Methylene tetrahydrofolate reductase gene mutation in sickle cell anaemia patients in Lagos, Nigeria
Oluwaseun Olabisi Adelekan, Ebele Ifeyinwa Uche, Taiwo Modupe Balogun, Vincent Oluseye Osunkalu, Akinsegun Abduljaleel Akinbami, Kamal Ayobami Ismail, Mulikat Adesola Badiru, Adedoyin Owolabi Dosunmu, Omolara Risqat Kamson
Corresponding author: Ebele Ifeyinwa Uche, Department of Haematology and Blood Transfusion, Lagos State University College of Medicine, Lagos, Nigeria 
Received: 21 Jun 2019 - Accepted: 12 Dec 2019 - Published: 30 Dec 2019
Domain: Internal medicine
Keywords: Sickle cell anaemia, methylene tetrahydrofolate reductase gene mutation, C677T, A1298C
©Oluwaseun Olabisi Adelekan et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Oluwaseun Olabisi Adelekan et al. Methylene tetrahydrofolate reductase gene mutation in sickle cell anaemia patients in Lagos, Nigeria. Pan African Medical Journal. 2019;34:213. [doi: 10.11604/pamj.2019.34.213.19524]
Available online at: https://www.panafrican-med-journal.com//content/article/34/213/full
Research 
Methylene tetrahydrofolate reductase gene mutation in sickle cell anaemia patients in Lagos, Nigeria
Methylene tetrahydrofolate reductase gene mutation in sickle cell anaemia patients in Lagos, Nigeria
Oluwaseun Olabisi Adelekan1, Ebele Ifeyinwa Uche2,&, Taiwo Modupe Balogun3, Vincent Oluseye Osunkalu4, Akinsegun Abduljaleel Akinbami2, Kamal Ayobami Ismail2, Mulikat Adesola Badiru1, Adedoyin Owolabi Dosunmu2, Omolara Risqat Kamson3
1Department of Haematology and Blood Transfusion, General Hospital Marina, Lagos, Nigeria, 2Department of Haematology and Blood Transfusion, Lagos State University College of Medicine, Lagos, Nigeria, 3Department of Haematology and Blood Transfusion, Lagos State University Teaching Hospital, Lagos, Nigeria, 4Department of Haematology and Blood Transfusion, College of Medicine, University of Lagos, Idiaraba, Lagos, Nigeria
&Corresponding author
Ebele Ifeyinwa Uche, Department of Haematology and Blood Transfusion, Lagos State University College of Medicine, Lagos, Nigeria
Introduction: the significant causes of mortality among individuals with sickle cell anaemia (SCA) such as acute chest syndrome and cerebrovascular disease are related to vascular occlusion. Polymorphisms of the methylene tetrahydrofolate reductase (MTHFR) gene in persons with sickle cell anaemia have been suggested as a potential risk for vaso-occlusive events, with the C677T and A1298C polymorphisms being the commonest. This study therefore aimed to establish the pattern of MTHFR C677T and A1298C gene mutations among adults with HbSS phenotype attending the Haematology Clinic in Lagos State University Teaching Hospital Lagos, Nigeria.
Methods: a cross-sectional study was done among SCA patients attending the Haematology Clinic of the Lagos State University Teaching Hospital (LASUTH), using age and sex matched HbAA controls. DNA extraction and gene analysis were done. The selective amplification of a particular segment of the DNA by polymerase chain reaction (PCR) was done and subsequent digestion of the amplified MTHFR gene into its various fragments.
Results: the overall prevalence of the C677T mutation among participants was 19.3% (37 of 192), while the prevalence of A1298C was 15% (29 of 192).
Conclusion: the prevalence of MTHFR C677T was higher than A1298C mutations among sickle cell anaemia subjects.
