A rare presentation of hepatocellular carcinoma in non-cirrhotic liver
Lamia Kabbage, Meryem Elkouhen, Ahmed Taghy, Kaoutar Znati, Nawal Kabbaj
Corresponding author: Lamia Kabbage, Faculty of Medicine, Mohammed V Souissi University, EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Rabat, Morocco 
Received: 02 Aug 2017 - Accepted: 12 Sep 2017 - Published: 22 Sep 2017
Domain: Gastroenterology,Hepatology,Oncology
Keywords: Hepatocellular carcinoma, GIST, non cirrhotic liver
©Lamia Kabbage et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Lamia Kabbage et al. A rare presentation of hepatocellular carcinoma in non-cirrhotic liver. Pan African Medical Journal. 2017;28:69. [doi: 10.11604/pamj.2017.28.69.13512]
Available online at: https://www.panafrican-med-journal.com//content/article/28/69/full
A rare presentation of hepatocellular carcinoma in non-cirrhotic liver
Lamia Kabbage1,2,&, Meryem El kouhen2, Ahmed Taghy1,3, Kaoutar Znati1,4, Nawal Kabbaj1,2
1Faculty of Medicine, Mohammed V Souissi University, Rabat, Morocco, 2EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Rabat, Morocco, 3Clinique Chirurgicale B, Ibn Sina Hospital, Rabat, Morocco, 4Pathology Department, Ibn Sina Hospital, Rabat, Morocco
&Corresponding author
Lamia Kabbage, Faculty of Medicine, Mohammed V Souissi University, EFD-Hepatogastroenterology Unit, Ibn Sina Hospital, Rabat, Morocco
Hepatocellular carcinoma is the most frequent type of liver malignancy. Most cases of hepatocellular carcinoma are secondary to either viral hepatitis (hepatitis B, C) or alcoholic cirrhosis. Liver cirrhosis due to any other causes is considered as a risk factor for development of hepatocellular carcinoma; however, hepatocellular carcinoma in non cirrhotic livers remains a rare condition. The present case report describes a 59-year-old woman patient admitted to explore right hypochondriac and epigastric pain, with no evidence of pre-existing liver disease and with a good general condition. The computed tomography was very suggestive of a gastro-intestinal stromal tumor. But, at laparotomy, a huge hepatic tumor was discovered. Histopathological study confirmed the presence of primary hepatocellular carcinoma. Hepatocellular carcinoma occurs more frequently on a cirrhotic liver. However, it can occur on a non cirrhotic liver and remains and extremely rare case.
The incidence of hepatocellular carcinoma (HCC) is constantly rising throughout the world with the majority of cases in Asia and Africa due to the high prevalence of hepatitis B virus (HBV) infection [1]. HCC is the most frequent type of primary malignant lesion of the liver, the sixth leading cause of cancer and the third leading cause of cancer death [2]. It develops on cirrhotic liver in 80% of cases, appearing in a 20% on healthy livers (fibrolamellar variant) or with non-cirrhotic chronic liver disease [3]. Besides this fibrolamellar variant, HCC on a healthy liver remains exceptional [4, 5]. We report a case of an HCC on a healthy liver diagnosed initially as a gastro-intestinal stromal tumor (GIST).
