Aberrant single metastasis to the elbow from primary rectal cancer: a rare presentation
Alessandro Bianchi, Marina Jimenez-Segovia, Jaume Bonnin-Pascual, Marga Gamundí-Cuesta, Myriam Fernandez-Isart, Monica Guillot-Morales, Diego Salinas-Gonzalez, Xavier Francesc Gonzalez-Argenté
Corresponding author: Alessandro Bianchi, Department of General Surgery, Hospital Universitario Son Espases, Palma de Mallorca, Spain 
Received: 29 Jan 2020 - Accepted: 14 Mar 2020 - Published: 31 Aug 2020
Domain: Oncology,Surgical oncology
Keywords: Metastasis, rectal carcinoma, colorectal carcinoma, elbow
©Alessandro Bianchi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Alessandro Bianchi et al. Aberrant single metastasis to the elbow from primary rectal cancer: a rare presentation. Pan African Medical Journal. 2020;36:383. [doi: 10.11604/pamj.2020.36.383.21634]
Available online at: https://www.panafrican-med-journal.com//content/article/36/383/full
Aberrant single metastasis to the elbow from primary rectal cancer: a rare presentation
Alessandro Bianchi1,&, Marina Jimenez-Segovia1, Jaume Bonnin-Pascual1, Marga Gamundí-Cuesta1, Myriam Fernandez-Isart1, Monica Guillot-Morales2, Diego Salinas-Gonzalez3, Xavier Francesc Gonzalez-Argenté1
&Corresponding author
Rectal adenocarcinoma usually metastasizes to the liver and lungs and when it has bone spread, it more frequently involves the vertebrae and pelvis. Thus, aberrant metastasis from a rectal adenocarcinoma to upper extremities with preservation of intra-abdominal organs is very uncommon. We present the case of an 80-year-old male patient with a diagnosis of adenocarcinoma of the rectum T4N1M1 with non-axial single bone metastases and with preservation of visceral organs. Anterior resection of rectum after neoadjuvant chemotherapy and radiotherapy were made. The bone metastasis received palliative radiotherapy and was not resected. The patient died 10 months after diagnosis. This clinical situation generally has a poor prognosis. When the patient complains of unusual bone pain it is necessary to suspect a malignant disease and even if extraordinarily rare, rectal cancer must be considered as a possible cause.
Colorectal cancer (CRC) is one of the most common malignancies worldwide. Its usual sites of metastasis are the regional lymph nodes, liver, lungs, breast and prostate. The patient's medical history generally indicates the primary site, and most patients are previously diagnosed in relation to a primary neoplasm and are successively treated accordingly. The most common primary sites are lungs in men and breasts in women [1]. Skeletal metastases are relatively rare in CRC; only 1% of all bone metastases. Osseous metastases are found in less than 25% of cases of CRC, while it is relatively frequent in breast, thyroid, bronchial, renal and prostate cancer [2]. When there is bone involvement, it is generally located at the level of the axial skeleton and the pelvis [3,4]. Rectal cancer has a different lymphatic drainage with respect to colon cancer, leading to the development of more frequent metastatic bone disease. Its proximity to Batson´s venous plexus connects with the vertebral venous system and leads to aberrant metastatic spread [5]. Even though this spread has a primary predilection for the liver and lung, propagation to alternative sites is rare, while spread to bone other than the pelvis or vertebrae is extremely rare [6]. This paper reports a case of a primary single metastasis to the elbow from a rectal carcinoma.
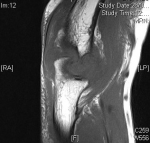
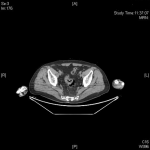
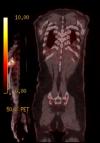
We present the case of an 80-year-old male who presented right elbow pain, which was disturbing his sleep and limiting his ability to perform his daily activities. In the anamnesis, 27 years ago the patient was diagnosed and treated for lung squamous cell carcinoma, receiving surgery and postoperative radiotherapy. As an initial part of the study, an elbow x-ray was requested, identifying a bone spur without appreciating any cortex lesion. Due to the persistence and lack of improvement of the symptoms, an magnetic resonance imaging (MRI) was performed, which showed a destructive lesion of the bone cortex of the elbow joint (Figure 1). Computed tomography (CT) scans were performed on the thorax, abdomen, and pelvis to identify the primary lesion and a thickening of the rectum was observed (Figure 2). Bone scintigraphy and positron emission tomography (PET) were performed to rule out distant dissemination of other metastatic lesions. No pulmonary or hepatic metastases were revealed and the only objectifiable metastatic lesion was the right elbow (Figure 3). In direct questioning, the patient reported no occasional bleeding in the rectum or alteration of the bowel movements. The colonoscopy showed a circumferential lesion 9 cm from the anal margin. Biopsy of the rectal lesion and elbow lesion confirmed a poorly differentiated invasive adenocarcinoma of primary and metastatic origin, respectively. The staging of a T4N1M1 lesion was completed with a rectal MRI, which reported rectal lesion extended to perirectal fat with enlarged lymph nodes. Anterior resection of rectum after neoadjuvant chemotherapy and radiotherapy were made. The bone metastasis received palliative radiotherapy and was not resected. The patient died 10 months after diagnosis.
