Villoglandular papillary adenocarcinoma: case report
Ghizlane Salek, Issam Lalia, Driss Moussaoui Rahali, Mohamed Dehayni
Corresponding author: Ghizlane Salek, Department of Gynecology Obstetrics, Military Training Hospital Med V, Rabat, Morocco 
Received: 12 Jul 2016 - Accepted: 07 Nov 2016 - Published: 08 Dec 2016
Domain: Clinical medicine
Keywords: Villoglandular, subtype of adenocarcinoma, young women
©Ghizlane Salek et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ghizlane Salek et al. Villoglandular papillary adenocarcinoma: case report. Pan African Medical Journal. 2016;25:232. [doi: 10.11604/pamj.2016.25.232.10305]
Available online at: https://www.panafrican-med-journal.com//content/article/25/232/full
Villoglandular papillary adenocarcinoma: case report
Ghizlane Salek1,&, Issam Lalya2, Driss Moussaoui Rahali1, Mohamed Dehayni1
1Department of Gynecology Obstetrics, Military Training Hospital Med V, Rabat, Morocco, 2Department of Radiotherapy, HMIMV, Rabat, Morocco
&Corresponding author
Ghizlane Salek, Department of Gynecology Obstetrics, Military Training Hospital Med V, Rabat, Morocco
Villoglandular papillary adenocarcinoma (VPA) is a very rare subtype of adenocarcinoma of the uterine cervix, but a well-recognized variant of cervical adenocarcinoma with a favorable prognosis and generally occurring in women of child-bearing age. Herein, we report a case of VPA diagnosed and managed successfully with conservative measure. This management is particularly desirable in young women to preserve reproductive capability.
The incidence of cervical adenocarcinoma is on the rise over the last decades. Villoglandular papillary adenocarcinoma (VPA) is a very rare subtype of adenocarcinoma of the uterine cervix. The true incidence of this form of adenocarcinoma is unknown. The classical histologic appearance of this entity is a surface papillary component of variable thickness with papillae that are usually tall and thin, but occasionally short and broad, with a fibrous stromal core. The tumor cells should have no more than mild-to-moderate nuclear atypicality and scattered mitotic figures. It affects a younger age group and has an excellent prognosis as compared to other endocervical adenocarcinomas [1, 2].
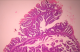
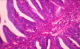
A 29 year old para 1 presenting with a history of postcoital bleeding for three months. She was not using contraceptives and was trying for a pregnancy. On per speculum examination, a suspicious growth on the posterior lip of the cervix was noted for which a punch biopsy was done. The histo-pathological examination showed moderately differentiated papillary adenocarcinoma with a villoglandular pattern (Figure 1, Figure 2, Figure 3). There was no evidence of lymphovascular space invasion. An MRI showed a 3.2 � 2.5 � 3.6 cm tumour arising from the anterior lip of the cervix, with distal parametrial involvement but no significant pelvic or retroperitoneal lymph node enlargement. The multi-disciplinary team meeting confirmed a stage IIB distal cancer of the cervix and decided to treat with chemo-radiotherapy. She received 45 Gy in 25 fractions of external beam radiotherapy to the pelvis with concomitant weekly cisplatin 40 mg/m2. The radiotherapy dose to the primary cervical tumour was 26 Gy to point A. The primary cervical tumour had responded well to the initial chemo radiotherapy. After 4 weeks the cervical lesion has completely responded.
Adenocarcinomas are the second most common type of cervical cancers in women comprising 10-20% of the cases. Villoglandular papillary adenocarcinoma (VGA) of cervix is a rare but well recognized histologic subtype of cervical adenocarcinoma . It tends to appear in younger women [1] and its indolent behavior permits fertility-preserving treatments. VGA was first reported by Young and Scully in 1989, who described three main histological features: exophytic proliferation, papillary architecture and mild to moderate cellular atypia [1]. The etiology of villoglandular papillary adenocarcinoma has not been well established [3]. An association between the use of oral contraceptives and villoglandular papillary adenocarcinoma was suggested by Jones et al. Although there are reports of an association between the use of oral contraceptives and cervical adenocarcinoma, a specific association is not found between the reproductive function of the patient and cervical adenocarcinoma. [4]. Treatment modalities range from cone biopsies to simple and radical hysterectomy with or without pelvic lymph node dissection and pre-postoperative radiation therapy [5-7]. Conflicting conclusions on the prognosis of villoglandular adenocarcinoma have been reported in various case series, most of them quoting excellent prognosis [1,8,10] with few reporting rapid deterioration [9-11]. The standard treatment for advanced adeno-squamous cervical cancer is chemo radiation. As our patient had a stage IIB distal villoglandular papillary adenocarcinoma, fertility sparing surgery was not an option. External beam radiotherapy with concomitant cisplatin chemotherapy, was used which resulted in good response. The prognosis following surgical treatment is excellent. Surgical treatments described are cone biopsy alone (7 patients), simple hysterectomy (11 patients), and radical hysterectomy (57 patients). Disease-free periods have ranged from 13 months to 7 years. Only one death has been reported in the literature in a woman who had iliac node metastases in association with clinical stage 1B villoglandular papillary adenocarcinoma. Thirty-six months after a radical hysterectomy, she developed vaginal recurrence and died of the disease in 46 months. The usually good prognosis is also reflected by the early stage that most tumors associated with villoglandular papillary adenocarcinoma present, with over 94% of patients Having stage 1 disease [12]. The absence of lymphovascular invasion and nodal metastases is usual. Because of the inherent good prognosis of this tumor, fertility-conserving procedures have been suggested [1]. Young and Scully recommended that the initial treatment should be a cone biopsy if three criteria were fulfilled: (1) The margins of the cone are clear of the disease, (2) the depth of invasion is no more than 3 mm, and (3) there shall be no evidence of lymphovascular invasion on histology.