A 59-year-old woman without pathological antecedents presented with a 2 months history of right hypochondriac and epigastric pain. She gave no history of jaundice or gastro-intestinal bleeding. She had a good general well being. On examination, the patient was not jaundiced and the body mass index (BMI) was in the standards (BMI = 24.6kg/m2). The abdominal examination revealed an enormous and firm mass of the right hypochondriac that reaches the right iliac fosse, no splenomegaly or ascites. She had no peripherical stigmata of chronic liver disease. Examination of other systems was unremarkable. Abdominal ultrasound was done and showed a hypodense and heterogeneous lesion of 10.6cm in diameter which could be located in the right hepatic lobe (doubt with a space tumor); otherwise, there were no signs of portal hypertension or ascites (Figure 1). An abdominal computed tomography (CT) revealed a tissular lesion of 151 x 108 x 82 mm with heterogeneous enhancement, located in the right flank having an intimate contact with the gastric antrum (Figure 2). It develops towards the hepatic hilus and compresses the biliay convergence inducing a slight intrahepatic bile ducts dilatation. No lymph nodes or ascites or signs of cirrhosis and portal hypertension were noticed. Therefore, the CT aspect was very suggestive of a GIST. The upper gastro-intestinal endoscopy revealed an extrinsic compression aspect in the antopyloric junction but did not show an endoluminal tumor. The liver tests showed minimum pattern of cholestasis: AP: 132UI/L (< 110), GGT: 32UI/L (< 50), total bilirubine: 31.2 mg/l (< 10) and a minimum increase in transaminases: GOT: 65UI/L (< 36), GPT: 90UI/L (< 34). Cell blood count (CBC) revealed a Hb of 10.8 gm/dL, WBC of 4800/cmm and a platelets of 160000/cm. The prothrombin level was 78%. Serology for viral hepatitis including HBsAg, HBcAb, HBsAb and HVC-Ab was negative. The patient underwent surgery for GIST resection. At laparotomy, the surgeon discovered an enormous hepatic tumor of 15cm in diameter, polylobed with dented contours, friable with necrotic foci and located in segments IV, V and VIII. The tumor was locally advanced, having a tight adherence with the gastric antrum, the first jejunal loop and omentum adherence. The tumor also invaded the gallbladder and the hepatic pedicle. Unfortunately, the tumor resection could not be done. Cirrhosis and liver chronic disease were rule out with a biopsy of the non-tumoral liver. The histopathological study of the surgical biopsy of the tumor revealed a well differentiated HCC (Figure 3). There were no eosinophilic, polygonal cells or wide lamellar bands of fibrous tissue that are characteristic of the fibrolamellar HCC. Since the tumor was unresectable, the patient was proposed for a treatment by sorafenib. Unfortunately, by lack of means, our patient could not have the chemotherapy by Sorafenib and she died after 5 months of HCC diagnosis.
HCC is the common type of primary liver cancer. It has an annual incidence of 600,000 newly diagnosed patients [6]. HCC in non cirrhotic liver is a relatively rare diagnosis: 14% in Schutte's cohort (664 cases of HCC) [7], 8.8% in Gomez-Rodriuez's cohort (469 cases of HCC) [8], 6.2% in Nunez-Martinez's cohort (469 cases of HCC) [9] and only 1.7% in Giannini's cohort including 3027 cases of HCC [10]. Some series of non cirrhotic HCC reported a lower male preponderance (male/female ratio: 1.3-2.1) as compared with the cirrhotic counterpart, where this ratio ranges from 3.2 to 8:1 [11]. The mean age is generally less advanced in non cirrhotic than in cirrhotic patients. Namely, cirrhotic HCC shows an unimodal age distribution, peaking at the 7th decade, whereas non cirrhotic HCC reveals a bimodal distribution, peaking at the 2nd and 7th decades [11]. In the presented case, the patient is a woman age of about sixty. Although liver cirrhosis is the main risk factor for HCC, this tumor may develop in patients with non cirrhotic chronic liver disease like chronic hepatitis B virus infection [12] and chronic hepatitis C virus infection [13, 14]. HCC can also develop in subjects without evidence of chronic liver disease. This condition remains exceptional and it represents only 0.32% in the literature's largest cohort of HCC including 3027 cases. This is compatible with the presented case as the patient showed no evidence of pre-existing liver disease. The pathogenesis is still not well understood. Several pathogenic risk factors are discussed such as ionizing radiation, exposure to toxins [5] and benign focal liver lesions, mainly the hepatocellular adenoma. Our patient had none of these risk factors (especially the hepatocellular adenoma). It can present as abdominal pain or discomfort in the right upper quadrant, jaundice, nausea, or "toxic syndrome" (weight loss, fever, malaise, asthenia, anorexia). Haemoperitoneum due to cancer rupture may be a life-threatening presentation of non cirrhotic HCC [11]. It may remain asymptomatic in more than half of cases explaining that it is often diagnosed at an advanced and inoperable stage. This was the case in this presentation. There was only a right hypochondriac and epigastric pain without any other associated symptoms. The patient had a good general condition. Therefore, the tumor was diagnosed at an advanced stage. Alpha-fetoprotein can be high or remain in the standards [15]. It exceeds 20 ng/dL less frequently in non cirrhotic than cirrhotic HCC patients (31-67% vs 59-84%) [11]. According to the guidelines, diagnosis is based on medical imagery and histology.
