Child sexual abuse: report of 311 cases with review of literature
Laila Essabar, Abdenbi Khalqallah, Badr Sououd Benjelloun Dakhama
Corresponding author: Badr Sououd Benjelloun Dakhama, Laboratory of Clinical and Pathological Psychology, Mohammed V University, Rabat, Morocco 
Received: 10 May 2014 - Accepted: 22 Sep 2014 - Published: 19 Jan 2015
Domain: Public Health
Keywords: Child, rape, incest, reporting, suicide, depression
©Laila Essabar et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Laila Essabar et al. Child sexual abuse: report of 311 cases with review of literature. Pan African Medical Journal. 2015;20:47. [doi: 10.11604/pamj.2015.20.47.4569]
Available online at: https://www.panafrican-med-journal.com//content/article/20/47/full
Child sexual abuse: report of 311 cases with review of literature
Laila Essabar1, Abdenbi Khalqallah1, Badr Sououd Benjelloun Dakhama2,&
1Department of Paediatric Medical Emergencies of Rabat children�s Hospital, Morocco, 2Laboratory of Clinical and Pathological Psychology, Mohammed V University, Rabat, Morocco
&Corresponding author
Badr Sououd Benjelloun Dakhama, Laboratory of Clinical and Pathological Psychology, Mohammed V University, Rabat, Morocco
Child sexual abuse (CSA) is a global problem that has significant consequences for public health; it has been a prominent topic of public concern for more than a decade, but many basic facts about the problem remain unclear or in dispute. We conducted a study of 311 cases of CSA in order to highlight the epidemiological features and negative impact on victims' well-being and to emphasize the need for a multidisciplinary approach to the primary prevention and management of CSA. We noted an increase in cases number with male predominance. Most of our patients came from lower socioeconomic classes. The perpetrators were male in 100% of cases; acquaintances in 70% of cases and family members in 22 cases. Physical examination were normal in 61% of cases, however, a range of psychological and physical effects were identified with dramatic health consequences: three cases of attempted suicide, five pregnancies and one case of HIV virus infection.
Childhood sexual abuse (CSA) is a complex life experience that has become the subject of great community concern and the focus of many legislative and professional initiatives. This is evidenced by the expanding body of literature on sexual abuse, public declarations by adult survivors and increased media coverage of sexual abuse issues. However, in Morocco, because sexual abuse is usually a hidden offense, there are no statistics on how many cases actually occur each year. Statistics cover only the cases that are disclosed to child protection associations, to children�s hospitals or to law enforcement. The purpose of our study is to highlight the epidemiological features and negative physical and mental health effects on CSA victims; and emphasize the need for a multidisciplinary approach to the primary prevention and management of CSA.
We conducted a 20 years (January 1993- March 2014) retrospective study of CSA victims consulting at the department of paediatric medical emergencies of Rabat children's Hospital. The clinical records of 311 patients were reviewed; we identified demographic data, CSA characteristics, clinical and psychological features and therapeutic and follow-up data.
Frequency
�
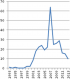
Before the late 1999s, CSA cases were sporadic. In the following decades, the number of cases reported annually increased with a peak in 2007, since that year a little decline was recorded (Figure 1).�
Demographic characteristics�
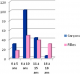
Age: we noted that approximately 15% of victims were between ages 0 and 5 years. Between ages 6 and 10 years, the percentage almost tripled (48%). Ages 11 to 15 years accounted for a quarter (26%) of cases, with children 16 years and older accounting for the remaining 11 % of cases (Figure 2).�
Gender: before the age of 16 years boys were at about two times higher risk than girls, with a percentage of 68 %. Victims 16 years and older were female in 82% of cases (Figure 2).�
Disabilities: we identified 3 cases of CSA with mental retardation�
Socioeconomic status: reported cases came from all socioeconomic classes; however, almost 72% of cases had a low socioeconomic status, the majority was living in sub-rural areas.�
Family structure: we observed some cases of familial impairments, in fact parental substance abuse was noted in 11% of cases, the absence of one/both parents was identified in 17% of cases, as well as the presence of a stepfather in the home (8%) and parental conflicts (45%).�
Abuse characteristics�
Offender: 100% of child sexual abuse perpetrators were men. Offender's relationship to victim: 81% of victims were sexually abused by a non-relative; offenders outside the family were casual acquaintances of the victim in 70% of cases and strangers in 30% of cases. Employers were the offenders in just 3% of victims. We identified 16% cases of incest; of these, two thirds were abused by their biological fathers. 7% of victims were abused by multiple offenders.�
Type of abuse: we noted a spectrum of sexual abuse types ranging from non-contact forms to contact forms of abuse, through to intercourse. In fact, 64% of victims were sodomized, 18% were subjected to fondling and 10% of cases had oral-genital intercourse. We also noted defloration in 8% and exposure to pornography in two cases. Furthermore, the sexual abuse was associated with physical violence in 21% of cases.�
Frequency of abuse: CSA occurred as repeated episodes in 67% of cases: of these, victims were reabused by the same perpetrator in 78% of cases.�
Disclosure: reporting delay ranges from a few hours to 24 months.�
Physical findings: clinical examination was normal in 61% of cases; it showed in the remaining cases non specific findings such as vulvovaginitis, erythema, anal fissures and perianal scars, as well as anal dilatation with stool soiling. We noted anal warts in one case. Signs of additional physical violence were noted in 11%.�
Psychological and behavioral symptoms�
We observed through our study an array of behavioral disorders with different degrees including fear, anxiety, irritability, regression in school performance, sleep disturbances, eating disorders, social problems as well as poor self-esteem. We also noted inappropriate sexualized in some cases. However, approximately 22% of our patients had no symptom. Incest victims had particularly severe problems such as depression and attempted suicide that was noted in three cases.�
Consequences�
The main consequences included three cases of suicide attempts; five cases of pregnancies, three of whom were subjected to incest. Two cases of sexually transmitted infections (STIs) were noted, HIV infection in one case (revealed by the systematic screening for STIs) and HPV anal warts in the second case.�
Management�
Management was based on a multidisciplinary approach with on numerous components ranging from medical and psychological treatment to reporting through social support.
Definition
�
Having a clear operational definition of child maltreatment - and CSA as a specific aspect of child maltreatment- is increasingly recognized as fundamental to effective preventative strategies [1]. The World Health Organization has defined child sexual abuse as being: "The involvement of a child in sexual activity that he or she does not fully comprehend, is unable to give informed consent to, or for which the child is not developmentally prepared and cannot give consent, or that violates the laws or social taboos of society. Child sexual abuse is evidenced by this activity between a child and an adult or another child who by age or development is in a relationship of responsibility, trust or power, the activity being intended to gratify or satisfy the needs of the other person. This may include but is not limited to: the inducement or coercion of a child to engage in any unlawful sexual activity; the exploitative use of a child in prostitution or other unlawful sexual practices; the exploitative use of children in pornographic performance and materials" [2].�
Statistics�
Designing effective child protection measures requires a reliable understanding of the extent of the problem and its context. Globally, the number of studies on the prevalence of CSA has been growing. Based on a summary of existing studies, WHO estimates that between approximately 20 percent of girls and 5 to 10 percent of boys are victims of sexual abuse all over the world [3]. In Morocco, like many developing countries, there is a huge lack in data and the existing findings don't reflect the accurate magnitude of the problem, the main challenge is the sociocultural context and the huge culture of silence that surround sexual issues. A further challenge is that current estimates vary widely as a function of the definitions used, the quality of data collection methods as well as the age of study participants and the age at which childhood is defined. As a global phenomenon, CSA was regarded as rare before the late 1970s. In the following decades, we noted through our study and many other series that the incidence increased dramatically (Figure 1) [4]. Although much of this apparent increase probably reflected a growing awareness among the public and professionals, some studies suggest that the overall incidence of child abuse and neglect increased [5]. The increase in our study may also be due to the creation in 1999 of the children's listening and protection center of the child rights observatory, a structure that provides support and encourages victims to disclose their victimization; reported cases of CSA, however, declined since 2007. This decline could be due to the creation of new medical centers where new cases were referred instead of our department.�
Risk factors�
While it is impossible to create a profile of children who will be sexually abused, it is possible to describe characteristics that are more common among victims and are identified as risk factors for CSA.�
Age: there is some discrepancy in the available data about whether teenagers are at higher risk or whether the risk is more uniformly distributed. Some data [6] show a relatively uniform risk for children after age 3. Other studies found that over half of the children who were sexually victimized were between 15-17 years old [7]. In our study, nearly half of cases were between 6 and 11years while children aged 16 years and older counted 11% because most of them were referred to the gynecological department (for girls) and the adult emergency department (for boys). Moreover, some studies [8] believe that, as a risk factor, age operates differentially for girls and boys, with high risk starting earlier and lasting longer for girls.�
Disabilities: physical disabilities are associated with increased risk [9]. Three factors seem to contribute to this increased vulnerability: dependency, institutional care, and communication difficulties. In a study of 150 interviewed deaf youth at a residential school, 75 children reported being sexually abused, 19 reported being victims of incest, and 3 reported both physical and sexual abuse [8]. We identified, in our study, 3 cases of CSA with mental retardation.�
Gender: all reliable studies conclude that girls experience more sexual abuse than do boys in 78% to 89% of cases [10]. Male children in our studies constitute a large proportion of victims before the age of 16 years.�
Socioeconomic status: although low socioeconomic status is a powerful risk factor for physical abuse and neglect, it has much less impact on CSA. However, a disproportionate number of CSA cases reported to Child Protective Services come from lower socioeconomic classes [11]. In our study, victims coming from economically disadvantaged backgrounds accounted about three quarters of cases.�
Family structure: parental inadequacy, unavailability, conflict, and a poor parent-child relationship show up most consistently in epidemiological studies [12-14] as risk factors for CSA. In many studies children with alcoholic, drug abusing, or emotionally unstable parents are also at risk, as are those with parents who are punitive or distant [15, 16]. However many victims of sexual abuse display none of these markers.�
Other types of victimization: children who experience other forms of victimization are more likely to be the target of sexual victimization [7, 17].
