Askin tumor mimicking a hydatid cyst of the lung in children: case report
El Hassane Kabiri, Abderrahmane Al Bouzidi, Meryem Kabiri
Corresponding author: El Hassane Kabiri, Department of Thoracic Surgery, Mohamed V Military Teaching Hospital, Riad 10100 Rabat, Morocco 
Received: 05 Aug 2011 - Accepted: 05 Aug 2012 - Published: 25 Feb 2014
Domain: Clinical medicine
Keywords: Askin tumor, chemotherapy, surgery
©El Hassane Kabiri et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: El Hassane Kabiri et al. Askin tumor mimicking a hydatid cyst of the lung in children: case report. Pan African Medical Journal. 2014;17:131. [doi: 10.11604/pamj.2014.17.131.1056]
Available online at: https://www.panafrican-med-journal.com//content/article/17/131/full
Askin tumor mimicking a hydatid cyst of the lung in children: case report
El Hassane Kabiri1, Abderrahmane Al Bouzidi1, Meryem Kabiri2
1Mohamed V Military Teaching Hospital, Morocco, 2Department of Pediatrics Childrens hospital, Facult� de m�decine et de Pharmacie, Hay Riad � Rabat 10100, Morocco
&Corresponding author
El Hassane Kabiri, Department of Thoracic Surgery, Mohamed V Military Teaching Hospital, Riad 10100
Rabat, Morocco
Askin tumor is a malignant small round cell tumor that originates from the thoracopulmonary region, usually observed in young subjects. We report a case of askin tumor in a 11 year-old men, who had in his past history a surgery for hydatid cyst of the liver, actually hospitalised for right pulmonary upper lobe mass of the lung. After resection of the mass, the pathological exam confirmed the diagnosis of primitive neuroectodermal tumor (PNET). An adjuvant treatment (radiotherapy and chemotherapy) was done; the patient died 11 months after surgery. Askin tumor is an exclusion diagnosis not always readily made.
In 1979, Askin and al first identified a PNET of the thoracopulmonary region in children and young adults as a specific pathological entity [1]. Askin tumors account for approximately 6. 5% of all PNETs, and arises in the periosteum, soft tissue, and extrapulmonary fields of the thoracic wall and in the lung. Over the last decade, diagnosis has greatly improved with the introduction of an array immunohistochemical markers. But, this tumor still raises many questions about its individualisation and its link with Ewing?s sarcoma (ES). Uniform treatment regimen remains undetermined. We report a case of askin tumour mimicking pulmonary hydatid cyst that is endemic in Morocco.
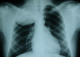
A 11 year-old child was referred to our department with a 1 month history of pain in the right chest. In his past history, he had a surgery of hydatid cyst of the liver three years ago. A physical examination revealed a diminution of the breath sound in the upper right lobe without other clinical sign, and the patient was in excellent condition. The chest X-ray realised in our patient showed right upper lobe opacity (Figure 1) and the first diagnosis suspected, within his past history and endemic aspect of hydatid disease in our region was a hydatid cyst of the lung. The patient was operated and we discovered tissular mass invading upper lobe with suspect parietal contact, we performed a complete resection of the mass with dorsal right upper lobe segmentectomy and resection of parietal pleural beside the tumour. , The diagnosis of askin?s tumor was established histological (Figure 2) on the presence of small cells with scant cytoplasm and focal necrosis, the cells were round and had scant cytoplasm with inconspicuous nucleoli. Mitotic figures were numerous. Rosettes were only focally identified, and immunohistochemistry objective that the tumor cells is positive for neuron-specific enolase (NSE) and CD99. Our patient receives adjuvant chemoradiotherapy with good evolution. Two years after the patient died with lung, liver and bone metastasis.
