Triplane fracture of the proximal tibia: a case report and literature review
Fekih Aymen, Othman Youcef, Saďdi Aymen, Aloui Issam, Abid Abderrazek
Corresponding author: Fekih Aymen, Department of Trauma and Orthopaedics Surgery Fattouma Bourguiba University Hospital, Monastir, Tunisia 
Received: 16 Dec 2018 - Accepted: 28 Mar 2019 - Published: 21 May 2019
Domain: Orthopedic surgery
Keywords: Proximal tibial triplane, physeal injury, child
©Fekih Aymen et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Fekih Aymen et al. Triplane fracture of the proximal tibia: a case report and literature review. Pan African Medical Journal. 2019;33:40. [doi: 10.11604/pamj.2019.33.40.17953]
Available online at: https://www.panafrican-med-journal.com//content/article/33/40/full
Triplane fracture of the proximal tibia: a case report and literature review
Fekih Aymen1,&, Othman Youcef1, Saďdi Aymen1, Aloui Issam1, Abid Abderrazek1
1Department of Trauma and Orthopaedics Surgery, Fattouma Bourguiba University Hospital, Monastir, Tunisia
&Corresponding author
Fekih Aymen, Department of Trauma and Orthopaedics Surgery Fattouma Bourguiba University Hospital, Monastir, Tunisia
Triplane fractures of the proximal tibia are less well known than the distal extremity. The diagnosis is based on a good analysis of X-rays and possibly CT images to better plan the management. The authors reports a triplane fracture of the proximal tibial in a 12 years old boy treated by closed reduction and internal fixation. To our knowledge, only a dozen cases have been reported in the literature with generally a good evolution of the fracture.
Triplane fracture of the proximal tibia occurs in three planes (transverse, sagittal and coronal) and it typically occurs in adolescence and crosses through the articular surface, the epiphysis, the physis and the metaphysis. Triplane fractures are known in the distal part of the tibia and were first described by Lynn in 1972 [1]. Triplane fractures in the proximal tibia are far less common than those in the distal tibial end, as was demonstrated in the current orthopaedics literature [2-5]. Diagnosis is generally easy with CT scan and treatment is most often surgical, especially in displaced fractures. In this report we describe a triplane fracture of the proximal tibial treated by closed reduction and internal fixation with good result at the last follow-up.
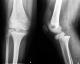
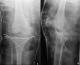
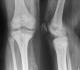
A 12-year-old boy with an overweight, consulted the emergency department after a closed trauma of the right knee following a fall from its own height. On examination, he has a painful and swollen knee with limited motion and there was no neurovascular abnormality. The antero-posterior radiograph revealed a fracture through the medial physis extending through the epiphysis classified Salter-Harris III (Figure 1 A). However, the lateral radiograph showed angulation and anterior displacement of the epiphysis classified Salter-Harris I (Figure 1 B). Unfortunately, the CT scan was not available that day, so we decided to operate the patient in emergency. Closed reduction was achieved under general anesthesia. The stabilization of the fracture was ensured by a horizontal pinning of the epiphysis and a cross pinning fixing the epiphysis to the metaphysis. A cast immobilization of 6 weeks was necessary to avoid any secondary displacement and to ensure a good consolidation of the fracture (Figure 2). After the removal of the pins, a functional rehabilitation was instituted to regain a good mobility of the knee. At the last one year follow up, the patient had no growth disturbance from injury (Figure 3) and had returned to normal activities with a good mobility of his knee (Figure 4).
