Neuroendocrine differentiation in a case of cervical cancer
Mona Mohamed Rashed, Alemayehu Bekele
Corresponding author: Department of Pathology, Damanhour National Medical Institute, affiliated to the: General Organization of Teaching Hospitals and Institutes, Egypt 
Received: 11 Jun 2010 - Accepted: 18 Jul 2010 - Published: 28 Jul 2010
Domain: Pathology
Keywords: Cervical cancer, cervix, chromogranine A, small cell carcinoma
©Mona Mohamed Rashed et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mona Mohamed Rashed et al. Neuroendocrine differentiation in a case of cervical cancer. Pan African Medical Journal. 2010;6:4. [doi: 10.11604/pamj.2010.6.4.262]
Available online at: https://www.panafrican-med-journal.com//content/article/6/4/full
Neuroendocrine differentiation in a case of cervical cancer
Mona Mohamed Rashed1, Alemayehu Bekele2
1Department of Pathology, General Organization of Teaching Hospitals and Institutes, Egypt, 2Department of Pathology, Jimma University, Ethiopia
&Corresponding author
Mona M. Rashed, MD, Department of Pathology, Damanhour National Medical Institute, affiliated to the: General Organization of Teaching Hospitals and Institutes, Egypt
Neuroendocrine neoplasm may occur in the uterine cervix; it accounts for 0.5-1% of all malignant tumors of the uterine cervix [1,2]. It is generally accepted that the integration of HPV into the host genome is the single most important event in evolution of cervical carcinomas [3]. Almost all neuroendocrine carcinomas of the cervix are associated with HPV 18 or seldom HPV 16 [4]. Neuroendocrine carcinomas most likely develop from neuroendocrine cells occurring in the normal endocervix or from stimulated multipotential reserve cells of the endocervical epithelium undergoing neuroendocrine metaplasia and hyperplasia [5]. Neuroendocrine tumors of uterine cervix are divided into small and large cell type as well as carcinoid and atypical carcinoid [3]. Small cell neuroendocrine carcinoma of the uterine cervix is a rare tumor with a highly aggressive clinical course and poor prognosis due to the high frequency of lymph node involvement at an early stage [4,6]. It is important to differentiate small cell carcinoma of the uterine cervix from other malignant tumors of the cervix [4]. Morphological features, cytopathology and histopathology as well as the immunocytochemistry studies play important roles in making an accuratediagnosis [2,7].
An Ethiopian female patient presented at the Gynecology Out-Patient Clinic at Jimma University Hospital, she was 42 years old; complaining of irregular vaginal bleeding over the previous three months. On clinical examination there was a cervical cauliflower mass about 4x4 cm, covering the entire cervical surface. The cervical mass was bleeding on touch. The pelvic ultrasound revealed a bulky cervix with a heterogeneous echo-pattern; moderate pelvic fluid collections were noticed. The patient was serologically negative for HIV. Total abdominal hysterectomy with bilateral salpingo-oophorectomy was performed. The uterus was of normal size with no recognizable tumors either grossly of microscopically. The lymph nodes couldn�t be assessed. The tumor was staged as Stage IB2: T1b2 N0 M0
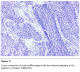
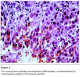
Histo-pathological examination of the cervical mass revealed tumor cells arranged into lobules and solid sheets, the tumor was composed of small undifferentiated cells that showed palisading at the periphery of clusters (figure 1). The tumor cells presented pleomorphic nuclei, with hyperchromatic nuclei, hyperchromatic granular chromatin and the cytoplasm was scanty. Moreover the nuclear-cytoplasmic ratio was high and there was an evidence of increased mitosis as well as apoptotic changes (figure 2).
Immuno-histochemical study was done aiming to recognize neuroendocrine differentiation of the tumor. The paraffin-embedded sections of the cervix were immune-histochemically characterized with antibody to chromogranin-A, the bound antibodies were detected by a standard avidin-biotin complex method with a peroxidase and diaminobenzidine color development system. The cervical tumor showed neuroendocrine differentiation, as demonstrated by chromogranin-A positivity (figure 3).
The diagnosis was pathologically reported as �Small Cell Type of Neuroendocrine Cancer of Uterine Cervix� and the patient was referred to the Oncology Department at Addis Ababa University for chemo-radiotherapy.
Small cell carcinomas of neuroendocrine origin are considered to be the poorly differentiated variety of carcinoid tumors; it is a rare tumor with a highly aggressive clinical course and poor prognosis due to the high frequency of lymph node involvement at an early stage [7]; thus neuroendocrine differentiation is an indicator of poor prognosis [8].
The normal endocervix contains as many as 20% of argyophilic cells resembling endocrine cells; cervical neuroendocrine tumor formation can arise from these cells [9]. Savargaonkar et al reported that neuroendocrine differentiation was present in 20.9% of his series study of cervical carcinoma [5].
Clinically, abnormal vaginal bleeding is the most commonly reported symptoms. In spite of the neuroendocrine origin of this tumor, the clinical carcinoid syndrome in the neuroendocrine tumors of the cervix is very unusual [10]; but on the other hand, a primary carcinoid tumor other than the cervix, with direct secretion of its mediators into the systemic circulation could be responsible for the carcinoid syndrome [9].