Sickle cell anaemia has been recognized as a problem of major public health significance by the World Health Organization [1]. The highest frequency of the disease is found in tropical regions particularly sub-Saharan Africa, India and the Middle East. More than 75% of sickle cell anaemia cases occur in sub-Saharan Africa [1]. Nigeria has the highest burden of sickle cell anaemia worldwide, with prevalence values ranging from 2% to 3% of the 140 million population [2-5]. Haemolytic and vaso-occlusive complications are seen in patients with sickle cell anaemia as well as a heightened occurrence of thrombo-embolic complications [6-9]. Thrombo-embolic complications remain a significant cause of morbidity and mortality in people with sickle cell anaemia [6, 10, 11]. These complications include stroke [12, 13], avascular necrosis of the head of femur [14], thrombotic microangiopathy [15], venous thromboembolism [16], retinopathy [17], end organ damage [18, 19], chronic leg ulcers [18, 19] amongst others. Hypercoagulability in sickle cell anaemia may be responsible for the increased development of vascular occlusion in certain organs [6, 19] and acute pain episodes [6, 20]. The causes of hypercoagulability in sickle cell anaemia are multifactorial. Factors such as increased plasma levels of homocysteine, reduced levels of natural anticoagulants like proteins C and S [21], increased levels of thrombin generation markers like thrombin-antithrombin (TAT) complexes or protein fragment 1+2 (F1+2) [22], increased D-dimer complexes, circulating antiphospholipid antibodies, increased tissue factor expression and adherence of sickled erythrocytes to the vascular endothelium, Factor V Leiden and prothrombin gene mutation have all been implicated [7, 8]. The MTHFR gene is 2.2 kilobases long and located on chromosome 1 at 1p36.3 [23, 24]. The complimentary DNA sequence is 2.2 kilobases long and consists of 11 exons [25]. This gene codes for the protein methylenetetrahydrofolate reductase (MTHFR) which catalyzes the conversion of 5, 10-methylenetetrahydrofolate to 5-methyltetrahydrofolate [23, 24]. 5-methyltetrahydrofolate is a major form of folate in the plasma [23, 24, 26] and it is a co-factor in the re-methylation of homocysteine to methionine thereby reducing plasma homocysteine levels [23, 24, 26]. Folate in its 5-methyl form, also participates in single-carbon transfers which occur as part of the synthesis of nucleotides and DNA methylation [24]. It is also involved in the synthesis of proteins, neurotransmitters and phospholipids [24]. Normal MTHFR activity maintains the level of circulating folate and methionine and possibly prevents accumulation of homocysteine [24]. Therefore, mutations in the MTHFR gene reduces the activity of the enzyme MTHFR leading to hyper-homocysteinaemia [23, 24, 26] and this is particularly heightened in patients with sickle cell anaemia who have an increased demand for folate due to their high red cell turnover or shortened red cell lifespan.
�
C677T and A1298C are the two most commonly studied polymorphisms of the MTHFR gene, which are associated with diminished enzyme activity of methylene tetrahydrofolate reductases resulting in the accumulation of homocysteine especially in individuals with low levels of folate [24, 27-30]. The significant causes of mortality among individuals with sickle cell anaemia such as acute chest syndrome and cerebrovascular disease are related to vascular occlusion [12, 31-36]. Polymorphisms of the MTHFR gene in persons with sickle cell anaemia have been suggested as a potential risk for vaso-occlusive events [37-41]. Furthermore, avascular necrosis of the femoral and humeral head is a common musculoskeletal complication seen in adults with sickle cell anaemia which reduces their quality of life [42]. MTHFR mutations have also been implicated as a probable risk factor for avascular necrosis in sickle cell anaemia [43-45]. This study aimed to establish the pattern of MTHFR gene mutations among adults with HbSS phenotype attending the Haematology Clinic of the Lagos State University Teaching Hospital (LASUTH) with a view to determine the role of MTHFR gene polymorphism as a contributory factor in their differential phenotypic expression. Also, very few studies have been published involving MTHFR gene mutations from Africa, therefore, our study would add to the body of knowledge currently available on the MTHFR gene mutations.
