Presentation, management, and outcome of snake-bite in two district hospitals in Ghana
Damien Punguyire, Frank Baiden, Josephat Nyuzaghl, Aaron Hultgren, Yvonne Berko, Stephan Brenner, Sari Soghoian, George Adjei, Anjali Niyogi, Rachel Moresky
Corresponding author: Damien Punguyire, Kintampo Municipal Hospital, Kintampo, Ghana 
Received: 19 Aug 2014 - Accepted: 09 Oct 2014 - Published: 28 Oct 2014
Domain: Epidemiology
Keywords: Antivenon, envenomation, snakebites, epidemiology, sub-Saharan Africa
©Damien Punguyire et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Damien Punguyire et al. Presentation, management, and outcome of snake-bite in two district hospitals in Ghana. Pan African Medical Journal. 2014;19:219. [doi: 10.11604/pamj.2014.19.219.5267]
Available online at: https://www.panafrican-med-journal.com//content/article/19/219/full
Original article 
Presentation, management, and outcome of snake-bite in two district hospitals in Ghana
Presentation, management, and outcome of snake-bite in two district hospitals in Ghana
Damien Punguyire1,&, Frank Baiden2, Josephat Nyuzaghl3, Aaron Hultgren4, Yvonne Berko2, Stephan Brenner5, Sari Soghoian6, George Adjei2, Anjali Niyogi7, Rachel Moresky8
1Kintampo Municipal Hospital, Kintampo, Ghana, 2Kintampo Health Research Center, Ghana, 3Bole District Hospital, Bole, Ghana, 4New York University Medical Center, New York, USA, 5Institute of Public Health, Ruprecht-Karls University of Heidelber, Heidelberg, Germany, 6Yale University, New Haven, CT 06520, United States, 7Tulane University, New Orleans, LA 70118, United States, 8Malman School of Public Health, Columbia University Medical Center, USA
&Corresponding author
Damien Punguyire, Kintampo municipal hospital, Kintampo, Ghana
Introduction: the burden of disease represented by snakebites is widely underestimated and often neglected public health problem in the tropics. There is insufficient epidemiological data to guide distribution of antivenin and proper management of venomous snakebites. We describe the presentation, management and outcome of snakebites in two district hospitals in Ghana.
Methods: using data collection sheet, we prospectively documented information on all snakebite victims presenting at two Ghanaian district hospitals from 1st January 2011 to 31st December 2011.
Results: 163 snakebites representing incidence of 92/100,000 were recorded with mean age of 24 (16SD) years. 62.0% were males and 41.7% were farmers. Most bites occurred in April (14.3%), June (12.4%) and November (12.4%) and had occurred when victims were involved in farm-related activities (50.3%). Average time of presentation after snakebite was 3.6 (1.0 SD) hours and commonest clinical presentations were pain (93.0%), swelling (84.0%) and bleeding (51%). Of the total cases 76.7% were given antivenon, 96.3% were given antibiotics, 91.4% corticosteroids and 58.3% antihistamines. No mortality was recorded.
Conclusion: provision of protocols and their strict adherence in the management of snakebites is required to limit unwarranted use of antibiotics and steroids in the management of snakebite. We recommend evaluation of all antivenins imported for management of snakebites to ascertain their effectiveness so as to reduce morbidity and mortality associated with snakebites in this region.
The burden of disease caused by snakebites is a widely underestimated and often neglected problem in Sub-Saharan Africa [1]. This region alone reports an estimated snake envenomations of 10,001 to 100,000 with an incidence of 8.9-93.3/100,000 persons per year and an estimated 1001 to 10,000 deaths representing a mortality rate of 0.5-5.9/100,000 persons per year [2]. Snakebites also cause significant morbidity from direct venom effects such as hemolysis, neurotoxicity, and severe tissue damage, as well as primary or secondary infections at the bite site [3].