Abuse characteristics Type of abuse: At the extreme end of the spectrum, sexual abuse includes sexual intercourse or its deviations. Yet all offences that involve sexually touching a child, as well as non-touching offenses and sexual exploitation, are just as harmful and devastating to a child's well-being. Touching sexual offenses include fondling; making a child touch an adult's sexual organs; and penetrating a child's vagina or anus no matter how slight with a penis or any object that doesn't have a valid medical purpose. Non-touching sexual offenses include: engaging in indecent exposure or exhibitionism; exposing children to pornographic material; deliberately exposing a child to the act of sexual intercourse; and masturbating in front of a child. Sexual exploitation can include engaging a child or soliciting a child for the purposes of prostitution; and using a child to film, photograph or model pornography. Physical violence is very rarely used; rather the perpetrator tries to manipulate the child's trust and hide the abuse [7, 17]. However in our study CSA was associated with physical violence in 21% of cases.
�
Perpetrators: the perpetrators of sexual abuse are overwhelmingly male. Male constituted 100% of the offenders in our study and more than 90% in many studies [10, 18, 19]. Although female perpetrators constitute a small percentage; abuse by female has been mushrooming recently [20]. According to studies, the third of convicted sex offenders were sexually abused as children [21]. Our study and several studies agree that approximately half of offenders are acquaintances [6, 22]. The studies differ more about the percentage who are family members, the range is going from 14% to 47% [17, 18, 23] with 16% in our work. Strangers make up the smallest group of perpetrators ranging from 7% to 25% [5, 10, 24, 25] with 24% in our study. The apparent percentage of extrafamilial perpetrators should not obscure the accurate proportion of intrafamilial abuse which tends to be underrepresented among reported cases given the sociocultural restraints surrounding sexual issues especially in developing countries like Morocco.�
Frequency of abuse: CSA frequently occurs as repeated episodes that become more invasive with time. Perpetrators usually engage the child in a gradual process of sexualizing the relationship over time [2]. In our study CSA was repeated in 67% of cases: of these, victims were reabused by the same perpetrator in 78% of cases.�
Dynamics of disclosure: children rarely disclose sexual abuse immediately after the event [26, 27]. Disclosure tends to be a process rather than a single episode and is often initiated following a physical complaint or a change in behavior. Disclosure was delayed in the majority of cases in our study reaching 24 months in a 12 years old incest case.�
Physical findings: the evaluation of children requires special skills and techniques in history taking, forensic interviewing and examination; the examiner may also need to address specific issues related to consent and reporting of child sexual abuse [28, 29]. In practice, clear physical findings of sexual abuse are seldom seen in children, as physical force is rarely involved. Many studies have found that normal and non-specific findings are common in sexually abused prepubertal girls [30, 31]; clinical examination in our study was normal in 61% of cases. Moreover, in the vast majority of cases the medical examination will neither confirm nor refute an allegation of sexual assault. Clinical examination may reveal physical health consequences [26, 32], that include gastrointestinal disorders (e.g. irritable bowel syndrome, non-ulcer dyspepsia, chronic abdominal pain); gynaecological disorders (e.g. chronic pelvic pain, dysmenorrhea, menstrual irregularities) and somatization (attributed to a preoccupation with bodily processes). Other serious consequences include pregnancy and sexually transmitted infections (STIs), pregnancy was noted in 5 cases in our study, three of whom were incest victims. A study of factors associated with teenage pregnancy [33], found that forced sexual initiation was the third most strongly related factor, after frequency of intercourse and use of modern contraceptives. An organization for teenage mothers in Costa Rica reported that 95% of its clients under the age of 15 had been victims of incest [34]. The prevalence of STIs in pediatric victims of sexual abuse depends on the type of abusive exposure, genital symptoms, prior consensual sexual activity in adolescents, and the regional prevalence of STIs in the adults [35]. Gellert et al [36] evaluated the risk for HIV seroconversion among children with a history of sexual abuse and found that 28 0.4% were HIV seropositive. Systematic screening for STIs in our study revealed HIV in one case. Sexual abuse is the most worrisome form of HPV transmission. One of our patients contracted HPV anal warts.�
Psychological and behavioural symptoms
A variety of adult psychiatric conditions have been clinically associated with CSA. These include the disorders of major depression, borderline personality disorder, somatization disorder, substance abuse disorders, posttraumatic stress disorder (PTSD), dissociative identity disorder, and bulimia nervosa [5]. This apparent diversity can be explained in part by the heterogeneity of CSA experiences, the complexity of the confounds among abuse severity variables, and a host of moderating and mediating constitutional and environmental variables together with important individual differences in coping strategies that may come into play at different points in development in any given case [37]. Some studies suggest that penetration, the duration and frequency of the abuse, force, the relationship of the perpetrator to the child, and maternal support affected the degree of symptomatology [38]. For instance, survivors of incest may have particularly severe problems, especially if the offender was a father or stepfather. 53% of adult survivors of incest said the abuse caused "some" or "great" long-term psychological effects [21]; in our study, incest resulted in three cases of attempted suicide. Numerous studies have found that sexually abused children exhibited more sexualized behaviors than various comparison groups, including non abused psychiatric patients [38-40]. These include such activities as kissing with one's tongue thrust into the other person's mouth, fondling one's own or another person's breasts or genitals, masturbation, and rythmic pelvic thrusting. Furthermore, a history of CSA, but not a history of physical abuse or neglect, is associated with a significantly increased arrest rate for sex crimes and prostitution irrespective of gender [41]. Despite the variety of behavioral disorders that was found in our study, initial psychological evaluation showed no symptoms in approximately 22% of our patients, this result was consistent with those of other studies [38]. The limited longitudinal data available, however, suggest that 10% to 20% of asymptomatic children will deteriorate over the next 12 to 18 months, this phenomenon is termed sleeper effects [5]. Thus, further studies will be needed to find out the long-term effects on our patients.
�
Management medical care: includes STIs screening and treatment; decisions about STI testing in children should be made on a case-by-case basis. If testing is warranted, age-appropriate diagnostic tests should be used. Presumptive treatment of children for STIs is not generally recommended [2]. STIs screening in our study was systematic, it was repeated when the abuse occurred recently because STI cultures were likely to be negative.�
Psychological treatment: an array of treatment protocols have been offered in the literature providing care for the victims, their families and also the perpetrators. Many studies showed that sexually abused children improved significantly over time [5]. A number of symptoms, especially aggression and sexualized behavior, remain largely resistant to these approaches, however.�
Reporting: every community has its own set of laws governing how, and to whom, a report regarding suspicion of child sexual abuse should be made. Typically the reporting law leaves the final determination as to whether or not abuse occurred to the investigators, not the reporters [42]. Morocco like most communities also has a mandatory reporting structure for professionals working with children.�
Counselling and social support: provide support to the victim and to those caring him. This may be required even if the child itself is not assessed as needing therapy.�
Follow-up consultation: is strongly recommended to ensure that the appropriate counselling referrals have been made and that there is adequate support for the child and family.
Child sexual abuse has substantial consequences not only for the affected persons, but also for society as a whole, and these can no longer be ignored. This Urgent situation has now been recognized in Morocco which is responding with a diverse range of prevention and intervention programs. However the serious shortcomings in data tend to impede the effectiveness of such measures. Thus, improved studies are required in order to provide data on the accurate magnitude of the CSA, on its distribution and factors that point to vulnerability.
The authors declare no competing interest.
All authors have read and approved the final version of the manuscript.
