Comment on “Dermatitis herpetiformis in an African woman”: the importance of direct immunofluorescence
Alice Verdelli, Marzia Caproni
Corresponding author: Alice Verdelli, Department of Surgery and Translational Medicine, Section of Dermatology, University of Florence, Florence, Italy 
Received: 25 Feb 2019 - Accepted: 16 Dec 2019 - Published: 20 Jul 2020
Domain: Dermatology
Keywords: Dermatitis herpetiformis, linear IgA bullous dermatosis, direct immunofluorescence
©Alice Verdelli et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Alice Verdelli et al. Comment on “Dermatitis herpetiformis in an African woman”: the importance of direct immunofluorescence. Pan African Medical Journal. 2020;36:196. [doi: 10.11604/pamj.2020.36.196.18397]
Available online at: https://www.panafrican-med-journal.com//content/article/36/196/full
Letter to the editors 
Comment on “Dermatitis herpetiformis in an African woman”: the importance of direct immunofluorescence
Comment on “Dermatitis herpetiformis in an African woman”: the importance of direct immunofluorescence
Alice Verdelli1,&, Marzia Caproni2
1Department of Surgery and Translational Medicine, Section of Dermatology, University of Florence, Florence, Italy, 2U.O. Dermatology I, P.O. Piero Palagi, USL Toscana Centro, University of Florence, Florence, Italy
&Corresponding author
Alice Verdelli, Department of Surgery and Translational Medicine, Section of Dermatology, University of Florence, Florence, Italy
We read with great interest the recent article by Machona MS et al. [1] on a 30-year-old female with a long history of itch and skin eruption associated to abdominal pain, nausea and vomiting. At clinical examination, the patient showed generalised, symmetrical polymorphic lesions on the trunk, buttocks, extensor surface of the lower limbs and upper limbs. According to skin morphology and histopathology, a diagnosis of dermatitis herpetiformis (DH) with suspected celiac disease (CD) was made. The patient underwent a gluten-free diet (GFD) associated to dapsone treatment, with the improvement of both signs and symptoms in the follow-up period. In our opinion, the diagnosis in this case could be consistent with linear IgA bullous dermatosis (LABD) more than DH. Indeed, the clinical and histopathological examinations cannot be considered criteria sufficient enough to establish a diagnosis of DH. Clinically, the patient presented tense blisters in a pearl necklace-like arrangement on the extremities. These lesions are morphologically consistent with LABD more than DH [2,3]. Moreover, the post-inflammatory hypo- and hyper-pigmented macules on the abdomen can be found in LABD, while they are not typical of DH, whose lesions usually clear without post-inflammatory dyschromia (Figure 1).
Histopatological examination showed a sub-epidermal bulla with eosinophilic inflammation which can be demonstrated in an autoimmune bullous disease such as LABD [4]. The accumulation of neutrophils at the papillary tips (microabscesses), usually found in DH, was not shown. According to DH diagnostic algorithm [5], in all the patients with clinical and/or histopathological findings suggestive for DH, a biopsy of perilesional skin for direct immunofluorescence (DIF) should be performed. DIF remains the gold standard for the diagnosis of DH, showing granular immunodeposits at the dermal papillae and/or along the basement membrane (Figure 1) [5,6]. Unfortunately, in this case it was not done. Moreover, IgA anti-tTG antibodies, which are considered the most sensitive and specific serologic investigation in patients with a suspected DH [5], were not collected. According to the most recent guidelines, duodenal biopsy could be avoided if immunopathological results are consistent with DH [7,8]. In this case, an endoscopy was performed but it did not reveal inflammatory changes. Even if a quarter of DH patients have normal small bowel villous architecture, in the long term, an increased density of gamma/delta intraepithelial lymphocytes can be demonstrated [9]. Finally, patients with LABD as well as DH dramatically respond to dapsone and treatment efficacy could not be considered as an adjuvant criteria for DH diagnosis [10].
