Peritoneal splenosis mimicking carcinomatosis
Faten Limaiem, Rahma Ayadi, Ghada Sahraoui, Saadia Bouraoui, Ahlem Lahmar, Sabeh Mzabi
Corresponding author: Faten Limaiem, University of Tunis El Manar, Tunis Faculty of Medicine, 1007, Tunisia 
Received: 19 Jan 2016 - Accepted: 10 Apr 2016 - Published: 22 Apr 2016
Domain: Clinical medicine
Keywords: Splenic trauma, splenosis, peritoneum
©Faten Limaiem et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Faten Limaiem et al. Peritoneal splenosis mimicking carcinomatosis. Pan African Medical Journal. 2016;23:222. [doi: 10.11604/pamj.2016.23.222.8904]
Available online at: https://www.panafrican-med-journal.com//content/article/23/222/full
Peritoneal splenosis mimicking carcinomatosis
Faten Limaiem1, Rahma Ayadi1, Ghada Sahraoui1, Saadia Bouraoui1, Ahlem Lahmar1, Sabeh Mzabi1
1University of Tunis El Manar, Tunis Faculty of Medicine, 1007, Tunisia
&Corresponding author
Faten Limaiem, University of Tunis El Manar, Tunis Faculty of Medicine, 1007, Tunisia
Splenosis is an uncommon benign condition resulting from heterotopic autotransplantation of splenic tissues onto exposed vascularised intra- and extraperitoneal surfaces following splenic trauma and surgeries. Splenosis may be mistaken for carcinomatosis upon standard imaging techniques. A 69-year-old female patient with a past medical history of hypertension and splenic trauma, underwent total esophagectomy with polar gastrectomy for adenocarcinoma of the gastric cardia. Macroscopic examination of the surgical specimen disclosed a tumour of the cardia measuring 5 cm in greatest diameter and several dark brown nodules of the greater omentum ranging in size between 2 mm and 12 mm. Histological examination of these nodules confirmed the diagnosis of peritoneal splenosis. The authors emphasize that in patients with a previous history of splenic trauma or surgery, clinicians must consider the existence of splenosis.
Splenosis is the spontaneous autotransplantation of splenic tissue after traumatic injury or splenectomy [1]. It usually occurs within the abdominal and pelvic cavity, involving visceral and parietal peritoneum. Most of the patients with splenosis are asymptomatic, however occasionally; abdominal splenosis can mimic peritoneal malignancy on imaging and pose a diagnostic dilemma. In this paper, we report a new case of peritoneal splenosis that was incidentally diagnosed in a 69-year-old female patient. Our aim was to highlight the clinicopathological features of this relatively rare entity.
A 69-year-old woman with a past medical history of hypertension, traumatic rupture of the spleen and adenocarcinoma of the gastric cardia was referred to the surgery department for surgical treatment of the gastric tumour. Physical examination of the patient was unremarkable. Laboratory tests showed elevated carcinoembryonic antigen levels (15,13 ng/ml). Abdominal computed tomography (CT) scan revealed a polylobed spleen with irregular contours (Figure 1). In addition, multiple intraperitoneal nodules were detected. Considering the past medical history of our patient, preoperative diagnosis of these nodules was either peritoneal splenosis or carcinomatosis. The patient underwent total esophagectomy with polar gastrectomy. Macroscopic examination of the surgical specimen disclosed a cardial tumour measuring 5 cm in diameter. In the greater omentum, there were multiple dark brown nodules ranging in size between 2 mm and 12 mm (Figure 2). Nine lymph nodes were found in the lesser and greater omentum. Histological examination of the tumour of the gastric cardia confirmed the diagnosis of adenocarcinoma of the gastric cardia that invaded the subserosa. The multiple dark brown peritoneal nodules corresponded histologically to normal splenic tissue containing both red and white pulp structures (Figure 3). All lymph nodes that were found in the greater and lesser omentum were not metastatic. On postoperative day 1, the patient died due to hemorrhagic shock.
