Ramsay Hunt syndrome
Yaseer Muhammad Tareq Khan, Nishat Fatema
Corresponding author: Yaseer Muhammad Tareq Khan, Department of Acute Internal Medicine, East Surrey Hospital, Surrey and Sussex Healthcare NHS Trust, Canada Ave, Redhill RH1 5RH, United Kingdom 
Received: 21 May 2019 - Accepted: 11 Nov 2019 - Published: 16 Dec 2019
Domain: Emergency medicine
Keywords: Ramsay Hunt syndrome, herpes zoster oticus, facial nerve palsy
©Yaseer Muhammad Tareq Khan et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yaseer Muhammad Tareq Khan et al. Ramsay Hunt syndrome. Pan African Medical Journal. 2019;34:201. [doi: 10.11604/pamj.2019.34.201.19207]
Available online at: https://www.panafrican-med-journal.com//content/article/34/201/full
Ramsay Hunt syndrome
Yaseer Muhammad Tareq Khan1,&, Nishat Fatema2
1Department of Acute Internal Medicine, East Surrey Hospital, Surrey and Sussex Healthcare NHS Trust, Canada Ave, Redhill RH1 5RH, United Kingdom, 2Department of Obstetrics and Gynecology, Imperial Hospital Limited, Chittagong, Bangladesh
&Corresponding author
Yaseer Muhammad Tareq Khan, Department of Acute Internal Medicine, East Surrey Hospital, Surrey and Sussex Healthcare NHS Trust, Canada Ave, Redhill RH1 5RH, United Kingdom
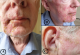
A 63-year-old man presented to our hospital with 2 days history of right-sided earache and numbness followed by the development of vesicular rash involving the right side of the face. There was no history of headache, tinnitus, giddiness or hearing impairment. Neurological examination revealed right-sided mild lower motor neuron type facial palsy (A) and vesicular rash in the distribution of maxillary and mandibular branch of trigeminal nerve without any sensorineural deafness (B, C). Routine all laboratory examinations including retroviral screening were normal. A clinical diagnosis of the Ramsay Hunt syndrome (RHS) was considered based on earache, facial paralysis and typical dermatomal distribution of rash. He was started with oral valaciclovir 1gm three times daily (TDS) for 7 days and Tab prednisolone 60mg daily for 5 days. Two days after initiation of the treatment vesicular lesions disappeared but neurological examination revealed right-sided grade IV facial nerve palsy. Ramsay Hunt syndrome or Herpes Zoster Oticus is characterized by reactivation of latent varicella zoster virus in the geniculate ganglion and subsequent spread to cranial nerve. The diagnosis is mainly clinical. The facial paralysis seen in Ramsay Hunt syndrome is often more severe with the increased rate of late neural denervation and decrease the chance of complete recovery.
Figure 1: A) ipsilateral (right) mild facial palsy; B) multiple vesicular lesions over right side of the face; C) preauricular vesicular rash