Askin's tumor or primitive neuroectodermal tumor (PNET), is an extremely malignant small cell tumor of the thoracopulmonary region. Originating from the neuroepithelial cells of the intercostals nerves, these tumors may involve the ribs, the soft tissue of the chest wall, and the lung. An indistinguishable t (11,22) translocation has been demonstrated in Askin?s and Ewing's tumour, perhaps indicating a common origin for these tumours [1, 2], and PNET's are members of Ewing sarcomas family tumours (ESFT). Askin tumor may present as a chest wall mass with thoracopulmonary symptoms such as chest pain, cough, or dyspnea. In our patient, who presented a thoracic pain, upper right lung mass was discovered, and because of his past history of surgery for hydatid cyst of the liver, three years ago, the first diagnosis evocated was a lung localisation of the hydatid cyst. The radiological characteristics of askin tumours are non specific, its might associated with inspissations pleural in 70% or effusion in 28% and rib involvement in 40% of cases. Differential diagnosis has to be made with other small cell tumors such as Ewing's sarcoma, rhabdomyosarcoma, malignant lymphoma, and neuroblastoma [3,4]. Histologically, it contains homogeneous small round-to- spindle cells growing in compact sheets on pseudo-lobules, and exhibit neurosercretory granules and cell. In ultra structures studies, occasionally rosette-like structures were evident but the lack of typical Homer-Wright rosettes excluded neuroblastoma. By immunohistochemistry, the tumor was strongly positive for neuron-specific enolase (NSE), which is a specific marker for neural elements, even though Ewing?s sarcoma and rhabdomyosarcoma may display NSE positive. Genetically, detection of EWS/FLI-1 fusion gene transcripts has recently become a useful tool for the diagnosis of PNET/ES [5]. In our case, the diagnostic of askin tumor was confirmed by histology (Figure 2)
�
Marina et al [6] felt there is a need at least two or three of these criteria for retain the diagnosis of askin's tumors: 1) presence of rosette of homer Wright, 2) origin from a peripheral nerve, 3)the positive of NSE or Leu-7, 4) existence of cytoplasmic extensions, neurosecretory granules and microtubules, 5) the translocation t (11, 22) q (24, 12), 6)detection of proto-oncogenes (N-myc, C-myb, C-ets-1), 7) an activity of biosynthetiques enzymes of the neurotransmitters (tyrosine hydroxylase, dopamine b hydroxylae and acetylcholine transferase).�
Multimodality therapy has improved local control and overall survival for patients with PNET of the chest wall, but uniform treatment regimens remains underteminated. Actually, standard treatment of askin's tumor comprises surgery after chemotherapy [7]. The prognosis in Askin tumor is very poor despite the combination of chemotherapy, radiotherapy, and surgical removal; with a 2 year survival of 38% [2]. Some authors suggest that aggressive treatment with preoperative chemotherapy, radical surgical resection, postoperative chemotherapy, and irradiation is the best approach to Askin tumor [7].
Askin tumors are rare but highly malignant and must treated by aggressive interdisciplinary management including radical surgery and chemotherapy.
Authors declared they have no conflicts of interest.
All authors contributed to the drafting of this manuscript and read and approved the final version.
Figure 1: Chest x-ray
revealed a voluminous opacity of the right upper pulmonary lobe
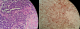
Figure 2: Histological analysis of the mass
- Askin FB, Rosai J, Sibley RK, Dehner LP, Mc Alister WH. Malignant small cell-tumor of the thoraco-pulmonary region in childhood - A distinctive clinicopathologic entity of uncertain histogenesis. Cancer. 1979; 43(6):2438-5. PubMed | Google Scholar
- Contesso G, Lombert-Bosch A, Terrier P et al. Does malignant small round cell tumor of the thoracopulmonary region (Askin tumor) constitute a clinicopathologic entity? An analysis of 30 cases with immunohistochemical and electron-microscopic support treated at the Institute Gustave Roussy. Cancer. 1992; 69(4):1012-20. PubMed | Google Scholar
- Huang DS, Tang SQ, Wang JW, Liu L, Lu S. Two cases of askin tumor misdiagnosed as pulmonary tuberculosis. Zhonghua Er Ke Za Zhi. 2004; 42(4):286. PubMed | Google Scholar
- Kabiri H, EL fakir Y, Mahassini N, Benamor J, Alaziz S, Elmaslout A, Imani F, Benosman A. Tumeur maligne thoraco-pulmonaire � petites cellules (tumeur d'askin). Rev Pneumol Clin. 1999; 55(1):21-5. PubMed | Google Scholar
- Moritake H, Sugimoto T, Kuroda H et al. Newly established Askin tumor cell line and overexpression of focal adhesion kinase in Ewing sarcoma family of tumors cell lines. Cancer Genet Cytogenet. 2003; 146(2):102-9. PubMed | Google Scholar
- Marina N M, Etcubanas E, Parman DM, Bowman LC, Green A. Peripheral primitive neuroectodermal tumor (Peripheral neuroepithelioma) In children: A review of the St Jude experience and controversies in Diagnosis and management. Cancer. 1989; 64(9):1952-60. PubMed | Google Scholar
- Veronesi G, Spaggiari L, De Pas T, Solli PG, De Braud F, et al. Preoperative chemotherapy is essential for conservative surgery of Askin tumors. J Thorac Cardiovasc Surg. 2003; 125(2):428-9. PubMed | Google Scholar