Cleft & facial deformity foundation (CFDF) outreach model: 6 year experience of an indigenous Nigerian mission in the surgical correction of facial clefts
Seidu Adebayo Bello, Saliu Adejumobi Balogun, Ifeoluwa Oketade, Nosa Ighile, Ntiense Udoh, Deborah Enebong
Corresponding author: Seidu Adebayo Bello, Cleft & Facial Deformity Foundation, Abuja, Nigeria 
Received: 28 Jul 2014 - Accepted: 31 Jan 2018 - Published: 10 Feb 2018
Domain: Clinical medicine
Keywords: Surgical correction, facial clefts, Nigerian, indigenous, surgical mission
©Seidu Adebayo Bello et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Seidu Adebayo Bello et al. Cleft & facial deformity foundation (CFDF) outreach model: 6 year experience of an indigenous Nigerian mission in the surgical correction of facial clefts. Pan African Medical Journal. 2018;29:109. [doi: 10.11604/pamj.2018.29.109.5092]
Available online at: https://www.panafrican-med-journal.com//content/article/29/109/full
Original article 
Cleft & facial deformity foundation (CFDF) outreach model: 6 year experience of an indigenous Nigerian mission in the surgical correction of facial clefts
Cleft & facial deformity foundation (CFDF) outreach model: 6 year experience of an indigenous Nigerian mission in the surgical correction of facial clefts
Seidu Adebayo Bello1,2,&, Saliu Adejumobi Balogun1,3, Ifeoluwa Oketade1,4, Nosa Ighile1,5, Ntiense Udoh1,5, Deborah Enebong1,5
1Cleft & Facial Deformity Foundation, Abuja, Nigeria, 2Oral and Maxillofacial Surgeon State House Medical Centre, Abuja, Nigeria, 3Out Centre for Health and Social Research, Lagos, Nigeria, 4Dental Clinic and Research Centre, Abuja, Nigeria, 5State House Medical Centre, Abuja, Nigeria
&Corresponding author
Seidu Adebayo Bello, Cleft & Facial Deformity Foundation, Abuja, Nigeria
Introduction: orofacial cleft has a worldwide distribution but it is peculiar in the developing countries due to poor healthcare facility with resultant high incidence of unoperated adult cleft. Various model of surgical mission by foreign experts had existed to combat this menace. The indigenous rotatory model by Cleft & facial deformity foundation is hereby presented.
Methods: carrying out an outreach programme in a rural area begins with the identification of a hospital with optimum facility, followed by effective awareness campaign, then a pre- surgical meeting with the hospital management. Personnel, equipment and materials were mobilised to the site while surgery usually lasted one week.
Results: seventeen outreach programmes were carried out in 10 different hospitals from March 2011 to June 2017. There were 546 orofacial cleft patients, 280 (51.3%) males and 266 (48.7%) females. The age ranged between 1 week to 70years with a mean age ± (SD) of 9.3±11.5. Four hundred and forty eight (82.1%) of the cleft patients were operated. Three hundred and twenty two (59.0%) patients were treated under general anaesthesia while 126 (23.1%) were treated under local anaesthesia. Eight surgeons and 4 anaesthetics were trained during the study period with several local practitioners benefitting from exposure to standard practice. Standard techniques were employed for cheiloplasty and palatoplasty. Minor complications were recorded with one mortality.
Conclusion: this model is an effective and efficient way of reaching out to the poor patients with orofacial cleft. Effective mobilization, large volume of safe and quality surgery, easy knowledge transfer and possibility of patient review are some of its advantages. With regular training and funding, it could be an effective way of minimising ignorance and eradicating adult cleft in Nigeria and other developing societies.
