A pulmonary aneurysm: don't forget Hughes-Stovin syndrome
Madiha Mahfoudhi, Sami Turki
Corresponding author: Madiha Mahfoudhi, Service de M�decine Interne A, H�pital Charles Nicolle, Tunis, Tunisie 
Received: 13 Dec 2014 - Accepted: 22 Dec 2014 - Published: 30 Apr 2015
Domain: Clinical medicine
Keywords: Pulmonary aneurysm, hemoptysis, Hughes-Stovin syndrome
©Madiha Mahfoudhi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Madiha Mahfoudhi et al. A pulmonary aneurysm: don't forget Hughes-Stovin syndrome. Pan African Medical Journal. 2015;20:445. [doi: 10.11604/pamj.2015.20.445.5938]
Available online at: https://www.panafrican-med-journal.com//content/article/20/445/full
A pulmonary aneurysm: don�t forget Hughes-Stovin syndrome
Madiha Mahfoudhi1,&, Sami Turki1
1Service de M�decine Interne A, H�pital Charles Nicolle, Tunis, Tunisie
&Corresponding author
Madiha Mahfoudhi, Service de M�decine Interne A, H�pital Charles Nicolle, Tunis, Tunisie
Hughes-Stovin syndrome is a scarce pathology associating pulmonary artery aneurysms and deep venous thrombosis and affecting commonly the young patient. A 27 year old man was hospitalised for recurrent hemoptysis and a left femoral vein thrombosis. Besides, he had oral ulcers. The ophthalmological examination was normal. Laboratory studies found a microcytic hypochromic anemia (hemoglobin: 11g/dl).The coagulation tests, the renal and the hepatic functions were normal. Besides, the bacteriological examination in search for mycobacterium tuberculosis and the immunological investigations were negative. The chest radiograph revealed a left surrounded para-hilar opacity. The CT of the chest confirmed the presence of a giant aneurysm in the left lower lobe pulmonary artery of 90 mm/72 mm, partially thrombosed, occupying the quasi-totality of the left pulmonary field. All abnormalities of hemostasis, a tumoral origin, a vasculitis like Beh�et's disease and an infectious etiology were eliminated in our patient. Therefore, Hughes-Stovin syndrome was our diagnosis. The patient was put on oral corticosteroid (1 mg/kg/day), and intravenous cyclophosphamide; the steroids were subsequently tapered and withdrawn after 6 months until reaching a minimal dose of 10 mg/day. There has been no recurrence of deep venous thrombosis or hemoptysis. There was no evidence of enlargement of the pulmonary artery aneurysms on chest CT scan control. He was programmed for an embolization because of the giant aspect of the aneurysm.
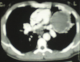
Figure 1: chest�s CT: a giant aneurysm in the left lower lobe pulmonary artery, with mural thrombus