�
HCC in non cirrhotic patients shows similar CT and magnetic resonance imaging (MRI) patterns to those of HCC in cirrhotic patients. At CT, it demonstrates characteristic enhancement during the arterial phase and wash-out during the venous and/or equilibrium phases [16]. At MRI, it is hyperintense on T2-weighted images. On T1-weighted images, the lesion is hypointense [16]. HCC from non cirrhotic livers tended to be unifocal, large, well-circumscribed, encapsulated lesions or dominant masses with smaller satellite lesions [16]. Unfortunately, the abdominal CT performed in the presented case was very suggestive of a GIST and misdiagnosed the hepatic tumor. According to histological classification criteria of the World Health Organization (WHO), the trabecular type is the most frequent form (41-76%) in non-cirrhotic HCCs, as it is in cirrhotic subjects [11]. In our case, the histological study confirmed the diagnosis. The HCC was well differentiated and there were no characteristics of a fibrolamellar HCC. In the non tumoral liver, there were no signs of cirrhosis or chronic hepatitis (healthy liver). Patients with HCC diagnosed at an early stage are optimal candidates for resection, liver transplantation or percutaneous ablation. Surgical resection is recommended for patients with single tumors, absence of clinically relevant portal hypertension and normal bilirubin. Transplantation is indicated in patients with 3 nodules of < 3 cm or with single tumors < 5 cm with liver function impairment precluding resection. Transarterial chemoembolization (TACE) is recommended in asymptomatic patients with multinodular tumors that have not invaded hepatic vessels nor been disseminated outside the liver. Sorafenib is indicated as the first line of treatment in patients who cannot benefit from the above therapeutic options and still have a preserved liver function [17, 18]. In the case of our patient, the tumor was diagnosed at a very late stage. The size of the tumor and the severity of loco-regional invasion made the surgical resection impossible. According to the tumor stage and to the liver's biological parameters, the patient was a candidate for chemotherapy by sorafenib. Survival of patients with HCC in non cirrhotic liver mainly depends on tumor related factors such as tumor size, existence of satellite lesions, existence of a tumor capsule, vascular invasion, grading, R0 resection and the amount of intraoperative blood transfusions [7]. The altered condition, tobacco consumption, macroscopic vascular invasion, the large size of the tumor and the non surgical treatment were predictive factors of a bad prognosis of HCC on a healthy liver [19]. In the presented case, the tumor related factors and the absence of treatment worsened the prognosis. In fact, the patient died 5 months after the diagnosis of HCC.
HCC on a healthy liver remains an exceptional condition. The pathogenesis is still not well understood. It is characterized by a clinical latency explaining the delay in the diagnosis and consequently, the poor prognosis at an advanced stage. Ultrasound monitoring; especially in patients with risk factors, finds its place in the early diagnosis of this exceptional tumor.
The authors declare no competing interest.
Lamia Kabbage was the doctor of the patient in charge of diagnosis and the follow up and wrote the manuscript. Meriem El kouhen was the doctor who has first seen the patient and did the first consultation. Kaoutar Znati was the pathologist who confirmed the diagnosis of HCC by histologic examination. Ahmed Taghy was the surgeon of the patient who performed the surgery and the biopsy. Nawal Kabbaj was the chief of the medical department who took care of the patient and took therapeutic decision for the patient in the multidisciplinary meeting and did the correction of the paper.