Splenosis results either from the spillage of cells from the spleen after splenic trauma or, from surgical procedures. Although splenosis is usually found in the peritoneal cavity, it has been reported in the retroperitoneum, the thorax and distant sites such as the brain [2,3]. Generally splenosis is diagnosed during routine diagnostic imaging such as abdominal ultrasound or computed tomography or as an incidental finding at laparotomy. Imaging modalities such as ultrasound, CT and MRI do not provide confirmatory diagnosis. Splenosis may resemble normal splenic tissue upon these imaging techniques and none can exclude carcinomatosis [4,5]. Abdominal splenosis must be differentiated from other peritoneal-based masses namely endometriosis, metastatic peritoneal implants, peritoneal mesothelioma, hemangiomas, and accessory spleen. Many radiologic and nuclear imaging techniques have been explored for non-invasive confirmation of suspected splenosis, with 99 m Technetium heat-damaged erythrocyte scintigraphy regarded as ideal due to preferential uptake in splenic tissue with normal liver uptake [6]. PET scans assist oncologists in treatment planning and malignancy response quantification. A literature review found no reports of splenosis exhibiting PET hypermetabolic activity [7]. Definitive diagnosis of peritoneal splenosis is based on histopathological examination. The histologic features of splenosis have been found to be indistinguishable from those of normal spleen, indicating the possibility of being capable of normal function. It appears that the reticuloendothelial function of the ectopic spleen is preserved to that of normal levels [8-10].
In summary, splenosis is a rare phenomenon that may be mistaken for carcinomatosis upon standard imaging techniques. In our case, peritoneal splenosis lead to confusion and suggested malignancy, as our patient had adenocarcinoma of the gastric cardia. Splenosis should be considered as a crucial differential diagnosis of peritoneal nodules in individuals with a history of splenic trauma or splenectomy to avoid unnecessary invasive diagnostic or therapeutic procedures.
The authors declare no competing interests.
Dr Faten LIMAIEM was the principle investigator who prepared, organized, wrote, and edited all aspects of the manuscript. Dr Rahma AYADI performed the gross and microscopic pathologic evaluation of the pathology specimen. She prepared all of the histology figures in the manuscript. She read, edited, and approved the final version of the manuscript. All the remaining authors read and approved the final manuscript.
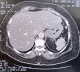
Figure 1: abdominal CT scan revealing a polylobed spleen with irregular contours and multiple intraperitoneal nodules
Figure 2: macroscopic examination of the peritoneal tissue revealing dark brown nodules ranging in size between 0, 2 and 1,2 cm
Figure 3: histological examination of the peritoneal nodules revealing normal splenic tissue containing both red and white pulp structures. (haematoxylin and eosin, original magnification x 200)
- Maillard JC, Menu Y, Scherrer A, Witz MO, Nahum H. Intraperitoneal Splenosis: diagnosis by ultrasound and computed tomography. Gastrointest Radiol. 1989; 14 (2):179-80. PubMed | Google Scholar
- Holstein A, Egberts EH, Stumpf O, Hiller W. Intraperitoneal splenosis: a simple diagnosis if you remember to think of it. Clin J Gastroenterol. 2009; 2 (6): 417-19. PubMed | Google Scholar
- Fremont RD, Rice TW. Splenosis: a review. South Med J. 2007;100 (6):589-93. PubMed | Google Scholar
- Ksiadzyna D, Pe�a AS. Abdominal splenosis. Rev Esp Enferm Dig. 2011; 103 (8): 421-6. PubMed | Google Scholar
- Lake ST, Johnson PT, Kawamoto S, Hruban RH, Fishman EK. CT of splenosis: patterns and pitfalls. Am J Radiol. 2012; 199 (6): W686-W693. PubMed | Google Scholar
- Malik UF, Martin MR, Patel R, Mahmoud A. Parenchymal thoracic splenosis: history and nuclear imaging without invasive procedures may provide diagnosis. J Clin Med Res. 2012; 2 (4): 180-4. PubMed | Google Scholar
- Kellert B, Caster M, Jean RD, Vaccarello L. Diffuse intra-abdominal splenosis presenting as carcinomatosis exhibiting positron emitted tomography hypermetabolic activity. Gynecologic Oncology Reports. 2013; 5 (2): 46-48. PubMed | Google Scholar
- Hathaway JM, Harley RA, Self S. Immunological function in post-traumatic splenosis. Clin Immunol Immunopathol. 1995; 74 (3):143-150. PubMed | Google Scholar
- Pisters PW, Pachter HL. Autologous splenic transplantation for splenic trauma. Ann Surg. 1994; 219 (3): 225-235. PubMed | Google Scholar
- Leemans R, Manson W, Snijder JA. Immune response capacity after human splenic autotransplantation. Ann Surg. 1999; 229 (1):279-85. PubMed | Google Scholar