An unusual presentation of neurosarcoidosis with progressive hearing loss
Abdellah Taous, Maha Aďt Berri, Mohamed Sinaa, Issam En-nafaa, Karim Nadour, Abdelhadi Rouimi
Corresponding author: Abdellah Taous, Department of Neurology, Military Hospital Moulay Ismail, Meknes, Morocco 
Received: 21 Oct 2016 - Accepted: 16 May 2017 - Published: 07 Nov 2017
Domain: Clinical medicine
Keywords: Hearing loss, neurosarcoidosis, rare complication
©Abdellah Taous et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Abdellah Taous et al. An unusual presentation of neurosarcoidosis with progressive hearing loss. Pan African Medical Journal. 2017;28:213. [doi: 10.11604/pamj.2017.28.213.11007]
Available online at: https://www.panafrican-med-journal.com//content/article/28/213/full
An unusual presentation of neurosarcoidosis with progressive hearing loss
Abdellah Taous1,&, Maha Aďt Berri1, Mohamed Sinaa2, Issam En-nafaa3, Karim Nadour4, Abdelhadi Rouimi1
1Department of Neurology, Military Hospital Moulay Ismail, Meknes, Morocco, 2Department of Anatomopathology, Military Hospital Moulay Ismail, Meknes, Morocco, 3Department of Radiology, Military Hospital Moulay Ismail, Meknes, Morocco, 4Department of Oto-rhino-laryngology, Military Hospital Moulay Ismail, Meknes, Morocco
&Corresponding author
Abdellah Taous, Department of Neurology, Military Hospital Moulay Ismail, Meknes, Morocco
Sarcoidosis is a granulomatous disease of unknown etiology that can involve several organ system. Neurological manifestations are not common and mostly include cranial neuropathies. However, auricular disorders are rare and exceptionally inaugural. We describe the case of a 46-year-old lady presented with hearing loss as the initial manifestation of sarcoidosis, and aim to raise awareness of this condition, that is often associated with significant morbidity.
Neurosarcoidosis is a rare inflammatory disorder of the nervous system, which occurs in 7% of patients with sarcoidosis [1]. Cranial nerves are the most commonly involved, particularly the optic nerve, the trigeminal and the facial nerve [2]. However, auricular disorders are rare and exceptionally inaugural [3]. We report the case of a 46-year-old lady presented with hearing loss as the initial manifestation of sarcoidosis.
A 46-year-old lady with no significant medical history, was referred to our department after a 7 months history of gradually worsening bilateral hearing loss without tinnitus, vertigo or aural discharge. Also, there were no other neurological or ocular symptoms. Clinical examination showed no neurological, otologic or ophthalmologic abnormalities. A pure tone audiogram revealed a bilateral sensorineural hearing loss, mild to moderate in the left ear and deep in the right. However, auditory brainstem response (ABR) showed normal morphology and latencies, and brain magnetic resonance imaging (MRI) with gadolinium enhancement revealed no lesions too, particularly in the cerebello-pontine angle. Routine blood tests showed a raised level of angiotensin-converting enzyme (ACE) at 253 IU (N: 12-68 IU), whereas hormonal dosages revealed no hypothalamic-pituitary axis dysfonction. There was bilateral hilar lymphadenopathy with infiltration at the thoracic computed tomography, and the salivary gland biopsy confirmed the diagnosis by finding non-caseating and giant-cell granulomas (Figure 1). The lumbar puncture showed increased proteins level (1,09g/l; upper normal limit 0,40g/l), an elevated IgG index in the cerebrospinal fluid, but no pleocytosis, According to Zajicek criteria the diagnosis of neurosarcoidosis (NS) was probable. Subsequently, the patient was given Methylprednisolone intravenously (1g/d for 3 days), before tapering oral steroids. The hearing acuity improved gradually over one year of follow up.
Hearing loss in systemic sarcoidosis remains a rare complication that is estimated to occur in only 1% to 7% of all patients with NS [4]. The most commonly involved cranial nerves was the optic nerve followed by the trigeminal and the facial nerve [2]. When it presents as the initial symptom of NS, whether unilateral or bilateral, it has a sudden or rapidly progressive onset 90% of the time [5]. There have been few reports describing it as one of the initial presenting symptoms of sarcoidosis in otherwise undiagnosed patients, however these were also associated with other neurological or ENT disturbances [6,7]. The diagnosis of neurosarcoidosis is based on clinical and radiological correlation in combination with a tissue biopsy [8, 9]. Although commonly requested, serum ACE has a poor predictive value in sarcoidosis. MRI is sensitive for detecting cerebral nervous system lesions of which leptomeningeal involvement with contrast enhancement is the most common finding; however, their appearances are highly variable, hence, reducing the specificity. Other findings include isolated mass lesions and diffuse inflammatory changes [8,9]. A normal MRI, as was the case of our patient does not rule out the possibility of neurosarcoidosis [8]. In large cohort of 305 patients with established neurosarcoidosis and cranial base manifestations, Carlson and al. found a meningeal enhancement only in 67% of cases [2]. Lack of abnormality on cerebral MRI despite symptoms of CNS involvement may be due to extra-cranial involvement of cranial nerves, to initially minimal perineural inflammatory infiltration or to the presence of granulomas too small to be detected by current imaging techniques.