Study area and population
�
The study was conducted among adult patients with sickle cell anaemia attending the Haematology Clinic of LASUTH, Lagos, Nigeria, while apparently healthy individuals with no known medical condition served as controls. LASUTH is a major tertiary healthcare facility, located in the south-western part of Nigeria, within the Lagos metropolis.�
Study design�
This was a cross-sectional study.�
Study period�
The study was carried out over a period of eight months from May 2016 to December 2016.�
Sampling technique�
Purposive non-probability sampling technique was used to recruit presumably healthy staff and students of LASUTH Ikeja with haemoglobin phenotype AA and they served as the control group. A sampling frame containing the list of individuals with sickle cell anaemia attending the adult Haematology Clinic in LASUTH was drawn and subjects were selected randomly. However, only individuals with a haemoglobin electrophoresis result showing the SS band were enrolled into the study. The inclusion criteria were: age between 18 and above; known patients with sickle cell anaemia (screened by the haemoglobin S solubility test and diagnosed by cellulose acetate electrophoresis at pH 8.6) who are in steady state defined as the period free of crisis extending from at least three weeks since the last clinical event and three months or more since the last blood transfusion, to at least one week before the start of a new clinical event [46]; haemoglobin AA persons (confirmed by cellulose acetate electrophoresis at pH 8.6) who served as the control group; those who met the above criteria and agreed to participate in the study by signing the informed consent form. The participants were classified as follows: adults with sickle cell anaemia in steady state; HbAA controls who were age and sex-matched with the adults with sickle cell anaemia. The exclusion criteria were: confirmed phenotype HbAC, HbAS; history of acute or chronic illness e.g. any febrile illness, hypertension, diabetes, epilepsy, asthma; intravenous drug users; non consenting participants.�
Sample size determination�
Sample size was determined using the formula for prevalence study by Daniel [47, 48].�
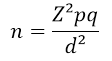
�
Where: n = sample size; Z = statistic for a level of confidence of 95%, which is conventional, Z value is 1.96; p = expected prevalence; q = 1-p; d = precision. Therefore, considering Z = 1.96; p = prevalence of MTHFR gene mutation among sub-Saharan Africans is 6% [49, 50]; p = 0.06; q = 1-p; d = 0.05; n = (1.96)2 x 0.06 x (1-0.06) / (0.05)2; n = 3.8416 x 0.06 x 0.94 / 0.0025; n = 0.216667 / 0.0025; n = 86.67; n = 87 (which is the minimum sample size in each group).�
However, in order to accommodate possible attrition or unforeseen errors in completing the study questionnaire or blood sample processing, an additional 10% (9 patients) of the calculated figure was added. Therefore, a total of 192 participants (96 in each group) were recruited into this study.�
Ethical consideration and clearance�
Ethical approval was obtained from the Health Research and Ethics Committee of LASUTH prior to commencement of the study.�
Participants' informed consent�
A written informed consent was obtained from all the participants before being recruited into the study. No participant was in any way coerced or cajoled to participate in this study. Study was done at no cost to the participants.�
Confidentiality�
The names and initials of all participants were not recorded or used to guarantee confidentiality. Participants were instead given code numbers. Paper records were secured in a cabinet inside a secured room. Electronic data was protected using a password known only to the researchers.�
Questionnaire administration and history taking�
Each participant was interviewed to obtain relevant demographic and clinical data with the use of a questionnaire. The questionnaire was administered to each participant by a member of the research team. Information on the HbSS subjects and their medical history including disease complications were retrieved from their case notes.�
Specimen collection and storage�
Seven milliliters of venous blood was drawn from each subject. Five milliliters of this was dispensed into sodium ethylene diamine tetra-acetate (EDTA) specimen bottles. This sample was used for a full blood count (FBC). This was analyzed within 2 hours of collection. Some of the blood collected in the EDTA specimen bottle was used for cellulose acetate electrophoresis test. The remaining two milliliters of the blood was dispensed into another set of EDTA bottles. These samples were prepared for DNA extraction and subsequently used for genetic analysis. The samples were washed with phosphate buffer saline (PBS) until the supernatant was white. The samples were then stored at the appropriate temperature till the DNA extraction was done. It was stored at 2-8°C if the DNA extraction was scheduled to be done within a week, at -20°C within a month and -80°C for a longer period of time.�
Statistical analysis�
All data obtained were entered into and analyzed using Statistical Package for Social Sciences (SPSS), version 22.0, Chicago, USA. Data summaries were presented in simple tables and frequencies. Data obtained from the study were evaluated for normality using the Kolmogorov-Smirnov test. Numerical data were expressed as mean�SD or median values for parametric and non-parametric data respectively. The differences in mean distribution of variables were tested using student t-test or ANOVA where appropriate (significant level was set at p < 0.05 or F < 0.05 for student t-test and ANOVA respectively). The degree of association between variables were evaluated with chi-square test and significance was set at p < 0.05.
