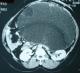
Huge mucinous cystadenoma of the pancreas mistaken for a pseudocyst
Iyiade Olatunde Olaoye, Micheal Dapo Adesina
Corresponding author: Iyiade Olaoye, University Of Ilorin Teaching Hospital, Nigeria 
Received: 01 Mar 2013 - Accepted: 31 Mar 2013 - Published: 03 May 2013
Domain: Clinical medicine
Keywords: Cystic tumor, pancreas, cystadenoma, pseudocyst
©Iyiade Olatunde Olaoye et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Iyiade Olatunde Olaoye et al. Huge mucinous cystadenoma of the pancreas mistaken for a pseudocyst. Pan African Medical Journal. 2013;15:6. [doi: 10.11604/pamj.2013.15.6.2494]
Available online at: https://www.panafrican-med-journal.com//content/article/15/6/full
Huge mucinous cystadenoma of the pancreas mistaken for a pseudocyst
Iyiade Olatunde Olaoye1,&, Micheal Dapo Adesina1
1University Of Ilorin Teaching Hospital, Nigeria
&Corresponding author
Iyiade Olaoye, University Of Ilorin Teaching Hospital, Nigeria
Cystic tumors of the pancreas are rare and can be confused with pseudocysts.We present a 50 year old woman with a huge mucinous cystadenoma of the pancreas initially diagnosed and managed with a cystojejunostomy and cyst wall biopsy. She required another laparotomy and tumor excision after histological diagnosis. Sensitivity of radiological imaging in differentiating between cystic pancreatic tumors and pseudocysts is limited. Cyst wall histology is diagnostic and biopsy of cyst wall should be done in cases with inconclusive preoperative diagnosis or questionable operative findings.
Cystic Neoplasms of the pancreas may be mistaken for pancreatic pseudocyst. Management of a pancreatic cystic tumor as pseudocyst may result in infection of the tumor or formation of gastric ulcers. Cross sectional radiological imaging may not be specific. Analysis of cystic fluid aspirate has improved diagnosis of pancreatic cystic lesions significantly. Biopsy and histology of cyst wall is diagnostic and should be considered in cases with inconclusive preoperative diagnosis and questionable intra operative findings. We present a patient with a huge mucinous cystadenoma of the pancreas initially mistaken for a pancreatic pseudocyst.
A 50 year old lady presented with four months history of back pain radiating towards the epigastrium. She also noticed a gradually increasing abdominal distension. She had weight loss. Bowel habits were normal. She had no previous history of abdominal pains or jaundice. She had an abdominal hysterectomy with left salphingo oophorectomy for uterine fibroids and left ovarian cyst two years before presentation. She had a huge firm non tender central abdominal mass occupying the upper 2/3 of the abdomen. Abdominal ultrasonography and CT scan (Figure 1) suggested a pancreatic pseudocyst. Fasting blood sugar and other relevant hematological parameters were normal. Laparotomy revealed a huge retroperitoneal cyst displacing the stomach upwards and the small bowel into the pelvis. The cyst had a thick wall and contained a thick viscid clear fluid. A biopsy of the wall of the cyst was taken and a cystojejunostomy fashioned. She had post-operative fever that was managed with parenteral antibiotics and was discharged eight (8) days after surgery.
�
Histology of cyst wall revealed Mucinous cystadenoma of the pancreas. She had another laparotomy and complete excision of an infected tumor. Tumor arose from the tail of pancreas and weighed about 3.6kg. Post-operatively, she had hypoproteineamia that improved before discharge. She was discharged fifteen days after the second surgery. She has been followed up for more than five years years and has remained well.
Cystic neoplasms of the pancreas are rare and comprise 10% to 15% of pancreatic cystic masses and only 1% of pancreatic cancers [1]. They are slow growing indolent tumors with low-grade malignant potentials and are mostly seen in middle aged women [2]. Commonly asymptomatic, they sometimes reach large sizes prior to diagnosis. Routine use of abdominal ultrasound, CT and MR has led to an increase in detection of pancreatic cystic lesions and reduced the average size at diagnosis [3,4]. Pancreatic cystic neoplasms consist of Mucinous cystic neoplasms which commonly arise from the body and tail of the pancreas, Serous Cystic neoplasms that are almost always benign, Intraductal papillary mucinous tumors (IPMT) and unusual cystic neoplasms including cystic islet cell tumors. Mucinous cystic neoplasms include mucinous cystadenomas (65%), proliferative cystic mucinous neoplasms (30%) and mucinous cystadenocarcinomas (<10%) [5].
