Schwannoma of the descending loop of the hypoglossal nerve: case report
Nadia M´jahad, Mohamed Ridal, Houda Chafai, Amal Douida, Hammas Naoual, Aamal Akamar, Mustapha Maaroufi, Mohamed Nourredine El Alami
Corresponding author: Nadia M´jahad, Department of Otorhinolaryngology (ENT) and Head - Neck Surgery, Hassan II University Hospital, Fez, Morocco 
Received: 13 May 2020 - Accepted: 21 May 2020 - Published: 08 Jun 2020
Domain: Otolaryngology (ENT)
Keywords: Schwannoma, hypoglossal nerve, descending loop
©Nadia M´jahad et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nadia M´jahad et al. Schwannoma of the descending loop of the hypoglossal nerve: case report. Pan African Medical Journal. 2020;36:73. [doi: 10.11604/pamj.2020.36.73.23500]
Available online at: https://www.panafrican-med-journal.com//content/article/36/73/full
Schwannoma of the descending loop of the hypoglossal nerve: case report
Nadia M´jahad1, 2, &, Mohamed Ridal1, 2, 3, Houda Chafai1, 2, Amal Douida1, 4, Hammas Naoual1, 4, Aamal Akamar1, 5, Mustapha Maaroufi1, 5, Mohamed Nourredine EL Alami1, 2, 3
1Faculty of Medicine and Pharmacy, Sidi Mohammed Benabdellah University, Fez, Morocco, 2Department of Otorhinolaryngology (ENT) and Head - Neck Surgery, Hassan II University Hospital, Fez, Morocco, 3Faculty of Medicine and Pharmacy, "Anatomy, Surgery and Anesthesiology" laboratory Sidi Mohammed Benabdellah University, Fez, Morocco, 4Department of Pathology, Hassan II University Hospital, Fez, Morocco, 5Department of Radiology, Hassan II University Hospital, Fez, Morocco
&Corresponding author
Nadia M´jahad, Department of Otorhinolaryngology (ENT) and Head - Neck Surgery, Hassan II University Hospital, Fez, Morocco
Schwannomas of the descending loop of the hypoglossal nerve are very rare. Existing literature of the schwannoma of the descending loop of the hypoglossal nerve is limited to two previously reported case. They are slow-growing tumors that may masquerade a carotid body tumor. We herein described a rare case of schwannoma of the descending loop of the hypoglossal nerve in the s rigth latero-cervical region with diagnostic imaging and histopathological findings. A 37-years-old woman has had a palpable firm, mobile mass in the right latero-cervical region, of imaging, MR images showed homogeneous hypointensity on T1-weighted imaging (T1-WI), heterogeneous hyperintensity on T2-WI, and heterogeneous enhancement on contrast-enhanced T1-WI. Diagnostic imaging using computed tomography (CT) and magnetic resonance imaging (MRI) was suspected of Chemodectoma or neurogenic tumor. At operation, a 4 cm mass arising from the descending loop of the hypoglossal nerve of was resected en bloc with the loop itself; Final diagnosis was confirmed on the basis of histopathological finding and intraoperative findings. Postoperative course was uneventful and the patient is free from disease recurrence at tree-year follow-up. En bloc resection remains the real curative treatment of Schwannomas, ensuring unlimited freedom from disease, although causing functional impairment which may be significant. Nonetheless recurrence should be prevented as, besides requiring reintervention, it may harbor a malignant evolution towards sarcoma. Schwannomas of the descending loop of the hypoglossal nerve may masquerade a chemodectoma of the carotid bifurcation and can be curatively resected without any functional impairment. This case confirmed the differential diagnosis on the basis of the intraoperative finding that the tumor was continuous with the hypoglossal nerve.