Age and gender
�
This was a cross-sectional study of 192 participants consisting of 96 SCA patients (cases) and 96 HbAA genotype (controls). A total of 202 participants were initially recruited into the study. Ten participants were excluded from the study altogether, seven on the basis of their haemoglobin phenotype while the others had incompletely filled questionnaires. Overall, the minimum age was 18 years and the maximum 59 years with a mean of 30.48�11.16 years. A total of 102 were females (53.1%) while 90(42.9%) were males. Amongst the cases, 51(53.1%) were females and 45 were males (46.9%) and their mean age was 29.33�10.37 years. The control group was exactly the same in number and gender distribution with the cases (Table 1).�
Prevalence of MTHFR C677T and A1298C mutations�
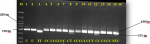
The overall prevalence of the C677T mutation among participants was 19.3% (37 of 192), while prevalence of A1298C was 15% (29 of 192) (Figure 1, Figure 2). The genotype frequencies for homozygous dominant (MTHFR 677CC), heterozygous dominant (MTHFR 677CT) and homozygous recessive (MTHFR 677TT) genes among the cases were 83.3%, 15.6% and 1% respectively. In the controls, genotype frequency was 78.1% for the homozygous dominant (CC) and 21.9% for the heterozygous dominant (CT). The homozygous recessive (TT) genotype was not detected among the controls in this study (Table 2). Similarly, the genotype frequencies of the A1298C mutation amongst the cases for the homozygous dominant (AA), heterozygous dominant (AC) and homozygous recessive (CC) were 84.4%, 14.6% and 1% respectively. However, in the controls, genotype frequencies were 85.4% for the homozygous dominant (AA), 12.5% for the heterozygous dominant (AC) and 2.1% for homozygous recessive (CC) genotype (Table 2).�
MTHFR C677T and A1298C allelic frequency distribution�
The relative frequencies of the 677T alleles for the cases and controls were 8.9% and 10.9% respectively while that of the 1298C alleles was 8.3% in both groups (Table 3).�
Ages and genders of participants with C677T and A1298C mutations�
Both mutations in the two groups were not statistically significant when correlated with the ages and genders of the participants except age vs A1298C in controls which was statistically significant (Table 4).
Studies have shown that MTHFR gene mutation results in the diminished activity of the MTHFR enzyme which is crucial in folate metabolism [26, 39]. Polymorphisms of the MTHFR gene in persons with sickle cell anaemia have been suggested as a potential risk for vaso-occlusive events [37, 39]. MTHFR mutations have also been implicated as a probable risk factor for avascular necrosis in sickle cell anaemia [43, 45]. Several genetic factors contribute to the phenotypic expression of individuals with sickle cell anaemia. The MTHFR gene mutations C677T and A1298C are some of such genetic polymorphisms which have been implicated as genetic modifiers of the disease. The prevalence of the C677T mutation among the subjects with HbSS was 16.6% and 21.9% in HbAA controls, showing no statistical difference. Likewise, the prevalence of the A1298C mutation was 15.6% in the cases and 1% lower in the control group. The population frequency of the A1298C allele is less documented than that of the C677T allele and there is inadequately published data about the prevalence of these mutations among Nigerians. These results were higher than a reported prevalence of 5% found in a study of African blacks [51], 9% in another research among African American individuals with sickle cell anaemia [52] and 12% described among Brazilian blacks [51]. However, it is comparable to a study done among a group of African American adults with sickle cell anaemia which reported a prevalence of 15% for the C677T mutation [53]. The prevalence of this mutation has been shown to vary in different populations. A higher prevalence of 36% [51], 38% [54] and 40% [51] has been reported among whites, French-Canadians and Asians respectively. Furthermore, the heterozygous dominant (CT) variant of the MTHFR C677T gene polymorphism was about 34% and 2.2% for the homozygous recessive (TT) variant type in a survey of Brazilians with sickle cell disease [39] and this differs from a frequency of 15.6% for CT variant and 1% for the TT variant found in HbSS individuals in this study. Though not statistically significant, the only homozygous (TT) variant detected was among the HbSS group, which is similar to other studies done in Africa. In a study in sub-Saharan Africa [55], there was no TT genotype identified among 234 individuals tested. In another research [56] involving 89 Africans from four tribes in sub-Saharan Africa, the frequency of the homozygous recessive TT genotype was also not reported. The frequency of the TT genotype among Blacks living outside Africa was also noted to be low [51]. This conflicts with a frequency of TT genotype ranging from 8% among Germans, 18% among Italians and 10-14% among whites living outside Europe to about 21% in Hispanics. These estimates suggest that the homozygous recessive TT variant is less common in Africans than in some other populations. Regarding the A1298C mutation, the homozygous recessive (CC) genotype frequency was 1% in cases and 2.1% in the controls which was not found to be statistically significant. This differs from a CC variant frequency of 6% seen in a survey carried out on 117 healthy Portuguese Caucasians [57]. The 6777T allele frequency ranged from 8.9% in the cases to 10.9% among the controls. This is in keeping with a prevalence of 12% in a study done among Blacks in Brazil [24] and 10% in another one carried out among Blacks in Georgia in the United States of America [24]. However, it was slightly higher than a prevalence of 6.3% generated from a pooled data on Africans in sub-Saharan Africa [24]. It is possible that some environmental or genetic factors not analyzed in this study could have modified the inheritance or expression of the MTHFR gene. Early identification of additional genetic risk factors for either preventive or therapeutic interventions is common clinical practice in the follow up of patients with SCA [30] and contributes to reduced morbidity and mortality in these patients. Even though our study found no significant difference in the prevalence of MTHFR gene mutation among the SCA patients and controls, this may be attributable to a Type II statistical error due to the small sample size used. It is possible that further research using a larger sample size which would be representative of the true prevalence of this mutation would demonstrate a significant difference.
