Management of a post-coital recto vaginal fistula at the Douala Gyneco-Obstetric and Pediatric Hospital: a case report
Alphonse Nyong Ngalame, Armand Talom Kamga, Rakya Inna, Darolles Wekam Mwadjie, Emile Telesphore Mboudou
Corresponding author: Alphonse Nyong Ngalame, Douala Gyneco-Obstetric and Pediatric Hospital, Douala, Cameroon 
Received: 03 May 2020 - Accepted: 16 May 2020 - Published: 03 Jul 2020
Domain: Obstetrics and gynecology
Keywords: Management, recto vaginal fistula, post-coital
©Alphonse Nyong Ngalame et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Alphonse Nyong Ngalame et al. Management of a post-coital recto vaginal fistula at the Douala Gyneco-Obstetric and Pediatric Hospital: a case report. Pan African Medical Journal. 2020;36:151. [doi: 10.11604/pamj.2020.36.151.23281]
Available online at: https://www.panafrican-med-journal.com//content/article/36/151/full
Case report 
Management of a post-coital recto vaginal fistula at the Douala Gyneco-Obstetric and Pediatric Hospital: a case report
Management of a post-coital recto vaginal fistula at the Douala Gyneco-Obstetric and Pediatric Hospital: a case report
Alphonse Nyong Ngalame1,&, Armand Talom Kamga2, Rakya Inna1, Darolles Wekam Mwadjie1, Emile Telesphore Mboudou2
&Corresponding author
Recto vaginal fistula can be secondary to various and multiple causes. However, intercourse is an exceptional cause. The objective of this work is to expose its clinical, therapeutic and prognostic particularities. We report the case of rectovaginal fistula in a 29-year-old patient, following consensual sex. She underwent posterior colpoperineorraphy under spinal anesthesia, with a favorable outcome. Post-coital recto vaginal fistula is a stigmatizing pathology responsible for polymorphic complications. Prompt care can improve quality of life and the obstetrical prognosis of the patient.
Post-coital recto vaginal fistula (RVF) which is an abnormal communication between the rectal and vaginal mucosae following sexual intercourse, is a rare but stigmatizing condition. It is usually associated with minimal or moderate per vaginal bleeding. Very few cases reported in the literature to date. In Nigeria, post-coital RVF represent 0.7 cases per 1000 gynecological emergencies [1]. In Ethiopia, a total of 91 cases of RVF were reported over a period of 6 years, with all linked to consented sexual intercourse and rape [2]. The main causes of RVF are obstetrical, followed by genital cancer, radiotherapy, Crohn's disease and anal abscess [3,4].
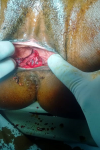
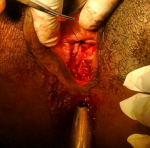
We report the case of a post-coital recto vaginal fistula in a 29-year-old patient, single, veterinary nurse, nulliparous and desiring fertility for 3 years now. She was referred to us from a district hospital by her attending physician for better management of a rectovaginal fistula, which occurred 6 hours before her admission following vigorous vaginal sexual intercourse and consented to in the supine position, according to the patient. There followed a vaginal bleeding which had motivated a first consultation in this hospital where she had received intravenous fluids with 500ml of Ringer´s lactate and the placement of a vaginal packing. Faced with the unavailability of the gynecologist on duty, the patient was immediately referred to us. Upon arrival, she complained of perineal pain, with a blood pressure of 123/87mmHg and a pulse rate of 113 beats per minute. The conjunctivae were pink. The vulva was stained with bright red blood with packing in place. When packing was removed, we discovered a complete tear at the level of the posterior vulva (Figure 1). On speculum examination, the cervix was anterior, macroscopically normal with no lesion at the posterior fornix. On vaginal examination, the cervix was anterior, long, thick and closed, the uterus was of normal size, with no lesion at the vaginal fornixes. We uncovered a 3cm longitudinal tear communicating totally between both rectal and vaginal mucosae at the lower third of the recto-vaginal wall. Its apex was approximately 3-4cm from the posterior fornix.
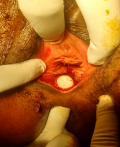
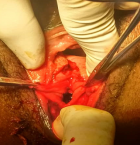
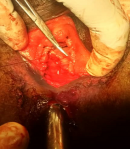
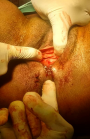
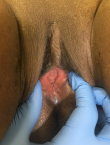
The external anal sphincter was intact (Figure 2). We concluded with a post-coital recto vaginal fistula of the lower third. The management consisted, after counseling the patient, in a posterior colpoperineorraphy in the operating room under spinal anesthesia. We equally offered her psycho-social support going forward. The operating procedures consisted in: betadine swab of perineum and vagina, placement of a size 12 Hegar´s dilator in the rectum, suturing of the rectal mucosa with absorbable vicryl No. 2/0 (Figure 3 and Figure 4), then a successive suture of the vaginal mucosa and of the cutaneous plane of the perineum with vicryl 0 (Figure 5). After satisfactory control of the hemostasis and checked for the solidity of the repair, we proceeded to a vaginal toileting (Figure 6). Early post-operatory follow-up was simple. She was discharge the next day under; gynecological betadine ovules and liquid for Sitz bath, amoxicillin-clavulanic acid 1g/12h and paracetamol 1g/8h orally. We also gave her diet and nutrition counseling to prevent constipation and had to suspend any sexual intercourse for the following 6 months. Her appointments for clinical review after 1 week and two months post-operatory were uneventful and satisfactory (Figure 7).
