Metastatic giant basal cell carcinoma: a case report
Bellahammou Khadija, Lakhdissi Asmaa, Akkar Othman, Rais Fadoua, Benhmidou Nawal, Elghissassi Ibrahim, M’rabti Hind, Errihani Hassan
Corresponding author: Bellahammou Khadija, Department of Medical Oncology, National Institute of Oncology, Rabat, Morocco 
Received: 06 Mar 2016 - Accepted: 07 Jun 2016 - Published: 22 Jun 2016
Domain: Clinical medicine
Keywords: Giant basal cell carcinoma, metastasis, prognosis
©Bellahammou Khadija et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Bellahammou Khadija et al. Metastatic giant basal cell carcinoma: a case report. Pan African Medical Journal. 2016;24:157. [doi: 10.11604/pamj.2016.24.157.9233]
Available online at: https://www.panafrican-med-journal.com//content/article/24/157/full
Metastatic giant basal cell carcinoma: a case report
Bellahammou Khadija1,&, Lakhdissi Asmaa1, Akkar Othman1, Rais Fadoua2, Benhmidou Nawal2, Elghissassi Ibrahim1, M’rabti Hind1, Errihani Hassan1
1Department of Medical Oncology, National Institute of Oncology, Rabat, Morocco, 2Department of Radiotherapy, National Institute of Oncology, Rabat, Morocco
&Corresponding author
Bellahammou Khadija, Department of Medical Oncology, National Institute of Oncology, Rabat, Morocco
Basal cell carcinoma is the most common skin cancer, characterised by a slow growing behavior, metastasis are extremely rare, and it occurs in less than 0, 1% of all cases.Giant basal cell carcinoma is a rare form of basal cell carcinoma, more aggressive and defined as a tumor measuring more than 5 cm at its largest diameter. Only 1% of all basal cell carcinoma develops to a giant basal cell carcinoma,resulting ofpatient's negligence. Giant basal cell carcinoma is associated with higher potential of metastasis and even death, compared to ordinary basal cell carcinoma.We report a case of giant basal cell carcinoma metastaticin lung occurringin a 79 years old male patient, with a fatal evolution after one course of systemic chemotherapy.Giant basal cell carcinoma is a very rare entity, early detection of these tumors could prevent metastasis occurrence and improve the prognosis of this malignancy.
Basal cell carcinoma (BCC) is the most common malignant skin tumor in the world with 750,000 cases reported annually in the United States alone [1, 2]; it is more common in males than females. BCC is a slow growing tumor; metastasis areextremely rareand reported in less than 0.1 %of cases [3]. The giant basal cell carcinoma, defined as a lesion with more than 5 cm at its largest diameter,is very rare and presents less than 1% of all basal cell carcinoma [3-5]. Their potential of metastasis is higher than ordinary basal cell carcinoma and the prognosis is very poor. Due to rarity of metastatic disease, all cases published in literature are limited to retrospective studies and cases reports. In this article, we present a case of giant basal cell carcinoma occurring in a 79 years old male patient metastasisin lungs with a fatal evolution.
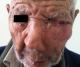
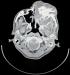
A 79 year-old male presented to our institution complaining of a painful ulcerated skin lesion localized in the left lower eyelid. The patient's history found no comorbidities. On Physical examination, an ulcerated lesionextending to the left orbite was noted (Figure 1). A facial neck and chest computed tomography showed a large enhancing mass of the left maxillary sinus measuring 60x65mm with bilateral suspicious lung nodules (Figure 2, Figure 3). A biopsy of the mass was performed, histopathological examination revealed an infiltrative basal cell carcinoma. A diagnosis of a giant basal cell carcinoma metastatic to the lungs was established;the patient had an ECOG performance status of 2, a blood workup showed he had normal renal function. Platinum based chemotherapy was decided. He received only one course of 5FU-ceplatin then decided tointerrupt the treatment. Unfortunately he died one month after the beginning of treatment.
Basal cell carcinoma is the most common malignant skin tumorand isusually characterized by a slowgrowth. Despite its high incidence, metastatic events are exceedingly rare.The reported frequency of metastatic dissemination is estimated to be less than 0.1% [3]. Risk factors include: Chronic sun exposure, radiation, light skin color, Immune-suppression, Exposure to arsenic, certain hereditary disease including Gorlin-Goltz syndrome and Xerodermapigmentosum, advanced age and male sex [6]. The clinical appearances and morphology are diverse, including micronodular, nodular, infiltrative, superficial,sclerosing,morpheaform,keratotic cystic and pigmented variants [7].