The prevalence of MTHFR C677T was higher than A1298C mutations among sickle cell anaemia subjects. This research was self-funded, and cost was a major limiting factor. A larger study using more than 96 HbSS and 96 HbAA could be more representative of the aims and objectives of this study.
What is known about this topic
- MTHFR gene mutation reduces the activity of the MTHFR enzyme and thus leads to hyperhomocysteinaemia;
- This is particularly heightened in patients with sickle cell anaemia who have an increased demand for folate due to their high red cell turnover or shortened red cell lifespan;
- Hyperhomocysteinaemia has been implicated with a number of complications in sickle cell anaemia including avascular necrosis of the femur head, acute chest syndrome etc.
What this study adds
- The prevalence of MTHFR C677T is higher than A1298C mutations among sickle cell anaemia subjects in Lagos, Nigeria.
The authors declare no competing interests.
Study conceptualization and design was done by OA and EU. Data acquisition by OA. Data analysis and interpretation by OA and AA. All the authors drafted and reviewed the manuscript. All authors read and approved the final version of the manuscript.
The authors are grateful to Mr Sola Ojewunmi who coordinated the DNA analysis.
Table 1: age and gender distribution of study participants
Table 2: MTHFR C677T and A1298C genotype frequency distribution for cases and controls
Table 3: MTHFR C677T and A1298C allelic frequency distribution for cases and controls
Table 4: association between ages and genders of participants with C677T and A1298C mutations
Figure 1: agarose gel representation of C677T genotyping; M represents the DNA marker (50-700 bp); lanes 1 and 2 are undigested PCR products (198 bp); lane 3 shows TT genotype (175bp); lanes 4-7, 9-11, and 13-15 show the CC genotype (198 bp); lanes 8 and 12 show CT genotype (198 and 175 bp)
Figure 2: agarose gel representation of A1298C genotyping; M represents the DNA marker (50-700 bp); lanes 1 and 2 are undigested PCR products (163 bp); lanes 3, 4, 7 and 11 show AC genotype (84, 56, and 30bp); lanes 5 and 14 show the CC genotype (84 and 30 bp); lanes 6, 8-10, 12, and 13 show AA genotype (56 and 30 bp); U = undigested PCR product; NTC = non-template control
- World Health Organization. Sickle-cell anaemia: report by the Secretariat (PDF). 2006. Accessed on 20 July 2014.
- Galadanci N, Wudil B, Balogun T, Ogunrinde G, Akinsulie A, Hasan-Hanga F et al. Current Sickle Cell Disease Management Practices In Nigeria. Int Health. 2014; 6(1): 23-28. Epub 2013 Oct 10. PubMed | Google Scholar
- Akinyanju OO. The National Burden of Sickle Cell Disease and The Way Forward. Sickle Cell Foundation Nigeria. 2010. Google Scholar
- Akinyanju OO. Profile of sickle cell disease in Nigeria. Ann N Y Acad Sci. 1989; 565: 126-136. PubMed | Google Scholar
- Juwah AI, Nlemadim EU, Kaine W. Types of anaemic crises in paediatric patients with sickle cell anaemia in Enugu, Nigeria. Arch Dis Child. 2004 Jun; 89(6): 572-6. PubMed | Google Scholar
- Steinberg MH. Sickle cell anemia, the first molecular disease: overview of molecular etiology, pathophysiology, and therapeutic approaches. Scientific World Journal. 2008 Dec 25; 8: 1295-324. PubMed | Google Scholar
- Ataga KI. Hypercoagulability and thrombotic complications in hemolytic anaemias. Haematologica. 2009; 94(11): 1481-1484. PubMed | Google Scholar
- Ataga KI, Cappellini MD, Rachmilewitz EA. Beta-thalassaemia and sickle cell anaemia as paradigms of hypercoagulability. Br J Haematol. 2007; 139(1): 3-13. PubMed | Google Scholar
- Naik RP, Streiff MB, Haywood C Jr, Nelson JA, Lanzkron S. Venous thromboembolism in adults with sickle cell disease; a serious and under recognized complication. Am J Med. 2013; 126(5): 443-449. PubMed | Google Scholar
- Siddiqui AK, Ahmed S. Pulmonary manifestations of sickle cell disease. Postgrad Med J. 2003; 79(933): 384-390. PubMed | Google Scholar
- Martins PRJ, Moraes-Souza H, Silveria TB. Morbidity-mortality in sickle cell disease. Rev Bras Hamatol Hemoter. 2010; 32(5): 378-383. Google Scholar
- Ohene-Frempong K, Weiner S, Sleeper L, Miller S, EmburyS, MoohrJW et al. Cerebrovascular accidents in sickle cell disease: rates and risk factors. Blood. 1998; 91(1): 288-294. PubMed | Google Scholar