Villoglandular papillary adenocarcinoma of the cervix is considered to have a favorable prognosis, and likewise, the treatment described is also conservative with close follow up; especially in young patients.
Author's declare no competing interest.
All authors have read and agreed to the final version of this manuscript and have equally contributed to its content and to the management of the case.
Figure 1: hematein eosin x 5 villoglandular adenocarcinoma composed of papillary and glandular structures lined with cylindrical cells sometimes mucosecreting
Figure 2: HEx200 ADK villoglandular: glands lined with mucosecreting cylindrical cells (arrows) without invasive element
Figure 3: HEX400 details of papillary structures lined with columnar cells with moderate atypia with few mitotic figures (arrow)
- Young RH and Scully RE. �Villoglandular papillary adenocarcinoma of the uterine cervix: a clinicopathologic analysis of 13 cases�. Cancer. 1989; 63(9): 1773-1779. PubMed | Google Scholar
- Jones MW, Silverberg SG, and Kurman RJ. �Well-differentiated villoglandular adenocarcinoma of the uterine cervix: a clinicopathological study of 24 cases�. International Journal of Gynecological Pathology. 1993; 12(1): 1-7. PubMed | Google Scholar
- Liao SY, Manetta A. Benign and malignant pathology of the cervix, including screening. Curr Opin Obstet Gynecol. 1993;5:497-503. PubMed | Google Scholar
- Jones MW, Kaounelis S, Papadaki H, Bakker A, Swalsky PA, Woods J, et al. Well differentiated villoglandular adenocarcinoma of the uterine cervix: Oncogene/tumor suppressor gene alterations and human papillomavirus genotyping. Int J Gynecol Pathol. 2000;19:110-7. PubMed | Google Scholar
- Reed W, Abeler VM, Trope CG. Villous glandular adenocarcinoma of the uterine cervix. A subtype with favourable prognosis? Tidsskr Nor Laegeforen. 1993;113:2569-71. PubMed | Google Scholar
- Datta CK. Well differentiated papillary villoglandular adenocarcinoma of the uterine cervix. W V Med J. 1997;93:186-8. PubMed | Google Scholar
- Bouman A, Oosterhuis GJ, Naudin TC, van Doorn GA. Villoglandular papillary adenocarcinoma of the cervix: beware of a wolf in sheep's clothing. Eur J Obstet Gynecol Reprod Boil. 1999;87:183-9. PubMed | Google Scholar
- Hoffman HS, Bazzurini L, Laird L, Murphy JC, Magriples U, Lewis J. Term delivery following conservative treatment for villoglandular papillary adenocarcinoma of the uterine cervix: report of a case and analysis of the literature. Gynecol Oncol. 2001;81(2):310. PubMed | Google Scholar
- Rubesa-Mihaljevic R, Vrdoljak-Mozetic D, Ostojic DV, Stemberger-Papic S, Sindik N, Krasevic M. Villoglandular papillary adenocarcinoma of the uterine cervix with aggressive clinical course: a case report. Coll Antropol. 2010;34(1):291-294. PubMed | Google Scholar
- Stanley-Christian H, Heim BK, Hines JF, Hall KL, Willett GD, Barnes WA. Villoglandular adenocarcinoma of the cervix: a report of three cases and review of the literature. Gynecol Oncol.1997;66(2):327-330. PubMed | Google Scholar
- Macdonald RD, Kirwan J, Hayat K, Herrington CS, Shawki H. Villoglandular adenocarcinoma of the cervix: clarity is needed on the histological definition for this difficult diagnosis. Gynecol Oncol. 2006; 100(1):192-194. PubMed | Google Scholar
- Garcea A, Nunns D, Ireland D, Brown L. A case of villoglandular papillary adenocarcinoma of the cervix with lymph node metastasis. BJOG. 2003;110:627-9. PubMed | Google Scholar