Schwannomas are benign, slow-growing tumors of the neural sheath, which may affect cranial, sympathetic and peripheral nerves [1-5]. Approximately 25 to 45% of extracranial schwannomas occur in the head and neck [4, 6], most likely around the glossopharyngeal space and the carotid artery sheath . Although occurrence in other sites is relatively rare, it has been reported to occur in the parotid gland, nose, paranasal sinuses, and the oral cavity [7- 9]; whereas schwannomas arising from the descending loop of the hypoglossal nerve are extremely rare [1, 10, 11]. In the present report, we described a case of schwannoma arising from the descending loop of the hypoglossal nerve in the right submandibular region with imaging and histopathological findings, masquerading a tumor of the carotid body.
A 37-year-old woman was referred for a non-tender, laterocervical mass enlarging within a month, without pain, dysphagia, dysarthria or any other symptom. At physical examination revealed a palpable firm, freely mobile mass measuring about 4 cm diameter, was not pulsating. Overlying skin was normal and no deviation, fasciculation or hemiatrophy of the tongue upon protrusion was observed. No lymph nodes were palpable. At cervical ultrasound examination (US), it appeared solid, heterogeneous and located between the internal (ICA) and external (ECA) carotid arteries, with normal flow velocities in both of them. Non-contrast CT revealed a well-circumscribed spherical 4, 8x3, 8x3, 2 cm mass with heterogeneous density in the right laterocervical region. Contrast-enhanced CT demonstrated inhomogeneous weak enhancement, and intratumoral blood vessels were strong enhancement. No evidence of cystic or necrotic degeneration was present in the CT (Figure 1). One weeks later, the patient underwent MR images, MR images showed homogeneous hypointensity on T1-weighted imaging (T1-WI), heterogeneous hyperintensity on T2-WI, and heterogeneous enhancement on contrast-enhanced T1-WI. With normal flow velocities in the internal and external carotid arteries (Figure 2), the lesion was suspected of neurogenic tumor on the basis of the above imaging findings. A fine needle aspiration biopsy was not performed, due to the risk of inadvertent arterial puncture and the sufficiently clear imaging indicating surgical excision in any case. Total excision of the tumor was performed under general anesthesia. At surgery, access was gained through a standard pre-sternocleidomastoid incision. The common carotid artery (CCA), ICA and ECA were controlled at distance from the mass and the hypoglossal nerve was identified and exposed along all its course crossing the carotid bifurcation. Intraoperatively, the tumor was wellen capsulated and delimited, arose from the descending branch of the hypoglossal nerve and was easily detached from the ICA and ECA. En bloc resection of the mass together with the descending branch of the hypoglossal nerve was performed (Figure 3). The post- operative course was uneventful and no neural deficit was observed. Histopathologic examination of the surgical specimen demonstrated a central mucous matrix and the surrounding nerve axon. The specimen also contained Antoni type A and Antoni type B. Antoni type A is composed of spindle shaped Schwann cells with elongated nuclei arranged in streams and nuclear palisades known Verocay bodies. Antoni type B consists of less spindle cells and a myxoid background, it was also characterized by positive immunohistochemical staining of S-100 protein and vimentin. Thus, the definitive diagnosis was schwannoma of the hypoglossal nerve. Regular controls, both clinical and with cervical US every 6 months on an outpatient basis were programmed. She is well and free from any disease recurrence at tree year follow-up.