- Menaa F. Stroke in sickle cell anemia patients: a need for multidisciplinary approaches. Atherosclerosis. 2013 Aug;229(2):496-503. Epub 2013 May 16. PubMed | Google Scholar
- Matos M, dos Santos Silva L, BrittoFernandes R, Dias Malheiros C, Pinto da Silva B. Avascular necrosis of the femoral head in sickle cell disease patients. OrtopTraumatolRehabil. 2012; 14(2): 155-160. PubMed | Google Scholar
- Shome DK, Ramadocai P, Al-Ajmi A, Ali F, Malik N. Thrombotic microangiopathy in sickle cell disease. Am Haematol. 2013; 92(4): 509-515. Epub 2012 Dec 7. PubMed | Google Scholar
- Austin H, Key NS, Benso, JM, Lally C, Dowling NF, Whitsett C et al. Sickle cell trait and the risk of venous thromboembolism among blacks. Blood. 2007 Aug 1; 110(3): 908-12. Epub 2007 Apr 4. PubMed
- Tantawy A, Andrawas N, Adly A, El KadyB, Shalash A. Retinal changes in children and adolescents with sickle cell disease attending a paediatric hospital in Cairo, Egypt: risk factors and relation to ophthalmic and cerebral blood flow. Trans R Soc Trop Med Hyg. 2013 Apr; 107(4): 205-11. Epub 2013 Feb 17. PubMed | Google Scholar
- Minniti CP, Delaney KM, Gorbach AM, Xu D, Lee CC, Malik N et al. Vasculopathy, inflammation, and blood flow in leg ulcers of patients with sickle cell anaemia. Am J Hematol. 2014 Jan; 89(1): 1-6. Epub 2013 Sep 19. PubMed | Google Scholar
- Hebbel RP. Ischemia-reperfusion injury in sickle cell anaemia: relationship to acute chest syndrome, endothelial dysfunction, arterial vasculopathy, and inflammatory pain. HematolOncol Clin North Am. 2014; 28(2): 181-198. PubMed | Google Scholar
- Colombatti R, De Bon E, Bertomoro A, Casonato A, Pontara E, Omenetto E et al. Coagulation Activation in Children with Sickle Cell Disease Is Associated with Cerebral Small Vessel Vasculopathy. PLoS ONE. 2013; 8(10): e78801. eCollection 2013. PubMed | Google Scholar
- el-Hazmi MA, Warsy AS, Bahakim H. Blood proteins C and S in sickle cell disease. ActaHaematol. 1993; 90(3): 114-119. PubMed | Google Scholar
- Liesner R, Mackie I, Cookson J, McDonald S, Chitolie A, Donohoe S et al. Prothrombotic changes in children with sickle cell disease: relationships to cerebrovascular disease and transfusion. Br J Haematol. 1998; 103(4): 1037-1044. PubMed | Google Scholar
- Vasisht S, Gulati R, Narang R, Srivastava N, Srivastava L, Manchada SC et al. Polymorphism (C677T) in the 5, 10-methylenetetrahydrofolate reductase (MTHHFR) gene: A preliminary study on North Indian men. Indian J Clin Biochem. 2002; 17(1): 99-107. PubMed | Google Scholar
- Botto LD, Yang Q. 5, 10-Methylenetetrahydrofolate Reductase Gene Variants and Congenital Anomalies: A Huge Review. Am J Epid. 2000; 151(9): 862-877. PubMed | Google Scholar
- Goyette P, Pia A, Milos R, Frosst P, Tran P, Chen Z. Gene structure of human and mouse methylenetetrahydrofolate reductase (MTHFR). Mamm Genome. 1998; 9(8): 652-6. PubMed | Google Scholar
- Goyette P, Frosst P, Rosenblatt D, Rozen R. Seven novel mutations in the methylenetetrahydrofolate reductase gene and genotype/phenotype correlations in severe methylenetetrahydrofolate reductase deficiency. Am J Hum Genet. 1995; 56(5): 1052-1059. PubMed | Google Scholar
- Alghasham A, Settin AA, Ali A, Dowaidar M, Ismail H. Association of MTHFR C677T and A1298C gene polymorphisms with hypertension. Int J Health Sci. 2012; 6(1): 3-11. PubMed | Google Scholar
- Hanson NQ, Aras O, Yang F, Tsai MY. C677T and A1298C Polymorphisms of the Methylenetetrahydrofolate Reductase Gene: Incidence and Effect of Combined Genotypes on Plasma Fasting and Post-Methionine Load Homocysteine in Vascular Disease. Clin Chem. 2001; 47(4): 661-666. PubMed | Google Scholar
- Tosson AM, Amr KS, Taher MB. Polymorphisms in folate-metabolizing genes as risk factors for congenital heart defects in Down syndrome in Egypt. Int J BiolRes. 2015; 6 (12): 963-966. Google Scholar
- Adams GT, Snieder H, McKie VC, Clair B, Brambilla D, Adams RJ et al. Genetic risk factors for cerebrovascular disease in children with sickle cell disease: design of a case-control association study and genomewide screen. BMC Med Genet. 2003 Jul 18; 4: 6. PubMed | Google Scholar
- Vinchinsky EP, Styles LA, Colangelo LH, Wright EC, Castro O, Nickerson B. Acute chest syndrome in sickle cell disease: Clinical presentation and course. Blood. 1997; 89(5): 1787.
