Pitfall of I-131 whole body scan: a mucinous adenocarcinoma of the ovary
Ali Sellem, Issam Msakni, Wassim Elajmi, Hatem Hammami
Corresponding author: Ali Sellem, Nuclear Medicine Department, Military Hospital of Tunis, Tunis, Tunisia 
Received: 11 Jan 2020 - Accepted: 23 May 2020 - Published: 08 Jun 2020
Domain: Oncology
Keywords: Thyroid cancer, mucinous adenocarcinoma, ovary, radioiodine, false positive
©Ali Sellem et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ali Sellem et al. Pitfall of I-131 whole body scan: a mucinous adenocarcinoma of the ovary. Pan African Medical Journal. 2020;36:72. [doi: 10.11604/pamj.2020.36.72.21507]
Available online at: https://www.panafrican-med-journal.com//content/article/36/72/full
Pitfall of I-131 whole body scan: a mucinous adenocarcinoma of the ovary
Ali Sellem1,&, Issam Msakni2, Wassim Elajmi1, Hatem Hammami1
1Nuclear Medicine Department, Military Hospital of Tunis, Tunis, Tunisia, 2Pathology Department, Military Hospital of Tunis, Tunis, Tunisia
&Corresponding author
Ali Sellem, Nuclear Medicine Department, Military Hospital of Tunis, Tunis, Tunisia
False positive radioiodine uptake following thyroidectomy for differentiated thyroid cancer has been reported in some cases. A 57-year-old female patient was referred for ablative radioiodine treatment four weeks after undergoing total thyroidectomy for papillary thyroid carcinoma. Posttherapeutic I-131 scintigraphy showed uptake in the neck and large focus in the lower abdomen and pelvis. Pathology revealed a mucinous adenocarcinoma of the right ovary.
Radioiodine is used for treating differentiated thyroid carcinoma [1]. The presence of uptake sites on the whole body scanning (WBS) following iodine 131 (I-131) may be caused by physiological radioiodine uptake, thyroid remnants or metastasis. However, the presence of unusual lesions may cause a false-positive results on radioiodine WBS; therefore, it is imperative to carefully evaluate abnormal scans in order to appropriately manage patients with differentiated thyroid cancer (DTC) [1]. We herein report an interesting case of false positive radioiodine uptake on an ovarian mucinous adenocarcinoma.
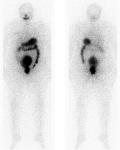
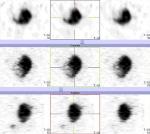
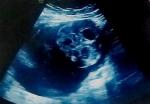
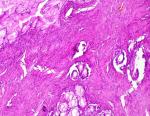
A 57-year-old female patient underwent total thyroidectomy. Histopathology revealed a follicular thyroid carcinoma (pT1bNxMx). Four weeks later she received, with thyroid hormone withdrawal, 3.7 GBq of 131I as a treatment. At this time, the serum thyroglobulin level was 2.7 ng/mL, TSH was 73 �IU/ml and antithyroglobulin antibody level was less than 20 IU/mL. Five days after the treatment, WBS (Figure 1) showed mild uptake in the neck, representing thyroid remnants, and a large and a high heterogeneous radioiodine accumulation in the median lower abdomen and pelvis confirmed by Single Photon Emission Computed Tomography (SPECT) (Figure 2). An ultrasound showed a right adnexal mass measuring 126 mm with a double tissue and cystic components with heterogeneous vascularization on color Doppler (Figure 3). The patient underwent a hysterectomy with bilateral oophorectomy. Pathological examination found a mucinous adenocarcinoma of the right ovary (Figure 4).
Ovarian radioiodine uptake at post-therapy WBS may occur in benign or malignant conditions [2-4]. Pathology examination is the only way to differentiate between the two conditions. The benign pathological diagnosis can be a benign thyroid tissue (struma ovarii) [2], a benign mucinous ovarian cystadenoma [5, 6] and an ovarian endometriosis cyst [2]. The malignant conditions were metastasis of thyroid cancer cells to ovary and thyroid cancer originating from embryonic thyroid tissue in the ovary, which may also result in focal ovarian uptake [2]. To our knowledge, this is the first case of false-positive radioiodine uptake in an ovarian mucinous adenocarcinoma. The suggested mechanisms of radioiodine uptake in the ovarian cystadenoma include increased vascularity and capillary permeability [7].
It is important to recognize the physiological and pathological aetiologies (unrelated to thyroid) that demonstrate 131 I uptake and may lead to false positif 131 I scan in patients of DTC.
The authors declare no competing interests.
Dr SELLEM, Dr HAMMAMI and Dr ELAJMI discussed the case and further explored this uptake. Dr MSAKNI allowed to make the diagnosis. Dr SELLEM wrote this clinical case. All authors have read and agreed to the final version of this manuscript.
Figure 1: post-therapeutic whole body scanning showing a mild uptake in the neck (thyroid remnants), and a large radioiodine accumulation in the median lower abdomen and pelvis
Figure 2: SPECT of the pelvis showing a large and heterogeneous radioiodine accumulation
Figure 3: ultrasonography showing a right adnexal mass measuring 126 mm with a double tissue and cystic components
Figure 4: HEx250: mucinous adenocarcinoma of the ovary, mucinous glands in a fibrous stroma
- Haugen BR, Alexander EK, Bible KC, Doherty MD, Mandel SJ, Nikiforov YR et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid. 2016;26(1):1-133. PubMed | Google Scholar
- Jong-Ryool Oh and Byeong-Cheol Ahn. False-positive uptake on radioiodine whole-body scintigraphy: physiologic and pathologic variants unrelated to thyroid cancer. Am J Nucl Med Mol Imaging 2012;2(3):362-385. Google Scholar
- Vincenzo Triggiani, Vito Angelo Giagulli, Michele Iovino, Giovanni De Pergola, Brunella Licchelli, Antonio Varraso, Franca Dicembrino, Guido Valle, Edoardo Guastamacchia. False positive diagnosis on 131iodine whole-body scintigraphy of differentiated thyroid cancers. Endocrine. 2016;53(3):626-35. PubMed | Google Scholar
- Leckzinscka Buton, Olivier Morel, Patricia Gault, Frédéric Illouz, Patrice Rodien, Vincent Rohmer. False-positive Iodine-131 whole-body scan findings in patients with differentiated thyroid carcinoma: Report of 11 cases and review of the literature. Ann Endocrinol. 2013;74(3):221-30. PubMed | Google Scholar
- Zhong-Ling Qiu, Yan-Hong Xu, Hong-Jun Song, Quan-Yong Luo. Unusual 131 uptake in a benign mucinous cystadenoma of the ovary in a patient with papillary thyroid cancer. Clin Nucl Med 2010; 35(12): 965-6. Google Scholar
- Fatema Alzahraa Almohamad, Tareq Ahmad, Basel Ahmad, Khalid Hussain, Lama Hadid, Majdi Zein, and Mohamad Ahmad. False-positive radioiodine accumulation in a huge pelvic mass after thyroidectomy for papillary carcinoma, a case report from Syria. J Surg Case Rep. 2018;28(2):028. PubMed | Google Scholar
- Brahm Shapiro, Vittoria Rufini, Ayman Jarwan, Onelio Geatti, Kimberlee J. Kearfott, Lorraine M. Fig, lan D. Kirkwood, and Milton D. Gross. Artifacts, anatomical and physiological variants, and unrelated diseases that might cause false-positive whole-body 131-I scans in patients with thyroid cancer. Semin Nucl Med. 2000;30(2):115-32. PubMed | Google Scholar