Misdiagnosis and maltreatment of pancreatic neoplasms as pseudocysts is not uncommon [6]. Lack of a history of trauma, chronic pancreatitis or a recent history suggestive of acute pancreatitis should raise a possibility of a cystic neoplasm of the pancreas. Imaging with CT and MRI may not be specific though MRI is more accurate at differentiating a cystic neoplasm from a pseudocyst. Percutaneous or endoscopic ultrasonography with guided aspiration and analysis of cystic fluid for amylase activity, carcinoembryonic antigen level, viscosity, presence of mucin, cytology, tumor markers and DNA analysis improves diagnosis significantly [3,7]. Carcino-embryonic antigen level estimation can be very sensitive in diagnosis of mucinous cystic tumors [8]. These investigations were not available for this patient. Intraoperatively, cystic neoplasms are thick walled and usually contain clear fluid, while pseudocysts fluid is usually grey, opalescent and contain blood or necrotic debris. Biopsy of cyst wall with frozen section and histology is diagnostic [9]. Maltreatment of cystic tumors as pseudocysts lead to infection as occurred in our patient and persistent painful gastric ulcers. Complete excision is the treatment of Mucinous cystic neoplasms of the pancreas because of the possibility of malignancy [1, 7]. Serous cystadenomas may be managed expectantly with close follow up. Recent improvement in morbidity and mortality of pancreatic surgery has encouraged complete excision in patients with serous cystadenoma. Complications of tumor resection include pancreatic fistula, portal vein thrombosis, abscesses, and hemorrhage.
Cystic neoplasms are rare but should be considered in cystic lesions around the pancreas. An absence of history of trauma or history suggestive of inflammation of the pancreas may suggest a cystic tumor necessitating a detailed preoperative evaluation. A biopsy and histology of cyst wall is diagnostic and is indicated in patients with inconclusive preoperative assessment or with questionable intraoperative findings.
The authors declare no competing interest.
Both authors managed the patient and contributed to the manuscript write up in ways that conform to ICMJE authorship criteria.
Figure 1: Huge mucinous cystadenoma of the pancreas CT Abdomen
- Horvath KD, Chabot JA. An aggressive resectional approach to cystic neoplasms of the pancreas. Am J Surg. 1999 Oct;178(4):269-74. PubMed| Google Scholar
- Delcore R, Thomas JH, Forster J, Hermreck AS. Characteristics of cystic neoplasms of the pancreas and results of aggressive surgical treatment. Am J Surg. 1992 Nov;164(5):437-41. PubMed| Google Scholar
- Gonzalvez Gasch AM, Mirete Ferrer C et al. A case of a solid renal mass together with a cystic pancreatic lesion in a 50-year-old patient. JOP. 2005 Mar 10;6(2):172-7. PubMed| Google Scholar
- Engelbrecht M, Bradshaw J, Smithuis R. Pancreatic Cystic Lesions - Diagnosis and management. Available at: http://rad.desk.nl/en/4ec7bb77267de#p4ec7bb772d8ba. Accessed November 2012.
- Sarr MG, Kendrick ML, Nagorney DM, Thompson GB et al. Cystic neoplasms of the pancreas: benign to malignant epithelial neoplasms. Surg Clin North Am. 2001 Jun;81(3):497-509. PubMed| Google Scholar
- Ooi LL, Ho GH, Chew SP, Low CH, Soo KC. Cystic tumours of the pancreas: a diagnostic dilemma. Aust N Z J Surg. 1998 Dec;68(12):844-6. PubMed| Google Scholar
- Al-Haddad M, El Hajj II, Eloubeidi MA. Endoscopic ultrasound for the evaluation of cystic lesions of the pancreas. JOP. 2010 Jul 5;11(4):299-309. PubMed| Google Scholar
- Cizginer S, Turner B, Bilge AR, Karaca C et al. Cyst fluid carcinoembryonic antigen is an accurate diagnostic marker of pancreatic mucinous cysts. Pancreas. 2011 Oct;40(7):1024-8. PubMed| Google Scholar
- Warshaw AL, Rutledge PL. Cystic tumors mistaken for pancreatic pseudocysts. Ann Surg. 1987 Apr;205(4):393-8. PubMed| Google Scholar