- Driss A, Asare KO, Hibbert JM, Gee BE, Adamkiewicz TV, Stiles JK. Sickle cell disease in the Post Genomic Era: A Monogenic Disease with a Polygenic Phenotype. Genomics Insights. 2009; 2009 (2): 23-48. PubMed | Google Scholar
- McLaughlin JF, Ballas SK. High mortality among children with sickle cell anemia and overt stroke who discontinue blood transfusion after transition to an adult program. Transfusion. 2016 May; 56(5): 1014-21. Epub 2015 Nov 23. PubMed | Google Scholar
- Ogun GO, Ebili H, Kotila TR. Autopsy findings and pattern of mortality in Nigerian sickle cell disease patients. The Pan African Medical Journal. 2014; 18: 30. eCollection 2014. PubMed | Google Scholar
- Platt OS, Brambilla DJ, Rosse WF, Milner PF, Castro O, Steinberg M et al. Mortality in Sickle Cell Disease -- Life Expectancy and Risk Factors for Early Death. N Engl J Med. 1994; 330(23): 1639-1644. PubMed | Google Scholar
- Gray A, Anionwu EN, Davies SC, Brozovic M. Patterns of mortality in sickle cell disease in the United Kingdom. J Clin Pathol. 1991; 44(6): 459-463. PubMed | Google Scholar
- Couto FD, Boas WV, Lyra I, Zanette A, Dupuit MF, Almeida MN et al. A C677T methylenetetrahydrofolate reductase (MTHFR) polymorphism and G20210A mutation in the prothrombin gene of sickle cell anemia patients from Northeast Brazil. Hemoglobin. 2004; 28(3): 237-241. PubMed | Google Scholar
- Rahimi Z, Merat A, Gerard N, Krishnamoorthy R, Nagel RL. Implications of the genetic epidemiology of globin haplotypes linked to the sickle gene in Southern Iran. Hum Biol. 2006; 78(6): 719-731. PubMed | Google Scholar
- Alves Jacob M, da Cunha Bastos C, Regina Bonini-Domingos C. The 844ins68 cystathionine beta-synthase and C677T MTHFR gene polymorphism and the vaso-occlusive event risk in sickle cell disease. Arch Med Sci. 2011 Feb; 7(1): 97-101. Epub 2011 Mar 8. PubMed | Google Scholar
- Wald DS, Law M, Morris JK. Homocysteine and cardiovascular disease: evidence on causality from a meta-analysis. BMJ. 2002; 325(7374): 1202-10. PubMed | Google Scholar
- Shmeleva VM, Kapustin SI, Papayan LP, Sobcynska-Malefora A, Harrington DJ, Savidge GF. Prevalence of hyperhomocysteinemia and the MTHFR C677T polymorphism in patients with arterial and venous thrombosis from North Western Russia. Thromb Res. 2003; 111(6): 351-8. PubMed | Google Scholar
- Hernigou P, Habibi A, Bachir D, Galacteros F. The natural history of asymptomatic osteonecrosis of the femoral head in adults with sickle cell disease. J Bone Joint Surg Am. 2006 Dec; 88(12): 2565-2572. PubMed | Google Scholar
- Kutlar A, Kutlar F, Turker I, Tural C. The methylene tetrahydrofolate reductase (C677T) mutation as a potential risk factor for avascular necrosis in sickle cell disease. Haemoglobin. 2001; 25(2): 213-217. PubMed | Google Scholar
- Akinyoola AL, Adediran IA, Asaleye CM, Bolarinwa AR. Risk factors for osteonecrosis of the femoral head in patients with sickle cell disease. Int Orthop. 2009 Aug; 33(4): 923-6. Epub 2008 Jul 17. PubMed | Google Scholar
- Chang JD, Hur M, Lee SS, Yoo JH, Lee KM. Genetic background of nontraumatic osteonecrosis of the femoral head in the Korean population. Clin Orthop Relat Res. 2008 May; 466(5): 1041-6. Epub 2008 Mar 19. PubMed | Google Scholar
- Akinola NO, Stevens SM, Franklin IM, Nash GB, Stuart J. Subclinical ischaemic episodes during the steady state of sickle cell anaemia. J Clin Pathol. 1992 Oct; 45(10): 902-906. PubMed | Google Scholar
- Naing L, Winn T, Rusli BN. Practical Issues in Calculating the Sample size for Prevalence Studies. Arch of OrofSci. 2006; 1: 9-14. Google Scholar
- Daniel WW. Biostatistics: A foundation for analysis in the health sciences. 7th Edition, John Wiley & Sons, Inc., Hoboken. 1999. Accessed on 21 July 2019.
