Small bowel involvement documented by capsule endoscopy in Churg-Strauss syndrome
Birane Beye, Gilles Lesur, Pierre Claude, Lionel Martzolf, Pierre Kieffer, Daniel Sondag
Corresponding author: Birane Beye, Service de Gastroent�rologie, H�pital Ambroise Par�, 92100 Boulogne, France 
Received: 25 Aug 2015 - Accepted: 08 Sep 2015 - Published: 17 Sep 2015
Domain: Clinical medicine
Keywords: Churg-Strauss Syndrome, small intestine involvement, video capsule endoscopy
©Birane Beye et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Birane Beye et al. Small bowel involvement documented by capsule endoscopy in Churg-Strauss syndrome. Pan African Medical Journal. 2015;22:41. [doi: 10.11604/pamj.2015.22.41.7810]
Available online at: https://www.panafrican-med-journal.com//content/article/22/41/full
Small bowel involvement documented by capsule endoscopy in Churg-Strauss syndrome
Birane Beye1,2,&, Gilles Lesur1, Pierre Claude3, Lionel Martzolf4, Pierre Kieffer4, Daniel Sondag3
1Service de Gastroent�rologie, H�pital Ambroise Par�, 9 avenue Charles de Gaulle, 92100 Boulogne, France, 2UFR 2S, Universit� Gaston Berger, St-Louis, S�n�gal, 3Service de Gastroent�rologie, Centre Hospitalier, 20 Avenue R�n� Laennec, 68100 Mulhouse, France, 4Service de M�decine Interne, Centre Hospitalier, 20 Avenue R�n� Laennec, 68100 Mulhouse, France
&Corresponding author
Birane Beye, Service de Gastroent�rologie, H�pital Ambroise Par�, 92100 Boulogne, France
Churg-Strauss syndrome is a small and medium vessel vasculitis and is also known as allergic granulomatous angiitis. Gastrointestinal involvement is common in patients with Churg-Strauss syndrome (20-50%). The most common symptoms are abdominal pain, diarrhoea and occasionally gastrointestinal bleeding and perforation. We present a case of Churg-Strauss syndrome with small bowel lesions documented by video capsule endoscopy.
Churg-Strauss syndrome (CSS) is a systemic and pulmonary vasculitis characterized by the combination of severe late-onset asthma, tissue and blood eosinophilia (greater than 1.5 G/L). It affects small and medium vessels, with segmental and transmural lesions, extravascular tissue infiltrates by eosinophil granulocytes, and granulomas with epithelioid and giant polynuclear cells [1]. Gastrointestinal events frequency is estimated between 20 and 50% of cases [2]. The most common symptoms are abdominal pain, diarrhoea and gastrointestinal bleeding [3]. Small bowel ulcer diagnosed by endoscopy is exceptionally reported in the literature [2]. We report a new case of Churg-Strauss syndrome presenting with small bowel lesions documented by capsule endoscopy.
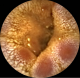
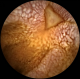
A 30-year-old man was assessed at our department for severe abdominal pain. His past medical history consisted of multiple allergies (pollen, dust mites, dog and cat hair) and a short three-day hospital stay for an exacerbation of asthma managed with oral corticosteroid treatment and bronchodilators. On admission, his temperature was 38�C and blood pressure 120/60 mmHg. Clinical examination of the abdomen and the digital rectal exam were normal. Initial investigations showed an elevated white blood cell count (15600/mm3) with marked eosinophilia (8700/mm3) and a high CRP level at 300mg/L (N<5) but normal renal and hepatic function. Blood and urine cultures, as well as parasite detection tests, were negative. Antineutrophil cytoplasmic antibodies (ANCA), desoxyribonucleic acid (DNA) antibody, anti-nuclear antigen were negative. Cryoglobulin and serologic markers for human immunodeficiency virus (HIV), hepatitis B virus (HBV) and hepatitis C virus (HCV) infection were negative. Upper gastrointestinal endoscopy pushed into the proximal jejunum showed an irregular aspect of the jejunal mucosa, without ulcers, corresponding to sub-acute inflammatory lesions, rich in eosinophils, without granulomas or signs of necrotizing vasculitis at histopathological biopsy analysis. Colonoscopy was normal and biopsies were not taken. Due to the persistence of abdominal pain, capsule endoscopy was performed, revealing submucosal edema with numerous lymphangiectasias and erythematous sites on top of some jejunal valves (Figure 1), as well as large ulcers of various shapes, occasionally geometric (Figure 2). The patient was re-admitted after a few weeks, in the dermatology ward for urticaria and polyarthritis. Treatment with prednisolone (40 mg/day) and azathioprine (2mg/kg/day) was introduced, with good clinical response. A few weeks later, he returned to the emergency department because of a generalized epileptic crisis with cerebral magnetic resonance imaging (MRI) findings suggestive of a likely vascular origin. In addition, heart, kidney and ENT (ear, nose and throat) abnormalities were documented. Taking into account the above clinical and biological evidence, and in light of the capsule endoscopy-demonstrated ulcers, a systemic disease was suspected, leading to a deltoid muscle biopsy which showed necrotizing vasculitis of small vessels with eosinophilia. The combination of asthma, eosinophilia more than 8000/mm3 and necrotizing vasculitis with eosinophilic infiltration of small vessels permitted to establish the diagnosis of CSS. Treatment with cyclophosphamide was started, with inflammatory syndrome and eosinophilia decrease. The initial response was good in terms of clinical symptoms and biological markers control.
