Unilateral multifocal choroidal ischemia revealing a giant cell arteritis: a case report
Zouheir Hafidi, Hanan Handor, Hamid Elmoussaif , Mina Laghmari, Abdelouahed Karmane, Samira Tachfouti, Rajae Daoudi
Corresponding author: Zouheir Hafidi, Universit� Mohammed V Souissi, Service d�Ophtalmologie A de l�H�pital des Sp�cialit�s, Centre Hospitalier Universitaire, Rabat, Maroc 
Received: 22 Jul 2013 - Accepted: 29 Oct 2014 - Published: 30 Oct 2014
Domain: Clinical medicine
Keywords: Giant cell arteritis, choroidal ischemia, multi focal, unilateral
©Zouheir Hafidi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Zouheir Hafidi et al. Unilateral multifocal choroidal ischemia revealing a giant cell arteritis: a case report. Pan African Medical Journal. 2014;19:228. [doi: 10.11604/pamj.2014.19.228.3132]
Available online at: https://www.panafrican-med-journal.com//content/article/19/228/full
Original article 
Unilateral multifocal choroidal ischemia revealing a giant cell arteritis: a case report
Unilateral multifocal choroidal ischemia revealing a giant cell arteritis: a case report
Zouheir Hafidi1,&, Hanan Handor1, Hamid Elmoussaif1, Mina Laghmari1, Abdelouahed Karmane1, Samira Tachfouti1, Rajae Daoudi1
1Universit� Mohammed V Souissi, Service d�Ophtalmologie A de l�H�pital des Sp�cialit�s, Centre Hospitalier Universitaire, Rabat, Maroc
&Corresponding author
Zouheir Hafidi, Universit� Mohammed V Souissi, Service d�Ophtalmologie A de l�H�pital des Sp�cialit�s, Centre Hospitalier Universitaire, Rabat, Maroc
The authors report an unusual case of multifocal choroidal ischemia revealing a giant cell arteritis. A 70 year-old woman presented for a sudden blurry vision in her right eye. The medical anamnesis revealed a previous history of recurrent bilateral fugax amaurosis; she experienced jaw claudication and headache in the few past days, with febricula and generalized weakness.
�
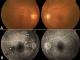
Physical examination, revealed a visual acuity of 6/30 in the right eye and 6/6 in the left eye. Fundoscopy of both eyes was unremarkable, there was, particularly, no optic disk swelling (Figure 1, A). General examination showed a decreased temporal artery pulse on the right side. Fluorescein angiogram of the right eye showed blockage corresponding to a choroidal hypoperfusion (white arrows), and no abnormalities of the left eye (Figure 1, B).�
The patient had a markedly increased erythrocyte sedimentation rate (ESR) (102 mm/hour), with a high level of C reactive protein (CRP) (45mg/dL). A biopsy of the right temporal artery was performed, and histological examination of the specimen showed a polymorphic inflammatory infiltrate associated with some multinucleated clusters of giant cells.�
The patient was diagnosed with Giant cell arteritis, according to the aforementioned histological and clinical data, and received a prompt intravenous three days bolus of methylprednisolone at a dose of 1g per day, relayed by oral corticosteroids at 1 mg/kg/day, during 6 weeks (until normalization of the CRP and ESR) with gradual tapering. Over the next 6 months her visual acuity improved to 6/15 in the right eye.�
Temporal arteritis is a subacute systemic panarteritis with predilection over cranial arteries�
Anterior ischemic optic neuropathy with or without the typical sectoral choroidal ischemia is the most common complication, leading to blindness unless it�s not treated, with a high rate of bilateralization. Isolated choroidal ischemia without retinal vascular occlusion or acute anterior ischemic neuropathy is a rare manifestation of this disorder [1, 2], and is reported to be rather sectoral.�
Unlike sectoral choroidal ischemia, which is, characteristically, due to the occlusion of the posterior ciliary arteries, multifocal choroidal ischemia is caused by the obstruction of the choriocapillaris [3]. Explaining the angiographic findings in this entity; mainly characterized by multifocal unsystematized hypo fluorescent areas, predominating around the optic disc, as noted in our case.�
Numerous disorders may be associated to multifocal choroidal ischemia including toxemia of pregnancy [4], malignant hypertension [5], Vogt-Koyanagi-Harada disease [6], polyarteritis nodosa [7], and other systemic disorders [8, 9]. However it�s not a common finding in giant cell arteritis, which affects large, medium, and small sized arteries, but not capillaries. Our documented case could reflect a possible involvement of choriocapillaris in giant cell arteritis.�
Finally, the treatment should also be considered in such cases, because choroidal ischemia may precede optic nerve involvement [10].
The authors declare no competing interest.
All authors contributed in this work. All authors read and approved the final manuscript.
Figure 1: (A) funduscopic examination: there is no optic disc abnormalities, the rest of the retina appeared normal; (B) Fluorescein angiogram showing a blockage corresponding to a choroidal infarction in the right eye (white arrows)
- Elluard M, Sitbon A, Barreau E. Acute sectoral choroidal ischemia: a case report. J Fr Ophtalmol. 2013 Feb;36(2):124-8. PubMed | Google Scholar
- Olali C, Aggarwal S, Ahmed S, Gupta M. Giant cell arteritis presenting as macular choroidal ischaemia. Eye (Lond). 2011 Jan;25(1):121-3. PubMed | Google Scholar
- Gaudric A, Sterkers M, Coscas G. Retinal detachment after choroidal ischemia. Am J Ophthalmol. 1987 Oct 15;104(4):364-72. PubMed | Google Scholar
- Chaine G, Attali P, Gaudric A, Colin M.C, Quentel G, Coscas G. Ocular fluorophotometric and angiographic findings in toxemia of pregnancy Arch. Arch Ophthalmol. 1986 Nov;104(11):1632-5. PubMed | Google Scholar
- Hayreh SS, Servais GE, Virdi PS. Fundus lesions in malignant hypertension. VI. Hypertensive choroidopathy. Ophthalmology. 1986 Nov;93(11):1383-400. PubMed | Google Scholar
- Touitou V, Escande C, Bodaghi B, Cassoux N, Wechsler B, Lemaitre C, et al. Diagnostic and therapeutic management of Vogt-Koyanagi-Harada syndrome. J Fr Ophtalmol. 2005 Jan;28(1):9-16. PubMed | Google Scholar
- Abouzahir A, Bennouk Y, El Qatni M, El Omri N, Hammi S, Badaoui M, et al. Ocular involvement in polyarteritis nodosa: two cases. J Fr Ophtalmol. 2012 Nov;35(9):724.e1-5. PubMed | Google Scholar
- Coscas G, Gaudric A, Dhermy P, Vernant JP, Cordonnier C. Choriocapillaris occlusion in Moschowitz's disease. J Fr Ophtalmol. 1981;4(2):101-11. PubMed | Google Scholar
- Rapoport P, Merle H, Smadja D. Ischemic choroidopathy in primary Sjogren's syndrome. Acta Ophthalmol Scand. 1998 Oct;76(5):627-8. PubMed | Google Scholar
- Slavin ML, Barondes MJ. Visual loss caused by choroidal ischemia preceding anterior ischemic optic neuropathy in giant cell arteritis. Am J Ophthalmol. 1994 Jan 15;117(1):81-6. PubMed | Google Scholar