scholar
- Nagata D, Gutierrez EB. Characteristics of HIV patients who missed their scheduled appointments. Rev Saude Publ. 2015 Dec 31;49:95. PubMed | Google Scholar
- Shumba C, Atuhaire L, Imakit R, Atukunda R, Memiah P. Missed doses and missed appointments: adherence to ART among adult patients in Uganda. ISRN AIDS. 2013 Jan 14;2013:270914. PubMed | Google Scholar
- Laprawat S, Peltzer K, Pansila W, Tansakul C. Alcohol use disorder and tuberculosis treatment: a longitudinal mixed method study in Thailand. South Afr J Psychiatry. 2017 May 30;23:1074. PubMed | Google Scholar
- Nijhawan AE, Liang Y, Vysyaraju K, Muñoz J, Ketchum N, Saber J et al. Missed initial medical visits: predictors, timing and implications for retention in HIV care. AIDS Patient Care STDs. 2017 May 1;31(5):213-21. PubMed | Google Scholar
- Horberg MA, Hurley LB, Silverberg MJ, Klein DB, Quesenberry CP, Mugavero MJ. Missed office visits and risk of mortality among HIV-infected subjects in a large healthcare system in the United States. AIDS Patient Care STDs. 2013 Aug 1;27(8):442-9. PubMed | Google Scholar
- Semvua SK, Orrell C, Mmbaga BT, Semvua HH, Bartlett JA, Boulle AA. Predictors of non-adherence to antiretroviral therapy among HIV infected patients in northern Tanzania. PLoS One. 2017 Dec 18;12(12):e0189460. PubMed | Google Scholar