Surgical treatment for unusual presentations of abdominal actinomycosis: two case reports
Clara Sampaio, Sofia Pina, Sofia Frade, Luís Moniz
Corresponding author: Clara Sampaio, Department of General Surgery, Centro Hospitalar Lisboa Central, Lisbon, Portugal 
Received: 11 Sep 2017 - Accepted: 25 Sep 2017 - Published: 10 Oct 2017
Domain: Infectious disease,General surgery
Keywords: Actinomycosis, bowel obstruction, sigmoid colon
©Clara Sampaio et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Clara Sampaio et al. Surgical treatment for unusual presentations of abdominal actinomycosis: two case reports. Pan African Medical Journal. 2017;28:133. [doi: 10.11604/pamj.2017.28.133.13858]
Available online at: https://www.panafrican-med-journal.com//content/article/28/133/full
Original article 
Surgical treatment for unusual presentations of abdominal actinomycosis: two case reports
Surgical treatment for unusual presentations of abdominal actinomycosis: two case reports
Clara Sampaio1,&, Sofia Pina1, Sofia Frade1, Luís Moniz1
1Department of General Surgery, Centro Hospitalar Lisboa Central, Lisbon, Portugal
&Corresponding author
Clara Sampaio, Department of General Surgery, Centro Hospitalar Lisboa Central, Lisbon, Portugal
Actinomycosis is a rare chronic disease caused by anaerobic Gram-positive Actinomyces species. These bacteria normally colonize the mouth, colon and urogenital tract and mucosal disruption is necessary to lead to infection. Due to its propensity to mimic other diseases, it is often misdiagnosed. It can mimic other conditions such as tuberculosis and malignancy and a preoperative diagnosis is rarely considered. An early diagnosis needs a high level of clinical suspicion and bacterial cultures in anaerobic conditions are necessary to identify the bacteria. Of the more than 30 species, Actinomyces Israelii is the most common human pathogen and one of the most involved in abdominal actinomycosis. Treatment includes high doses of antibiotic therapy sometimes combined with surgery in the case of complicated disease such as bowel obstruction. The authors report two cases of abdominal actinomycosis presenting with bowel obstruction and bowel perforation by a strange body.
Actinomyces spp. an anaerobic Gram-positive bacterium, does not exist freely in nature but normally colonizes the human oropharynx, gastrointestinal and female genital tract. The disease-actinomycosis-however, is rare and was first described in 1879 by Israel [1]. Human actinomycosis is most frequent in the cervicofacial (50-65%), thoracic (15-30%) and abdominopelvic regions (20%) [2]. It usually occurs in immunocompetent persons and mucosal disruption of the gastrointestinal tract, anywhere from the mouth to the rectum is typically the portal of entry. Other important risk factor includes the presence of the intrauterine contraceptive device (IUD) allowing ascension of the bacteria into the uterus where focal necrosis is thought to be the breach required for disease to occur [3].
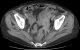
Case 1: a 50-year-old woman proceeded to the emergency department with lower left abdominal pain, anorexia, weight loss (10Kg in 1 month) and constipation. On examination, her vital signs were normal but she complained with lower left abdominal pain and a palpable mass in the same region. The laboratory results of the patient showed anemia. Computerized tomography (CT) and magnetic resonance imaging (MRI) scans revealed a 66 x 33mm mass attached to the left adnexa and sigmoid colon causing proximal colonic distention and a dilated ureter on that side (Figure 1). At laparotomy, an inflammatory abscessed mass of the sigmoid colon was found and a sigmoid resection with primary anastomosis was carried out. Histology showed an inflammatory mass with multiple abscesses containing colonies of Actinomyces spp. As soon as pathology report became available, intramuscular penicillin treatment was initiated followed by oral penicillin. In the meantime, the IUD was removed but the follow-up exams revealed a cervix inflammatory process. A total abdominal hysterectomy and salpingo-ophorectomy was performed and histology specimen revealed uterine actinomycosis. No postoperative complications were observed and the patient was discharged to complete 12 months of oral treatment.
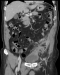
Case 2: a 68-year-old man presented with a 2-month history of left iliac fossa pain without altered bowel habits or fever. On physical examination, he had pain and tenderness in left lower quadrant (LLQ). The laboratory data showed elevated leukocyte count. Urgent CT scan revealed a mass in LLQ with vesical and sigmoid colon wall thickening suggesting a bowel perforation by a strange body (Figure 2). The patient underwent a laparotomy, an inflammatory sigmoid mass extending to the bladder and abdominal wall was found and a sigmoid and partial vesical resection was performed. Final pathology report was consistent with actinomycosis and the patient started a 12-month course of penicillin. At 1-year follow-up he was free from disease and asymptomatic.