- Matthews RG. Methylenetetrahydrofolate Reductase: A Common Human Polymorphism and Its Biochemical Implications. The Chem Rec. 2002; 2(1): 4-12. PubMed | Google Scholar
- Franco RF, Araijo AG, Guerreiro JF, Eliom J, Zago MA. Analysis of the 677 C-->T mutation of the methylenetetrahydrofolate reductase gene in different ethnic groups. ThrombHaemost. 1998; 79: 119-21. PubMed | Google Scholar
- Adekile AD, Kutlar F, Haider MZ, Kutlar A. Frequency of the 677 C-->T mutation of the methylenetetrahydrofolate reductase gene among Kuwaiti sickle cell disease patients. Am J of Hematol. 2001; 66(4): 263-266. PubMed | Google Scholar
- Andrade FL, Annichino-Bizzacchi JM, Saad ST, Costa FF, Arruda VR. Prothrombin mutant, factor V Leiden, and thermolabile variant of methylenetetrahydrofolate reductase among patients with sickle cell disease in Brazil. Am J Hematol. 1998 Sep; 59(1): 46-50. PubMed | Google Scholar
- Zimmerman SA, Ware RE. Inherited DNA mutations contributing to thrombotic complications in patients with sickle cell disease. Am J Hematol. 1998 Dec; 59(4): 267-272. PubMed | Google Scholar
- Frosst P, Blom H, Milos R, Goyette P, Sheppard CA, Matthews RG et al. A candidate genetic risk factor for vascular disease: a common mutation in the methylenetetrahydrofolate reductase gene. Nat Genet. 1995 May; 10(1): 111-113. PubMed | Google Scholar
- Schneider JA, Rees DC, Liu YT, Clegg JB. Worldwide distribution of a common methylenetetrahydrofolate reductase mutation (letter). Am J Human Genet. 1998; 62(5): 1258-60. PubMed | Google Scholar
- Pepe G, Camacho-Vanegas O, Guisti B, Brunelli T, Marcucci R, Attanasio M et al. Heterogeneity in world distribution of the thermolabile C677T mutation in 5,10-methylenetetrahydrofolate reductase. Am J Human Genet. 1998; 63(3): 917-20. PubMed | Google Scholar
- Castro R, Rivera I, Ravasco P, Jakobs C, Blom HJ, Camilo ME et al. 5, 10-methylenetetrahydrofolate reductase 677C T and 1298A C mutations are genetic determinants of elevated homocysteine. Q J Med. 2003 Apr; 96: 297-303. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
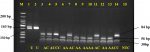 Figure 2: agarose gel representation of A1298C genotyping; M represents the DNA marker (50-700 bp); lanes 1 and 2 are undigested PCR products (163 bp); lanes 3, 4, 7 and 11 show AC genotype (84, 56, and 30bp); lanes 5 and 14 show the CC genotype (84 and 30 bp); lanes 6, 8-10, 12, and 13 show AA genotype (56 and 30 bp); U = undigested PCR product; NTC = non-template control
Figure 2: agarose gel representation of A1298C genotyping; M represents the DNA marker (50-700 bp); lanes 1 and 2 are undigested PCR products (163 bp); lanes 3, 4, 7 and 11 show AC genotype (84, 56, and 30bp); lanes 5 and 14 show the CC genotype (84 and 30 bp); lanes 6, 8-10, 12, and 13 show AA genotype (56 and 30 bp); U = undigested PCR product; NTC = non-template control