Orofacial cleft is a congenital disease with a worldwide distribution. Africa population is the least affected, [1] but peculiar because of high level of ignorance and poverty [2,3]. The aetiology is complex and likely to have both genetic and environmental factors [4,5]. The surgical literature is consistent in recommending early repair of orofacial cleft, typically completing primary repair of the lip and palate by the age of two years. This is a mirage in developing countries due to poverty. Surgical missions have been variously described as "outreach", "medical brigades", "volunteer trips", and "'humanitarian assistance" [6]. In a review of articles published over 25 years (1985-2009), mission sending are dominated by four countries-USA, Canada, United Kingdom, and Australia while receiving countries include South and central America, Asia and regional African [6,7]. Surgical missions have always been a means of assisting the predominantly poor patients in the resource limited developing countries by the more technologically advanced specialists from the western world [8-10]. Several models of surgical missions for the repair of orofacial defects have been described. Under the auspices of "Impact Foundation Bangladesh", non-governmental organisation based in Dhaka, Bangladesh, some American surgeons carried out 3 surgical missions between 2006 and 2008 [2]. A Dutch/German based non-profit organization; "NOMA foundation" established a Noma Hospital at the northern part of Nigeria and carry out a regular surgical mission on noma and other orofacial defects including facial clefts. In January 2002, the Mobile Cleft Lip Camp was established in Bangladesh by local doctors and nurses [11]. With support from Smile-Train, GS memorial plastic surgery hospital in India carried out outreach programmes to mobilise patient from the rural areas to the hospital for operation [12]. In October 2006, a US surgical team affiliated with the organization "'Operation of Hope" worked with physicians and nurses in Harare Central Hospital (HCH), Zimbabwe to evaluate 63 patients with orofacial clefts while other missions have been reported from Ghana [5,13]. Establishment of 'The Smile Train' by Charles Wang and Brian Mullaney in 1999 in USA with the sole aim of assisting the orofacial cleft patients all over the world appears to have changed the face of surgical mission. The Smile Train did not believe in taking missionary surgeons to the place of need to operate upon cleft children. Instead, it believed in improving the infrastructure and training so that local hospitals and doctors could take care of their own patients [12]. Free surgical missions is a common phenomenon in developing countries and it is typically carried out by specialists from developed countries, [2] with a few report of local initiatives [11,13]. This study was conceived to document the experience of a local initiative for knowledge dissemination and reference among medical community, as well as sensitising the fast growing population of medical specialists in the developing world.
Historical background
�
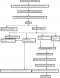
Cleft & Facial Deformity Foundation Outreach Model (CFDFOM) was born in 2011, out of the founder's search for a domestic approach to the scourge of cleft lip and palate as well as other facial deformities, in Nigerian societies. The manpower is made up of the core volunteers and local hospital staff. The core volunteers are made up of a group of surgery related volunteer professionals drawn from different hospitals across Nigeria, and headed by the founder, Dr Seidu Adebayo Bello. He is a Nigeria based Oral and Maxillofacial Surgeon, a fellow of both West African College of Surgeons and Nigeria Postgraduate Medical College, with wide training experience locally and abroad. The Anaesthesia is coordinated by Mr Ntiense E. Udoh and Zherem Dagett, holders of a diploma in anaesthesia with more than 20 year experience in anaesthesia locally and abroad. A rural hospital with relatively adequate theatre, laboratory and ward facilities was selected for the programme. A comprehensive flow of activities of this model is shown in Figure 1. Following a decision to carry out a programme in a particular hospital, volunteers and patients were mobilized while the programme lasted one week. Most patients were usually discharged within the period while the few ones unfit for discharge were either left in the care of local staff or moved to a more advanced facility depending on the required expertise. The funding was borne by the founder, some individuals and corporate organizations with Smile-Train foundation and TY Danjuma Foundation.�
Presurgical activities�
Mobilisation of patients, hospital staff, equipment and materials�
Mobilisation of patients was carried out through radio and television advertisements, posters and handbills in English and local languages as well as traditional rulers, health ministries and local government councils system. The health department of local government councils and provincial health ministries has a mobilization unit that permeates different towns and villages within a council or a province. Similarly, the leader of the traditional rulers has a mobilisation unit that is coordinated by a palace secretary with a number of uniformed motorcycle riders in its employment. Posters and handbills in English and local languages were distributed through these mobilization units. Churches, mosques, markets and other public places were the other units of mobilization. Effective mobilization of the local hospital staff is very central to the success of an outreach programme. A meeting was always scheduled with the hospital management which is made up of the hospital chairman and the heads of every unit in the hospital. The meeting provided an opportunity to explain the concept of the organisation's programme which is an indigenous solution to the problems of Nigerians. These meetings have metamorphosed into a formal training session on the first day of the outreach programmes presently. The hospitals for the programme were chosen due to the presence of reasonably adequate theatre and ward facilities, including at least a functional anaesthetic machine, an operating table, the sterilising unit and ward beds. The foundation acquired 2 patient monitors (MINETRAY MEC 100) for the purpose of standardising practice and ensuring safety of operations. For every programme, cleft instruments, theatre consumables, anaesthetic drugs and postoperative drugs were mobilized to the hospital.�
Administrative office�
The organisation maintained a well-equipped administrative office at the hospital. It was coordinated by a secretary who also oversees other logistic issues like feeding of workers, hotel accommodation for core volunteers, ensuring availability of drugs and other miscellaneous activities. The administrative office was busy throughout the programme. It ensured the collation of patients' data from the screening centre; daily production of theatre operation lists as well as enquiry centre for old and new patients.�
Screening day 1�
Information to the public included an instruction to assemble at the designated hospital on the first day for screening. This approach eliminates the extra expenses incurred travelling to the hospital for screening by patients and core volunteers. Schematic flow of patients on screening day is shown in Figure 1. Documentations were carried out in standard hospital patients' case files. Screening ensured separation of patients as well as collation of data for research purposes. The surgically fit cleft and maxillofacial pathology patients were referred for laboratory investigation including basic haematology and biochemistry and thereafter proceeded to the wards for admission. The number of patients admitted on the screening day depended on the number of available bed space. Priorities were usually given to patients that came from a far distance and cleft palate patients who usually stay a little longer on bed. Subsequently, admission of patients was phased out as operated patients were discharged to maximise available bed spaces.�
Operating days and anaesthesia�
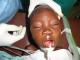
Operations proceeded smoothly with effective collaborative effort by different units. As a general guide, cheiloplasty in patients above 12 years were done under local anaesthesia using 2% xylocaine with 1/200000 adrenaline; 10-15ml was usually enough for a procedure. Cheiloplasty in patients below 12 years and palatoplasty in all patients were done under orotracheal intubation (Figure 2). Induction of anaesthesia in children was inhalational (with halothane), parenteral in adult while maintenance was done with isofluorane in all the patients. Adequate analgesia was ensured throughout the procedure. Monitoring and maintenance of stable essential parameters of ECG, blood pressure, oxygen saturation and temperature was done throughout the procedure with multi-parameter patient monitor (MINEDRAY MEC 1000 PORTABLE, Hamburg Germany). Careful drug selection of less depressant effect in premedication, induction, analgesia and maintenance of anaesthesia ensured awake extubation with early recovery of protective reflexes. All the patients were extubated within the operating room, kept in the recovery room for about 10 to 30 minutes and transferred to the wards accompanied with prophylactic broad spectrum antibiotics and analgesics. Thereafter, the nurses in the wards continued the management.�
Discharge and appointment�
Cleft lip patients were discharged 24 to 48 hours post-surgery except there was a complication, while cleft palate patients were discharged 72 to 96 hours. This practice ensured maximum utilization of the few available bed spaces in the hospital. All the discharges done during the week were temporary as all the patients reconvened on the eight day to be addressed together (Figure 3). They were equally given a review appointment which usually took place two months after the final discharge. Patients were all informed on how to reach the chief surgeon in case of a complication.�
Two months follow up�
This follow up visit provided an opportunity for the surgeon to review the patients with a view to study the progress of healing and determine the next line of action. It also offered the foundation the opportunity of evaluating the quality of life of the patients post-surgery.