Figure 1: reported cases by year in our study
Figure 2: age and gender of victims in our study
- Alexander Butchart, Harvey AP, Tilman F�rniss, et al. Preventing child maltreatment: a guide to taking action and generating evidence. Geneva, World Health Organization. 2006. http://whqlibdoc.who.int/publications/2006/9241594365_eng.pdf.Accessed 23 April, 2014. PubMed | Google Scholar
- World Health organization. GUIDELINES FOR MEDICO-LEGAL CARE FOR VICTIMS OF SEXUAL VIOLENCE: Child sexual abuse (2003). pp: 75-93. http://whqlibdoc.who.int/publications/2004/924154628x.pdf. Accessed 10 March , 2014. PubMed | Google Scholar
- World Health Organization, Crimes against Children Research Center. Promoting Research to Prevent Child Maltreatment: Summary report of the XIXth ISPCAN International Congress on Child Abuse and Neglect. 2012. http://www.who.int/violence_injury_prevention/violence/child/ispscan_report_june201pdf. Accessed 24 April, 2014. PubMed | Google Scholar
- Finkelhor David. Child sexual abuse: New theory & research. NY: The Free Press. 1984; Vol 77(2): pp xii. PubMed | Google Scholar
- Frank WP. Ten-Year Research Update Review: Child Sexual Abuse. J AM ACAD/ Child adolesc psychiatry. 2003; 42(3): 269-278. PubMed | Google Scholar
- Bolen RM, Scannapieco M. Prevalence of child sexual abuse: A corrective metanalysis. Social Service Review. 1999; 73(3):281-313.. PubMed | Google Scholar
- Finkelhor David, Heather Hammer, Sedlak AJ. Sexually assaulted children: National estimates and characteristics, in OJJDP: Juvenile Justice Bulletin. US Department of Justice. 2008. https://www.ncjrs.gov/pdffiles1/ojjdp/214383.pdf. Accessed 21 April , 2014. Google Scholar
- Sullivan PM, Vernon McCay, Scanlan JM. Sexual Abuse of Deaf Youth. Am Ann Deaf. 1987; 132(4): 256-262. PubMed | Google Scholar
- Westcott Hl, Jones DP. Annotation: the abuse of disabled children. J Child Psychol Psychiatry. 1999; 40(4):497-506. PubMed | Google Scholar
- Synder HN. Sexual assault of young children as reported to law enforcement: Victim, incident and offender characteristics: a NIBRS Statistical Report. USA Department of Justice. 2000. http://www.bjs.gov/content/pub/pdf/saycrle.pdf. Accessed 20 April , 2014. PubMed | Google Scholar
- Finkelhor David. Epidemiological factors in the clinical identification of child sexual abuse. Child Abuse Negl. 1993; 17(1):67-70. PubMed | Google Scholar
- Moore KA, Nord CW, Peterson JL. Nonvoluntary sexual activity among adolescents. Family Planning Perspectives. 1989; 21(3):110-14. PubMed | Google Scholar
- Finkelhor, Sharon Araji. High-risk children. A sourcebook on child sexual abuse. 1986. Beverly Hills. Sage publications. PubMed | Google Scholar
- Paveza GJ. Risk factors in father-daughter child sexual abuse: A case control study. Journal of interpersonal violence. 1988; 3(3): 290-306. PubMed | Google Scholar
- Christopher Bagley, Richard Ramsay. Sexual abuse in childhood: Psychosocial outcomes and implications for social work practice. Journal of Social Work and Human Sexuality. 1986; 4(1):33-47. PubMed | Google Scholar
- Collings Steven. Childhood sexual abuse in a sample of South Africa university males: Prevalence and risk factors. South Afr J Psychol. 1991; 21(3): 153-158. PubMed | Google Scholar
- Kilpatrick DG, Acierno Ron, Saunders BE, et al. Risk factors for adolescent substance abuse and dependence: Data from a national sample. J Consult Clin Psychol. 2000; 68(1):19-30. PubMed | Google Scholar
- Jones LM, Finkelhor David, Kathy Kopiec. Why is sexual abuse declining? A survey of state child protection administrators. Child Abuse & Neglect. 2001; 25(9): 1139-1158. PubMed | Google Scholar
- Crewdson John. By Silence Betrayed: Sexual Abuse of Children in America.1st edition. 1988. NY. Little Brown & Co (T). Google Scholar
- Allen CM. Women and men who sexually abuse children: A comparative study. Orwell, VT: Safer Society Press, 1984. Google Scholar