Post-coital RVF is a rare entity: 0.7/1000 gynecological emergencies in Nigeria [1], 91 cases in Ethiopia [2] and 32 cases reported in Senegal [5]. According to the available body of literature, the predisposing factors for post-coital RVF are; young age (15-30 years), parity (0-1), supine position during sexual intercourse, first intercourse, rough intercourse, peno-vaginal disproportion, inadequate physical and emotional preparation of the woman for intercourse and intercourse during the puerperal period [5-8]. Our patient was a 29-year-old nulliparous woman who just had consented though violent intercourse in the supine position. She has had multiple previous sexual relationships with the same partner, which permitted us to rule out the possibility of peno-vaginal disproportion. The most common site of vaginal injuries at coitus is the vaginal vault particularly the posterior fornix. Other sites include; right fornix, left fornix and lower vagina [9]. Our patient presented with a post coital recto vaginal fistula of the lower third. The diagnosis of post-coital RVF is essentially based on clinical examination, as was the case in our patient. However, there are methods of paraclinical investigations when the clinical diagnosis is not obvious. We can cite; colonoscopy, barium enema, computed tomography, magnetic resonance imaging [10]. An anorectal ultrasound may also be used to check the integrity of the anal sphincter. All these were not necessary in our patient due to the active bleeding and easy access of the lesion without external anal sphincter involvement. Surgical repair of post-coital RVF can be done either locally (by a trans-vaginal or trans-rectal approaches) or by a trans-abdominal approach [10]. The trans-abdominal approach is generally indicated for upper fistulas secondary to Crohn's disease, cancer or radiotherapy [10]. In our patient we proceeded to a transvaginal approach since she had a lower fistula. Post-operative medical care involves; local perineal care with antiseptics, oral antibiotics to safeguard against superinfection, analgesics, dietary counselling to prevent constipation, abstain from sex and psychosocial support of the couple.
Post-coital recto vaginal fistula is a rare entity. However, it can cause serious damage that can alter the patient's quality of life in the medium and long term, as well as her obstetrical prognosis. In the face of any post coital vaginal trauma, a careful clinical examination would be enough to start treatment quickly and thus improve the prognosis.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: exposure of the different vulvo-perineal layers
Figure 2: recto vaginal fistula
Figure 3: exposure of torn rectal mucosa
Figure 4: repair of rectal mucosa
Figure 5: repair of the vaginal mucosa
Figure 6: end result after posterior colpo-perineorrhaphy
Figure 7: complete healing on day 60 post operatory
- Abasiattai AM, Etuk SJ, Bassey EA, Asuquo EEJ. Vaginal injuries during coitus in calabar: a 10-year review. Niger Postgrad Med J. 2005;12(2):140-144. PubMed | Google Scholar
- Muleta MB, Williams G. Postcoital injuries treated at the Addis Ababa Fistula Hospital, 1991-97. Lancet. 1999;354(9195):2051-2052. PubMed | Google Scholar
- DeBeche-Adams TH, Bohi JL. Rectovaginal fistulas. Clin Colon Rectal Surg. 2010;23(2):99-103. PubMed | Google Scholar
- Ekwempu CC. Fistulae. In: Textbook of obstetrics and gynaecology for medical students: Agboola A (ed), Heinemann Pub, Nig Heinemann Pub, Nig. 1988;1:46-59.
- Cisse CT, Dionne P, Cathy A, Mendes V, Diadhious F, Ndiaye PD. Vaginal injuries during coitus. Dakar Med. 1998;43(2):135-138. PubMed | Google Scholar
- Omu AE. Vaginal injuries during coitus. Trop J Obstet Gynaecol. 1991;2:115-118.
- Ijaiya MA, Mai AM, Aboyeji AP, Kumanda V, Abiodun MO, Raji HO. Rectovaginal fistula following sexual intercourse. Annals of African Medicine. 2009;8(1):59-60. PubMed | Google Scholar
- Amenu D. Rectovaginal fistula in a newly-married woman. Gynecol Obstet (Sunnyvale). 2015;5(6):296. Google Scholar
- Anate M. Vaginal trauma at sexual intercourse in Ilorin, Nigeria: an analysis of 36 cases. West Afr J Med. 1989;8(3):217-222. PubMed | Google Scholar
- Vogel J, Johnson E, Morris A, Paquette IM, Saclarides TJ, Feingold DL et al. Clinical practice guideline for the management of anorectal abscess, fistula-in-ano and rectovaginal fistula. Dis Colon Rectum. 2016;59(12):1117-1133. PubMed | Google Scholar