�
In Ghana, the saw-scaled viper Echis ocellatus is a commonly found species responsible for the majority of snake envenomation. Most bites occur among rural and farming populations who are exposed to the vipers during agricultural activities. Bites of this species carry relatively high morbidity and mortality due to local tissue necrosis as well as systemic coagulopathies induced by the venom [4]. Anti-venom such as the FAV-Afrique polyvalent anti-venom (Avenits Pasteur) has been used effectively in the treatment of Echis bites [5]. Unfortunately, the supply of effective anti-venom within and outside the health system is often unreliable, or its therapeutic use is too costly for many victims to access [6].�
As a result, effective anti-venom may often be substituted by cheaper, less effective ones [7,8]. A more comprehensive understanding of the local epidemiologic, social, and clinical aspects surrounding snakebites and envenomation can help policy makers and front line health professionals design appropriate strategies to improve prevention and management of these injuries, and reduce snakebite morbidity and mortality. In order to add to the currently available knowledge, we undertook a case series study in two districts of Ghana located in the forest-savanna transition belt. Our data examine and describe the presentation of snakebite cases, the clinical management of the victims, and the treatment outcomes.
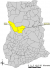
The study was conducted in the Kintampo North Municipality in the Brong-Ahafo Region and the Bole District in the Northern Region of Ghana. Figure 1 is a map Ghana showing the Kintampo north and Bole districts.The vast parts of each of the two districts are essentially rural and characterized by subsistence farming. Each district has one hospital which serves as the main referral health facility for a number of rural health centers. Common snakebites documented in these hospitals in previous years include vipers, cobras, pythons, adders and black mambas.
�
This study included a prospective documentation of snakebite cases presenting to the two hospitals in the period between January and December 2012. We collected detailed quantitative information on the sociodemographic background of the victims, the exposure and circumstances associated with the bite, the pre-hospital care received by the victim, as well as the clinical presentation and treatment outcomes during hospital stay. A specifically-designed questionnaire was administered to victims or close relations after a patient�s initial presentation to the hospital. We supplemented this primary data with clinical information from the medical records of the victims. Health care providers who participated in data collection at the two hospitals were doctors and physician assistants. These were trained in using the data collection sheets, and instructed to notify a member of the study team each time a snakebite victim was admitted, to follow-up the case and update the questionnaire form accordingly until the patient�s discharge or death. We defined snakebites as patients who saw the snake and claimed to have been bitten, or if the patient sustained a definite fang marks and snake was seen or not by the patient, or if patient had clinical evidence of snakebite and snake was seen but no fan marks were identified.�
We used EPI-DATA (version 2.2) for data entry into a digital database. Data analysis using descriptive statistics was done using STATA version 12. Ethical approval for the study was obtained from the institutional review boards of the Kintampo Health Research Center, the Ghana Health Service, and the Columbia University, New York.
One hundred and sixty-three of the snakebite cases (82 in Bole and 81 in Kintampo) were reported during the 12-month study period. This gives a facility-based incidence of 110/100,000 population in Bole and 74/100,000 population in Kintampo, and an overall incidence of 92/100,000 population. Table 1 shows the socio-demographic characteristic snakebite victims. Snakebite victims were generally young with a mean age of 24(16SD) years.