A total of 17 outreach programmes were carried out in 10 different hospitals from March 2011 to June 2017. They are located in Kuje, Bwari, Kwali, Karshi and the surrounding provinces of Kogi, Nassarawa, Niger, Taraba, Edo and Katsina. A total of 546 patients were in attendance, comprising 280 (51.3%) males and 266 (48.7%) females. Four hundred and forty eight (82.1%) patients were operated while 98 (17.9%) were not. There were 516 (94.5%) typical orofacial cleft patients while 30 (5.5%) were atypical cleft. The age range of the patients was 1 week to 70 years with a mean age ± (SD) of 9.4±11.9 years. One hundred and ninety six (35.9%) patients were less than 2 years, 176 (32.2%) were between 2 and 10 years, 160 (29.3 %) were between 10 and 40 years, while 14(2.6 %) were more than 40 years. The pattern of cleft presentation is shown in Table 1. One hundred and forty four (26.4%) patients got the information about the programme through friends, 114 (20.9%) by radio/television, 83 (15.2%) by handbills and posters while 84 (15.4%) got it through other means including church, mosque and traditional rulers.
�
Four hundred and forty eight (82.1%) of the cleft patients were operated while 98 (17.9%) could not be operated for reasons including underage, low PCV occasioned by undernutrition and anaesthetic challenge in one case. The surgical procedures were: primary cheiloplasty 349 (63.9%), secondary cheiloplasty 12 (2.2%), primary palatoplasty 61 (11.2%), secondary palatoplasty 4 (0.7%), primary cheiloplasty and palatoplasty 1(0.2%) and anatomic repair 27 (4.9%). The Method of repairs employed is shown in Table 2. Tessier class cases were repaired with a local flap (anatomical repair) while the only lower lip defect was repaired with V shaped plasty. Three hundred and twenty two (59.0%) patients were treated under general anaesthesia while 126 (23.1%) were treated under local anaesthesia. The duration of admission, calculated from surgery to discharge day, ranged from 1-10 days with mean SD 3.3±2.5 days. Most cases of cheiloplasty in adults were given temporary discharge within 48 hours of surgery while only one case of facial cleft repaired with a transposition flap was transferred to an advanced facility and was discharged after 9 days. Eight surgeons and 4 anaesthetics were trained during the study period with several local practitioners benefitting from exposure to cleft lip and palate surgeries. There were 4 cases of failed intubation experienced in babies ranging between 3 and 8 months with wide complete cleft lip and palate. Three were successfully operated 6 months later while the last was lost to follow up. Prolonged recovery up to 40mins was observed in three cases and they were thought to be due to hypothermia. There was fluid aspiration in one patient whose mother broke the preanaesthetic fasting rule, leading to cancellation of the palatoplasty after resuscitation. One case of mortality was recorded in a 5 year old cleft palate who developed complication of anaesthesia but was lost later at the intensive care unit of the hospital. One hundred and fifty five (34.6%) patients turned up for review while 293 (65.4%) did not. Improved speech, self-worth, better psychological feelings and acceptance in the society have been reported by the patients as compared to their pre-surgery experience. Persistent bleeding associated with wound dehiscence was recorded in 8 (2.7%) patients. The dehiscence was found to be due to rotated and proclined upper incisors in 4 (1.4%) adult cleft cases and it resolved with teeth extraction and secondary closure. Mild wound dehiscence due to infection was recorded in another 4 (1.4%) patients. Formation of hypertrophy scar was recorded in 15(5.1) patients especially following wound dehiscence and healing by secondary intention. Palatoplasty recorded the highest complication with fistula formation in 5 (14.7%) and flap necrosis in one (2.9%) case.