- Groth NA. Men Who Rape: The Psychology of the Offender. 1979. NY. Plenum Press. PubMed | Google Scholar
- Wonderlich SA, Wilsnack RW, Wilsnack SC et al. Childhood sexual abuse and bulimic behavior in a nationally representative sample. Am J Public Health. 1996; 86(8): 1082-1086. PubMed | Google Scholar
- Briere John, Elliott DM. Prevalence and psychological sequelae of self-reported childhood physical and sexual abuse in a general population sample of men and women. Child Abuse Negl. 2003; 27(10): 1205-1222. PubMed | Google Scholar
- Finkelhor David, Jennifer Dziuba-Leatherman. Children as victims of violence: A national survey. Pediatrics. 1994; 94(4): 413-420. PubMed | Google Scholar
- Hanson RF, Kievit LW, Saunders BE et al. Correlates of adolescent reports of sexual assault: Findings from the National Survey of Adolescents. Child Maltreat. 2003; 8(4): 261-272. PubMed | Google Scholar
- Lori Frasier. Medical Evaluation of Child Sexual Abuse: A Practical Guide, 2nd ed. Arch Pediatr Adolesc Med. 2002; 156(6): 627. PubMed | Google Scholar
- Summit RC. The Child Sexual Abuse Accomodation Syndrome. Child Abuse and neglect. 1983; 7(2):177- 193. PubMed | Google Scholar
- Finkel MA, Giardino AP. Medical evaluation of child sexual abuse: A practical guide, 2nd ed. 2002. Thousand Oaks, Calif. Sage Publications. PubMed | Google Scholar
- David Muram. The medical evaluation of sexually abused children. Journal of Pediatric and Adolescent Gynecology. 2003; 16(1): 5-14. PubMed | Google Scholar
- Emans SJ. Physical examination of the child and adolescent. In: Heger Astrid, Emans SJ, Muram David, eds. Evaluation of the sexual abused child, 2nd ed. NY. Oxford University Press, 2000: 57-78. PubMed | Google Scholar
- Berenson AB, Chacko MR, Wiemann CM et al. A case-control study of anatomic changes resulting from sexual abuse. Am J Obstet Gynecol. 2000; 182(4): 820-834. PubMed | Google Scholar
- Heger Astrid. Making the diagnosis of sexual abuse: ten years later. In: Heger Astrid, Emans SJ, Muram David, eds. Evaluation of the sexually abused child. NY. Oxford University Press. 2000: 1-10. PubMed | Google Scholar
- Jewkes R, Vundule C, Maforah F et al. Relationship dynamics and teenage pregnancy in South Africa. So Sci Med. 2001; 5 (5): 733-744. PubMed | Google Scholar
- Laura LO, Jessica RS. Gender violence interdisciplinary perspectives. NY. New York University Press. 1997. p:235. PubMed | Google Scholar
- Bechtel Kirsten. Sexual abuse and sexually transmitted infections in children and adolescents. Current Opinion in Pediatrics. 2010; 22 (1): 94-99. PubMed | Google Scholar
- Gellert GA, Durfee MJ, Berkowitz CD, et al. Situational and sociodemographic characteristics of children infected with human immunodeficiency virus from pediatric sexual abuse. Pediatrics. 1993; 91(1): 39-44. PubMed | Google Scholar
- Mark Chaffin , Jeffrey NW, Roscoe Dykman . School age children's coping with sexual abuse: abuse stresses and symptoms associated with four coping strategies. Child Abuse Negl.1997; 21(2): 227-240. PubMed | Google Scholar
- Kendall-Tackett KA, Williams LM, Finkelhor David. Impact of sexual abuse on children: A review and synthesis of recent empirical studies. Psychological Bulletin. 1993; 113(1): 164-180. PubMed | Google Scholar
- Paolucci Elizabeth, Genuis Mark, Violato Claudio. A meta-analysis of the published research on the effects of child sexual abuse. J Psychol. 2001; 135(1):17-36. PubMed | Google Scholar
- Friedrich WN, Fisher JL, Dittner CA et al. Child sexual behavior inventory: normative, psychiatric, and sexual abuse comparisons. Child Maltreat. 2001; 6(1): 37-49. PubMed | Google Scholar
- Widom CS , Ames MA. Criminal consequences of childhood sexual victimization. Child Abuse Negl. 1994; 18(4): 303-318. PubMed | Google Scholar
- Kalichman SC. Mandated reporting of suspected child abuse: ethics, law and policy. 1933. Washington DC. Amer Psychological Assn. PubMed | Google Scholar