Therefore, repetition and follow-up studies may confirme evolution of those CNS lesions [10]. The histological studies demonstrate lesions at all levels from the cochlea to the brainstem, but the main mechanism is an infiltration of the arachnoid vessels [11]. The normality of ABR in our patient suggests that the hearing impairment was of cochlear origin, whereas almost all cases of related sarcoidosis sensorineural hearing loss reported in the litterature were of retrocochlear origin likely due to a basilar meningitidis involving the cochleovestibular nerve [5]. Although evidence-based treatment guidelines derived from standard clinical trials are not available, early treatment of neurosarcoidosis is recommended. Corticosteroids are the first line treatment for neurosarcoidosis. Oral prednisone in dosages of 40-80mg/d will usually suppress disease progression and may even improve clinical manifestations. There may be some benefit of giving higher dose of corticosteroids such as Methylprednisolone 1000 mg/d intravenously for 3-5 days before the oral steroids, however the prognosis of the hearing loss is usually poor [8, 11, 12]. Our patient had the chance to get an early diagnosis and treatment, which resulted in a significant improvement in hearing.
In dealing with patients with atypical or rapidly progressive hearing loss, it’s mandatory to consider to the possibility of sarcoidosis and conduct a full neurological and general examination for evidence of this condition.
The authors declare no competing interests.
All authors have read and agreed to the final version of this manuscript.
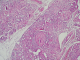
Figure 1: salivary gland biopsy showing a parenchyma with non-caseating and giant-cell granulomas
- James D. Neurological complications of sarcoidosis. Sage Journal. 1967; 60(11): 1169-1170. Google Scholar
- Carlson ML, White JR Jr, Espahbodi M, Haynes DS, Driscoll CL, Aksamit AJ et al. Cranial base manifestations of neurosarcoidosis: a review of 305 patients. Otol Neurotol. 2015 Jan; 36(1): 156-66. PubMed | Google Scholar
- Allen RKA, Sellars RE, Sandstrom PA. A prospective study of 32 patients with neurosarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis. 2003 Jun; 20(2): 118-25. Google Scholar
- Cama E, Santarelli R, Muzzi E et al. Sudden hearing loss in sarcoidosis: otoneurological study and neuroradiological correlates. Acta Otorhinolaryngol Ital. 2011 Aug;31(4):235-8. PubMed | Google Scholar
- Colvin IB. Audiovestibular manifestations of sarcoidosis: a review of the literature. Laryngoscope. 2006 Jan; 116(1): 75-82. PubMed | Google Scholar
- Sugaya F, Shijubo N, Takahashi H, Abe S. Sudden hearing loss as the initial manifestation of neurosarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis. 1996 Mar;13(1):54-6. PubMed | Google Scholar
- Tharp BR, Pfeiffer JB. Sarcoidosis and the acoustic nerve. Arch Otolaryngol. 1969 Sep; 90(3): 360-6. PubMed | Google Scholar
- Nozaki K, Judson MA. Neurosarcoidosis: clinical manifestations, diagnosis and treatment. Presse Med. 2012 Jun; 41(6 Pt 2): e331-48. PubMed | Google Scholar
- Hoitsma E, Faber CG, Drent M, Sharma OP. Neurosarcoidosis: a clinical dilemma. Lancet Neurol. 2004 Jul; 3(7): 397-407. PubMed | Google Scholar
- Sherman Jl, Stern BJ. Sarcoidosis of the CNS: Comparison of Unenhanced and Enhanced MR Images. AJR Am J Roentgenol. 1990 Dec; 155(6): 1293-301. PubMed | Google Scholar
- Moine A, Frachet B, Van Den Abbeele T, Tison P, Battesti JP. Deafness and sarcoidosis. Ann Otolaryngol Chir Cervicofac. 1990; 107(7): 469-73. PubMed | Google Scholar
- Baughman RP. Therapeutic options for sarcoidosis: new and old. Curr Opin Pulm Med. 2002 Sep; 8(5): 464-9. PubMed | Google Scholar