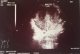
Figure 1: abdominal ultrasonography: heterogeneous masse probably depending of the right hepatic lobe
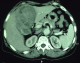
Figure 2: abdominal CT: heterogeneous hepatic masse misdiagnosed as GIST
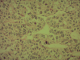
Figure 3: histopathological study of liver biopsy with well differenciated cells consistent with HCC
- El-Serag HB. Hepatocellular carcinoma. N Engl J Med. 2011; 365(12): 1118-27. PubMed | Google Scholar
- Forner A, Ayuso C, Isabel Real M, Sastre J, Robles R, Sangro B et al. Diagnosis and treatment of hepatocellular carcinoma. Med Clin (Barc). 2009; 132(7): 272-87. PubMed | Google Scholar
- Renedo F, De la Revilla J, Calleja JL. Carcinoma hepatocelular. Medicine. 2008; 10: 770-6. Google Scholar
- Casanova-Mart�nez L, Castillo-Grau P, Jaquotot-Herranz M et al. Hepatocellular carcinoma in non-cirrhotic liver. Rev Esp Enferm Dig. 2012; 104(9): 505-6. PubMed | Google Scholar
- Singh P, Kaur H, Lerner RG, Patel R, Rafiyath SM, Singh Lamba G. Hepatocellular carcinoma in non-cirrhotic liver without evidence of iron overload in a patient with primary hemochromatosis: review. J Gastrointest Cancer. 2012; 43(1): 36-9. PubMed | Google Scholar
- Elmakki EE. A Rare Presentation of Hepatocellular Carcinoma in a Young Adult: a case report. Oman Med J. 2014; 29(1): 1-3. Google Scholar
- Sch�tte K, Schulz C, Poranzke J, Antweiler K, Bornschein J, Bretschneider T et al. Characterization and prognosis of patients with hepatocellular carcinoma (HCC) in the non-cirrhotic liver. BMC Gastroenterol. 2014; 14: 117. PubMed | Google Scholar
- G�mez Rodr�guez R, Romero Guti�rrez M, Gonz�lez de Frutos C et al. Clinical characteristics, staging and treatment of patients with hepatocellular carcinoma in clinical practice: prospective study of 136 patients. Gastroenterol Hepatol. 2011; 34(8): 524-31. PubMed | Google Scholar
- N��ez Mart�nez �, Matilla Pe�a A, Merino Rodr�guez B et al. Descriptive study of hepatocellular carcinoma in noncirrhotic liver. Gastroenterol Hepatol. 2011; 34(5): 322-8. PubMed | Google Scholar
- Giannini EG, Marenco S, Bruzzone L, Savarino V, Farinati F et al. Hepatocellular carcinoma in patients without cirrhosis in Italy. Dig Liver Dis. 2012; 45(2): 164-9. PubMed | Google Scholar
- Trevisani F, Frigerio M, Santi V, Grignaschi A, Bernardi M. Hepatocellular carcinoma in non-cirrhotic liver: a reappraisal. Dig Liver Dis. 2010; 42(5): 341-7. PubMed | Google Scholar
- Wang Q, Luan W, Villanueva GA, Rahbari NN, Yee HT, Manizate F, Hiotis SP. Clinical prognostic variables in young patients (under 40 years) with hepatitis B virus-associated hepatocellular carcinoma. J Dig Dis. 2012; 13(4): 214-8. PubMed | Google Scholar
- Nosotti L, D'Arca T, Marignani M, Balducci G. Hepatocellular Carcinoma in a non-cirrhotic liver of a HCV-Positive Woman with sustained viral response. Mediterr J Hematol Infect Dis. 2011; 3(1): e2011050. PubMed | Google Scholar
- Nash KL, Woodall T, Brown AS, Davies SE, Alexander GJ. Hepatocellular carcinoma in patients with chronic hepatitis C virus infection without cirrhosis. World J Gastroenterol. 2010; 16(32): 4061-5. PubMed | Google Scholar
- Alkofer B, Lepennec V, Chiche L. Hepatocellular cancer in the non-cirrhotic liver. J Visc Surg. 2011; 148(1): 3-11. PubMed | Google Scholar
- Di Martino M, Saba L, Bosco S, Rossi M, Miles KA, Di Miscio R et al. Hepatocellulat carcinoma (HCC) in non-cirrhotic liver: clinical, radiological and pathological findings. Eur Radiol. 2014; 24(7): 1446-54. PubMed | Google Scholar
- Meloni TF, Di Stasi M, Rolle E, Solbiati L, Tinelli C et al. Sustained complete response and complications rates after radiofrequency ablation of very early hepatocellular carcinoma in cirrhosis: Is resection still the treatment of choice. Hepatology. 2008; 47(1): 82-9. PubMed | Google Scholar
- Llovet JM, Ricci S, Mazzaferro V, Hilgard P, Gane E, Blanc JF et al. SHARP investigators study group: sorafenib in advanced hepatocellular carcinoma. N Engl J Med. 2008; 359: 378-90. Google Scholar
- W�rns MA, Bosslet T, Victor A, Koch S, Hoppe-Lotichius M, Heise M, Hansen T, Pitton MB, Niederle IM, Schuchmann M, Weinmann A, D�ber C, Galle PR, Otto G. Prognostic factors and outcomes of patients with hepatocellular carcinoma in non-cirrhotic liver. Scand J Gastroenterol. 2012; 47(6): 718-28. PubMed | Google Scholar