�
The majority were men (62.0%). Male victims were generally younger (20.3,13.6SD years) compared to females(30.3,17.6SD years). The youngest patient was a two yearsold boy who was in the company of older siblings hunting while in the bush. The oldest patient was a 92 female farmer who was bitten on the right leg while working on the farm. Only about 47% of the victims had any form of education with less than 1% going beyond secondary education. Most victims were farmers (41.7%) or students (33.1 %). The highest number of snakebite cases were recorded during the months of April (14.3%), June (12.4%) and November (12.4%). Two thirds (68%) of the bites occurred at night.�
Table 2 shows the distribution of snakebite by exposure characteristics. Bites occurred most when victims were undertaking farming-related activities (50.3 %), other outdoor events (playing on the field, hunting for rats) (16.0%), or in-house activities (waking up to urinate, sleeping) (13.5%). About 86%% of bites occurred at the extremities with lower limb involvement constituting almost 73%. In cases where the snake was seen (58.3%), the majority (75.9%) could not describe the color. The most common colors of snake that were reported were black in 17 cases, black and white in 2 cases, and green in 1 case. Victims or other individuals present at the scene identified the 17 �black� snakes as cobras. In 12 cases, victims/bystanders reported that vipers were involved, which they identified by their local names (i.e. Akwatia and Kyereben). All victims reported to the hospital more than one hour after the snakebite. Average time of presentation after the snakebite was 3.6 (1.0SD) hours and this did not differ with sex and age of victims. The majority (49%) of the patients presented to the emergency room between 4-12 hours after snakebite occurred. Only five patients reported to the hospital more than 24 hours after being exposed to snakebite. Two of these late presenters had received a form of herbal medication prior to presentation at the hospital. In general, few patients received any form of pre-hospital treatment. Pre-hospital treatments that were reported included external application of local herbs (35 cases), incision at the site of bite (16 cases), wound cleaning with water (10 cases), and application of tourniquet (6 cases) or �black stone� to the site of bite (5 cases). Other traditional remedies included concoctions to swallow (2 cases) and application of a starchy fluid from the bark of the pawpaw tree.�
Table 3 displays the clinical manifestations of snakebites.The most frequently encountered clinical presentation was pain at bite site (93%), swelling (84%), and local bleeding (51%). Other manifestations of envenomation included generalized edema (27%), hypotension, hematemesis (12%), dizziness (12%), as well as headache, fever, chills, diarrhea, hematemesis, and anuria. 107 (66.0%) patients showed a prolonged clotting time as measured by the whole blood clotting test. Management and outcome of snakebite patients is presented in Table 4. A total of 125 cases (77%) received snake anti-venom. The majority of patients (61%) were given between 2-5 vials of the snake anti-venom; only one patient received 12 vials before full recovery was achieved. In 47.2% of the cases, the snake anti-venom was supplied free of charge from the Ghana Health Service through regional medical stores, while in 48.8% of the cases the anti-venom was directly purchased by the patient from the hospitals� pharmacies (25.6%) or from pharmaceutical shops in town (23.2%). Most patients also received antibiotics for infection prophylaxis (96%), corticosteroids (91%), and anti-tetanus prophylaxis (74%). Blood transfusions were given to 10% of the patients.�
Nearly all patients (98%) were admitted to the hospitals. Of these, 78.4% were successfully treated and discharged, 4% requested for discharge against advice from the medical team, while 17.3% were referred to a higher level health facilities for reasons such as shortage of blood at the hospital, shortage of anti-venom, and severe infection requiring advanced care. On average a snakebite patient stayed in the hospital for 4.4(1.9SD) days. The length of stay did not vary with age or sex of the victim.
The cumulative incidence of snakebites in our study was 92/100,000 population
�
This health facility based estimate is comparable to similar findings in sub-Saharan Africa [9,10]. The results may, however, grossly underestimate the incidence of snakebites in the general population. Victims of snakebites in sub-Saharan Africa may self-medicate or seek treatment with traditional healers, and may die or recover without ever reaching a health facility [1]. In many areas of Africa, the incidence of snakebites estimated from household or community based studies is 3-5 times higher as compared with health facility based studies [11,12]. The reasons for the difference in incidence documented at each of the two sites in our study are unclear. The disparity could represent a difference in the actual incidence of snakebite, or reflect a difference hospital utilization rates in Bole compared to Kintampo. Patients may either come from adjacent communities or patients may decide to go to another hospital outside of the catchment area [1]. The circumstances surrounding snakebite events among patients in both of the study sites were largely consistent with