The CSS diagnosis has been retained in our case in view of the combination of asthma, blood eosinophilia, inflammatory syndrome, pulmonary infiltrates and extrapulmonary events. Five of the six ACR (American College of Rheumatology) diagnostic criteria (asthma, blood eosinophilia > 10%, peripheral neuropathy, pulmonary infiltrates, abnormal maxillary sinus and extravascular tissue eosinophilia) were present in our patient [1]. Presence of at least four of these criteria allows the diagnosis of CSS, with a sensitivity of 85% and a specificity of 99.7%. Gastrointestinal tract involvement represents the fourth leading cause of death in cases of severe disease after cardiac, neurological and kidney manifestations [4]. Gastrointestinal symptoms during CSS occur in 54% of patients on average, marked, however, by significant variations of up to 92%. The most common symptoms are abdominal pain, representing 59% [3], followed by nausea, vomiting and diarrhoea. In our patient, gastrointestinal symptoms were the first extrapulmonary manifestation and the revelation mode of CSS, a fact in itself rare [5]. This digestive-onset form may be particularly compromising and a poor prognostic factor according to some authors [2], encompassing many dangerous complications perforation [6,7], ischemia [4,6], bleeding [5,8] or obstruction [4], responsible for 30% of deaths during CSS. In our case report, the intestinal disease was analysed using the technique of capsule endoscopy, so far reported only once in the literature [2].
Gastrointestinal events during Churg and Strauss syndrome are reported in one third of patients on average. Most macroscopic involvement are identified by conventional endoscopy, laparotomy or at autopsy. Ulcerations of the small intestine are very few described, and prevalence underestimated, because their exploration is often incomplete. We must therefore think of capsule endoscopy as the need for their evidence is real, because representing part of bad prognostic factors, especially when they are severe, forcing an emergency induction therapy.
The authors no competing interests.
Birane BEYE make substantial contribution, acquisition of data, interpretation of data and draft the manuscript; Gilles LESUR and Daniel SONDAG contributed to acquisition of data and provided critical revision of the article; Pierre CLAUDE, Lionel MARTZOLF and Pierre KIEFFER provided critical revision of the article. All authors have read and agreed to the final manuscript.
Figure 1: submucosal edema with lymphangiectasias and erythematous sites on top of some jejunal valves
Figure 2: geometric ulcer (triangular)
- Noth I, Strek ME, Leef AR. Churg-Strauss syndrome. Lancet. 2003; 361(9357):587-594. PubMed | Google Scholar
- Sanchez R, Aparicio JR, Baeza T, Calero Y. Capsule endoscopy diagnosis of intestinal involvement in a patient with Churg-Strauss syndrome. Gastrointest Endosc. 2006; 63(7): 1082-4. PubMed | Google Scholar
- Lanham JG, Elkon K, Pusey C, Hughes G. Systemic vasculitis with asthma and eosinophilia: a clinical approach to the Churg-Strauss Syndrome. Medicine. 1984; 63(2):65-81.. PubMed | Google Scholar
- Pagnoux C, Mahr A, Guillevin L. Manifestations abdominales et digestives au cours des vascularites syst�miques. Ann Med Intern. 2003; 154(7):457-467. PubMed | Google Scholar
- Fraioli P, Barberis M, Rizzato G. Gastrointestinal presentation of Churg-Strauss syndrome. Sarcoidosis. 1994; 11(1):42-5. PubMed | Google Scholar
- Murakami S, Misumi M, Sakata H, Hirayama R, Kubojima Y, Nomura K, Ban S. Churg-Strauss syndrome manifesting as perforation of the small intestine: report of a case. Surg Today. 2004; 34(9):788-792. PubMed | Google Scholar
- Sharma MC, Rajni S, Sidhu BS. Perforation of small intestine caused by Churg-Strauss syndrome. J Clin Gastroenterol. 1996; 23(3):232-5. PubMed | Google Scholar
- Kazuhiko H, Yasushi H, Hiroyuki T, Youshin A, Yukisato k, Masako K. Ileal ulcers and cytomegalovirus infection in case of Churg-Strauss syndrome. Arch Pathol Lab Med. 2005; 129(6):e141-3. PubMed | Google Scholar