The phenomenon of aberrant skeletal metastasis is relatively rare and the first case was reported in 1870 by Curling et al. who described a concomitant lesion in the radius during an autopsy of a patient with rectal cancer [7]. The pathways of metastatic dissemination in rectal cancer are generally multiple. In the first place, dissemination can occur through the peritoneum, generating peritoneal carcinomatosis and ovarian metastases in female patients [8]. Secondly, the tumour cells can spread through lymphatic drainage, affecting the local lymph nodes, paraaortic and even inguinal lymph nodes [9]. Finally, venous dissemination occurs through the middle and lower haemorrhoidal veins that drain the rectum into the inferior vena cava allowing an ascending hematologic spread, reaching the liver, the spleen and ultimately the lungs [10]. Despite this, cases of metastatic dissemination in unusual sites have been described. Cases reported in the literature include the adrenal glands, the pituitary glands and thyroid gland [11], the heart, the bile duct [12], the brain [13] and, as in the case presented, the upper extremities [14]. Bone involvement is not usual for metastatic dissemination of rectal cancer but is typical in other types of cancer such as breast, thyroid, bronchial, renal and prostate cancer [2]. Osseous metastases are found in less than 25% of the cases of CRC. Kanathan et al. reported an incidence of skeletal metastases of 1% in a retrospective study of 137 patients with rectal cancer. Due to the lymphatic drainage of the rectum, bone metastases from rectal cancer do not usually appear in peripheral bones, with the typical locations being the vertebrae and pelvis [15]. This could be explained by the presence of Batson's venous plexus, which allows metastases to bypass the portal and cava venous systems. The sacral venous plexus is rich in anastomosis and the distal valvular formation is anatomically variable. The connections between the vertebral and epidural veins associated with a low blood pressure system could cause the blood to pass into the vertebral system [16].
Another peculiar aspect of this clinical case is the bone metastatic dissemination with preservation of intra-abdominal organs. Distal dissemination without organ involvement is an extremely rare event but may result from a combination of host immune response, chemotactic factors of vascular permeability and other mechanisms of cell signalling [17]. Taking into these factors, metastases could spread without following the usual pathways that avoid the venous portal and cava systems and facilitate bone seeding. As in the case presented, the only metastasis detected was located in the right elbow, with both the scintigraphy and PET-CT scan being negative. Patients with colorectal cancer usually have relatively non-specific symptoms: rectal bleeding, bowel movement changes and abdominal pain are the three main symptoms of rectal cancer that may also occur in benign disease. It has been described that many cancer patients usually have more than one symptom [18]. The peculiarity of the case presented is that the patient reported no symptoms or any bowel movement alterations. In a situation of clinical and symptomatic silence, the screening could have detected the appearance of the rectum tumour long before it had become metastatic since the extension study began after the discovery of a lytic lesion of the elbow. The detection of metastasis is generally an unfavourable event, so when an initial diagnosis of metastatic rectal cancer has been made, patients usually have a poor prognosis. Of all the possible metastatic locations described in the literature, the bone location is the worst for average survival, varying between 4 to 7 months according to the series [19]. Bonnheim et al. describe an average survival of 10 months when patients suffer a single metastasis and a 6-month survival when bone metastasis is also associated with other distant metastases [20]. In spite of presenting a good tolerance to neoadjuvant therapy and surgery, the patient survived ten months due to progressive degeneration, and probably the persistence of the elbow bone disease.
We present a case of a patient with primary metastatic rectal adenocarcinoma of the elbow with no evidence of visceral dissemination. This type of pathological entity is particularly rare and, for this, it is essential to maintain a high index of suspicion of an underlying malignancy in unusual cases of bone pain. When aberrant skeletal metastases of rectal adenocarcinoma has been confirmed, the patient is often already at an advanced stage. In general, in these cases the prognosis is poor. This case indicates that careful clinical and pathological evaluations are important in order to make a definitive diagnosis and that palliative treatment should be considered in therapeutic treatment.
The authors declare no competing interest.
MGC, MFI, MGM and DSG were involved in the treatment of the patient. XGA, MJS, JBP and AB carried out the bibliographic research. AB elaborated the manuscript, which was revised by JBP and XGA. All authors read and approved the final manuscript.
In memory of the author's father, Carlo Bianchi, the patient in this case, who faced his illness without complaining and with great optimism. It was, even at this juncture, an example of great courage and dignity. May he rest in peace and be remembered thanks to this publication.