Significance and challenges of CFDF outreach rotatory of care
�
Free surgical mission is a common phenomenon in developing countries and it is typically carried out by specialists from developed countries, [2] with a few report of local initiatives [11,13]. CFDF model is a wholly indigenous concept to tackle the scourge of facial deformity in Nigerian society; especially adult unoperated orofacial cleft patients. It is made up of professionals that have adopted the concept of volunteering (Figure 4). Several editorials in the medical and social sciences literature have raised important questions about potential unintended consequences of short-term medical volunteer work abroad [14-17]. They raised concern about the ability of short-term volunteers to provide safe and effective medical services in the setting of language and cultural barriers that impair clear communication between patients and health-care providers. As Nigerians, it is easy to understand the geopolitical considerations, secure necessary approval with little effort from approving authorities, and map out mobilization strategy. Unlike foreigners, long term planning is not necessary to actualize an outreach programme, neither is an intermediary organisation necessary. Ease of communication with the local healthcare providers and patients facilitate logistics and patients' management at reasonably low cost. Mobilisation is an important aspect of a surgical mission. Our model ensures dissemination of information to the grassroot. Forty-two per cent of the patients received the information through hand delivered posters and friends while another 20.9% were informed through television and radio. While wondering how patients could remain unaware of the cleft care facilities in the areas where centres have existed for several years, Singh [12] concluded that such rural patients are extremely poor, illiterate, keep company of uneducated people, and do not read newspapers or watch TV. They get interested only if they are fortunate enough to be informed of this facility by a trusted relative or friend who has witnessed the miracles of cleft care in her family, village or community. In a review of foreign mission to Guatemala by the Americans, every interviewee expressed appreciation for the service that visiting teams provided to their communities and many acknowledged the personal sacrifices that individual volunteers made in order to provide these services [7]. However some local health workers perceived them as possessing attitudes that foster dependence and lack respect for local practitioners and local knowledge and practices related to health. The need to integrate local workers was emphasised for a successful outreach programme. Even though doctors on foreign mission have local training as a top priority, some local practitioners don't regard them as equal partners thereby creating a barrier to training. This barrier is completely broken by this model such that local doctors, anaesthetist and nurses learn freely and consequently join the team as permanent volunteers. CFDF outreach model is a rotatory model that takes surgical mission to rural areas of Nigeria, creating awareness and carrying out surgical repairs. In comparison, one model mobilises patients from rural areas and carry out surgery at a particular location [12] while another model is the typical mission, as observed in Bangladesh where a foreign group carried out 3 surgical missions between 2006 and 2008 [2]. With this model under discussion, it was possible to execute 17 programmes within 6 years, created awareness in several communities and completed 449 operations. Taking surgical mission to the grassroot rural population resulted in impressive attendance by adults who had already lost hope of access to surgery due to extreme poverty, superstition and ignorance. Only 30.5% of the patients were less than 2 years, 41.2% were actually more than 10 years of age. Although no study to the best of our knowledge has made the observation, anedoctal evidence shows that more adult cleft patient attends surgical missions compared with hospital patients. Pattern of cleft presentation seen is not different from varying patterns already described in the literature.�
The surgical process at the outreach programme is similar to what is obtainable at the standard centres. Palatoplasty is generally more challenging and hence some surgical missions concentrate only on cheiloplasty. The standard nature of our practice made it possible to carry out palatoplasty successfully in our patients with minor complications (Figure 5, Figure 6). The 35% attendance recorded during review process with this model is impressive in the opinion of the authors. Patients are generally reluctant to go back to the hospital in Nigeria for review, especially when there was no obvious discomfort or complication. Follow-up care frequently came up as a major issue when considering why long-term presence is important after a foreign surgical mission [7]. In the review of foreign surgical mission in Guatemala by the Americans, one interviewee pointed out, "Most problems take longer than one week to fix without continuity and the care is not complete. In addition, many Guatemalan healthcare providers expressed willingness to provide the follow-up care to patients with whom they had personal contact, but stated that providing follow-up care to patients with whom they were unfamiliar could be problematic. In the CFDF outreach model, review process is an advantage which is possible because the volunteers