Schwannomas are benign tumors. They usually develop from the sensory component of cranial nerves, most commonly from 8th and 10th cranial nerves. Hypoglossal nerve schwannoma is rare, since this nerve is purely motor. Schwanomas of the vagus and hypoglossal nerve are known to potentially masquerade a tumor of the carotid body at preoperative imaging, due to the close situation of these structures [12-16]. However, true schwannomas arising from the hypoglossal nerve are usually associated with hemiatrophy, fasciculation and deviation of the tongue upon protrusion [15], which can be rarely caused also by schwannomas of the cervical vagus nerve [16], whereas carotid body tumors are almost never associated with such symptoms. Schawanomas of the descending branch of the hypoglossal nerve should be neurologically asymptomatic, until compression of adjacent cranial nerves occurs, given the absence of functional actions of the descending branch itself, which was the case in this presentation. However, as well as tumors arising from the hypoglossal and vagus nerve, they may masquerade a carotid body tumor at diagnostic imaging [1]. This too occurred in the case object of this report. Histopathological examination demonstrates two types of schwannomas cells: Antoni type A and Antoni type B. The Antoni type A are spindle-shaped cells with parallel rows of palisading nuclear organized in whorls and waves, while the Antoni type B consists of spindle cells haphazardly scattered in a delicate, fibrillar microcystic matrix. Most schwannomas contain a mixture of both Antoni type A and Antoni type B tissue [17]. As for Schwannomas arising from other cranial nerves, excision of the mass en block with the whole nerve is the best option in order to achieve a curative treatment [3], given that, limited to the descending loop of the hypoglossal nerve, this purpose can be reached without any functional impairment. The need for a curative resection is supported by the opportunity of avoiding a redo operation in case of recurrence and by the possibility that both primary and recurrent Schwannomas may potentially show an evolution towards sarcoma [3, 13, 18-20]. Technical tips of the reported case include the standard access through a presternocleidomastoid incision, as for a standard carotid endarterectomy, a separate control of CCA, ECA and ICA together with systemic heparinization, should the need for clamping of the carotid bifurcation arise. For large masses, extending high, above C1, as anticipated at preoperative imaging, nasal intubation should be considered, in order to gain sufficient exposure toward the base of the skull and for gaining safe control of the distal ICA. Due to its anatomical situation and to the small diameter of the Schwannoma reported herein, this adjuct maneuver was, obviously, not necessary. No matter from which nerve the Schwannoma arises, regular controls, both clinical and US, on a 6-month basis for at least the first 3 years, then on a yearly basis, are strongly advised, in order to promptly detect and treat any eventual recurrence, although this is expected to be extremely rare after a proper curative resection [1].
Extra cranial hypoglossal schwannoma is very rare and few cases have been described in the literature. Existing literature of the schwannoma of the descending loop of the hypoglossal nerve is limited to two previously reported case, and this report adds that prompt resection of even small masses involving the carotid bifurcation is always indicated in order to obtain the maximum possibilities of a durable cure, limiting at maximum functional impairment. Despite the rarity of schwannomas, this condition should be considered in differential diagnoses for masses localised in the neck.
The authors declare no competing interests.
The authors have contributed to the diagnostic and therapeutic management of patients and to the writing of this work. All the authors contributed to the conduct of this work. All authors have read and approved the final version of the manuscript.
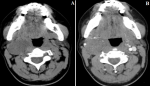
Figure 1: non-contrast (A) and contrast-enhanced (B) CT images; the mass was located lateral to the right submandibular region contrast-enhanced CT demonstrated enhancement of intratumoral blood vessels
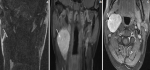