known risks. For example, global patterns of injury from snakebite suggest that it is predominantly an occupational health risk among agricultural workers [5], with the highest frequency of bites during months devoted to planting and harvest, and a majority of events occurring from late afternoon to early evening [13]. Also, snakes tend to hide during the day to avoid human activity and tend to be more of a risk in darkness when they venture out to look for prey. In our sample, most (66.3%) bites occurred in the evenings when the victims were engaged in farm related activities or other outdoor ventures. In Ghana, the rainy season usually falls between April and September, and farmers start preparing their farms for cultivation around April and May. Planting occurs in June and harvesting in late October and November. A majority of the bites documented in our sample occurred during the months of April (14.29%), June (12.42%) and November (12.42%), which aligns with the farming activities of this mostly agrarian population.�
Most of the snakebite victims in our sample were children and young adults, which is also in agreement with other reports [6,14, 15]. The high incidence of snakebites in these segments of the population is most likely because children and young adult males are those who most often work outdoors in contact with vegetated areas. For example, children in rural areas of Africa are commonly used as herds� men. This outdoor exposure coupled with their natural curiosity might put them at a higher risk for snakebites [15]. About 72% of snakebites in this study involved the lower limbs, which is consistent with most epidemiological findings [10,16]. Tan reported upper limb bites to be more common, but the majority of victims in Tan�s study were soldiers in field training and snake catchers whose outdoor activities differ from those of farming [14].�
Of note, the zero mortality rate attributable to snakebite in our sample was unexpected based on previously published data [1]. This finding might represent a selection bias, and is difficult to interpret without knowledge of the true incidence and outcomes of envenomation in the community. Factors which might have influenced patient outcomes in our sample include the pattern of help-seeking behavior observed, the identity and toxicity of the snakes involved, and therapeutic interventions provided at the health centers. Early presentation to a hospital, coupled with training of emergency staff in snakebite management protocols and adequate supply of anti-venom have been implicated in reducing mortality associated with venomous bites in sub-Saharan Africa [10]. The average time of presentation following the bite in our sample was 3.6 (1.0 SD) hours, which is much earlier than reported in previous studies in this part of the region [10], but comparable to another study done in Nepal [17]. This would suggest a differing health-seeking behavior of the snakebite victims examined in our study, and may have been a factor influencing the health outcomes.�
Different health seeking behavior in the study population was also suggested by the relatively low rates of traditional medicine use and pre-hospital self-treatment reported by patients in the study. Only 21.5% reported any use of herbal medication or application of �black stone� to the bite site prior to presentation at the emergency ward. Secondary injuries from other common forms of first aid, such as tourniquet application or incision and manipulation of the wound, were also relatively rare in this cohort. Similar studies have reported much higher rates of traditional medicine use among victims of snakebites [18]. It is possible that the patients in this study underreported use of traditional or herbal therapies due to fear of repercussions from health care providers [19]. However, the findings might also suggest a degree of confidence in allopathic medical care for this indication.�
The most common clinical features resulting from snakebites in our study were related to local effects such as pain, swelling, and bleeding. Bleeding was present in 51% of the cases and prolonged clotting was 66.0%. These findings suggest a high proportion of cases were likely attributable to vipers, a commonest venomous snakebite in Ghana (16) with hemotoxic venom. Bleeding is usually caused by combined effects of procoagulants contained in the hemotoxic venom of some snake species, which activates factors II and X as well as rhexic hemorrhagins that directly damage the capacitance vessel endothelial basement membrane, leading to disseminated intravascular coagulopathy [20]. Coagulopathic features range from local bleeding or bleeding from nostrils, mouth and wound site, some of which were experienced by our study participants, and 66.0% of patients showed a prolonged clotting time as a result of envenomation. The whole blood clotting time test is a simple, easy and reliable test to determine the degree of coagulopathy as well as to monitor the effectiveness of anti-venom in restoring blood coagulability [21]. The clotting time is considered prolonged or positive when whole blood in a test tube fails to clot at room temperature after 20 minutes.�
Snake anti-venom in this study was administered in about 77% of cases, much higher than reported in other, similar studies [22,23]. This finding might reflect the combined effects of various efforts of the study hospitals to procure snake anti-venom from pharmaceutical companies and local chemical sellers outside the usual supply and procurement systems. Snake anti-venom supplied from outside the routine system cost an equivalent of US$ 35.00 per vial as compared with free distribution from the routine health system. These extra costs are often too high for patients. In addition, the therapeutic effect of these anti-venoms is sometimes doubtful as maintenance of the cold-chain cannot be fully guaranteed in the light of unreliable power supply in these settings. The snake anti-venom used in our study consisted of a lyophilized polyvalent enzyme-refined equine immunoglobulin imported from India. It is produced by Vins Bioproduct limited, and targeted against the venom of four major snake species: the common krait, the Indian cobra (Naja naja), the Russell�s viper, and the Saw-scaled viper [24]. This anti-venom�s therapeutic effectiveness against African snake species, which may be antigenically distinct from Indian snakes, has not yet been verified although other anti-venoms from India showed poor performance against African snakes [5,16]. Over 84% of the victims received between 2-10 vials of antiserum with an average of 4.5vials per victim, a further demonstration of poor results associated with the anti-venom against snakes in this setting. Guideline for administration of anti-venom as well as repeated doses was based on the presence of evidence of envenomation such as prolonged clotting time, bleeding from any part of the body apart from site of bite, evidence of shock, central nervous system manifestations or any prostration following snakebite. Although documentation of adverse reaction to anti-venom was poor, massive use of corticosteroids and antihistamines in this study could possibly be due to these reactions or in their anticipation from previous experience. However, steroids and antihistamines have no documented value as a preventive measure to reduce the incidence of anaphylaxis associated with anti-venom use [25].�
Administration of effective snake anti-venom remains the gold standard in treating life-threatening reactions to snakebites. Unlike the weight-based dosing of many other medications, amount of anti-venoms is usually dependent on the type of snake and the amount of venom injected through the bite [15] as well as the patient�s clinical evolution, abnormal findings, response to initial anti-venom given and patient co-morbidities. Anti-venom should be administered as early as possible during the course of the envenomation, once the activity of venom in the victim�s body has been clinically proven and in order to prevent further deterioration of the patient�s condition [20]. Over 96% of respondents were given prophylactic antibiotics probably due to lack of guidelines, which could lead to wasteful use of antibiotics with potential side effects and development of drug resistance. Prophylactic antibiotics have no documented benefits after snakebite, except for suspicion of secondary infection [13]. 74.2% of the patients were given anti-tetanus. This is similar to observations made by Omogbai et al [26]. Most snakes carry pathogenic organisms, such as Clostridium tetani, in their mouths as part of normal oral flora, and snakebites usually cause punctured wounds [27]. Anti-tetatus prophylaxis should therefore routinely be given after assessing the status of immunization. Blood products, such as packed red blood cells, should only be given for specific indications such as severe haemorrhage or anaemia. Where resources are available transfusion of fresh frozen plasma or Vitamin K administration has been recommended for uncontrolled bleeding when prothrombin time( PT) and partial thromboplastin time(PTT are prolonged [28].�
This study has limitations which affects its interpretation. First, data collection was facility-based. With this, our study cannot provide concise estimates on the incidence of snake bites not reported to the hospital, or about victims who sought care outside the formal health care system. The incidence of snake-bites observed by us is therefore likely an underestimate of the true incidence in this population. To estimate the population-based incidence of snakebites, a household survey would have been the more appropriate method. However, this approach would have been too time consuming and resource-intensive given the geography of the Bole and Kintampo districts. Our facility-based incidence estimates still illustrate an important piece of the epidemiology of snake-bites in health facilities in rural Sub-Saharan Africa and thus provides useful information for health planning purposes related to the appropriate distribution and supply of anti-venom, especially during those seasons when there is an increased risk.�
Secondly, in a good number of cases the snakes were not seen and even in cases where a snake was seen, color description was proffered and no effort was made to identify them for lack of capacity. Proper identification of snakes would have provided good epidemiological information on the type of snakes in the geographic area which could improve the management of snakebites in the region. Lastly, missing information on some of the variables in our data could result in misclassification of variables. However this missing information occurred randomly and therefore its effect will be minimal.