are indigenous. The concept of multidisciplinary approach to the management of cleft lip and palate deformity is the standard worldwide. Zbar et al. [18] stated 'during the past three decades, it has become increasingly clear that successful cleft management requires a multidisciplinary, long-term, team approach. Patients with cleft lip and palate conditions, for example, need oral/maxillofacial surgeons for the initial surgical repair of the cleft lip/palate, with more post-surgical care often required. Patients can require follow-up future visits to plastic surgeons for minor repairs, orthodontists to repair damaged teeth and jaws, speech therapists to improve challenges with speech' care which they are unlikely to receive in their communities after the medical mission team departs [19,20]. This concept is obtainable to a limited extent in some parts of Nigeria especially where teaching hospitals are located. This is however lacking in most places, our area of practice inclusive, where surgery appears to be the main focus of care. The foundation has in its fold a paediatrician that screens the children and advice appropriately on nutrition. The awareness been created has started yielding results with some specialists like orthodontics and speech therapists showing interests. The foundation hopes to establish a centre in future where comprehensive care will be undertaken.�
This model is not without its challenges. Funding is a major issue because the surgical missions are carried out in hospitals without facilities for such operations. Patients' mobilisation; drugs, equipment and consumables acquisition; feeding and hotel accommodation for volunteers and other sundry materials require funding for successful operations. High level of distrust makes it difficult to have local funders. Even though it is cheaper than foreign mission, funding has always been a major consideration. When sharing accounts of his medical mission to Zimbabwe, Buchman wonders if 'the money that was spent on their stay could have been better spent on medical equipment, medications, or even basics such as food and housing' [21]. Abdullah asks "what business did our team of 10 members have spent approximately $30,000 toward travel and hotel costs, when the entire cost of building a new 30-bed wing for the hospital in Ghana was $60,000" [22].With regular funding of the indigenous mission by foreign and local organisations, the challenge is surmountable. Regular training of the volunteers is also a challenge which is necessary for effective and efficient service delivery. In a resource limited environment, this model provides effective management of resources while minimizing the scourge and stigmatization associated with cleft patients especially the adults who have reported a low self-esteem because of their condition. Organising the programme in the local hospitals reduce the travel cost by some of the beneficiaries which has been a hindrance, as reported by some of the patients. The frequency of the outreach programme also creates tremendous awareness in the various communities. Americans founded, in 2002, "Children's Health International Medical Project of Seattle" (CHIMPS), a resident-run, faculty-supported international medical program at El Salvador [23]. Using the experience gathered from the project, Suchdev et al [23] outlines 7 guiding principles for a successful mission including: mission, collaboration, education, service, teamwork, sustainability, and evaluation. From the foregoing, the model under consideration has substantially complied with these principles and hence could be a useful model.
Cleft & Facial Deformity Foundation employs the services of purely local medical practitioners for its outreach programmes but requires regular funding. Being conversant with the environment, political decisions like citing of a programme could be done quickly without an intermediary as obtainable with foreign missions. Effective mobilization, large volume of safe and quality surgery, easy knowledge transfer and possibility of patient review are some of the advantages of the model over the foreign based missions. Efforts should be made to establish a multidisciplinary cleft care centre in Nigeria; this will not only improve the quality of cleft care but also provides an avenue for training and research. With adequate training, good funding and available volunteers, it could be an effective and efficient way of minimising ignorance and eradicating adult cleft in Nigeria and African societies.
Authors declare no competing interest.
SA Bello, the founder and director of the organisation conceived the study and supervised the whole processes. All authors are volunteer members of the organisation and were all actively involved in the collection of data. SA Bello, Nosa Ighile, N. Udoh and DJ Enebong, S Balogun participated in literature search. S Balogun, I Oketade and SA Bello contributed to data collation and analysis. SA Bello, S Balogun, and N. Udoh participated in manuscript preparation. All authors read and approved the manuscript.
The following volunteer members of the organisation are acknowledged: Emmanuel Chong, Sanni Gora, Olayemi Balogun, Dr Maryam Keshinro, David Babatunde and Moridiyat Tiamiyu. We are greatly indebted to the approving authorities and hospital staff of various hospitals. We are equally grateful to individuals with little contributions in cash or kind for the actualisation of the outreach programmes especially Smile-Train Foundation, Maizube Nigerian Ltd. and TY Danjuma Foundation.