Figure 1: magnetic resonance imaging (MRI) showing the destructive lesion of the bone cortex of the elbow junction
Figure 2: computed tomography (CT) that identifies the primary lesion at the level of the rectum
Figure 3: positron emission tomography (PET) that show only the metastatic lesion in the right elbow
- Watanabe M, Tada M, Satomi T, Chikazu D, Mizumoto M, Sakurai H. Metastatic rectal adenocarcinoma in the mandibular gingiva: a case report. World J Surg Oncol. 2016 Jul 29;14(1):199. PubMed | Google Scholar
- Hage WD, Aboulafia AJ, Aboulafia DM. Incidence, location, and diagnostic evaluation of metastatic bone disease. Orthop Clin North Am. 2000 Oct;31(4):515-28. PubMed | Google Scholar
- Besbeas S, Stearns MW. Osseous metastases from carcinomas of the colon and rectum. Dis Colon Rectum. 1978 Jun;21(4):266-8. PubMed | Google Scholar
- Choi JH, Kim SJ, Oh JY, Ryu SR, Shim KS, Kim KH et al. A case of rectal cancer with sternal metastasis as initial presentation. J Korean Med Sci. 1995 Aug;10(4):303-6. PubMed | Google Scholar
- Katoh M, Unakami M, Hara M, Fukuchi S. Bone metastasis from colorectal cancer in autopsy cases. J Gastroenterol. 1995 Oct;30(5):615-8. PubMed | Google Scholar
- Connelly TM, Piggott RP, Waldron RM, O'Grady P. Unusual osseous metastases from rectal adenocarcinoma: a case report and review of the literature. J Gastrointest Surg. 2015 Jun;19(6):1177-86. PubMed | Google Scholar
- Curling TB. Case of cancerous stricture of the rectum, producing obstruction, successfully relieved by colotomy. The Lancet. 1870 Jan 1 ;95(2418):3. Google Scholar
- Morales Soriano R, Morón Canis JM, Molina Romero X, Pérez Celada J, Tejada Gavela S, Segura Sampedro JJ et al. Influence of simultaneous liver and peritoneal resection on postoperative morbi-mortality and survival in patients with colon cancer treated with surgical cytoreduction and intraperitoneal hyperthermic chemotherapy. Cir Esp. 2017 Apr;95(4):214-21. PubMed | Google Scholar
- Mesko TW, Rodriguez-Bigas MA, Petrelli NJ. Inguinal lymph node metastases from adenocarcinoma of the rectum. Am J Surg. 1994 Sep;168(3):285-7. PubMed | Google Scholar
- Rahbari NN, Bork U, Kircher A, Nimitz T, Schölch S, Kahlert C et al. Compartmental differences of circulating tumor cells in colorectal cancer. Ann Surg Oncol. 2012 Jul;19(7):2195-202. PubMed | Google Scholar
- Cheung WY, Brierley J, Mackay HJ. Treatment of rectal cancer metastases to the thyroid gland: report of two cases. Clin Colorectal Cancer. 2008 Jul;7(4):280-2. PubMed | Google Scholar
- Seshadri RA, Majhi U. Endobiliary metastasis from rectal cancer mimicking intrahepatic cholangiocarcinoma: a case report and review of literature. J Gastrointest Cancer. 2009;40(3-4):123-7. PubMed | Google Scholar
- Samlali H, Bouchbika Z, Bennani Z, Taleb A, Benchekroune N, Jouhadi H et al. Brain metastasis from rectal adenocarcinoma: about a case and review of the literature. Pan Afr Med J. 2017;26:58. PubMed | Google Scholar
- Stomeo D, Tulli A, Ziranu A, Perisano C, De Santis V, Maccauro G. Acrometastasis: a literature review. Eur Rev Med Pharmacol Sci. 2015;19(15):2906-15. PubMed | Google Scholar
- Kanthan R, Loewy J, Kanthan SC. Skeletal metastases in colorectal carcinomas: a Saskatchewan profile. Dis Colon Rectum. 1999 Dec;42(12):1592-7. PubMed | Google Scholar
- Batson OV. The function of the vertebral veins and their role in the spread of metastases. Ann Surg. 1940 Jul;112(1):138-49. PubMed | Google Scholar
- Huddy SP, Husband EM, Cook MG, Gibbs NM, Marks CG, Heald RJ. Lymph node metastases in early rectal cancer. Br J Surg. 1993 Nov;80(11):1457-8. PubMed | Google Scholar
- Thompson MR, Perera R, Senapati A, Dodds S. Predictive value of common symptom combinations in diagnosing colorectal cancer. Br J Surg. 2007 Oct;94(10):1260-5. PubMed | Google Scholar
- Santini D, Tampellini M, Vincenzi B, Ibrahim T, Ortega C, Virzi V et al. Natural history of bone metastasis in colorectal cancer: final results of a large Italian bone metastases study. Ann Oncol. 2012 Aug;23(8):2072-7. PubMed | Google Scholar
- Bonnheim DC, Petrelli NJ, Herrera L, Walsh D, Mittelman A. Osseous metastases from colorectal carcinoma. Am J Surg. 1986 Apr;151(4):457-9. PubMed | Google Scholar