Actinomycosis is an uncommon subacute or chronic infection caused by anaerobic Gram-positive Actinomyces species, most frequently Actinomyces israelii [4]. The disease occurs worldwide, has no sex, age or race predilection [5] and there is no documented person-to-person transmission [6]. Abdominal actinomycosis makes up about 20% of cases and is the most indolent and non-specific presentation, mimicking malignancy, tuberculosis and inflammatory bowel disease [7, 8]. Actinomyces normally colonizes the human gastrointestinal mucosa and some predisposing factors to disease include surgical trauma, appendicitis, diverticulitis, foreign bodies or neoplastic processes [9]. Another important risk factor is the presence of IUD since the bacterium is found in up to 25% of cervical smears performed in these women and uterine trauma can contribute to actinomycosis development. Abdominal actinomycosis can spread into the neighbouring tissues and pelvis, usually extending to the ovary, but pelvic actinomycosis is predominantly associated with IUD. Most commonly, abdominal actinomycosis occurs in the ileocecal region and rarely in the ascending and left side colon with few reported cases [10, 11]. May present with nonspecific symptoms such as abdominal pain and fever and there may not always be a palpable mass. Fewer than 10% of cases are diagnosed pre-operatively [12] and the final diagnosis is usually made with the demonstration of actinomycotic granules in histologic sections and isolating Actinomyces species in cultures [13].
Abdominal actinomycosis is a rare indolent disease with nonspecific symptoms that should be included in the differential diagnosis in patients with abdominal masses with malignancy or inflammatory characteristics. Patients require prolonged treatment with penicilin G or amoxicilin but surgical treatment is often required because of difficulty in preoperative diagnosis. Medical and surgical combined therapy is usually effective in about 90% of cases [14].
The authors declare no competing interests.
Clara Sampaio, Sofia Pina and Sofia Frade collected the patient's clinical data, Luís Moniz analyzed the data, Clara Sampaio wrote the paper.
Figure 1: abdominal CT scan demonstrating a sigmoid tumor like mass
Figure 2: CT scan shows a mass in left lower quadrant with bowel wall thickening suggesting perforation
- Israel J. Neue Beobactungen auf dem Bebiete der Mykosen des Menshen. Virchows Archiv fur Pathologische Anatomie. 1878; 74: 15-53. Google Scholar
- Heo S, Shin S, Kim J, Lim H, Seon H, Jung S, Jeong Y, Kang H. Imaging of Actinomycosis in Various Organs: a comprehensive review. RadioGraphics. 2014; 34(1): 19-33. PubMed | Google Scholar
- Choi M, Hong D, Seong W, Lee Y, Park I. Pelvic actinomycosis confirmed after surgery: single center experience. Arch Gynecol Obstet. 2010; 281(4): 651-656. PubMed | Google Scholar
- Malik A, Papagrigoriadis S, Leather A, Rennie J, Salisbury J, Beese R. Abdominopelvic mass secondary to actinomyces israelli mimicking cancer: report of two cases. Tech Coloproctol. 2005; 9(2): 170-1. PubMed | Google Scholar
- Jacobs RF, Schutze GE. Actinomycosis In: Behrman RE, Kliegman R, Jeson HB, editors. Nelson textbook of paediatrics, Philadelphia: WB Saunders. 2000; 16: 822-4. Google Scholar
- Smergo RA Jr, Foglia G. Actinomycosis. Clin Infect Dis. 1998; 26(6): 1255-61. Google Scholar
- Acevedo F, Baudrand R, Letelier LM, Gaete P. Actinomycosis: a great pretender: case reports of unusual presentations and a review of the literature. Int J Infect Dis. 2008; 12(4): 358-62. PubMed | Google Scholar
- Cintron JR, Del Pino, Duarte B, Wood D. Abdominal actinomycosis: report of two cases and review of literature. Dis Col Rectum. 1996; 39: 105-108. Google Scholar
- Filippou D, Psimitis I, Zizi D, Rizos S. A rare case of ascending colon actinomycosis mimicking cancer. BMC Gastroenterology. 2005; 5: 1. PubMed | Google Scholar
- Norwood MG, Bown MJ, Furness PN, Berry DP. Actinomycosis of the sigmoid colon: an unusual cause of large bowel perforation. ANZ J Surg. 2004; 74(9): 816-816. PubMed | Google Scholar
- Meyer P, Nwariaku O, McClelland RN, Gibbons D, Leach F, Sagalowsky AI, Simmag C, Jeyarajah DR. Rare presentation of actinomycosis as an abdominal mass: report of a case. Dis Colon Rectum. 2000; 43(6): 872-875. PubMed | Google Scholar
- Wong V, Turmezei T, Weston V. Actinomycosis. BMJ. 2011; 343: d6099. PubMed | Google Scholar
- Valour F, Sénéchal A, Dupiex C, Karsensty J, Lustig S, Breton P, Gleizal A, Boussel L, Laurent F, Braun E, Chidiac C, Ader F, Ferry T. Actinomycosis: etiology, clinical features, diagnosis, treatment and management. Infection and Drug Resistance. 2014; 7: 183-197. PubMed | Google Scholar
- Kim JC, Ahn BY, Kim HC, Yu CS, Kang GH, Ha HK, Lee MG. Efficiency of combined colonoscopy and computed tomography for diagnosis of colonic actinomycosis: a retrospective evaluation of eight consecutive patients. Int J Colorectal Dis. 2000; 15(4): 236-242. PubMed | Google Scholar