To conclude, the diagnosis of autoimmune bullous diseases is not easy and requires specific examinations. A correct early diagnosis is essential to provide adequate treatment. Since DH patients, contrary to LABD patients, need a lifelong GFD, we suggest to re-evaluate this case in order to make a correct diagnosis and to set the most appropriate long-term treatment.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: (A) linear IgA bullous dermatosis characterized by tense blisters grouped on the periumbilical area in a 10-year-old male; (B) linear IgA bullous dermatosis: hyper-pigmented macules after treatment with dapsone in a 10-year-old male; (C) linear IgA bullous dermatosis: direct immunofluorescence on perilesional skin shows a linear IgA deposit along the dermo-epidermal junction; (D) post-bullous erosions in the gluteal region in a 32-year-old patient with dermatitis herpetiformis; (E) resolution of skin lesions in a patient with dermatitis herpetiformis after a 4-month gluten-free diet; (F) dermatitis herpetiformis: direct immunofluorescence on perilesional skin shows granular immunodeposits at the dermal papillae
- Machona MS, Gupta M, Mudenda V, Ngalamika O. Dermatitis herpetiformis in an African woman. Pan Afr Med J. 2018;30:119. PubMed | Google Scholar
- Antiga E, Maglie R, Quintarelli L, Verdelli A, Bonciani D, Bonciolini V et al. Dermatitis herpetiformis: novel perspectives. Front Immunol. 2019;10:1290. PubMed | Google Scholar
- Antiga E, Caproni M, Fabbri P. Linear immunoglobulin A bullous dermatosis: need for an agreement on diagnostic criteria. Dermatology. 2013;226(4):329-32. PubMed | Google Scholar
- Otten JV, Hashimoto T, Hertl M, Payne AS, Sitaru C. Molecular Diagnosis in Autoimmune Skin Blistering Conditions CurrMol Med. 2014 Jan;14(1):69-95. PubMed | Google Scholar
- Caproni M, Antiga E, Melani L, Fabbri P. Italian Group for Cutaneous Immunopathology. Guidelines for the diagnosis and treatment of dermatitis herpetiformis. J Eur Acad Dermatol Venereol. 2009;23(6):633-8. PubMed | Google Scholar
- Antiga E, Verdelli A, Calabrò A, Fabbri P, Caproni M. Clinical and immunopathological features of 159 patients with dermatitis herpetiformis: an Italian experience. G Ital Dermatol Venereol. 2013;148(2):163-9. PubMed | Google Scholar
- Husby S, Koletzko S, Korponay-Szabó I, Kurppa K, Mearin ML, Ribes-Koninckx C et al. European society paediatric gastroenterology, hepatology and nutrition guidelines for diagnosing coeliac disease 2020. Pediatr Gastroenterol Nutr. 2020;70(1):141-156. PubMed | Google Scholar
- Antiga E, Caproni M. The diagnosis and treatment of dermatitis herpetiformis. Clin Cosmet Investig Dermatol. 2015;8:257-65. PubMed | Google Scholar
- Mansikka E, Hervonen K, Salmi TT, Kautiainen H, Kaukinen K, Collin P et al. The Decreasing Prevalence of Severe Villous Atrophy in Dermatitis Herpetiformis: a 45-Year Experience in 393 Patients. J Clin Gastroenterol. 2017;51(3):235-239. PubMed | Google Scholar
- Witte M, Zillikens D, Schmidt E. Diagnosis of Autoimmune BlisteringDiseases. Front Med (Lausanne). 2018 Nov2;5:296. PubMed
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
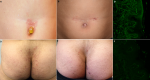 Figure 1: (A) linear IgA bullous dermatosis characterized by tense blisters grouped on the periumbilical area in a 10-year-old male; (B) linear IgA bullous dermatosis: hyper-pigmented macules after treatment with dapsone in a 10-year-old male; (C) linear IgA bullous dermatosis: direct immunofluorescence on perilesional skin shows a linear IgA deposit along the dermo-epidermal junction; (D) post-bullous erosions in the gluteal region in a 32-year-old patient with dermatitis herpetiformis; (E) resolution of skin lesions in a patient with dermatitis herpetiformis after a 4-month gluten-free diet; (F) dermatitis herpetiformis: direct immunofluorescence on perilesional skin shows granular immunodeposits at the dermal papillae
Figure 1: (A) linear IgA bullous dermatosis characterized by tense blisters grouped on the periumbilical area in a 10-year-old male; (B) linear IgA bullous dermatosis: hyper-pigmented macules after treatment with dapsone in a 10-year-old male; (C) linear IgA bullous dermatosis: direct immunofluorescence on perilesional skin shows a linear IgA deposit along the dermo-epidermal junction; (D) post-bullous erosions in the gluteal region in a 32-year-old patient with dermatitis herpetiformis; (E) resolution of skin lesions in a patient with dermatitis herpetiformis after a 4-month gluten-free diet; (F) dermatitis herpetiformis: direct immunofluorescence on perilesional skin shows granular immunodeposits at the dermal papillae