Although the fractures of the epiphyseal cartilage injuries are common in the childhood, epiphyseal fractures involving the proximal tibia entities are very rare and account for 1 to 3% of all physeal injuries [6, 7]. Salter-Harris type I to V occur from both indirect and direct mechanism of injury [8]. In distal tibia, the triplane fracture occurs due to the asymmetrical closure of the physis, from central to antero-medial to posteromedial and finishing with closure of the lateral margin of the physis. The proximal tibial physis has a more symmetrical closure, which may explain the rarity of a triplane fracture in this location [5]. Another theory in favor of this rare situation is related to the attachments of the medial and lateral collateral ligaments which result in the stresses from the knee being transmitted to the metaphysis and not the epiphysis [3]. That's why the mostly triplane fractures consist of a coronal fracture of the metaphysis, a transverse fracture of the physis and a sagittal intra-articular fracture of the epiphysis. In practical terms, most triplane fracture are easily diagnosed by plain film radiography. The value of Computed Tomography(CT) especially 3D reconstruction for defining the injury pattern and preoperative planning in these rare and technically demanding cases is highlighted [3, 5]. In triplane fractures involving the proximal tibia, the Magnetic Resonance Imaging (MRI) scan has probably more significant value than the CT scan, as tibial plateau fractures may be associated with cruciate ligament and meniscal tears [9]. We did not perform neither CT scan nor MRI scan because the diagnosis is obvious and imaging was not available that day. The primary goals of treatment are anatomic reduction of the articular fragments with avoidance of further injury to the growth plate. Fracture stabilization is ensured either by screws or by pins. According to some authors [9, 10] the control of the reduction can be performed by knee arthroscopy. The advantages of this arthroscopic reduction are complete evacuation of hemarthrosis, diagnostic evaluation of the cruciate ligaments, the meniscus and the metaphyseal part of the fracture lines extend through the physis into the epiphysis and the joint [4, 5]. A cast immobilization is recommended for at last 6 weeks to prevent secondary displacement and obtain a good consolidation.
Proximal tibial triplane fractures are rare injuries but carry with them the need for clinical vigilance. These fractures are high energy injuries that can result in multiple intra-articular and physeal fragments that require individual anatomic reduction and stabilization in order to prevent future arthritis, pain, and deformity. Because of the involvement of the physeal growth plate, long-term radiographic follow-up of the affected extremity is necessary to treat any angular deformity or leg length difference that might occur.
The authors declare no competing interests.
All authors have read and agreed to the final version of this manuscript and have equally contributed to its content and to the management of the case.
Figure 1: (A) anteroposterior
radiograph of the right knee demonstrating Salter-Harris III
fracture fragment; (B) lateral radiograph of the right knee demonstrating
Salter-Harris I fracture
fragment and anterior displacement of the epiphysis
Figure 2: (A) post-operative anteroposterior and lateral (B) radiographs of the right knee
Figure 3: (A) anteroposterior and lateral (B) radiographs of the right knee with consolidation of the fracture at the last one year follow up
Figure 4: normal flexion of the right knee at the last one year follow up
- Lynn MD. The triplane distal tibial epiphyseal fracture. Clin Orthop. 1972; 86: 187. PubMed | Google Scholar
- Pietu G, Cistac C, Letenneur J. Triplane fractures of the upper head of tibia: à propos of two cases. Rev Chir Orthop Reparat Appareil Moteur. 1991; 77(2): 121. PubMed | Google Scholar
- Conroy J, Cohen A, Smith RM, Matthews S. Triplane fracture of the proximal tibia. Injury. 2000; 31(7): 546-548. PubMed | Google Scholar
- Hermus JP, Driessen MJ, Mulder H, Bos CF. The triplane variant of the tibial apophyseal fracture: a case report and a review of the literature. J Pediatr Orthop B. 2003; 12(6): 406-8. PubMed | Google Scholar
- Strelzow J, Aarvold A, Reilly CW. Triplane Fracture of the Proximal Tibia: a case report and literature review. Case Rep Orthop. 2017; 2017: 6490728. PubMed | Google Scholar
- Ogden JA, Tross RB, Murphy MJ. Fractures of the tibial tuberosity in adolescents. The Journal of Bone & Joint Surgery-American. 1980; 62(2): 205-215. PubMed | Google Scholar
- Mubarak SJ, Kim JR, Edmonds EW, Pring ME, Bastrom TP. Classification of proximal tibial fractures in children. J Child Orthop. 2009; 3(3): 191-197. PubMed | Google Scholar
- Zionts LE. Fractures around the knee in children. Journal of the American Academy of Orthopaedic Surgeons. 2002; 10(5): 345-355. PubMed | Google Scholar
- Wiedemann M. Dislocation fracture of the head of the tibia. II. Therapeutic procedure. Unfallchirgie. 1995; 21(4): 188-197. PubMed | Google Scholar
- Lobenhoffer P. Minimally invasive knee joint surgery. ZentralblChir. 1997; 122(11): 974-985. PubMed | Google Scholar