Psychiatric disorders in the acoustic neuroma: about a case
Samira Younes, Sabria Khouadja, Samia Younes, Rim Ben Soussia, Walid Bouali, Ahmed Haj Mohamed, Lazhar Zarrouk
Corresponding author: Sabria Khouadja, Department of Psychiatry, University Hospital of Tahar Sfar, Mahdia, Tunisia 
Received: 11 Feb 2019 - Accepted: 22 May 2019 - Published: 04 Jun 2019
Domain: Psychiatry
Keywords: Neurofibromatosis type 2, vestibular schwannoma, acoustic neuroma, hearing loss, psychiatry, psychosis
©Samira Younes et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Samira Younes et al. Psychiatric disorders in the acoustic neuroma: about a case. Pan African Medical Journal. 2019;33:80. [doi: 10.11604/pamj.2019.33.80.18398]
Available online at: https://www.panafrican-med-journal.com//content/article/33/80/full
Psychiatric disorders in the acoustic neuroma: about a case
Samira Younes1, Sabria Khouadja1,&, Samia Younes2, Rim Ben Soussia1, Walid Bouali1, Ahmed Haj Mohamed1, Lazhar Zarrouk1
1Department of Psychiatry, University Hospital of Tahar Sfar, Mahdia, Tunisia, 2Department of Neurology, University Hospital of Tahar Sfar, Mahdia, Tunisia
&Corresponding author
Sabria Khouadja, Department of Psychiatry, University Hospital of Tahar Sfar, Mahdia, Tunisia
Neurofibromatosis type 2 (NF2) is a rare autosomal dominant disorder characterized by formation of central nervous system tumors. They are associated to significant morbidity due to multiple problems such as hearing loss that can lead to many psychiatric disorders.
Within the clinical picture of neurofibromatosis type 2 (NF2), vestibular schwannomas (or acoustic neuromas) are usually those with the greatest repercussion on a patient's quality of life. Given that patients can show non-specific symptoms for a long time, the diagnosis of the disease can be delayed for several years.
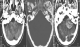
This is the case of a 21 year old patient who was admitted to our ward under the state hospitalization mode for instability, emotional and behavioral disorder. Our patient had a medical history of a one-sided deafness treated with a hearing prosthesis. For his psychiatric history, he was followed irregularly by a free-lance psychiatrist. The beginning of trouble dated back to 3 years marked by the installation of behavioral disorders such as fugue, agitation, irritability, sleep disorder and physical carelessness. A worsening of symptoms is 3 months, stated by the appearance of hostility and delusion of persecution towards his mother. The patient declines to eat the food that his mother cooked for him. He threatened her with a knife and he asked his sister to rewash his clothes. Overall, the clinical overview includes a delirium, clastic agitation strikes, emotional lability, cerebral ataxia and conjunctival hyperemia. A brain scanner was requested because of clinical presentation and the normality of laboratory tests, but also psychotropic intolerance including antipsychotics. The brain scan showed an association of bilateral acoustic neuromas, cavernous and intraventricular meningioma (Figure 1). These clinical and radiological signs met the diagnosis criteria for NF2 according to the consensus conference of the National Institute of Health in Bethesda established in the USA in 1988.
NF2, secondary to a defection in chromosome 22, is characterized by the appearance of schwannomas of the 8th cranial nerve, as well as ocular alterations and meningiomas. NF2 is a rare clinical entity. According to recent studies, incidence of 1:25 000 and prevalence greater than 1:80 000 are estimated [1, 2]. The onset of NF2 is usually around 18-24 years, although the range is from birth to 70 years [3]. The most common symptoms are the appearance of neurological, ocular and cutaneous. Among the neurological lesions, the most observed characteristics are bilateral vestibular schwannomas. Initial symptoms include tinnitus, hearing loss and alterations in balance that begin insidiously; however, hearing loss may occur suddenly [4]. Treatment for the various symptoms of NF2 is similar for sporadic tumors of the same type. However, multidisciplinary management is obligatory to minimize disabilities and to avoid morbidity secondary to treatment of these tumors. The main prognostic factors are mean age at diagnosis, presence of intracranial meningiomas and treatment in specialized centers [5].