In conclusion, more men report cases of snakebites than women in the two districts studied and tend to occur in the months with higher Agricultural activities. The bites are mostly in the lower limbs. There was a routine use of antibiotics, corticosteroids and antihistamines as prophylaxis due to lack of guidelines in the management of snakebites. Also, administration of anti-venom produced for Indian snakes which already showed poor performance in this setting could lead to prolonged hospitalization. We recommend provision of protocols and their strict adherence in the management of snakebites as a means of limiting unwarranted use of antibiotics and steroids. We further recommend evaluation of all anti-venoms imported for management of snakebite to ascertain their effectiveness so as to reduce morbidity and mortality associated with snakebites in this region.
The authors declare no competing interest.
All the authors participated equally in the conception, design; implementation and write-up of this manuscript and have read and approved the final version of this manuscript before submission.
The authors would like to thank the management and staff of the two hospitals for their full support towards this work. Our appreciation goes to the two research assistants, Helen Fabea of Kintampo municipal hospital and Alhassan Dauda of Bole district hospital for their time. Fundings: this research was fully sponsored by Systems Improve at the District Hospital and Regional Training of Emergency Care (SiHARTe).
Table 1: characteristics of victims and circumstances of snakebite exposure
Table 2: distribution of victims by snakebite exposure characteristics
Table 3: clinical signs and symptoms of snakebites presenting to the two hospitals
Table 4: management and outcome of snakebites in the two district hospitals
Figure 1: a map of Ghana showing Kintampo north and Bole districts
- Chippaux JP. Estimate of the burden of snakebites in sub-Saharan Africa: a meta-analytic approach. Toxicon. 2011; 57(4):586-99. PubMed | Google Scholar
- Kasturiratne A, Wickremasinghe A, de Silva N, Gunawardena NK, Pathmeswaran A, Premaratna R, et al. The global burden of snakebite: a literature analysis and modelling based on regional estimates of envenoming and deaths. PLoS Med. 2008; 5(11):e218. PubMed | Google Scholar
- Abubakar SB, Abubakar IS, Habib AG, Nasida A, Durfa N, Yusuf PO, et al. Pre-clinical and preliminary dose-finding and safety studies to identify candidate antivenoms for treatment of envenoming by saw-scaled or carpet vipers (Echis ocellatus) in northern Nigeria. Toxicon. 2010; 55(4):719-23. PubMed | Google Scholar
- Chippaux JP, Stock RP, and Massougbodji A. Methodology of clinical studies dealing with the treatment of envenomation. Toxicon. 2010; 55(7):1195-212. PubMed | Google Scholar
- Warrell DA. Snake bite. Lancet. 2010; 375(9708):77-88. PubMed | Google Scholar
- Visser LE, Kyei-Faried S and Belcher DW. Protocol and monitoring to improve snake bite outcomes in rural Ghana. Trans R Soc Trop Med Hyg. 2004; 98(5):278-83. PubMed | Google Scholar
- Gutierrez JM, Williams D, Fan HW, Warell DA. Snakebite envenoming from a global perspective: towards an integrated approach. Toxicon. 2010; 56(7):1223-35. PubMed | Google Scholar
- Laing GD, Renjifo JM, Ruiz F, Harrison RA, Nasidi Gutierrez J-M, Rowley PD, Warell DA, et al. A new Pan African polyspecific antivenom developed in response to the antivenom crisis in Africa. Toxicon. 2003; 42(1):35-41. PubMed | Google Scholar
- Larreche S, Mion G, Mayet A, Verret C, Puidupin M, Benois A, et al. Antivenin remains effective against African Viperidae bites despite a delayed treatment. Am J Emerg Med. 2011; 29(2):155-61. PubMed | Google Scholar