The distinction of squamous, glandular and neuroendocrine carcinomas of the cervix is clinically significant for at least two reasons. First, a poorly differentiated carcinoma of glandular origin, even with early invasion, is likely to have a worse prognosis than a similar squamous tumor [11]. Second, neuroendocrine carcinomas are inherently more aggressive than their squamous counterparts and are managed with different protocols [12]. Expression of chromogranin A, synaptophysin, and various other proteins involved in the formation of neurosecretory granules or CD 56, a neural cell adhesion molecule, can be used as markers of neuroendocrine differentiation, as in neuroendocrine carcinomas of other organs [13]. Neuroendocrine carcinomas of the cervix are regarded as highly aggressive tumors [14] with subclinical hematogenous and lymphatic metastases frequently even in early disease. Neuroendocrine features in poorly differentiated carcinomas of the cervix indicate a poor outcome [15]. Sixty-five percent of patients with cervical non-small cell neuroendocrine carcinomas die within 3 yr of diagnosis [1].
We concluded that it is important to differentiate small cell carcinoma from other malignant tumors of the uterine cervix. The diagnosis of small cell neuroendocrine carcinoma depends on the combination of light microscopy and immunohistochemistry. Morphological features play an important role in making a diagnosis and the immunohistochemistry study can offer an additional useful assistance.
The authors declare no competing interests.
M.Rashed was the pathologist responsible for confirming the diagnosis of the case by the immunohistochemistry study. A. Bekele was the first to see the case as neuroendocrine carcinoma and both shared the ideas in reporting this case report.
Figure 1: Tumor composed of small undifferentiated cells that showed palisading at the periphery of clusters (H&Ex200)
Figure 2: The tumor cells presenting pleomorphic nuclei, with hyperchromatic nuclei with hyperchromatic granular chromatin and the cytoplasm is scanty (H&Ex200)
Figure 3: The cervical tumor showing neuroendocrine differentiation, as demonstrated by chromogranin-positivity (Chromogranin-Ax400)
- Gilks CB, Young RH, Gersell DJ, Clement PB. Large cell carcinoma of the uterine cervix: a clinicopathologic study of 12 cases. Am J Surg Pathol. 1997 Aug;21(8):905-14. This article on PubMed
- Huang L, Li C, Chen C, Lee C, Chu P. Small Cell Carcinoma of the Uterine Cervix: A Case Report with Emphasis on Cytopathological Findings. Tzu Chi Med J. 2006; 18(6)
- Mannion C, Park WS, Man YG, Zhuang Z, Albores-Saavedra J, Tavassoli FA. Endocrine tumors of the cervix: Morphologic assessment expression of human papilloma virus, and evaluation for loss of heterozygosity on 1p, 3p, 11q, and 17p.Cancer. 1998; 83:1391-1400. This article on PubMed
- Conner MG, Richter H, Moran CA, Hameed A, Albores-Saavedra J. Small cell carcinoma of the cervix: A clinicopathologic and immunohistochemical study of 23 cases. Ann Diagn Pathol. 2002; 6:345-348. This article on PubMed
- Savargaonkar PR, Hale RJ, Mutton A, Manning V, Buckley CH. Neuroendocrine differentiation in cervical carcinoma. J Clin Pathol. 1996;49:139-141. This article on PubMed
- Albores-Saavedra J, Gersell D, Gilks CB et al. Terminology of endocrine tumors of the uterine cervix: results of a workshop sponsored by the College of American Pathologists and the National Cancer Institute. Arch Pathol Lab Med. 1997 Jan;121(1):34-9. . This article on PubMed
- Bermudez A, Vighi S, Garcia A, Sardi J. Neuroendocrine cervical carcinoma: a diagnostic and therapeutic challenge. Gynecol Oncol. 2001 Jul;82(1):32-9. This article on PubMed
- Koch CA, Azumi N, Furlong MA, Jha RC, Kehoe TE, Trowbridge CH, O�Dorisio TM, Chrousos GP and Clement SC. Carcinoid Syndrome Caused by an Atypical Carcinoid of the Uterine Cervix. J Clin Endocrinol Metab. 1999 Nov;84(11):4209-13. This article on PubMed
- Stockdale AD, Leader M, Phillips RH, Henry K. The carcinoid syndrome and multiple hormone secretion associated with a carcinoid tumour of the uterine cervix Case report. Br J Obstet Gynaecol. 1986 Apr;93(4):397-401. This article on PubMed
- Benda JA. Histopathologic prognostic factors in early stage cervical carcinoma. J Natl Cancer Inst Monogr. 1996;(21):27-34. This article on PubMed
- Ambros RA, Park JS, Shah KV, Kurman RJ. Evaluation of histologic, morphometric, and immunohistochemical criteria in the differential diagnosis of small cell carcinomas of the cervix with particular reference to human papillomavirus types 16 and 18. Mod Pathol. 1991 Sep;4(5):586-93. This article on PubMed
- Dallenbach-Hellweg G, Doeberitz M, Trunk MJ. Color Atlas of Histopathology of the Cervix Uteri; Malignant Tumor, Neuroendocrine Types, Second Edition; 2005, 165-166 . .
- O�Hanlan KA, Goldberg GL, Jones JG, Runowicz CD, Ehrlich L, Rodriguez-Rodriguez L. Adjuvant therapy for neuroendocrine small cell carcinoma of the cervix: review of the literature. Gynecol Oncol. 1991 Nov;43(2):167-72. This article on PubMed
- Barret RJ, Davos I, Leuchter RS, Lagasse LD. Neuroendocrine features in poorly differentiated and undifferentiated carcinomas of the cervix. Cancer. 1987 Nov 1;60(9):2325-30. This article on PubMed