Table 1: pattern of orofacial cleft presentation among patients at the outreach programmes
Table 2: method of repairs among the cleft patients
Figure 1: schematic flow of activities in cleft & facial deformity foundation surgical outreach model
Figure 2: just completed left cheiloplasty under endotracheal intubation
Figure 3: a cross section of operated patients just before discharge
Figure 4: a cross section of volunteers
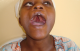
Figure 5: cleft palate before repairs
Figure 6: cleft palate two months post-surgery
- Vanderas AP. Incidence of Cleft Lip, Cleft Palate, and Lip and Palate Among Races: A review. Cleft Palate Journal.1987; 24(3):216-225. PubMed | Google Scholar
- Aziz SR, Rhee ST, Redai I. Cleft surgery in rural Bangladesh: reflections and experiences. J Oral Maxillofac Surg. 2009; 67:1581-1588. PubMed | Google Scholar
- Adeyemo WL, Ogunlewe MO, Desalu I et al. Cleft deformities in adults and children aged over six years in Nigeria: Reasons for late presentation and management challenges. Clinical, Cosmetic and Investigational Dentistry. 2009; 1:63-69. PubMed | Google Scholar
- Butali A, Mossey PA. Epidemiology of orofacial clefts in Africa: methodological challenges in ascertainment. Pan Afr Med J. 2009; 1(2):5-14. PubMed | Google Scholar
- Donkor P, Bankas DO, Agbenorku P, Plange-Rhule G, Ansah SK. Cleft lip and palate in Kumasi, Ghana: 2001-200 J Craniofac Surg. 2007; 18:1376-1379. PubMed | Google Scholar
- Martiniuk ALC, Manouchehrian M, Negin JA and Zwi AB. Brain Gains: a literature review of medical missions to low and middle-income countries. BMC Health Services Research. 2012; 12:13. PubMed | Google Scholar
- Green T, Green H, Scandlyn J, Kestler A. Perceptions of short-term medical volunteer work: a qualitative study in Guatemala. Globalization and Health. 2009. 5:4. PubMed | Google Scholar
- Chiu Y, Weng Y, Chen C, Yang C, Chiou H, Lee M. A comparative study of Taiwan's short-term medical missions to the South Pacific and Central America. BMC International Health and Human Rights. 2012; 12:37. PubMed | Google Scholar
- Walsh DS. A framework for short-term humanitarian health care projects. Int Nurs Rev. 2004; 51:23-26. PubMed | Google Scholar
- Panosian C, Coates TJ. The new medical 'missionaries' - grooming the next generation of global health workers. N Eng J Med. 2006; 354:1771-177. PubMed | Google Scholar
- Ghani S, Mannan A, Sen S et al. The problems of establishing modern cleft lip and palate services in Bangladesh. J Surg. 2004; 2:43. PubMed | Google Scholar
- Singh SK. Smile Train The ascendancy of cleft care in India. Indian J Plast Surg. 2009 October; 42(Suppl): S192-S198. PubMed | Google Scholar
- Pham AM, Tollefson T. Cleft deformities in Zimbabwe, Africa. Arch Facial Plast Surg. 2007; 9:385. PubMed | Google Scholar
- Bezruchka S. Medical tourism as medical harm to the third world: Why? For whom? Wilderness Environ Med. 2000; 11:77-78. Google Scholar
- Bishop R, Litch JA. Medical tourism can do harm. Br Med J. 2000; 320:1017. PubMed | Google Scholar
- Wolfberg AJ. Volunteering overseas - lessons from surgical brigades. N Engl J Med. 2006; 354:443-445. PubMed | Google Scholar
- Van Tilburg CS. Attitudes toward medical aid to developing countries. Wilderness Environ Med. 1995; 6:264-268. PubMed | Google Scholar
- Zbar RI, Rai SM, Dingman DL. Establishing cleft malformation surgery in developing nations: a model for the new millennium. Plast Reconstr Surg. 2000; 106(4):886-889. PubMed | Google Scholar
- Mendoza RL. Public health policy and medical missions in the Philippines: the case of oral-facial clefting. Asia Pac J Public Health. 2009; 21(1):94-103. PubMed | Google Scholar
- Mulliken JB. The changing faces of children with cleft lip and palate. N Engl J Med. 2004; 351(8):745-747. PubMed | Google Scholar
- Buchman S. Tariro: Finding hope in Zimbabwe. Can Fam Physician. 2007; 53(11):1971-1973. PubMed | Google Scholar
- Adullah F. Perspective of West Africa: why bother to 'mission'? Arch Surg. 2008; 143(8):728-729. Google Scholar
- Suchdev P, Ahrens K, Click E, Macklin L, Evangelista D, Graham E. A Model for Sustainable Short-Term International Medical Trips. Ambulatory Pediatrics. 2007; 7 (4) : 317-320. PubMed | Google Scholar