The giant basal cell carcinoma is a rare form of basal cell carcinoma normally defined as a basal cell carcinoma with more than 5 cm at its largest diameter.Only 1% of basal cell carcinoma develops to a giant basal cell carcinoma,due to long duration and patient's negligence in most cases [4]. Giant basal cell carcinoma has been associated with higher incidence of metastasis compared to the ordinary basal cell carcinoma [3, 4] typically to lymph nodes, bone, and lung. The prognosis is poor and the median survival in metastatic cases is around 8 months [8].
Sites of predilection for basal cell carcinoma are head and neck;giant basal cell carcinomas were most likely to occur on the back, face, and upper extremities. The pathogenesis of giant basal cell carcinoma is linked to a mutation of the PTCH gene, mapped to the q22.3 locus of chromosome. This gene has a role in tumor suppression by inhibiting a regulatory signaling cascade of the Sonic Hedgehog pathway [9].
Treatment modalities includesimple excision, electrodessication, curettage, cryotherapy, Mohs Micrographic surgery, topical treatment (imiquimod), photodynamic therapy, radiotherapy and chemotherapy. Chemotherapy for giant basal cell carcinoma can be local and systemic. Systemic treatment is considered for inoperable and metastatic lesions. Due to the rarity of metastatic cases, the literature on chemotherapy for basal cell carcinoma is limited to cases reports. Drugs used for systemic therapy include methotrexate, bleomycin , vincristine, 5-FU, cyclophosphamide, dactinomycin and toyomycin, platinum and taxanes [9]. Vismodegib,a Hedgehog pathway inhibitor is now approved for the treatment of metastatic or locally advanced BCC that has recurred after surgery or which is incurable with surgery or radiation, [10].
Although only 1% of basal cell carcinoma develops into giant basal cell carcinoma, early detection of these tumors by physicians or patients could prevent tumor extension and reduce the risk of metastasis which leads to improve the prognosis of such rare entity.
The authors declare no competing interests.
The case report was written by Bellahammou Khadija. All authors have read and agreed to the final version of this manuscript and have equally contributed to its content and to the management of the case.
Figure 1: ulcerated lesion extending to the left orbit
Figure 2: facial computed tomography showing a large enhancing mass of the left maxillary sinus
Figure 3: thoracic computed tomography showing bilateral suspicious lung nodules
- Mae G, Leffell D, Ziegler A, Gross E, Brash D, Bale A. Relationship between sunlight exposure and a key genetic alteration in basal cell carcinoma. J Natl Cancer Inst.1996; 88(6):349-354. PubMed | Google Scholar
- Amin S, Motamedi K, Ochsner M, Song TE, Hybarger CP. Mechansims and efficacy of vismodegib in the treatment of basal cell carcinoma. Discov Med. 2013; 16(89):229-232. PubMed | Google Scholar
- Lackey LP, Sargent LA, Wong L, Brzezienski M, Kennedy JW. Giant basal cell carcinoma surgical management and reconstructive challenges. Ann Plast Surg. 2007; 58:250. PubMed | Google Scholar
- Randle HW, Roenigk RK, Brodland DG. Giant basal cell carcinoma (T3): who is at risk? Cancer. 1993; 72:1624. PubMed | Google Scholar
- Manstein CH, Gottlieb N, Manstein ME, Beidas OE. Giant basal cell carcinoma: 11-year follow-up and seven new cases. Plast Reconstr Surg. 2011;128:105. PubMed | Google Scholar
- Gilbody JS, Aitken J, Green A. What causes basal cell carcinoma to be the commonest cancer? Aust J Public Health. 1994; 18(2): 218-21. PubMed | Google Scholar
- Mollet T, Clapper R, Smith M, Garcia C. Not all basal cell carcinomas are created equal: a case of a fatal BCC. Dermatol Online J. 2013; 19:9. PubMed | Google Scholar
- Ting PT, Kasper R, Arlette JP. Metastatic basal cell carcinoma: report of two cases and literature review. J Cutan Med Surg. 2005 Jan; 9 (1):10-5. PubMed | Google Scholar
- Zoccali G et al. Giant basal cell carcinoma of the skin: literature review and personal experience. J Eur Acad Dermatol Venereol. 2012 Aug;26(8):942-52. PubMed | Google Scholar
- Sekulic A et al. Pivotal ERIVANCE basal cell carcinoma study: 12-month update of efficacy and safety of vismodegib in advanced BCCJ. J Am Acad Dermatol. 2015 Jun;72(6):1021-6.e8. PubMed | Google Scholar