�
Hearing aids may be helpful early in the course of the disease [6]. The treatment of hearing loss should include patient referral to an audiologist and for lip-reading training, as well as hearing aids like cochlear implants or brainstem implants [6]. Kraepelin [7] was the first to describe the presence of paranoia and persecutory delusions in patients with impaired hearing. In a more recent meta-analysis of epidemiologic studies, the investigators found an increased risk of hearing impairment for all psychosis outcomes, such as hallucinations, delusions, psychotic symptoms and delirium, although the odds ratios were relatively small. Early exposure to hearing impairment led to elevate the risk of later development of schizophrenia. The investigators suggested that potential mechanisms underlying this association include loneliness and disturbances of source monitoring (locating the source of sounds and interpreting these sounds) [8]. In another study, self-reported hearing impairment was associated with increased frequency of psychotic symptoms among those using a hearing aid in younger persons but not older adults [9].�
Depression is a particularly important construct to examine given anecdotal evidence from a number of treatment centers of increased rates of suicide among acoustic neuroma patients compared to the general population [10]. Furthermore, in a recent focus group study among acoustic neuroma patients, an association was found between severe postoperative headaches, depression and suicidal ideation [11]. Thomas and colleagues [12] found a fourfold increase in scores above a clinically significant cutoff for anxiety and depression symptoms among patients with a hearing impairment compared with the general population. In another study among community respondents in underserved areas and using self-rated scales, subjects who reported sensory loss had high rates of depression and a compromised quality of life compared with respondents without these impairments [13]. In yet another study, investigators explored the associated relationship of hearing impairment with anxiety symptoms. They found that, compared with individuals with no hearing impairment, the odds of prevalent anxiety were significantly higher among individuals with mild hearing impairment, and for those with moderate or severe impairment the odds were even greater. Hearing aid use was not significantly associated with lower likelihood of anxiety [14].
Early diagnosis, multidisciplinary management in specialized units and improvements in treatment could increase hope and quality of life for the patients.
The authors declare no competing interests.
All authors have contributed to this article and have read and agreed to the final manuscript.
Figure 1: axial section of the brain scan showing tumor of the left cerebellopontine angle extending to the left auditory meatus
- Evans DG, Moran A, King A, Saeed S, Gurusinghe N, Ramsden R. Incidence of vestibular schwannoma and neurofibromatosis2 in the North West of England over a 10-year period: higher incidence than previously thought. Otol Neurotol. 2005; 26(1): 93-97. PubMed | Google Scholar
- Antinheimo J, Sankila R, Carp�n O, Pukkala E, Sainio M, J��skel�inen J. Population-based analysis of sporadic and type 2 neurofibromatosis-associated meningiomas and schwannomas. Neurology. 2000; 54(1): 71. PubMed | Google Scholar
- Evans DG, Huson SM, Donnai D, Neary W, Blair V, Newton V et al. Clinical study of type 2 neurofibromatosis. Q J Med. 1992 Aug; 84(304): 603-618. PubMed | Google Scholar
- Evans DGR. Neurofibromatosis 2 (Bilateral acoustic neurofibromatosis, central neurofibromatosis, NF2, neurofibromatosis type II). Genet Med. 2009 Sep; 11(9): 599-610. PubMed | Google Scholar
- P�rez-Grau M, Mir� N, Prades J, Verg�s J, Lareo S, Roca-Ribas F. Neurofibromatosis type 2. Acta Otorrinolaringol Esp. 2010 Jul-Aug; 61(4): 306-311. Epub 2010 Feb 6. PubMed
- Evans DG, Baser ME, O'Reilly B, Rowe J, Gleeson M, Saeed S et al. Management of the patient and family with Neurofibromatosis 2: a consensus conference statement. Br J Neurosurg. 2005 Feb; 19(1): 5-12. PubMed | Google Scholar
- Kraepelin, Emil. Psychiatrie. vol. IV. Barth Verlag, Leipzig. 1915; 1441.
- Linszen MM, Brouwer RM, Heringa SM, Sommer IE. Increased risk of psychosis in patients with hearing impairment: review and meta-analyses. Neurosci Biobehav Rev. 2016 Mar; 62: 1-20. PubMed | Google Scholar
- Van der Werf M, van Boxtel M, Verhey F, Jolles J, Thewissen V, Van Os J. Mild hearing impairment and psychotic experiences in a normal aging population. Schizophr Res. 2007 Aug; 94(1-3): 180-6. Epub 2007 May 23. PubMed | Google Scholar
- Farace E, Marshall LF. Quality of life in acoustics. J Neurosurg. 2003 Nov; 99(5): 807-808, discussion 808-9. PubMed | Google Scholar
- Brooker J, Burney S, Fletcher J, Dally M. A qualitative exploration of quality of life among individuals diagnosed with an acoustic neuroma. Br J Health Psychol. 2009 Sep; 14(Pt 3): 563-578. Epub 2008 Dec 3. PubMed | Google Scholar
- Thomas A. Acquired hearing loss: psychological and social implications. Orlando (FL): Academic Press; 1984.
- Armstrong TW, Surya S, Elliott TR, Brossart DF, Burdine JN. Depression and health-related quality of life among persons with sensory disabilities in a health professional shortage area. Rehabil Psychol. 2016 Aug; 61(3): 240-250. Epub 2016 Feb 18. PubMed | Google Scholar
- Contrera KJ, Betz J, Deal J, Choi JS, Ayonayon HN, Harris T et al. Association of hearing impairment and anxiety in older adults. J Aging Health. 2017 Feb; 29(1): 172-184. Epub 2016 Jul 8. PubMed | Google Scholar