- Sloan DJ, Dedicoat MJ, and Lalloo DG. Healthcare-seeking behaviour and use of traditional healers after snakebite in Hlabisa sub-district, KwaZulu Natal. Trop Med Int Health. 2007; 12(11):1386-90. PubMed | Google Scholar
- Chippaux J, Vieillefosse S, Sall O, Mafouta, R, Diallo A. Appraisal of snakebite incidence in Senegal, West Africa. Bulletin de la Soci�t� de pathologie exotique (1990). 2005; 98(4):277-282. PubMed | Google Scholar
- Dabo A, Kouriba B, Traor� A, Diarra Y, Doumbo O. Snakebites in the Sudanian and Sahelian zones of Mali: epidemiology, symptoms and treatment. Med Trop. Mars 2010; 70(1):49-52. PubMed | Google Scholar
- Blaylock R. Epidemiology of snakebite in Eshowe, KwaZulu-Natal, South Africa. Toxicon. 2004; 43(2):159-66. PubMed | Google Scholar
- Tan HH. Epidemiology of snakebites from a general hospital in Singapore: a 5-year retrospective review (2004-2008). Ann Acad Med Singapore. 2010; 39(8):640-7. PubMed | Google Scholar
- Wood D, Webb C, and DeMeyer J. Severe snakebites in northern KwaZulu-Natal: treatment modalities and outcomes. S Afr Med J. 2009; 99(11):814-8. PubMed | Google Scholar
- Visser LE, Kyei-Faried S, Belcher DW, Geelhoed DW, van Leeuwen JS, van Roosmalen. Failure of a new antivenom to treat Echis ocellatus snake bite in rural Ghana: the importance of quality surveillance. Trans R Soc Trop Med Hyg. 2008; 102(5):445-50. PubMed | Google Scholar
- Pandey DP. Epidemiology of snakebites based on field survey in Chitwan and Nawalparasi districts, Nepal. J Med Toxicol. 2007; 3(4):164-8. PubMed | Google Scholar
- Snow RW, Bronzan R, Roques T, Nyamawi C, Murphy S, Marsh K. The prevalence and morbidity of snake bite and treatment-seeking behaviour among a rural Kenyan population. Ann Trop Med Parasitol. 1994; 88(6):665-71. PubMed | Google Scholar
- Aubel J, Rabei H and Mukhtar M. Health workers' attitudes can create communication barriers. World Health Forum. 1991; 12(4):466-71. PubMed | Google Scholar
- Blaylock RS. The identification and syndromic management of snakebite in South Africa: review article. South African Family Practice. 2005; 47(9):48-53. PubMed | Google Scholar
- Bawaskar HS and Bawaskar PH. Profile of snakebite envenoming in western Maharashtra, India. Trans R Soc Trop Med Hyg. 2002; 96(1):79-84. PubMed | Google Scholar
- Simpson ID and Blaylock RS. The anti snake venom crisis in Africa: a suggested manufacturers product guide. Wilderness Environ Med. 2009; 20(3):275-82. PubMed | Google Scholar
- Simpson ID and Jacobsen IM. Antisnake venom production crisis--who told us it was uneconomic and unsustainable? Wilderness Environ Med. 2009; 20(2):144-55. Google Scholar
- VB. VINS Bioproducts Limited? from http://www.vinsbio.in/svaip.html. 2014, Retrieved March 11, 2014. PubMed | Google Scholar
- Nuchprayoon I, Pongpan C and Sripaiboonkij N. The role of prednisolone in reducing limb oedema in children bitten by green pit vipers: a randomized, controlled trial. Ann Trop Med Parasitol. 2008; 102(7):643-9. PubMed | Google Scholar
- Omogbai EK, Nworgu ZA, Imhafidon M, Ikpeme A, Ojo DO, Nwako CN. Snake bites in Nigeria: a study of the prevalence and treatment in Benin City. Tropical Journal of Pharmaceutical Research. 2002; 1(1):39-44. PubMed | Google Scholar
- Akubue PI. Poisons in our Environment and Drug Overdose: In A guide for Health Professionals and the Lay Public 1997. Enugu: Snaaps Press Ltd. 77�82. PubMed | Google Scholar
- Cribari C. Management of Poisonous Snakebites: American college of surgeons committee on trauma, 2004. Sub-committee on publications. Google Scholar