Figure 2: MR images showed masse was located later to the right submandibular region (arrow), homogeneous hypo intensity on T1-WI (A), heterogeneous hyper intensity on T2-WI (B), and heterogeneous enhancement on contrast-enhanced T1-WI (C)
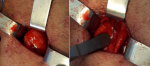
Figure 3: intraoperative, the tumor was well-encapsulated and continuous with the descending branch of the hypoglossal nerve
- Giulio Illuminati, Giulia Pizzardi, Rocco Pasqua, Piergaspare Palumbo, Schwannoma of the descending loop of the hypoglossal nerve: Case report. International Journal of Surgery Case Reports. 2017;34:20-22. Google Scholar
- Matthew K Lee, Douglas R Sidell, Abie H Mendelsohn, Keith E Blackwell. Hypoglossal Schwannoma Masquerading asa Carotid Body Tumor. Case Reports in Otolaryngology. 2012; 842761:4. PubMed | Google Scholar
- Illuminati G, Pizzardi G, Minni A, Masci F, Ciamberlano B, Pasqua R et al. Superiority of resection over nucleation for schwannomas of the cervical Vagus nerve: a retrospective cohort study of 22 consecutive patients. Int J Surg. 2016;29:74-78. PubMed | Google Scholar
- Yasumatsu R, Nakashima T, Miyazaki R, Segawa Y, Komune S. Diagnosis and management of extracranial head and neck schwannomas: a review of 27 cases. Int J Otholarungol. 2013;2013:973045. PubMed | Google Scholar
- Colreavy MP, Lacy PD, Huges J, Bouchier-Hayes D, Brennan P, O´Dwyer AJ et al. Head and neck schwannomas-a 10 year review. J Laryngol Otol. 2000;114:119-124. PubMed | Google Scholar
- Ducatman BS, Scheithauer BW, Piepgras DG, Reiman HM, Ilstrup DM. Malignant peripheral nerve sheath tumors: a clinicopathologic study of 120 cases. Cancer. 1986;15:57-21. PubMed | Google Scholar
- Fornaro R, Salerno A, Constantin Filip D. Schwannoma of the hypoglossal nerve: Review of the literature based on an illustrative case. Molecular and clinical oncology. 2017;7: 288-294. PubMed | Google Scholar
- Hari Ram, Agrawal SP, Chakrabarti S, Husain N. Hypoglossal Schwannoma of Parapharyngeal Space: An Unusual Case Report. J Maxillofac Oral Surg. 2015;14(Suppl 1):S73-S76. PubMed | Google Scholar
- Babatunde O, Bamgbose, Akiko Sato, Yoshinobu Yanagi, Miki Hisatomi. A Case of Schwannoma of the Submandibular Region. The Open Dentistry Journal. 2018;12:12-18. PubMed | Google Scholar
- Morey Mas MA, Iriarte Ortabe JI, Caubet Biayna J, Hamdan HA. Neurinoma of the descending loop of the hypoglossal nerve: report of a case. An Otorrinolaringol Ibero Am. 2001;28:523-529. PubMed | Google Scholar
- Agha RA, Fowler AJ, Saetta A, Barai I, Rajmohan S, Orgill DP. The SCARE Group, The SCARE statement: consensus-based surgical case report guidelines. Int J Surg. 2016;34:180-186. PubMed | Google Scholar
- Suthar PP, Mistry KA, Rajan P, Ankit P, Mehta C. Isolated hypoglossal nerve Schwannoma: an uncommon presentation of Schwannoma. J Clin Diagn Res. 2015;9:TJ01-TJ02. PubMed | Google Scholar
- Lee RM, Ong CP, Jacobsen AS, Chan MY, Hwang WS. Malignant peripheral nerve sheath tumor mimicking carotid body tumor-case report and review. J Pediatr Surg. 2011;46:554-558. PubMed | Google Scholar
- Leec MK, Sidell DR, Mendelsohn AH, Blackwell KE. Hypoglossal schwannoma masquerading as a carotid body tumor. Case Rep Otolaryngol. 2012;2012:842761. PubMed | Google Scholar
- Biswas D, Marnane CN, Mal R, Baldwin D. Extracranial head and neck schwannomas-a 10 year review. Auris Nasus Larynx. 2007;34:353-359. PubMed | Google Scholar
- Rallis G, Mourouzis K, Maltezos C, Stathopoulos P. Hemiatrophy of the tongue caused by an extensive vagus nerve schwannoma masquerading as a carotid chemodectoma. J Maxillofac Oral Surg. 2015;14:366-369. PubMed | Google Scholar
- Langner E, Del Negro A, Akashi HK, Ara�jo PP, Tincani AJ, Martins AS. Schwannomas in the head and neck: retrospective analysis of 21 patients and review of the literature. Sao Paulo Med J. 2007;125(4):220-2. PubMed | Google Scholar
- Mahajan V, Rao S, Gupta P, Munjal M, Agrawal S. Angiosarcoma developing in a vagal schwannoma: a rare case report. Head Neck Pathol. 2015;9:405-411. PubMed | Google Scholar
- Liu HL, Yu SY, Li GK, Wei WI. Extracranial head and neck Schwannomas: a study of the nerve of origin. Eur Arch Otorhinolaryngol. 2011;268:1343-1347. PubMed | Google Scholar
- Ziadi A, Saliba I. Malignant peripheral nerve sheath tumor of intracranial nerve:a case series review. Auris Nasus Larynx. 2010;37:539-545. PubMed | Google Scholar